If you or a loved one is dealing with an enlarged prostate, it’s important to understand the nursing considerations and management that come with it. In this article, we’ll explore the key factors that nurses should keep in mind when caring for patients with an enlarged prostate. From understanding the symptoms and complications to providing effective pain management and promoting patient education, nurses play a crucial role in supporting those with this condition. So, whether you’re a nurse looking to enhance your knowledge or someone seeking information about caring for a loved one, this article will provide valuable insights into the important nursing considerations for enlarged prostate.

Assessment
Medical history
When assessing a patient with an enlarged prostate, obtaining a thorough medical history is crucial. This includes asking about any previous urological conditions, surgeries, or treatments. It is important to inquire about the patient’s current symptoms, such as urinary hesitancy, frequency, urgency, and nocturia. Additionally, documenting any underlying medical conditions, medications, allergies, and family history of prostate issues will provide valuable information for the overall assessment and management of the patient’s condition.
Physical assessment
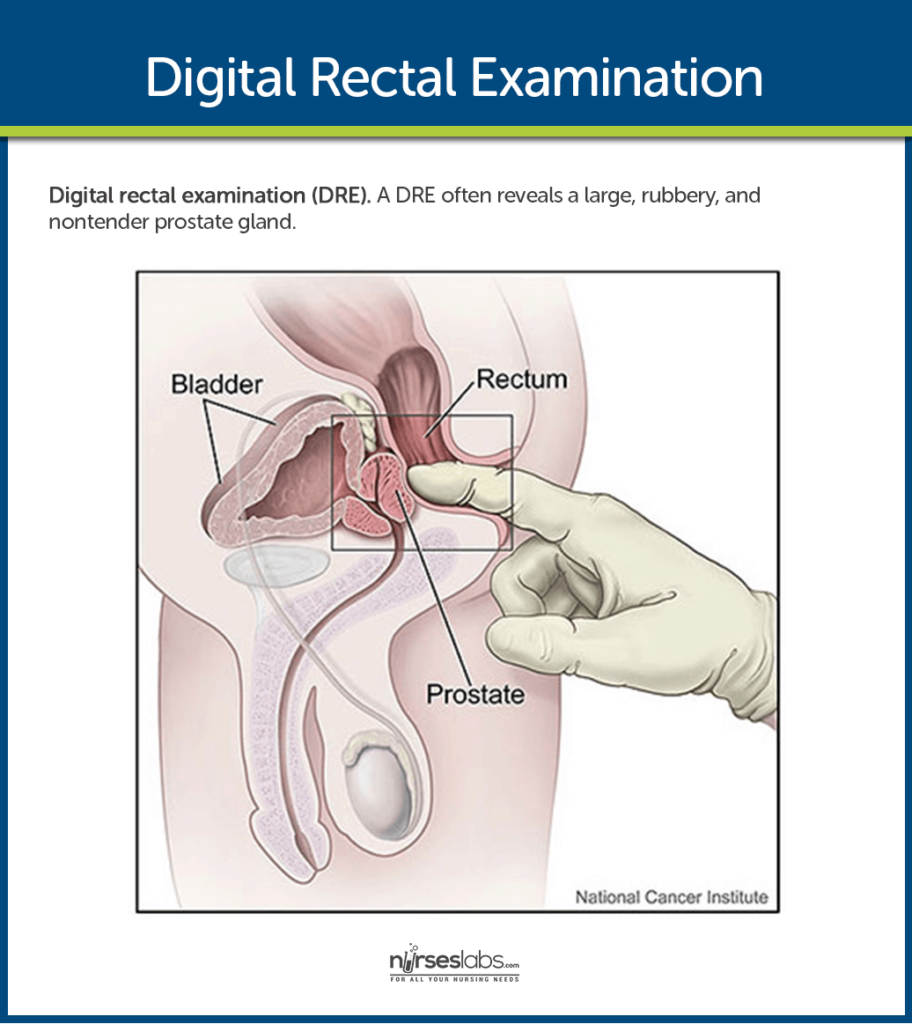
A comprehensive physical assessment should be conducted to evaluate the patient’s prostate health. This includes performing a digital rectal examination (DRE), in which the healthcare provider palpates the prostate gland to assess its size, shape, and consistency. The DRE allows for the detection of any abnormalities or signs of prostate cancer. Additionally, vital signs should be monitored, and a general physical examination should be conducted to assess for any other potential health issues.
Urological assessment
In addition to the medical history and physical assessment, a urological assessment is essential in evaluating the patient’s urinary function. This assessment typically involves measuring the patient’s urine output, assessing the characteristic of urine, and identifying any signs of infection or complications. Uroflowmetry, a test that measures the rate and volume of urine flow, may also be performed to further evaluate the patient’s urinary function and identify any obstruction in the urinary tract. Other diagnostic tests, such as a cystoscopy or transrectal ultrasound, may be ordered by the urologist to gather more detailed information about the patient’s condition.
Diagnostic Tests
Prostate-specific antigen (PSA) test
The PSA test measures the levels of a protein called prostate-specific antigen in the patient’s blood. Elevated PSA levels can indicate prostate inflammation, infection, or cancer. It is important to inform the patient that an elevated PSA level does not necessarily mean they have prostate cancer and that further diagnostic tests and evaluation are necessary for a definitive diagnosis.
Digital rectal examination (DRE)
The DRE is a physical examination in which the healthcare provider inserts a gloved, lubricated finger into the patient’s rectum to assess the prostate gland. This examination allows for the detection of any abnormalities, such as enlargement, nodules, or irregularities in the prostate gland. It is essential to educate the patient about the DRE procedure, ensuring they understand its significance in diagnosing and monitoring their condition.
Transrectal ultrasound
A transrectal ultrasound involves the use of a probe inserted into the rectum to create images of the prostate gland. This diagnostic test helps evaluate the size, shape, and structure of the prostate. It is commonly used to assist in guiding other procedures, such as biopsy or prostatectomy, and provides valuable information for treatment planning and monitoring.
Urinalysis
Urinalysis involves the examination of the patient’s urine sample for the presence of red and white blood cells, bacteria, and other abnormalities. This test helps identify urinary tract infections and provides additional information about the patient’s kidney function. Educating the patient about the importance of providing a clean catch urine sample and explaining the purpose of the urinalysis will ensure accurate results and promote their understanding of the diagnostic process.
Uroflowmetry
Uroflowmetry measures the rate and volume of urine flow during urination. This non-invasive test is performed by having the patient urinate into a special uroflowmeter device. Uroflowmetry helps evaluate the strength of the patient’s urinary stream and identify potential obstructions in the urethra. It is important to instruct the patient on the correct technique for uroflowmetry to obtain accurate results.
Cystoscopy
Cystoscopy is a procedure that involves the insertion of a thin tube with a camera into the urethra and bladder to visualize the urinary tract. This procedure allows for a direct examination of the bladder and urethra, helping identify any abnormalities, such as bladder stones or tumors. The patient should be educated about the potential discomfort and minimal risks associated with cystoscopy to alleviate any anxieties they may have.

Symptom Management
Education about the condition
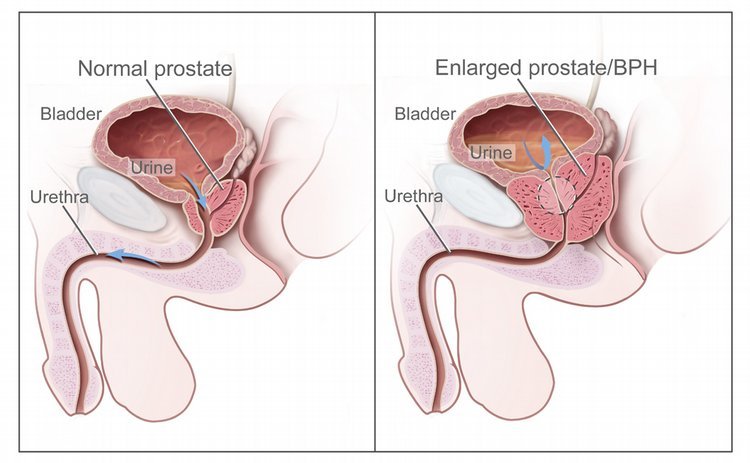
Providing education to patients about their enlarged prostate condition is essential for self-management and adherence to treatment plans. Patients should be educated about the anatomy and function of the prostate, the causes of prostate enlargement, and the potential complications associated with the condition. It is important to explain the treatment options available, including lifestyle modifications, medication, and surgical interventions, and facilitate shared decision-making with the patient.
Fluid management
Encouraging patients to maintain an adequate fluid intake is important in managing their symptoms. Drinking plenty of water helps flush out the bladder and reduces the risk of urinary tract infections. However, patients should also be educated about avoiding excessive fluid intake before bedtime to minimize nocturia.
Pharmacological interventions
Medications are often prescribed to manage the symptoms of an enlarged prostate. Alpha-blockers, such as tamsulosin, help relax the muscles in the prostate and bladder neck, improving urinary flow. 5-alpha-reductase inhibitors, like finasteride, can reduce the size of the prostate gland over time. Anticholinergic drugs, such as oxybutynin, may be used to alleviate symptoms like urgency and frequency. It is crucial to educate patients about the purpose, potential side effects, and proper administration of these medications.
Catheterization
In some cases, catheterization may be necessary to help manage urinary retention or incontinence associated with an enlarged prostate. Educating patients about the different types of catheters, such as intermittent catheters or indwelling catheters, and demonstrating proper catheter insertion and care techniques will empower them to manage their catheterization effectively.
Bladder training
Bladder training involves helping patients regain control over their bladder and improve their urinary urgency and frequency. This can be achieved by gradually increasing the time intervals between urination, practicing relaxation techniques, and utilizing distraction techniques when experiencing the urge to urinate. Providing information and teaching patients about bladder training techniques can significantly improve their urinary symptoms and quality of life.
Pelvic floor exercises
Pelvic floor exercises, also known as Kegel exercises, are beneficial in strengthening the muscles that support the bladder and urethra. These exercises involve contracting and relaxing the pelvic floor muscles to enhance urinary control. Teaching patients how to correctly perform pelvic floor exercises and encouraging regular practice can help improve their bladder function and reduce urinary symptoms.
Nutrition counseling
Providing nutrition counseling to patients with an enlarged prostate can contribute to overall symptom management. Encouraging a healthy and balanced diet, rich in fruits, vegetables, whole grains, and lean proteins, is important for maintaining prostate health. Educating patients about foods or beverages that may aggravate their symptoms, such as caffeine or alcohol, and discussing dietary modifications to alleviate symptoms can be beneficial.
Medication Administration
Alpha-blockers
Alpha-blockers are a class of medications commonly used to relax the smooth muscles in the prostate and bladder neck, improving urinary flow. They work by blocking the alpha-adrenergic receptors. Examples of alpha-blockers include tamsulosin, alfuzosin, doxazosin, and terazosin. It is important to educate patients about the proper administration, potential side effects, and the importance of regular medication compliance when using alpha-blockers for symptom management.
5-alpha-reductase inhibitors
5-alpha-reductase inhibitors, such as finasteride and dutasteride, are medications that help reduce the size of the prostate gland over time by inhibiting the production of dihydrotestosterone (DHT). These medications are typically used in patients with significant prostate enlargement. Patients should be informed about the potential benefits, side effects, and duration of treatment associated with 5-alpha-reductase inhibitors.
Anticholinergic drugs
Anticholinergic drugs, such as oxybutynin, tolterodine, and solifenacin, can be used to alleviate bladder spasms and reduce urinary urgency and frequency. These medications work by blocking the action of acetylcholine on the bladder muscles. Patients need to be educated about the potential side effects, such as dry mouth or constipation, and the importance of regular medication use for symptom relief.
Pain medication
In some cases, patients may experience pain or discomfort associated with an enlarged prostate. Pain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs) or acetaminophen, can be used to alleviate these symptoms. However, caution should be exercised when administering pain medication, considering the patient’s medical history and any contraindications or potential drug interactions.

Patient Education
Understanding the condition and treatment options
Educating patients about their enlarged prostate condition and the available treatment options is crucial in promoting their active participation in decision-making and self-management. Patients should be provided with clear and concise information about the causes, risk factors, and potential complications of an enlarged prostate. Additionally, they need to be informed about the available treatment options, including lifestyle modifications, medication, and surgical interventions, along with the potential benefits and risks associated with each treatment modality.
Monitoring for complications
Patients need to be educated about the potential complications of an enlarged prostate and the importance of regular monitoring. They should be informed about the signs and symptoms of complications, such as urinary retention, urinary tract infections, or bladder stones. Patients should be encouraged to seek immediate medical attention if they experience any unusual or worsening symptoms.
Lifestyle modifications
Implementing lifestyle modifications can be beneficial in managing the symptoms of an enlarged prostate. Patients should be educated about the importance of maintaining a healthy diet, avoiding excessive fluid intake before bedtime, limiting caffeine and alcohol consumption, and practicing regular physical exercise. Additionally, educating patients about the potential effects of tobacco use and providing resources for smoking cessation can contribute to their overall health and well-being.
Follow-up care
Regular follow-up care is essential in monitoring the patient’s prostate health and ensuring the effectiveness of the chosen treatment plan. Patients should be informed about the recommended follow-up schedule and the importance of attending scheduled appointments. Monitoring the patient’s symptoms, conducting necessary diagnostic tests, and adjusting the treatment plan based on their response will promote optimal outcomes and disease management.
Signs of exacerbation
Educating patients about the signs and symptoms of an exacerbation of their enlarged prostate condition is essential in promoting early intervention and preventing complications. Patients should be informed about the warning signs, such as severe urinary retention, hematuria, fever, or worsening urinary symptoms. Instructing patients to seek immediate medical attention if they experience any of these symptoms will help ensure timely management and prevent further deterioration of their condition.
Catheter Care
Maintaining catheter patency
Proper catheter care is essential in preventing complications and maintaining catheter patency. Patients with indwelling catheters should be educated about the importance of maintaining a sterile urine collection system and adhering to a regular catheter irrigation and flushing schedule as advised by their healthcare provider. Additionally, they should be instructed on how to properly secure and clean the catheter insertion site to minimize the risk of infection.
Prevention of infection
Infection prevention is vital for patients with catheters, as they are at an increased risk of developing urinary tract infections. Patients should be educated on the importance of maintaining good hygiene, including regular handwashing, and proper cleaning and care of their catheter and collection bag. They should also be instructed to monitor for signs of infection, such as bladder spasms, cloudy or foul-smelling urine, or fever, and seek medical attention if these symptoms arise.
Monitoring for catheter-related complications
Patients with catheters should be educated about potential complications associated with catheter use and instructed on how to monitor for them. These complications may include urinary tract infections, blockages, bladder spasms, or leakage around the catheter. Patients should be encouraged to report any unusual symptoms or concerns promptly to their healthcare provider for further evaluation and management.
Surgical Interventions
Transurethral resection of the prostate (TURP)
Transurethral resection of the prostate (TURP) is a surgical procedure commonly performed to alleviate urinary obstruction caused by an enlarged prostate. In this procedure, the excess prostate tissue is removed using a specialized instrument inserted through the urethra. Patients should be educated about the TURP procedure, including the preparation required, the potential risks and benefits, and the post-operative care involved.
Laser surgery
Laser surgery, such as photoselective vaporization of the prostate (PVP) or holmium laser enucleation of the prostate (HoLEP), is an alternative surgical option for patients with an enlarged prostate. Laser surgery utilizes laser energy to destroy or remove the excess prostate tissue, relieving the urinary obstruction. Patients should be educated about the different laser surgery techniques available, their potential benefits, and the expected recovery and post-operative care involved.
Prostatectomy
Prostatectomy involves the complete removal of the prostate gland and is typically reserved for patients with severe prostate enlargement or prostate cancer. Depending on the extent of the procedure, a prostatectomy can be performed using open surgery, laparoscopy, or robotic-assisted techniques. Patients should be provided with detailed information about prostatectomy, including the potential risks and benefits, the expected recovery period, and the post-operative care required.
Post-operative Care
Pain management
Post-operative pain management is essential for patients who have undergone surgical interventions for an enlarged prostate. Adequate pain relief ensures the patient’s comfort and promotes early mobilization. Patients should be educated about the prescribed analgesics and the appropriate administration schedule. It is important to assess their pain levels regularly and adjust the pain management plan accordingly.
Monitoring for complications
Following surgical interventions, patients should be closely monitored for potential complications, such as hemorrhage, infection, or urinary retention. Monitoring vital signs, assessing the surgical site for signs of infection or bleeding, and evaluating urinary output are crucial in identifying any post-operative complications. Patients should be educated about the warning signs of complications and instructed to seek immediate medical attention if they experience any of these symptoms.
Bladder training
After surgical interventions, patients may need to relearn and regain control of their bladder function. Bladder training techniques, similar to those described earlier, can be beneficial in helping patients adjust to any changes in urinary function and improve their continence. Educating patients about the importance of bladder training, providing detailed instructions, and offering ongoing support will promote their successful post-operative recovery.
Self-care instructions
Patients should receive comprehensive self-care instructions to promote optimal post-operative recovery and minimize complications. These instructions may include wound care, catheter care if applicable, medication administration and management, diet and activity restrictions, and information about when to resume normal activities or return to work. Providing clear and written instructions will help ensure that patients have the necessary knowledge and tools to care for themselves after surgery.
Psychosocial Support
Emotional support
Diagnosing and managing an enlarged prostate can have a significant emotional impact on patients. It is essential to provide emotional support, empathy, and reassurance throughout their healthcare journey. Active listening, validating their concerns, and addressing their fears and anxieties can help alleviate emotional distress and promote a sense of well-being.
Counseling
Counseling can be beneficial for patients who are experiencing significant emotional or psychological stress related to their enlarged prostate condition. Referring patients to a mental health professional, such as a counselor or therapist, can provide them with a safe and supportive space to discuss their feelings, cope with any emotional challenges, and develop strategies for managing stress.
Support groups
Connecting patients with support groups or peer-to-peer networks can be invaluable in providing them with a sense of community, encouragement, and understanding. Support groups allow patients to share their experiences, learn from others, and gain new perspectives. Encouraging patients to participate in support groups tailored to prostate health can help them navigate their condition with increased knowledge and support.
Collaboration with Interdisciplinary Team
Consulting with urologist
Collaboration with a urologist is essential in the assessment, diagnosis, and management of patients with an enlarged prostate. Consulting and seeking guidance from the urologist can help validate nursing assessments, receive expert recommendations for treatment, and establish an effective care plan. Maintaining open lines of communication, sharing relevant information, and actively involving the urologist in the patient’s care will contribute to a collaborative and comprehensive approach to their management.
Collaboration with pharmacist
Collaborating with a pharmacist can greatly aid in providing optimal medication management for patients with an enlarged prostate. Pharmacist consultation can help ensure accurate dosage calculations, identify potential drug interactions or contraindications, and provide valuable information about medication side effects or administration. Regular communication with the pharmacist allows for medication reconciliation, adherence monitoring, and adjustments to the patient’s pharmacological regimens as needed.
Collaboration with dietitian
Incorporating a dietitian into the interdisciplinary team can offer significant benefits for patients with an enlarged prostate. Dietitians can provide individualized nutrition counseling, supporting patients in making healthy dietary choices that promote prostate health. Collaboration with a dietitian allows for the identification of specific dietary modifications that may help manage symptoms or minimize complications associated with an enlarged prostate.
Referral to physical therapist
Referring patients to a physical therapist can contribute to their overall management and recovery from an enlarged prostate. Physical therapists can provide specialized interventions, such as pelvic floor muscle training, to help patients improve their urinary control and bladder function. Collaboration with a physical therapist ensures that patients receive comprehensive care that addresses both the physical and functional aspects of their condition.
In conclusion, nursing considerations for patients with an enlarged prostate encompass a range of assessments, diagnostic tests, symptom management strategies, medication administration, patient education, post-operative care, psychosocial support, and collaboration with the interdisciplinary team. By addressing these various aspects, healthcare providers can ensure comprehensive and individualized care that promotes the well-being and quality of life for patients with an enlarged prostate.