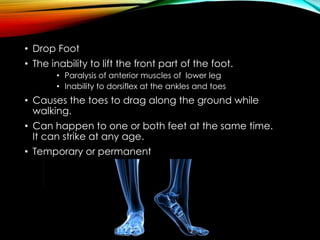
Are you a nurse looking for important information on how to provide the best care for patients with foot drop? Look no further! This article will provide you with nursing considerations and management strategies that can help improve the quality of life for individuals with foot drop. From understanding the causes and symptoms of foot drop to learning about effective interventions and assistive devices, this comprehensive guide will equip you with the knowledge and skills needed to support your patients throughout their recovery journey. So, grab a cup of coffee, sit back, and let’s dive into the world of nursing considerations for patients with foot drop!
Assessment
Patient history
When assessing a patient with foot drop, it is important to gather a thorough patient history. This includes information about the onset and progression of the condition, any underlying medical conditions that may contribute to foot drop, and any previous treatments or interventions. Additionally, it is crucial to inquire about the patient’s functional limitations and how foot drop impacts their daily activities.
Physical examination
A comprehensive physical examination is vital in assessing foot drop. The nurse should observe the patient’s gait, noting any abnormal movements or compensatory strategies. The strength and sensation of the affected leg should be evaluated, along with range of motion of the ankle and foot. It is also important to assess for any muscle atrophy or contractures that may have developed as a result of foot drop.
Gait analysis
Analyzing the patient’s gait is an essential component of the assessment process. The nurse should observe how the patient walks, paying attention to their stride length, foot clearance, and foot placement. This can provide valuable information about the severity of the foot drop and any compensatory mechanisms the patient may be using. Gait analysis can help guide treatment plans and assist in monitoring progress over time.
Etiology
Neurological causes
Foot drop can be caused by various neurological conditions, such as nerve injuries or compression, spinal cord lesions, or central nervous system disorders. These conditions can affect the functioning of the muscles responsible for ankle and foot movement. It is important for nurses to be aware of these underlying neurological causes and collaborate with other healthcare professionals to address them properly.
Muscular causes
Muscular causes of foot drop may include muscle weakness or paralysis in the muscles responsible for lifting the foot. This can be due to conditions such as muscular dystrophy, peripheral neuropathy, or muscle imbalances. Understanding the muscular causes of foot drop is essential for designing an effective treatment plan that focuses on strengthening and rehabilitating the affected muscles.
Mechanical causes
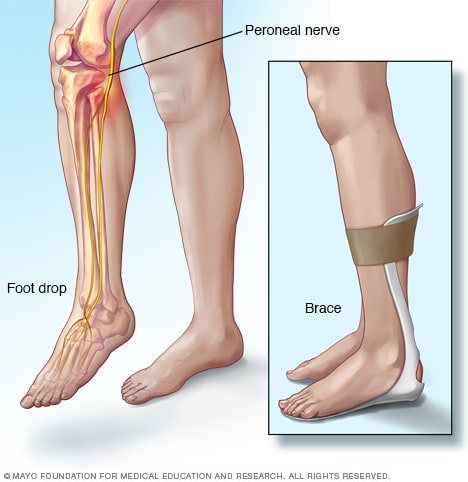
Mechanical causes of foot drop often result from trauma or injury to the muscles, tendons, or bones in the leg or foot. This can include fractures, ligament tears, or damage to the peroneal nerve. Identifying and addressing the mechanical causes of foot drop may involve surgical interventions or the use of orthotic devices to provide stability and support.
Complications
Muscle atrophy
Muscle atrophy can occur as a result of foot drop, especially if the condition is long-standing or left untreated. When the foot and ankle are not fully utilized during walking, the muscles can weaken and shrink over time. Nurses should monitor for signs of muscle atrophy, such as decreased muscle bulk or strength, and collaborate with the healthcare team to implement interventions to prevent further muscle deterioration.
Contractures
Foot drop can lead to contractures, which are tightening or shortening of muscles, tendons, or ligaments. This can result in limited range of motion and difficulty in achieving a normal gait pattern. Nurses should regularly assess for any signs of contractures, such as stiffness or limited joint mobility, and work with physical therapists to develop stretching and range of motion exercises to prevent or minimize contracture development.
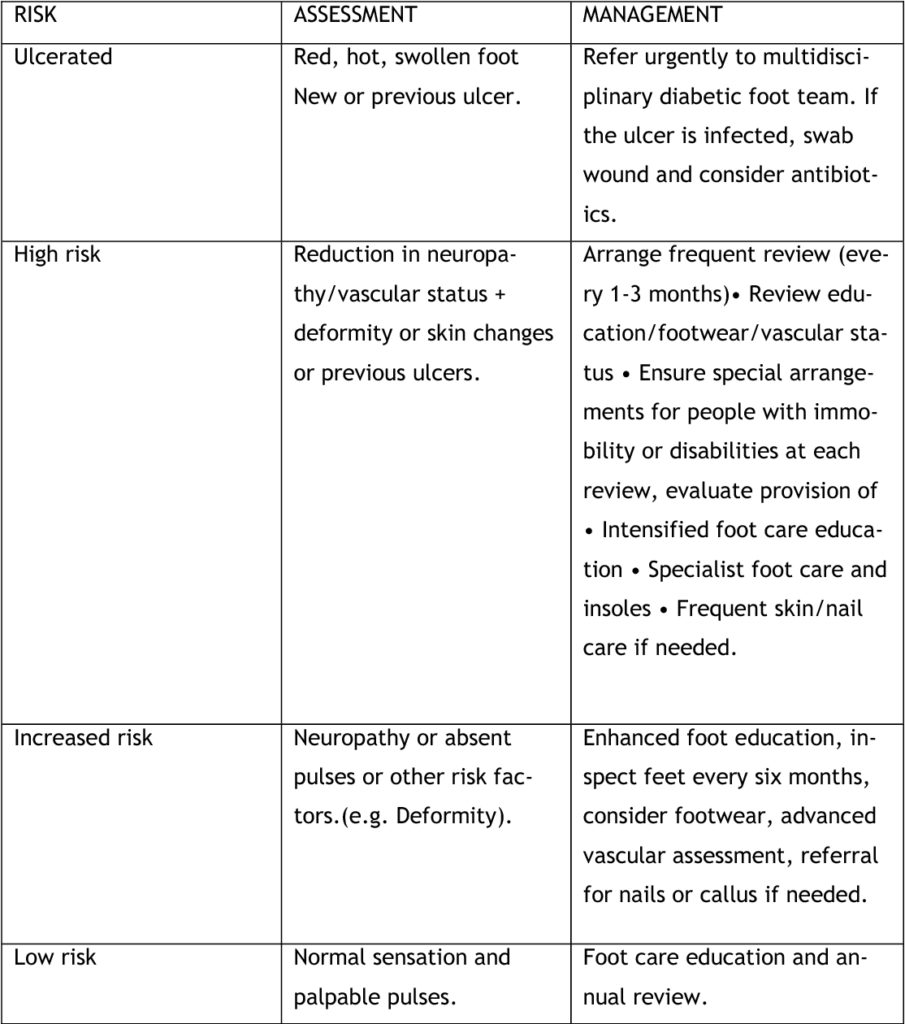
Skin breakdown
Foot drop increases the risk of skin breakdown, particularly in areas that bear excessive pressure or friction during walking. Nurses should inspect the patient’s skin regularly, paying close attention to areas such as the heel, ball of the foot, and bony prominences. It is important to promote proper positioning, provide adequate cushioning, and educate patients on the importance of regular skin checks and proper foot care.
Falls and injuries
Foot drop can significantly increase the risk of falls and injuries. Patients with foot drop may have difficulty maintaining balance and may trip or stumble more easily. Nurses should assess the patient’s fall risk and implement appropriate interventions to reduce the risk of falls, such as ensuring a safe environment, providing assistive devices, and educating patients on fall prevention strategies.
Collaborative Care
Physical therapy
Physical therapy plays a crucial role in the management of foot drop. Physical therapists can design individualized exercise programs to strengthen the muscles involved in foot and ankle movement, improve range of motion, and enhance overall lower limb function. Nurses should collaborate with physical therapists to ensure patients receive appropriate therapy and assist in monitoring progress.
Occupational therapy
Occupational therapy focuses on helping patients regain independence and improve their ability to perform daily activities. Occupational therapists can provide adaptations and techniques to compensate for foot drop, such as teaching patients how to use assistive devices or modifying their home environment to enhance safety. Nurses should work with occupational therapists to address functional limitations related to foot drop and provide ongoing support and education to patients.
Orthotic devices
Orthotic devices, such as ankle-foot orthosis (AFO), can provide support and stability to the affected foot and ankle, helping to eliminate or reduce the impact of foot drop on gait. Nurses should collaborate with the healthcare team to ensure proper fitting and use of orthotic devices and educate patients on their benefits and potential limitations.
Bracing and splinting
Bracing and splinting may be used as temporary or long-term interventions to address foot drop. They can provide support to the ankle and foot, prevent or correct contractures, and promote proper alignment during walking or standing. Nurses should assist in the application and adjustment of braces or splints as prescribed, and educate patients on their proper use and maintenance.

Nursing Interventions
Promoting mobility
Nurses play a vital role in promoting mobility for patients with foot drop. This includes assisting patients with transferring, ambulation, and exercises to maintain or improve lower limb function. Nurses should encourage and support patients to actively participate in mobility activities to prevent muscle weakness and functional decline.
Preventing complications
To prevent complications associated with foot drop, nurses should implement measures such as regular skin inspections, proper positioning, and appropriate use of assistive devices. Nurses should also educate patients and caregivers on the importance of practicing good foot care, performing regular skin checks, and promptly reporting any skin changes or abnormalities.
Assisting with daily activities
Patients with foot drop may face challenges in performing various daily activities like dressing, bathing, and toileting. Nurses should provide assistance and guidance to patients, enabling them to adapt to their limitations and find techniques to complete these activities more independently. Occupational therapists can also contribute to developing strategies to enhance daily activities.
Educating patient and family
Education is a crucial aspect of nursing care for patients with foot drop. Nurses should provide clear and concise information about the causes, management strategies, and potential complications of foot drop. Patients and their families should be educated on the proper use of assistive devices, home modifications, fall prevention techniques, and the importance of adhering to prescribed rehabilitation and exercise programs.
Exercise and Rehabilitation
Range of motion exercises
Range of motion exercises are essential for maintaining or improving joint flexibility and preventing the development of contractures. Nurses should collaborate with physical therapists to teach patients appropriate range of motion exercises for the foot and ankle. Regular performance of these exercises can help maintain joint mobility and prevent further limitations in movement.
Strengthening exercises
Strengthening exercises focus on improving the strength and function of the muscles involved in foot and ankle movement. Nurses should work closely with physical therapists to guide patients in performing exercises that target the specific muscles affected by foot drop. Strengthening exercises can help patients regain muscle strength, improve gait, and enhance overall lower limb function.
Balance and coordination training
Balance and coordination training are crucial aspects of rehabilitation for patients with foot drop. Physical therapists can design exercises and activities that challenge the patient’s balance and improve their ability to maintain proper posture and stability during walking. Nurses should encourage patients to actively participate in balance and coordination training to enhance their overall mobility and reduce the risk of falls.
Assistive Devices
Ankle-foot orthosis (AFO)
Ankle-foot orthosis (AFO) is a commonly used assistive device for patients with foot drop. AFOs provide support to the foot and ankle, helping to maintain proper alignment and facilitate a more normal gait pattern. Nurses should collaborate with the healthcare team to ensure proper fitting and use of AFOs, educate patients on their benefits and limitations, and provide ongoing support and monitoring.
Foot drop stimulator
Foot drop stimulators are electrical devices that stimulate the muscles involved in foot and ankle movement, helping to lift the foot during walking. Nurses should work closely with the healthcare team to educate patients on the proper use and maintenance of foot drop stimulators and monitor their effectiveness. Regular follow-up and adjustment may be necessary to optimize the benefits of these devices.
Canes, crutches, and walkers
Assistive devices such as canes, crutches, and walkers can provide additional support and stability for patients with foot drop. These devices can be used to compensate for the muscle weakness or instability associated with foot drop and improve the patient’s ability to maintain balance and walk with more confidence. Nurses should assist patients in selecting the right assistive device and ensure proper training and use.
Skin Care
Inspecting skin regularly
Regular skin inspections are essential for preventing skin breakdown in patients with foot drop. Nurses should visually inspect the skin for any redness, swelling, breakdown, or signs of infection. The assessment should be focused on areas at higher risk of pressure or friction, such as the heel, ball of the foot, and bony prominences. Any abnormalities should be reported to the healthcare team for further evaluation and intervention.
Proper positioning
Proper positioning is crucial in preventing pressure ulcers and skin breakdown. Nurses should encourage patients with foot drop to maintain optimal positioning, which includes avoiding prolonged periods of pressure on vulnerable areas. The use of pillows, cushions, or specialized positioning devices can help alleviate pressure and reduce the risk of skin problems.
Applying moisturizers and barrier creams
Moisturizers and barrier creams can help keep the skin hydrated and protect it from excessive friction or irritation. Nurses should educate patients on the importance of applying moisturizers regularly, especially to dry or vulnerable areas. Barrier creams can provide an additional protective layer to prevent moisture loss and reduce the risk of skin breakdown.

Fall Prevention
Assessing fall risk
It is essential for nurses to assess the fall risk of patients with foot drop. This can include evaluating factors such as gait instability, muscle weakness, balance impairments, and environmental hazards. Fall risk assessments can help identify the need for specific interventions and assistive devices, as well as guide patient education on fall prevention strategies.
Maintaining a safe environment
Creating a safe environment is crucial in preventing falls for patients with foot drop. Nurses should collaborate with the healthcare team to ensure the patient’s living space is free from clutter, has adequate lighting, and is equipped with safety measures such as handrails and grab bars. Eliminating tripping hazards and ensuring proper flooring surfaces can significantly reduce the risk of falls.
Using assistive devices
Assistive devices such as canes, crutches, and walkers can play a vital role in fall prevention for patients with foot drop. Nurses should educate patients on the proper use and selection of these devices, ensuring they are properly fitted and regularly maintained. Regular training and practice in using assistive devices can enhance mobility and reduce the risk of falls.
Patient Education
Foot drop causes and management
Educating patients about the causes and management of foot drop is a fundamental aspect of nursing care. Nurses should explain the underlying conditions or factors contributing to foot drop, such as neurological or muscular causes. Patients should be informed about the available treatment options, including physical therapy, orthotic devices, and assistive devices. Providing patients with a clear understanding of foot drop can empower them to actively participate in their care.
Proper use of assistive devices
Proper use of assistive devices is crucial for maximizing their benefits and ensuring patient safety. Nurses should provide detailed instructions on how to use canes, crutches, walkers, or orthotic devices correctly. Patients should be educated on proper fitting, adjustment, and maintenance of these devices. Additionally, ongoing support and follow-up should be provided to address any issues or concerns related to the use of assistive devices.
Importance of exercise and rehabilitation
Nurses should emphasize the importance of exercise and rehabilitation in managing foot drop. Patients should be educated on the benefits of regular exercise, such as improving muscle strength, maintaining joint flexibility, and promoting functional independence. Emphasizing the role of physical therapy and rehabilitation programs can motivate patients to actively participate in their treatment and adhere to prescribed exercises and activities.
Skin care and prevention of complications
Education on skin care and prevention of complications is essential for patients with foot drop. Nurses should educate patients and caregivers on the importance of regular skin inspections, proper positioning, and the use of moisturizers and barrier creams. Patients should be taught strategies to prevent pressure ulcers and skin breakdown, such as shifting weight, avoiding prolonged pressure, and maintaining good hygiene practices.
In conclusion, nursing considerations for patients with foot drop involve a comprehensive assessment of patient history, physical examination, and gait analysis. Understanding the etiology of foot drop, including neurological, muscular, and mechanical causes, is crucial for effective collaborative care. Nurses play a vital role in preventing complications, promoting mobility, and providing education to patients and their families. By implementing exercise and rehabilitation programs, utilizing assistive devices, and promoting proper skin care and fall prevention strategies, nurses can contribute to improved outcomes for patients with foot drop.