In this article, you will discover essential nursing considerations for individuals diagnosed with congestive heart failure (CHF). As a nurse, understanding the unique needs and challenges that come with this condition is vital to providing proper care and support. From monitoring vital signs and fluid balance to administering medications and educating patients on lifestyle modifications, your role in managing CHF plays a crucial role in improving patient outcomes and enhancing their quality of life. Join us as we explore the important nursing considerations and interventions for individuals living with congestive heart failure.
Assessment
Physical assessment
During a physical assessment, the nurse will thoroughly examine the patient’s body, paying close attention to the signs and symptoms of congestive heart failure (CHF). This includes assessing peripheral edema, auscultating the heart for abnormal heart sounds like S3 and S4, and inspecting the skin for signs of cyanosis or pallor. Additionally, the nurse will assess the patient’s blood pressure, heart rate, and respiratory rate, as these vital signs provide essential information about the patient’s cardiovascular and respiratory status.
Cardiovascular assessment
The cardiovascular assessment focuses on evaluating the patient’s heart and circulatory system. The nurse will listen to the patient’s heart sounds using a stethoscope, paying attention to any irregularities or murmurs. They will also assess the patient’s blood pressure, checking for any signs of hypertension or hypotension. Additionally, the nurse will assess the patient’s peripheral pulses and capillary refill time, as these can indicate poor circulation.
Respiratory assessment
In a respiratory assessment, the nurse will evaluate the patient’s breathing and lung function. They will assess the patient’s respiratory rate, rhythm, and effort, noting any signs of dyspnea or orthopnea. The nurse will also auscultate the patient’s lungs, listening for crackles or wheezes, which can indicate fluid accumulation in the lungs. This assessment is crucial in detecting any respiratory complications or worsening of the patient’s condition.
Fluid status assessment
Assessing the patient’s fluid status allows the nurse to monitor for fluid overload or dehydration, both of which can have severe consequences for patients with congestive heart failure. The nurse will measure and record the patient’s intake and output, closely monitoring for any imbalances. They will also assess the patient’s weight regularly, as sudden weight gain can imply fluid retention. By carefully assessing the patient’s fluid status, the nurse can promptly intervene and adjust the treatment plan as needed.
Psychosocial assessment
A psychosocial assessment focuses on evaluating the patient’s emotional and mental well-being. Patients with congestive heart failure may experience anxiety, depression, or feelings of hopelessness. The nurse will take the time to communicate with the patient, assessing their emotional state and providing emotional support. They will also assess the patient’s support systems and identify any additional psychosocial needs that require attention, such as referral to support groups or counseling services.
Diagnostic tests
Chest X-ray
A chest X-ray is a common diagnostic test used to assess the heart and lungs of patients with congestive heart failure. It helps identify any structural abnormalities, such as an enlarged heart or fluid buildup in the lungs. The nurse will collaborate with the healthcare team to ensure that the patient undergoes the chest X-ray as ordered and will monitor the results to determine the appropriate interventions.
Electrocardiogram (ECG)
An electrocardiogram (ECG) measures the electrical activity of the heart and helps detect any irregularities in the heart rhythm. Patients with congestive heart failure often have arrhythmias, such as atrial fibrillation or ventricular tachycardia. The nurse will assist in the placement of the ECG electrodes and observe the ECG tracing for any abnormalities. They will report any concerning findings to the healthcare team promptly.
Echocardiogram
An echocardiogram is a non-invasive test that uses sound waves to create images of the heart. It allows healthcare providers to assess the structure and function of the heart, including the thickness of the heart’s walls, the pumping ability of the heart, and the function of the heart valves. The nurse will ensure that the patient understands the purpose and process of the echocardiogram, providing support and reassurance throughout the procedure.
Cardiac catheterization
Cardiac catheterization is an invasive procedure that involves threading a thin tube (catheter) through blood vessels to the heart. It provides detailed information about the heart’s blood flow, pressures, and oxygen levels. The nurse will prepare the patient for the procedure, ensuring that they understand the risks and benefits. They will monitor the patient closely during and after the procedure, documenting any changes in vital signs or complications.
Laboratory tests
Laboratory tests play a crucial role in assessing and managing congestive heart failure. The nurse will collect blood samples to measure various parameters, including electrolyte levels, renal function, liver function, and cardiac biomarkers. These tests help evaluate the patient’s overall health, monitor the effects of medications, and detect any complications or worsening of the condition. The nurse will ensure samples are collected timely, accurately, and report the results to the healthcare team for appropriate intervention.

Medication management
Diuretics
Diuretics are medications commonly prescribed to patients with congestive heart failure to reduce excess fluid in the body through increased urine output. The nurse will monitor the patient’s fluid status closely, assessing intake and output and evaluating the response to diuretic therapy. They will educate the patient about the importance of taking the medication as prescribed and discuss potential side effects such as electrolyte imbalances or dehydration.
Angiotensin-converting enzyme (ACE) inhibitors
ACE inhibitors are medications that help dilate blood vessels, reduce blood pressure, and decrease the workload on the heart. The nurse will assess the patient’s blood pressure before and after administering ACE inhibitors, ensuring that it remains within a safe and therapeutic range. They will also monitor for any signs of allergic reactions or adverse effects, such as persistent cough or angioedema.
Beta blockers
Beta blockers are medications that slow down the heart rate and reduce blood pressure, helping to improve the heart’s efficiency. The nurse will closely monitor the patient’s vital signs, including heart rate, blood pressure, and respiratory rate, before and after administering beta blockers. They will assess for any signs of bradycardia or hypotension and educate the patient about the importance of regular medication intake.
Aldosterone antagonists
Aldosterone antagonists are medications that help reduce fluid retention and decrease the workload on the heart. The nurse will monitor the patient’s electrolyte levels, particularly potassium, as aldosterone antagonists can cause hyperkalemia. They will educate the patient about dietary restrictions and signs of electrolyte imbalances, emphasizing the importance of regular laboratory tests.
Digitalis glycosides
Digitalis glycosides, such as digoxin, are medications that help strengthen the heart’s contractions and regulate the heart rate. The nurse will closely monitor the patient’s heart rate and rhythm, documenting any changes or abnormalities. They will assess for signs of digitalis toxicity, such as nausea, vomiting, or visual disturbances, and educate the patient about the importance of regular medication intake.
Vasodilators
Vasodilators are medications that help dilate blood vessels, reducing the workload on the heart and improving blood flow. The nurse will closely monitor the patient’s blood pressure, heart rate, and respiratory rate before and after administering vasodilators. They will assess for any signs of hypotension or reflex tachycardia, educating the patient about potential side effects and signs to report.
Fluid and diet management
Monitoring fluid intake and output
The nurse will closely monitor the patient’s fluid intake and output to maintain a balance and prevent fluid overload or dehydration. They will measure and document the volume of fluids the patient consumes and excretes, including urine output, vomit, and wound drainage. By accurately monitoring fluid intake and output, the nurse can identify any imbalances and adjust the treatment plan accordingly.
Restricting sodium intake
Sodium restriction is an essential component of managing congestive heart failure. The nurse will educate the patient about the importance of limiting sodium intake and provide guidance on reading food labels and selecting low-sodium options. They will work closely with the dietitian to develop a customized meal plan that meets the patient’s nutritional needs while adhering to sodium restrictions.
Adjusting fluid restriction
Fluid restriction may be necessary for patients with congestive heart failure to prevent fluid overload. The nurse will work closely with the healthcare team to determine the appropriate fluid restriction for the patient and educate them about its importance. They will monitor the patient’s fluid status regularly, adjusting the restriction as needed based on the patient’s clinical condition and response to treatment.
Monitoring daily weights
Daily weight monitoring is crucial in managing congestive heart failure as it helps detect fluid retention or loss. The nurse will instruct the patient to weigh themselves daily, preferably in the morning and wearing similar clothing. They will provide clear instructions on how to use the scale accurately and teach the patient how to interpret weight changes, emphasizing the importance of reporting any significant fluctuations promptly.
Educating patients on fluid and diet management
The nurse plays a pivotal role in educating patients about fluid and diet management in congestive heart failure. They will provide comprehensive education about sodium restriction, fluid intake and output monitoring, and the significance of maintaining a healthy weight. The nurse will teach the patient how to identify hidden sources of sodium in their diet, encourage them to drink fluids in moderation, and promote adherence to the prescribed treatment plan.
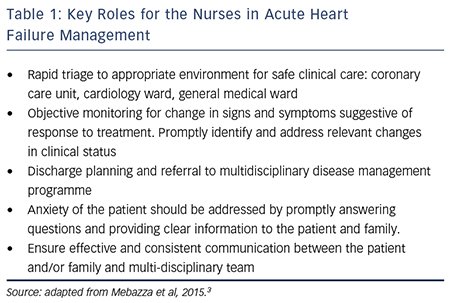

Activity and rest considerations
Monitoring activity tolerance
The nurse will assess the patient’s ability to engage in physical activity and monitor their tolerance. They will carefully observe for any signs of fatigue, shortness of breath, or chest pain during activity. By monitoring activity tolerance, the nurse can adjust the patient’s activity level and make appropriate recommendations to prevent exacerbations and promote optimal health.
Encouraging appropriate exercise
Regular exercise can be beneficial for patients with congestive heart failure when done under proper guidance. The nurse will educate the patient about the importance of exercise and encourage them to engage in appropriate activities, such as walking or low-impact exercises. They will work closely with the physical and occupational therapists to develop an individualized exercise plan that suits the patient’s needs, abilities, and limitations.
Providing rest periods
Rest is vital for patients with congestive heart failure to conserve energy and prevent excessive strain on the heart. The nurse will ensure that the patient receives adequate rest periods throughout the day, scheduling activities and interventions accordingly. They will emphasize the importance of balancing physical activity with rest and teach the patient relaxation techniques to promote overall well-being.
Safety precautions during activities
To prevent falls and injuries, the nurse will implement safety precautions during activities. They will ensure that the environment is free from hazards, such as loose rugs or cluttered spaces, and provide assistive devices, if necessary, for mobility support. The nurse will educate the patient and their family members about fall prevention strategies, emphasizing the importance of maintaining a safe and secure environment.
Promoting sleep and relaxation
Adequate sleep and relaxation are essential for patients with congestive heart failure to restore energy and support overall well-being. The nurse will assess the patient’s sleep patterns and provide recommendations for facilitating a good night’s sleep. They will teach relaxation techniques, such as deep breathing or guided imagery, to help the patient manage stress and promote a sense of calm.
Oxygen therapy
Assessing oxygen saturation
Oxygen saturation levels indicate the amount of oxygen in the blood. The nurse will assess the patient’s oxygen saturation using a pulse oximeter, ensuring that it remains within a safe range. They will monitor the patient’s respiratory status regularly, including respiratory rate and effort, to detect any signs of respiratory distress or hypoxia.
Administering supplemental oxygen
Supplemental oxygen therapy may be necessary for patients with congestive heart failure who have low oxygen levels. The nurse, in collaboration with the healthcare team, will administer supplemental oxygen as prescribed, closely monitoring the patient’s response. They will ensure the proper placement of the oxygen delivery device, provide education on its use, and guide the patient in maintaining appropriate oxygen flow.
Assessing response to oxygen therapy
The nurse will continuously assess the patient’s response to oxygen therapy, observing for any improvement in oxygen saturation and respiratory status. They will communicate any changes or concerns to the healthcare team promptly and collaborate in adjusting the oxygen therapy plan as necessary.
Monitoring for oxygen toxicity
High levels of supplemental oxygen can potentially lead to oxygen toxicity, causing damage to the lungs or other organs. The nurse will closely monitor the patient for signs and symptoms of oxygen toxicity, such as chest pain, coughing, or difficulty breathing. By monitoring for oxygen toxicity, the nurse can promptly intervene and ensure the patient’s safety.

Psychosocial support
Assessing emotional well-being
The nurse will assess the patient’s emotional well-being, recognizing that congestive heart failure can be emotionally distressing. They will create a supportive and empathetic environment, allowing the patient to express their feelings and concerns. The nurse will actively listen, validate the patient’s emotions, and offer appropriate resources or referrals for additional support.
Managing anxiety and depression
Patients with congestive heart failure may experience anxiety or depression due to the impact of the condition on their daily lives. The nurse will employ various strategies to help manage anxiety and depression, including therapeutic communication, relaxation techniques, and providing information and education. They will collaborate with the healthcare team to determine if additional interventions, such as therapy or medications, are necessary.
Educating patients and families
Education is a crucial aspect of psychosocial support. The nurse will provide comprehensive education to patients and their families about congestive heart failure, its management, and the importance of adherence to the treatment plan. They will ensure that the information is presented in a clear and understandable manner, addressing any questions or concerns the patient or family may have.
Referring to support groups or counseling services
Support groups and counseling services can provide valuable emotional support and guidance for patients with congestive heart failure. The nurse will assess the patient’s need for additional psychosocial support and refer them to appropriate resources. They will provide information about local support groups, counseling services, or online communities where the patient can connect with others facing similar challenges.
Promoting positive coping strategies
The nurse will promote positive coping strategies to help patients and their families navigate the challenges associated with congestive heart failure. They will encourage the patient to engage in activities that bring joy and fulfillment, provide emotional support, and teach stress management techniques. By promoting positive coping strategies, the nurse can enhance the patient’s overall well-being and quality of life.
Patient education
Teaching about disease process
Patient education plays a significant role in managing congestive heart failure. The nurse will educate the patient about the underlying disease process, explaining how the heart’s function is affected and the implications for overall health. They will use appropriate teaching materials and techniques to ensure the patient’s understanding, empowering them to actively participate in their own care.
Explaining medication regimen
Understanding the medication regimen is essential for patients with congestive heart failure. The nurse will explain each prescribed medication, including its purpose, dosage, potential side effects, and the importance of adherence. They will teach the patient how to take medications correctly, including any specific instructions, such as taking medications with food or at certain times of the day.
Highlighting signs and symptoms of worsening condition
Recognizing the signs and symptoms of worsening congestive heart failure is crucial for timely intervention. The nurse will educate the patient about the red flags to watch out for, such as increased shortness of breath, sudden weight gain, or chest pain. They will emphasize the importance of alerting the healthcare team promptly to prevent complications and ensure appropriate management.
Demonstrating self-care techniques
Self-care techniques can empower patients to manage their congestive heart failure effectively. The nurse will demonstrate various self-care techniques, such as monitoring blood pressure at home, performing daily weights correctly, or using relaxation techniques. They will provide hands-on guidance and ensure that the patient feels confident in performing these techniques independently.
Providing resources for further information
To facilitate ongoing education and support, the nurse will provide patients with congestive heart failure with additional resources for further information. This may include reputable websites, pamphlets, or other educational materials. The nurse will encourage the patient to ask questions, seek reliable information, and discuss any concerns with the healthcare team.

Monitoring and documentation
Monitoring vital signs
Regular monitoring of vital signs is essential for patients with congestive heart failure. The nurse will measure and document the patient’s blood pressure, heart rate, respiratory rate, and oxygen saturation at regular intervals. They will pay close attention to any significant changes or fluctuations, promptly reporting them to the healthcare team for appropriate interventions.
Documenting intake and output
Accurate documentation of the patient’s fluid intake and output is crucial for managing congestive heart failure. The nurse will carefully record the volume of fluids the patient consumes and excretes, including urine output, vomit, and wound drainage. They will document these values at specific intervals, allowing for effective assessment and identification of any imbalances.
Recording daily weights
Daily weight monitoring is a fundamental tool for managing congestive heart failure. The nurse will meticulously document the patient’s daily weights, ensuring consistency in measuring techniques and timing. They will record the values accurately, including any significant increases or decreases, and report them to the healthcare team promptly.
Assessing laboratory values
Laboratory values provide valuable information about the patient’s overall health and response to treatment. The nurse will assess the patient’s laboratory values, including electrolyte levels, renal function, liver function, and cardiac biomarkers. They will monitor changes in these values, interpreting and documenting them correctly to aid in guiding the patient’s care.
Reporting and documenting changes in condition
The nurse plays a critical role in identifying and reporting any changes in the patient’s condition promptly. They will document all observed changes, including worsening symptoms, side effects of medications, or any concerns raised by the patient or their family members. By providing accurate and timely documentation, the nurse ensures effective communication and coordination of care.
Collaboration with interdisciplinary team
Communicating with physicians
Effective communication between nurses and physicians is essential for managing congestive heart failure. The nurse will collaborate closely with the physician, reporting any changes in the patient’s condition, vital signs, or laboratory values. They will provide updates on the patient’s response to treatment and seek clarification or guidance when necessary.
Working with pharmacists
Pharmacists play a vital role in medication management for patients with congestive heart failure. The nurse will collaborate with the pharmacist, seeking their expertise in drug interactions, dosage adjustments, or potential side effects. They will ensure that the patient’s medication regimen aligns with current guidelines and recommendations, promoting safe and effective care.
Collaborating with social workers
Social workers can provide valuable support and resources to patients with congestive heart failure. The nurse will collaborate with social workers to address any psychosocial needs or challenges faced by the patient and their family. They will ensure that appropriate referrals or interventions are made, aiming to optimize the patient’s overall well-being.
Consulting with dietitians
Dietitians play a crucial role in managing the dietary needs of patients with congestive heart failure. The nurse will collaborate with dietitians to develop a customized meal plan that meets the patient’s nutritional needs while adhering to sodium restrictions. They will communicate any specific dietary requirements or adjustments promptly, ensuring a well-rounded and balanced approach to nutritional care.
Coordinating with physical and occupational therapists
Physical and occupational therapists play an essential role in promoting optimal mobility and independence for patients with congestive heart failure. The nurse will collaborate closely with the therapists to establish appropriate goals and interventions, working together to maximize the patient’s functional abilities and ensure a safe and supportive environment.
In conclusion, nurses play a vital role in the comprehensive management of patients with congestive heart failure. Through thorough assessment, effective communication, patient education, and collaboration with the interdisciplinary team, nurses can provide the necessary support and care to help patients manage their condition and improve their quality of life. By addressing the physical, psychosocial, and educational needs of patients, nurses contribute significantly to the successful management of congestive heart failure.