Ulcerative colitis is a chronic inflammatory bowel disease that affects millions of people worldwide. In this article, we will explore the various risk factors associated with the development of ulcerative colitis and discuss effective precautions that can be taken to manage the condition. From genetics to environmental factors, understanding these risk factors is crucial for early detection and prevention. By implementing the right precautions, individuals can lead a healthier and more comfortable life, minimizing the impact of ulcerative colitis on their daily routine. So, let’s dive into the world of ulcerative colitis and arm ourselves with valuable information to protect our well-being.
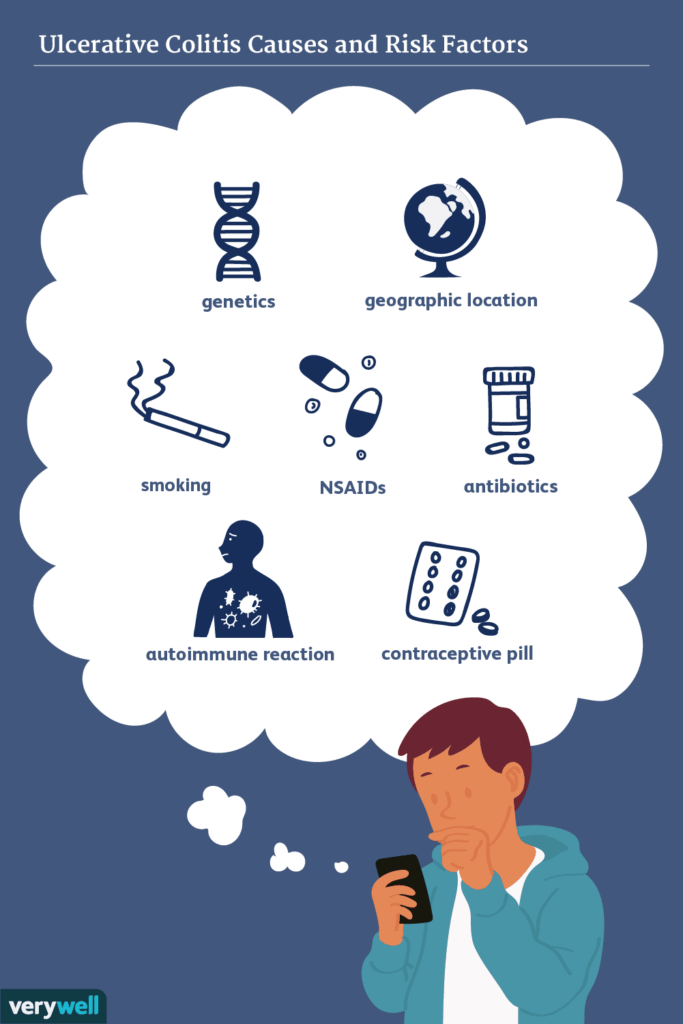
Risk Factors
Ulcerative colitis is an autoimmune disease that affects the colon and rectum. While the exact cause of this condition is unknown, there are several risk factors that have been associated with its development. By understanding these risk factors, you can take necessary precautions to minimize your chances of developing ulcerative colitis.
Genetics
Genetics play a significant role in the development of ulcerative colitis. If you have a family history of this condition, your risk of developing it increases. Research suggests that certain genes may predispose individuals to an abnormal immune response in the colon, leading to the development of ulcerative colitis.
Ethnicity also plays a significant role in the risk of developing ulcerative colitis. Studies have shown that certain ethnic groups, such as Ashkenazi Jews, have a higher prevalence of this condition compared to other populations. This indicates that there may be genetic factors specific to certain ethnicities that contribute to the development of ulcerative colitis.

Immune System
The immune system plays a crucial role in protecting the body against infections and diseases. In individuals with ulcerative colitis, the immune system mistakenly attacks the healthy cells lining the colon, triggering inflammation. Several factors related to the immune system can contribute to the development of this condition.
An abnormal immune response is one of the primary factors contributing to ulcerative colitis. In individuals with this condition, the immune system overreacts to normal bacteria or viruses in the colon, leading to chronic inflammation.
Reduced immune regulation is another factor that increases the risk of developing ulcerative colitis. In individuals with this condition, the immune system fails to regulate the inflammatory response effectively, leading to prolonged inflammation and damage to the colon.
Furthermore, a defective mucosal barrier, which is responsible for preventing harmful substances from entering the colon, can also contribute to the development of ulcerative colitis. When the mucosal barrier is compromised, bacteria and other harmful substances can penetrate the lining of the colon, triggering an immune response and inflammation.
Environmental Factors
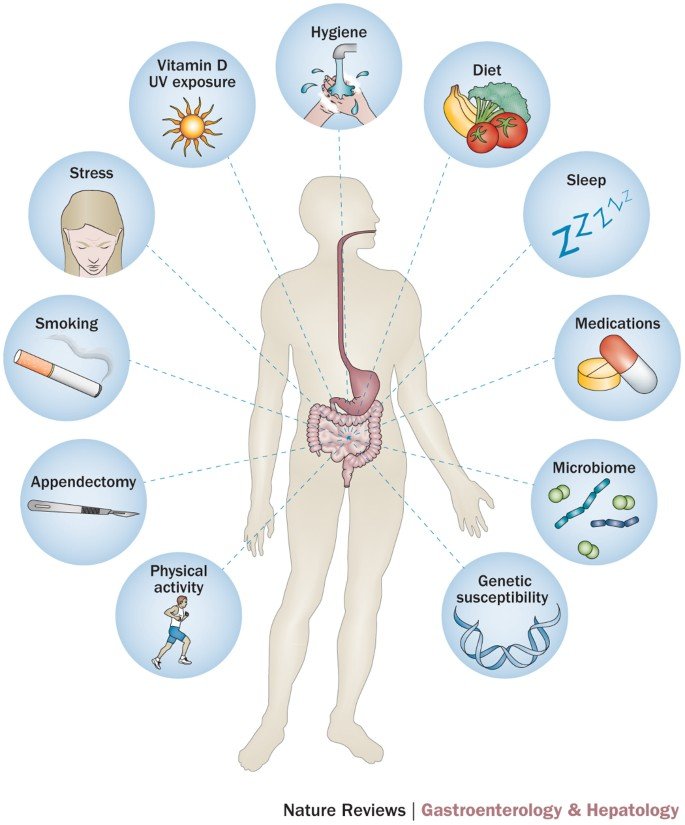
While genetics and the immune system are significant contributors to ulcerative colitis, environmental factors also play a role in its development. Certain aspects of modern living, such as urbanization and westernized lifestyle, have been associated with an increased risk of developing this condition.
Urban living, characterized by a higher population density and exposure to pollutants and toxins, has been linked to an increased risk of ulcerative colitis. The environmental factors present in urban areas may disrupt the balance of bacteria in the gut and trigger an inflammatory response.
Similarly, a westernized lifestyle, which includes a diet high in processed foods and low in fiber, has been associated with an increased risk of ulcerative colitis. This type of diet can affect the composition of gut bacteria and contribute to inflammation in the colon.
Exposure to certain infections has also been linked to an increased risk of ulcerative colitis. Infections such as Escherichia coli (E. coli) and Campylobacter have been associated with the development of this condition. It is believed that these infections can trigger an abnormal immune response in susceptible individuals.
Furthermore, the hygiene hypothesis suggests that reduced exposure to certain microbes and parasites due to improved hygiene practices may contribute to the development of autoimmune diseases like ulcerative colitis. This theory suggests that exposure to a diverse range of microbes in early life helps regulate the immune system, and a lack of exposure can lead to immune dysfunction and inflammation.

Smoking
Smoking has been identified as a significant risk factor for ulcerative colitis. Individuals who smoke have an increased risk of developing this condition compared to non-smokers. Moreover, if you already have ulcerative colitis, smoking can worsen the symptoms and increase the likelihood of flare-ups.
The exact mechanism through which smoking increases the risk of ulcerative colitis is not yet fully understood. However, it is believed that smoking affects the immune system and disrupts the balance of gut bacteria, leading to inflammation in the colon. Quitting smoking is an essential step in reducing the risk of developing ulcerative colitis or managing the symptoms if you already have the condition.
Age and Gender
Age and gender can also influence the risk of developing ulcerative colitis. This condition typically begins during adolescence or early adulthood, with the peak age of onset being between 15 and 30 years old. However, it can develop at any age.
There is also a difference in the risk between genders, with men and women having a similar overall risk but with variations in age of onset and disease course. Women are more likely to be diagnosed with ulcerative colitis in their 50s, whereas men are more likely to be diagnosed in their 60s. These gender differences may be due to hormonal, genetic, or environmental factors that have yet to be fully understood.
Ethnicity
Ethnicity plays a role in the risk of developing ulcerative colitis. Studies have shown that certain ethnic groups have a higher prevalence of this condition compared to others. For example, individuals of Ashkenazi Jewish descent have a significantly increased risk of developing ulcerative colitis.
The reasons for these ethnic differences are not yet fully understood. Genetics, environmental factors, and other cultural or socioeconomic factors specific to certain populations may contribute to the variations in prevalence observed among different ethnicities.
Taking Certain Medications
Certain medications have been associated with an increased risk of ulcerative colitis. Nonsteroidal anti-inflammatory drugs (NSAIDs), commonly taken for pain relief, have been linked to the development of this condition. Prolonged or high-dose NSAID use may disrupt the balance of bacteria in the gut and trigger inflammation in the colon.
Oral contraceptives, commonly used by women for birth control, have also been associated with an increased risk of ulcerative colitis. It is believed that the hormones present in oral contraceptives may affect the immune system and contribute to the development of autoimmune diseases.
Isotretinoin, a medication commonly used for the treatment of severe acne, has been linked to the development of ulcerative colitis. While the exact mechanism is unknown, it is believed that isotretinoin may alter the balance of gut bacteria and trigger an immune response in susceptible individuals.
It is important to note that the risk associated with these medications is relatively low, and many individuals may take them without developing ulcerative colitis. However, if you have a personal or family history of autoimmune diseases, it is essential to discuss the potential risks and benefits of these medications with your healthcare provider.

Personal or Family History of Autoimmune Diseases
If you have a personal or family history of autoimmune diseases, your risk of developing ulcerative colitis is increased. Studies have shown a strong association between ulcerative colitis and other autoimmune conditions, such as rheumatoid arthritis and type 1 diabetes. This indicates that there may be common genetic or immune-related factors that contribute to the development of these conditions.
If you have a personal or family history of autoimmune diseases, it is crucial to monitor your symptoms closely and seek medical advice if you notice any changes or worsening symptoms. Early detection and intervention can help manage the condition more effectively and prevent complications.
Monitor Symptoms and Seek Medical Advice
Regularly tracking your symptoms is essential in managing ulcerative colitis. By keeping a symptom diary, you can identify any patterns or triggers that may worsen your symptoms. This can help you make necessary lifestyle changes or seek medical advice if needed.
If you experience worsening symptoms or notice any changes in your condition, it is important to contact your healthcare provider. They can assess your symptoms, conduct necessary tests, and adjust your treatment plan accordingly. Regular check-ups and follow-ups with your healthcare provider are also crucial in managing ulcerative colitis and preventing future complications.
In conclusion, ulcerative colitis is a complex condition with various risk factors. By understanding these risk factors, you can take necessary precautions to minimize your chances of developing this condition or manage it effectively if diagnosed. Take the necessary steps to maintain a healthy lifestyle, seek medical advice when needed, and stay proactive in managing your symptoms.