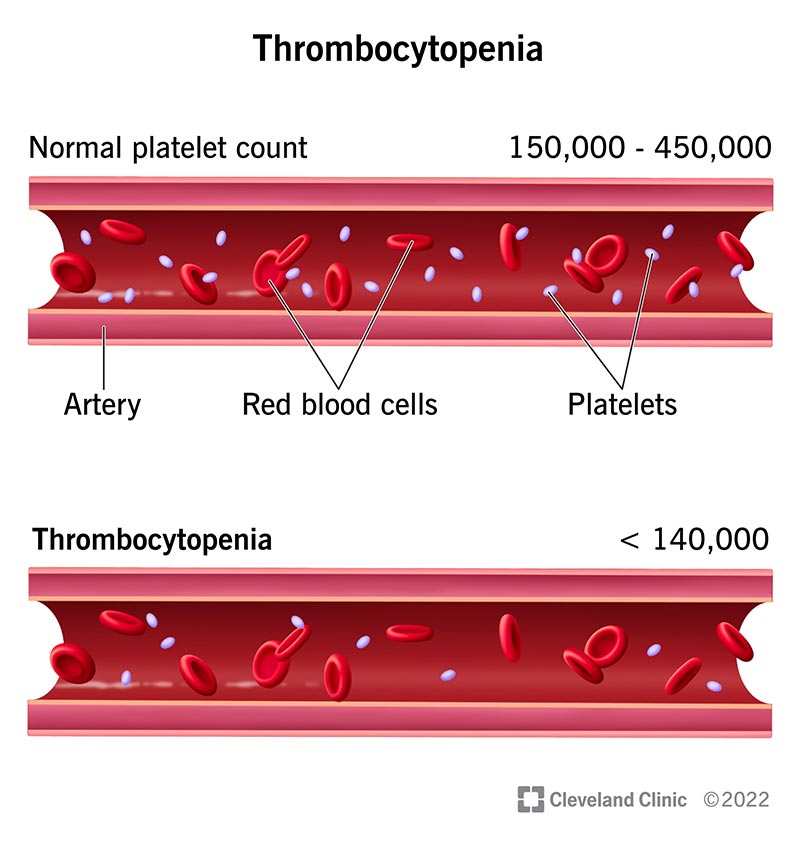
Thrombocytopenia, or low blood platelets, can be a concerning condition with a range of potential risk factors. Whether it’s due to medication side effects, autoimmune disorders, or certain infections, understanding these risk factors is crucial to taking the necessary precautions. This article provides a valuable overview of the different risk factors associated with thrombocytopenia and offers practical measures individuals can take to minimize the potential impact of this condition on their overall health. So, if you’ve ever wondered about thrombocytopenia and how to protect yourself, keep reading!

Risk Factors for Thrombocytopenia
Thrombocytopenia, or low blood platelet count, can be caused by various factors. Understanding these risk factors is crucial in managing and preventing the condition. Here are some of the key risk factors for thrombocytopenia:
Underlying Health Conditions
Certain underlying health conditions can increase the risk of developing thrombocytopenia. These include:
- Bone Marrow Disorders: Conditions such as aplastic anemia, myelodysplastic syndromes, and leukemia can affect the production of platelets in the bone marrow, leading to thrombocytopenia.
- Cancers: Patients with certain types of cancer, such as leukemia, lymphoma, and multiple myeloma, are at a higher risk of developing thrombocytopenia due to the impact of the cancer itself or the treatments involved.
- Kidney or Liver Disease: Chronic kidney disease and liver disease can disrupt platelet production and clearance, contributing to thrombocytopenia.
- HIV/AIDS: Individuals with HIV/AIDS may experience low platelet counts as a result of both HIV infection itself and certain medications used for treatment.
- Systemic Lupus Erythematosus (SLE): This autoimmune disorder can cause the immune system to attack platelets, leading to thrombocytopenia.
- Rheumatoid Arthritis: In some cases, rheumatoid arthritis can result in the destruction of platelets, leading to thrombocytopenia.
- Hypersplenism: This condition, characterized by an enlarged spleen, can trap and destroy platelets, causing thrombocytopenia.
- Myelodysplastic Syndromes: These disorders affect the production of healthy blood cells, including platelets, leading to low platelet counts.
- Thrombotic Thrombocytopenic Purpura (TTP): TTP is a rare blood disorder characterized by blood clots forming in small blood vessels, leading to a decrease in platelet count.
- Heparin-Induced Thrombocytopenia (HIT): HIT is a condition that can occur as a result of heparin therapy, leading to a decrease in platelet count.
Medications or Treatments
Certain medications and treatments can also contribute to the development of thrombocytopenia. These include:
- Chemotherapy: Chemotherapy drugs used to treat cancer can suppress the bone marrow’s ability to produce platelets, resulting in thrombocytopenia.
- Radiation Therapy: Similar to chemotherapy, radiation therapy can damage the bone marrow and decrease platelet production, leading to low platelet counts.
- Antibiotics: Some antibiotics, such as certain types of penicillin and sulfonamides, can cause a drop in platelet count in some individuals.
- Anticoagulants: These medications, used to prevent blood clots, can occasionally lead to thrombocytopenia as a side effect.
- Antiplatelet Drugs: While these medications are used to prevent blood clotting, they can also lower platelet counts.
- Heparin: Heparin, a blood-thinning medication, can cause a decrease in platelet count in some individuals, resulting in heparin-induced thrombocytopenia.
- Immune Globulin: In rare cases, treatment with immune globulin can cause thrombocytopenia.
- Platelet Transfusion: Though uncommon, platelet transfusions can sometimes lead to a decrease in platelet count.
- Bone Marrow Transplant: Thrombocytopenia can occur as a complication of a bone marrow transplant, as the body’s immune system may attack the newly transplanted cells.
- Splenectomy: Removal of the spleen for various reasons can affect platelet counts, potentially leading to thrombocytopenia.
Infections
Certain infections can contribute to the development of thrombocytopenia. These include:
- Viral Infections: Viruses such as Epstein-Barr virus (EBV), cytomegalovirus (CMV), HIV, and hepatitis C can cause low platelet counts.
- Bacterial Infections: Bacterial infections such as sepsis can sometimes lead to thrombocytopenia by affecting platelet production or by causing destruction of platelets.
- Parasitic Infections: Parasitic infections like malaria can cause thrombocytopenia by interfering with the body’s normal platelet function.
- Hepatitis C: Chronic hepatitis C infection can cause thrombocytopenia due to the destruction of platelets.
- HIV/AIDS: Besides the direct impact on platelet counts, HIV infection can also make individuals more susceptible to other infections that may lead to thrombocytopenia.
- Cytomegalovirus (CMV): CMV infection can induce thrombocytopenia, particularly in individuals with weakened immune systems.
- Epstein-Barr Virus (EBV): In some cases, EBV infection can lead to low platelet counts and subsequently thrombocytopenia.
- H. pylori Infection: H. pylori, a bacteria that can cause stomach ulcers, has been associated with thrombocytopenia in some individuals.
- Hemolytic Uremic Syndrome (HUS): HUS, often caused by certain strains of E. coli infection, can result in kidney damage and thrombocytopenia.
- Dengue Fever: This viral infection, transmitted by mosquitoes, can cause severe thrombocytopenia due to increased destruction and decreased production of platelets.
Autoimmune Disorders
Autoimmune disorders occur when the immune system mistakenly attacks healthy cells, including platelets. These conditions can contribute to thrombocytopenia. Common autoimmune disorders associated with thrombocytopenia include:
- Immune Thrombocytopenia (ITP): ITP is an autoimmune disorder where the immune system attacks platelets, leading to a decreased platelet count.
- Systemic Lupus Erythematosus (SLE): SLE is a chronic autoimmune disease that can affect multiple organs, including the blood cells. It can lead to thrombocytopenia due to immune system dysfunction.
- Rheumatoid Arthritis: Rheumatoid arthritis, an autoimmune condition, can occasionally result in thrombocytopenia when the immune system attacks platelets.
- Antiphospholipid Syndrome: This autoimmune disorder characterized by abnormal blood clotting can also cause thrombocytopenia.
- Systemic Sclerosis: Also known as scleroderma, this disorder can affect multiple systems, including the blood cells, potentially leading to thrombocytopenia.
- Graves’ Disease: An autoimmune condition affecting the thyroid gland, Graves’ disease can occasionally cause thrombocytopenia.
- Crohn’s Disease: Though rare, Crohn’s disease can lead to low platelet counts in some individuals.
- Ulcerative Colitis: Similar to Crohn’s disease, ulcerative colitis can sometimes result in thrombocytopenia.
- Mixed Connective Tissue Disease (MCTD): MCTD is an autoimmune disease that presents with overlapping features of several connective tissue disorders, including thrombocytopenia.
- Sjögren’s Syndrome: This autoimmune disorder primarily affects the tear and salivary glands but can also impact the platelet count in some individuals.
Family History
Genetic factors can contribute to an individual’s risk of developing thrombocytopenia. Here are some family history-related risk factors:
- Genetic Predisposition: Having a family history of thrombocytopenia can increase the likelihood of developing the condition.
- Inherited Thrombocytopenic Disorders: Certain genetic conditions, such as Bernard-Soulier syndrome and Glanzmann’s thrombasthenia, are inherited disorders that cause low platelet counts.
- Familial Autoimmune Disorders: In some cases, several family members may have autoimmune disorders that can include thrombocytopenia as one of their manifestations.
- Congenital Amegakaryocytic Thrombocytopenia (CAMT): This rare inherited disorder affects the production of platelets in the bone marrow, leading to thrombocytopenia.
- Fanconi Anemia: Fanconi anemia is an inherited blood disorder that can be associated with a decreased platelet count.
- Wiskott-Aldrich Syndrome: This rare X-linked disorder affects blood cells, including platelets, resulting in thrombocytopenia.
- May-Hegglin Anomaly: In this inherited condition, the platelets are larger than normal, leading to low platelet counts.
- Sebastian Syndrome: Like May-Hegglin anomaly, Sebastian syndrome is also characterized by large platelets and low platelet counts.
- Thrombocytopenia-Absent Radius (TAR) Syndrome: TAR syndrome is a genetic disorder that affects the development of both platelets and the radius bone in the forearm.
- X-Linked Thrombocytopenia (XLT): XLT is an inherited condition primarily affecting males and causing low platelet counts due to a genetic mutation.
Chronic Liver Disease
Chronic liver diseases can impact platelet counts and contribute to thrombocytopenia. Common chronic liver conditions associated with thrombocytopenia include:
- Cirrhosis: As the liver becomes increasingly damaged and scarred, it can disrupt platelet production and lead to thrombocytopenia.
- Hepatitis B: Chronic hepatitis B infection can affect the liver’s ability to produce platelets, resulting in low platelet counts.
- Hepatitis C: Besides the direct impact on platelet counts, chronic hepatitis C infection can cause immune-mediated destruction of platelets, leading to thrombocytopenia.
- Alcoholic Liver Disease: Long-term alcohol consumption can cause liver damage and adversely affect platelet production, leading to low platelet counts.
- Primary Biliary Cirrhosis: This autoimmune liver disease can cause liver damage, which can subsequently lead to thrombocytopenia.
- Primary Sclerosing Cholangitis: Another autoimmune liver disease, primary sclerosing cholangitis, can contribute to thrombocytopenia.
- Wilson Disease: Wilson disease is a genetic disorder that affects copper metabolism in the body and can result in liver damage, leading to thrombocytopenia in some individuals.
- Hemochromatosis: This inherited disorder results in the accumulation of iron in the body, including the liver, potentially leading to thrombocytopenia.
- Budd-Chiari Syndrome: This rare condition is characterized by the obstruction of the hepatic veins, resulting in liver damage and low platelet counts.
- Autoimmune Hepatitis: This chronic liver disease caused by an autoimmune response can lead to liver damage and, in turn, thrombocytopenia.
Chemotherapy or Radiation
Cancer treatments such as chemotherapy and radiation therapy can have adverse effects on the bone marrow, leading to thrombocytopenia. Here are some factors related to cancer treatments:
- Chemotherapy Side Effects: Chemotherapy drugs can impact the production of platelets in the bone marrow, leading to low platelet counts.
- Radiation Side Effects: Similar to chemotherapy, radiation therapy can damage the bone marrow and affect platelet production.
- Bone Marrow Suppression: Cancer treatments can suppress the normal functioning of the bone marrow, leading to decreased platelet production.
- Myelosuppressive Agents: Certain chemotherapy drugs are specifically designed to suppress the bone marrow, which can result in thrombocytopenia.
- Total Body Irradiation: This treatment modality used in bone marrow transplantation can damage the bone marrow and impact platelet counts.
- Radiation to Bone Marrow: When radiation therapy is targeted to areas containing bone marrow, it can affect platelet production and lead to thrombocytopenia.
Alcohol Consumption
Excessive alcohol consumption can contribute to thrombocytopenia. Here are some factors related to alcohol consumption:
- Liver Damage: Long-term excessive alcohol consumption can cause liver damage, which can disrupt platelet production and result in thrombocytopenia.
- Bone Marrow Suppression: Chronic alcohol abuse can also suppress the bone marrow’s ability to produce platelets, leading to low platelet counts.
Pregnancy and Childbirth
Pregnancy and childbirth can sometimes lead to thrombocytopenia due to various physiological changes. Here are some factors related to pregnancy and childbirth:
- Gestational Thrombocytopenia: Low platelet counts can occur in some pregnant women without any underlying health conditions or complications. This condition is known as gestational thrombocytopenia and typically resolves after childbirth.
- Pre-eclampsia and HELLP Syndrome: These pregnancy-related conditions can cause damage to blood vessels and result in low platelet counts.
- Immune Thrombocytopenic Purpura (ITP) in Pregnancy: Some women may develop ITP during pregnancy, causing a decrease in platelet count. It is important for them to get proper medical care to manage their condition during pregnancy and childbirth.
Age
The risk of developing thrombocytopenia can increase with age. Older individuals may be more susceptible to certain health conditions, medications, and treatments that can contribute to low platelet counts.

Precautions for Thrombocytopenia
While it may not always be possible to prevent thrombocytopenia entirely, there are precautions and measures you can take to minimize the risks associated with the condition. Here are some key precautions for individuals with thrombocytopenia:
Avoiding Trauma and Injury
As thrombocytopenia can lead to prolonged bleeding and difficulty clotting, it is essential to take precautions to avoid trauma and injuries. Here are some guidelines to follow:
- Be cautious during physical activities: Engage in sports and physical activities that carry a lower risk of injury or trauma.
- Use protective gear: Wear appropriate protective gear, such as helmets, knee pads, and elbow pads, when participating in higher-risk activities.
- Take extra care while handling sharp objects: Be cautious while handling knives, scissors, and other sharp objects to avoid accidental cuts and injuries.
- Ensure a safe environment: Make sure your living and working environments are free from tripping hazards and other potential sources of injury.
Maintaining Good Hygiene
Maintaining good hygiene practices is crucial for individuals with thrombocytopenia. Here are some hygiene precautions to follow:
- Wash your hands regularly: Wash your hands with soap and water for at least 20 seconds, especially before handling food, after using the restroom, and after coming into contact with potentially contaminated surfaces.
- Use hand sanitizer when soap is not available: If soap and water are not readily available, use an alcohol-based hand sanitizer to effectively clean your hands.
- Avoid close contact with sick individuals: Limit your exposure to individuals who are sick or have active infections.
- Practice good oral hygiene: Brush and floss your teeth regularly to maintain good oral health and prevent the risk of infections.
Vaccinations
Vaccinations are an essential preventive measure for individuals with thrombocytopenia. Here are some key vaccinations to consider:
- Influenza (Flu) Vaccine: Getting an annual flu vaccine is important to reduce the risk of developing influenza, which can lead to complications in individuals with thrombocytopenia.
- Pneumococcal Vaccines: Vaccination against pneumococcal bacteria can protect against pneumococcal infections, which can be severe for individuals with thrombocytopenia. Doctors may recommend different pneumococcal vaccines based on age and individual risk factors.
- Hepatitis B Vaccine: The hepatitis B vaccine is recommended for individuals with chronic liver disease or those at an increased risk of exposure to hepatitis B virus.
- Other Vaccinations: Depending on individual circumstances and medical history, doctors may recommend additional vaccinations such as tetanus, diphtheria, pertussis (Tdap), and others.
Preventing Bleeding
Taking steps to prevent bleeding can significantly reduce the risks associated with thrombocytopenia. Here are some measures to prevent bleeding:
- Handle sharp objects safely: Use caution while handling knives, scissors, razor blades, or other sharp objects. Always cut away from your body and keep blades covered when not in use.
- Shave with care: Use an electric razor instead of a traditional razor blade to minimize the risk of cuts and nicks.
- Avoid contact sports: Engage in low-impact or non-contact sports or activities to minimize the risk of serious injuries.
- Use a soft-bristled toothbrush: Brush your teeth gently using a soft-bristled toothbrush to prevent gum bleeding.
- Avoid certain medications: Avoid over-the-counter medications that can increase the risk of bleeding, such as nonsteroidal anti-inflammatory drugs (NSAIDs) or aspirin, unless otherwise instructed by your healthcare provider.
Medication Management
Proper management of medications is crucial for individuals with thrombocytopenia to avoid further complications. Here are some medication-related precautions:
- Follow prescribed medication regimen: Take all medications exactly as prescribed by your healthcare provider, including any platelet-stimulating medications or other treatments.
- Avoid medications that can worsen thrombocytopenia: Some medications, such as certain antibiotics or anticoagulants, can further decrease platelet counts. Inform your healthcare provider about your condition and any medications you are taking.
- Notify healthcare providers: Inform all healthcare providers, including dentists and specialists, about your thrombocytopenia and any medications you are taking.
- Be cautious with herbal supplements: Inform your healthcare provider about any herbal supplements or alternative therapies you are using, as some may have an impact on platelet function or count.
Knowing Emergency Procedures
In the event of bleeding or other medical emergencies, it is essential to be familiar with appropriate emergency procedures. Here are some guidelines to follow:
- Know when to seek immediate medical attention: Be aware of the symptoms and signs that require immediate medical attention, such as uncontrolled bleeding, severe bruising, or prolonged bleeding after minor injuries.
- Keep emergency contact information accessible: Have emergency contact numbers readily available so that you can quickly reach out for medical assistance if needed.
- Inform those around you: Make sure your family members, close friends, or coworkers are aware of your condition and know how to access emergency medical assistance.
Regular Medical Check-ups
Regular medical check-ups are crucial for individuals with thrombocytopenia to monitor their condition and receive appropriate care. Here are some key considerations:
- Schedule regular appointments with healthcare providers: Follow the recommended schedule for routine check-ups, and attend all appointments to monitor your platelet levels and overall health.
- Discuss your thrombocytopenia: Inform your healthcare provider about your thrombocytopenia and any changes or concerns you may have.
- Follow up on treatment plans: Adhere to the treatment plan prescribed by your healthcare provider, and inform them about any difficulties or side effects you may experience.
- Discuss potential risks: Inquire with your healthcare provider about potential risks associated with specific activities or medications, and seek their advice on risk management strategies.
Adhering to Treatment Plans
Compliance with prescribed treatment plans is essential for individuals with thrombocytopenia. Here are some recommendations for adhering to treatment plans:
- Take medications as prescribed: Strictly adhere to any medication regimens recommended by your healthcare provider.
- Follow dietary guidelines: If you have any dietary restrictions or recommendations due to your thrombocytopenia or an underlying health condition, ensure that you follow them.
- Attend all recommended therapies or treatments: If your treatment plan includes therapies such as platelet transfusions or specific treatments for an underlying condition, make sure to attend all scheduled sessions or appointments.
Awareness of Symptoms
Being aware of the symptoms associated with thrombocytopenia is crucial in managing the condition effectively. Here are some common symptoms to watch out for:
- Unusual or excessive bleeding: Pay attention to any signs of prolonged bleeding from minor cuts or injuries, frequent nosebleeds, or bleeding gums.
- Easy bruising: Take note if you develop bruises easily, especially without any significant trauma or injury.
- Petechiae or purpura: Watch for the appearance of small, reddish or purple spots on the skin, known as petechiae, or larger patches of purple bruise-like lesions called purpura.
- Fatigue or weakness: Be mindful of any unexplained fatigue or weakness that may be related to thrombocytopenia or an underlying health condition.
- Increased menstrual bleeding or heavy periods: If you are experiencing unusually heavy menstrual bleeding, it could be a possible symptom of thrombocytopenia.
Healthy Lifestyle Practices
Maintaining a healthy lifestyle is beneficial for overall health and can also help manage thrombocytopenia. Here are some healthy lifestyle practices to adopt:
- Balanced Diet: Consume a well-balanced diet that includes plenty of fruits, vegetables, whole grains, lean proteins, and healthy fats. This can help support optimal platelet production and overall health.
- Regular Exercise: Engage in regular physical activity as recommended by your healthcare provider. Exercise can improve blood circulation and overall cardiovascular health.
- Stress Management: Practice stress management techniques such as relaxation exercises, meditation, or engaging in activities you enjoy to reduce stress levels.
- Adequate Sleep: Aim for a consistent sleep schedule and ensure you are getting enough quality sleep each night to support overall health and well-being.
- Moderate Alcohol Consumption: If you consume alcohol, do so in moderation. Excessive alcohol intake can exacerbate thrombocytopenia and associated liver damage.
- Smoking Cessation: If you smoke, consider quitting as smoking can have detrimental effects on overall health, including blood clotting mechanisms.
- Avoidance of Recreational Drugs: Illicit drugs can have damaging effects on various systems in the body, including blood clotting and platelet function. Avoid recreational drug use.
- Maintaining a Healthy Weight: Maintain a healthy weight through a combination of regular physical activity and a balanced diet, as excess weight can contribute to numerous health issues.
By understanding the risk factors associated with thrombocytopenia and taking appropriate precautions, individuals can minimize the impact of this condition on their lives. It is crucial to work closely with healthcare providers to monitor platelet levels, receive appropriate treatment, and take steps to prevent complications. Maintaining an overall healthy lifestyle and adhering to treatment plans can go a long way in managing thrombocytopenia effectively.