If you or someone you know is living with heart disease, it is important to understand the nursing considerations and management strategies that can help improve quality of life. From medication management to lifestyle modifications, nurses play a crucial role in supporting individuals with heart disease. In this article, we will explore some key nursing considerations for heart disease, highlighting the importance of regular screenings, patient education, and the implementation of evidence-based practices. By implementing these nursing strategies, we can empower individuals with heart disease to take control of their health and enhance their overall well-being.
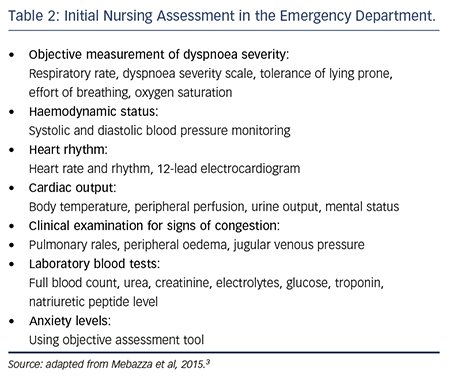
Assessment
History taking
In order to provide appropriate care for individuals with heart disease, a thorough history taking is essential. This includes gathering information about the patient’s medical history, family history, and any previous cardiac events. It is important to inquire about symptoms such as chest pain, shortness of breath, and fatigue. Additionally, assessing lifestyle factors such as diet, exercise habits, and smoking history can provide insight into the patient’s overall cardiovascular health.
Physical examination
A comprehensive physical examination is crucial for assessing the patient’s cardiovascular status. This includes measuring vital signs such as blood pressure, heart rate, and oxygen saturation levels. The healthcare provider should also listen to the patient’s heart and lung sounds, as well as assess for any signs of swelling or fluid retention. A thorough examination of the extremities can help identify any peripheral vascular disease or poor circulation.
Diagnostic tests
Various diagnostic tests can aid in the management of heart disease. These may include electrocardiograms (EKGs), stress tests, echocardiograms, and angiograms. These tests provide valuable information about the structure and function of the heart, as well as any potential blockages or abnormalities. It is important to ensure that the patient understands the purpose and potential risks of these tests, as well as any necessary preparation or restrictions.
Medication Management
Administering medications
As a nurse, one of your important responsibilities is administering medications to individuals with heart disease. This may involve giving medications such as beta blockers, calcium channel blockers, or antiplatelet agents. It is crucial to accurately calculate and measure the dosage, as well as adhere to the proper route of administration. In addition, providing education to patients about their medications, including potential side effects and the importance of adherence, can help ensure optimal outcomes.
Monitoring medication effects
Regular monitoring of the patient’s response to medication is essential for managing heart disease. This may involve assessing blood pressure, heart rate, and any laboratory values that may be affected by the medication. Additionally, monitoring for adverse reactions or side effects is crucial. By closely observing the patient’s condition and communicating any changes to the healthcare provider, you can play a vital role in promoting medication safety and efficacy.
Identifying potential drug interactions
Patients with heart disease often require multiple medications, which increases the risk of potential drug interactions. As a nurse, it is important to be knowledgeable about the medications being used and their potential interactions. This includes understanding the mechanism of action, potential adverse effects, and any contraindications or precautions. By conducting a thorough medication review and effectively communicating with the healthcare team, you can help prevent drug interactions and optimize patient safety.
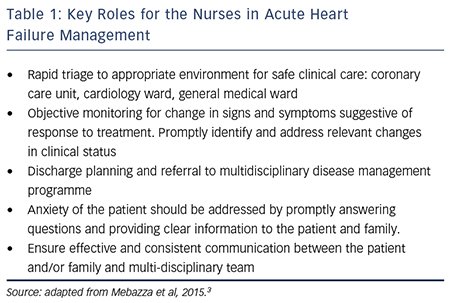

Dietary Modifications
Low-sodium diet
A key aspect of managing heart disease is implementing a low-sodium diet. This helps reduce fluid retention and lower blood pressure, reducing the workload on the heart. As a nurse, you can provide guidance and education to patients on how to effectively follow a low-sodium diet. This may involve recommending alternatives to high-sodium foods, teaching patients how to read food labels for sodium content, and providing resources for healthy recipes and meal planning.
Heart-healthy diet
In addition to a low-sodium diet, promoting a heart-healthy diet can significantly impact cardiovascular health. This includes encouraging the consumption of fruits, vegetables, whole grains, lean proteins, and healthy fats. As a nurse, you can provide education on the benefits of specific nutrients and foods, as well as strategies for incorporating them into daily meals. By supporting patients in making healthy dietary choices, you can help improve their overall cardiovascular well-being.
Monitoring fluid intake
Monitoring fluid intake is crucial for individuals with heart disease, as excessive fluid retention can exacerbate symptoms and lead to complications. As a nurse, you can educate patients on the importance of monitoring their fluid intake and provide guidance on appropriate daily limits. This may involve recommending specific fluid restrictions based on the patient’s condition and working with the healthcare team to adjust fluid orders as needed. Regularly assessing fluid status, including monitoring for signs of fluid overload, is also essential for effective management of heart disease.
Lifestyle Changes
Encouraging regular exercise
Regular exercise plays a vital role in managing heart disease. As a nurse, you can encourage and support patients in incorporating exercise into their daily routine. This may involve discussing the benefits of exercise for cardiovascular health, providing recommendations for appropriate exercise types and intensity levels, and assisting with developing an individualized exercise plan. Additionally, monitoring the patient’s progress and providing ongoing motivation and support can help ensure adherence to a regular exercise regimen.
Smoking cessation counseling
Smoking is a major risk factor for heart disease, and quitting smoking can significantly improve cardiovascular outcomes. As a nurse, you can play a crucial role in assisting patients with smoking cessation. This may involve providing education on the health risks of smoking, offering resources and support for quitting, and referring patients to smoking cessation programs or healthcare providers specialized in smoking cessation. By advocating for smoking cessation and providing ongoing support, you can contribute to better heart health for your patients.
Managing stress levels
High levels of stress can have a negative impact on heart health. As a nurse, you can help individuals with heart disease manage their stress levels. This may involve teaching stress management techniques, such as relaxation exercises, deep breathing, and mindfulness. Additionally, you can provide guidance on lifestyle modifications to reduce stress, such as incorporating regular breaks and engaging in hobbies and activities that promote relaxation. By addressing the emotional well-being of patients, you can support their overall cardiovascular health.
Patient Education
Explaining heart disease and its implications
Providing education to patients about heart disease and its implications is vital for their understanding and engagement in self-care. As a nurse, you can explain the underlying causes of heart disease, the importance of managing risk factors, and the potential complications. Using clear and simple language, you can help patients comprehend their condition and the necessary steps for effective management. This includes discussing the role of medication, lifestyle modifications, and regular follow-up appointments in maintaining cardiovascular health.
Teaching self-care techniques
Empowering patients to take an active role in their own care is a fundamental aspect of nursing management for heart disease. This involves teaching self-care techniques that individuals can implement on a daily basis. These may include monitoring blood pressure at home, recognizing signs of worsening symptoms, and knowing when to seek medical attention. By providing clear instructions, educational materials, and ongoing support, you can help patients become more confident and competent in managing their condition.
Educating on medication adherence
Medication adherence is essential for achieving optimal outcomes in heart disease management. As a nurse, you can educate patients on the importance of taking their medications as prescribed and how to establish a medication routine. This includes discussing potential barriers to adherence, such as forgetfulness or concerns about side effects, and providing strategies to overcome these challenges. Regularly assessing medication adherence and addressing any concerns or misconceptions can help promote medication adherence and improve patient outcomes.
Pain Management
Assessing and monitoring pain levels
Managing pain effectively is crucial for individuals with heart disease. As a nurse, you play a key role in assessing and monitoring pain levels. This may involve using pain assessment tools to determine the intensity of pain, as well as evaluating the location, duration, and quality of the pain. Regularly reassessing the patient’s pain levels throughout their hospital stay or outpatient visits can help ensure that appropriate interventions are implemented to alleviate discomfort.
Administering pain medications
Administering pain medications is an essential nursing responsibility in managing pain associated with heart disease. This may involve administering analgesics such as opioids, nonsteroidal anti-inflammatory drugs (NSAIDs), or nitroglycerin. It is crucial to be knowledgeable about the specific medications being used, including their pharmacokinetics, potential side effects, and any contraindications or precautions. Administering pain medications safely and effectively can help improve patient comfort and promote optimal healing.
Implementing non-pharmacological pain relief methods
In addition to pain medications, non-pharmacological pain relief methods can be effective in managing pain associated with heart disease. These may include relaxation techniques, distraction techniques, heat or cold therapy, and massage. As a nurse, you can collaborate with the healthcare team to implement appropriate non-pharmacological pain relief methods. Providing education and support to patients in utilizing these techniques can help reduce pain and improve overall well-being.
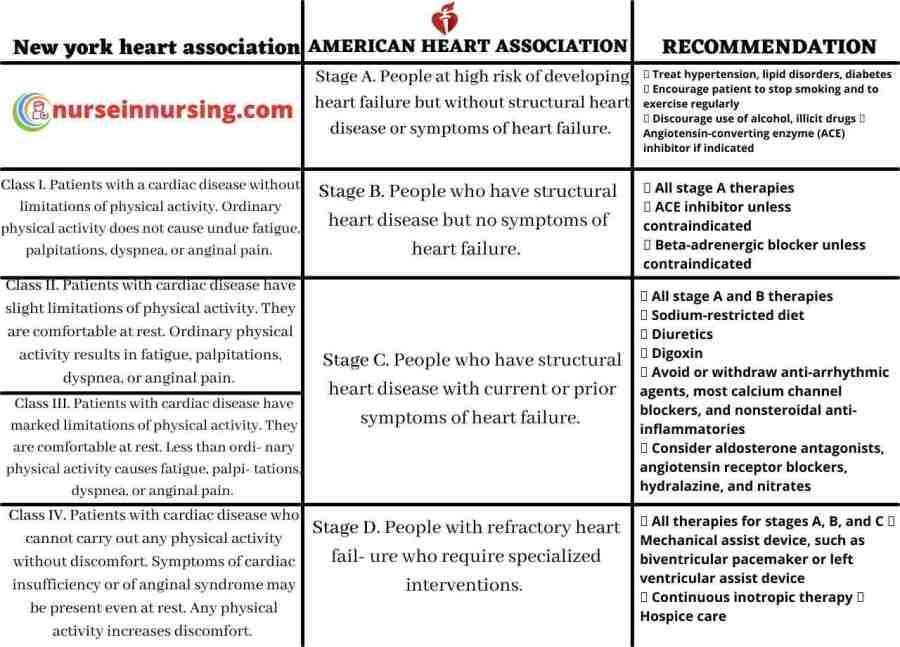
Managing Comorbidities
Recognizing and addressing concurrent conditions
Individuals with heart disease often have concurrent conditions that require management. As a nurse, it is important to be vigilant in recognizing and addressing these comorbidities. This may involve monitoring for signs and symptoms of conditions such as diabetes, hypertension, or renal dysfunction. Collaborating with the healthcare team and providing appropriate interventions and referrals can help prevent complications and optimize the patient’s overall health.
Coordinating care with other healthcare providers
Effective management of heart disease often involves coordination with various healthcare providers. As a nurse, you can play a crucial role in coordinating care and ensuring effective communication among the healthcare team. This may involve sharing relevant patient information, scheduling appointments, and advocating for the patient’s needs and preferences. By facilitating collaboration and continuity of care, you can help ensure that the patient receives comprehensive and cohesive healthcare services.
Adjusting treatment plan accordingly
As the patient’s condition and needs change, it is important to adjust the treatment plan accordingly. This may involve modifying medication dosages, adding or discontinuing medications, or implementing additional interventions to address emerging issues. Working collaboratively with the healthcare team, including the patient and their family, allows for ongoing assessment and modification of the treatment plan. By continuously evaluating and adjusting the plan of care, you can optimize patient outcomes and ensure individualized care.
Monitoring Vital Signs
Regular blood pressure assessment
Regular blood pressure assessment is a fundamental aspect of nursing management for heart disease. As a nurse, you will be responsible for monitoring and recording the patient’s blood pressure. This includes measuring blood pressure at appropriate intervals, such as before and after medication administration or as per the healthcare provider’s orders. By closely monitoring blood pressure trends, you can identify any changes or abnormalities that may require further intervention or adjustment of the treatment plan.
Monitoring heart rate and rhythm
Monitoring heart rate and rhythm is essential for assessing the cardiovascular status of individuals with heart disease. As a nurse, you will assess the patient’s heart rate and rhythm through palpation, auscultation, or by using medical devices such as an electrocardiogram (ECG). Regularly evaluating heart rate and rhythm can provide valuable information about the effectiveness of medications, the presence of arrhythmias, or any changes that may require further investigation or intervention.
Evaluating oxygen saturation levels
Evaluating oxygen saturation levels is important for assessing the respiratory status of individuals with heart disease. As a nurse, you will measure oxygen saturation levels using a pulse oximeter. This non-invasive method allows for continuous monitoring of oxygen levels in the patient’s bloodstream. Regularly assessing oxygen saturation levels can help identify any signs of hypoxia or respiratory distress, allowing for prompt intervention and appropriate management of the patient’s condition.

Infection Prevention
Assessing for signs of infection
Individuals with heart disease are often at an increased risk of developing infections. As a nurse, it is important to assess patients for any signs and symptoms of infection. This includes monitoring for typical signs such as fever, increased heart rate, and changes in respiratory status. Additionally, recognizing the occurrence of common infections such as respiratory or urinary tract infections is crucial. By promptly identifying and responding to signs of infection, you can prevent complications and promote the patient’s overall well-being.
Educating the patient about preventive measures
Educating patients about preventive measures is essential in reducing the risk of infection in individuals with heart disease. As a nurse, you can provide guidance on strategies such as proper hand hygiene, respiratory hygiene, and immunizations. This includes explaining the importance of regular handwashing, avoiding close contact with sick individuals, and staying up-to-date with recommended vaccines. By empowering patients through education, you can help them take proactive steps to protect themselves from infections.
Promoting proper hand hygiene
Proper hand hygiene is crucial in preventing the spread of infections. As a nurse, you can play a significant role in promoting hand hygiene among patients with heart disease. This includes educating patients on the proper technique for handwashing, reminding them to wash their hands regularly, and providing access to hand sanitizers or handwashing facilities. By incorporating hand hygiene practices into the daily routine of patients, you can contribute to minimizing the risk of infections and promoting overall health.
Psychosocial Support
Identifying emotional concerns
Individuals with heart disease often experience emotional concerns and may require additional psychosocial support. As a nurse, it is important to be attentive to any signs of emotional distress or psychological symptoms. This may include anxiety, depression, or feelings of fear and uncertainty. By conducting regular assessments and actively listening to patients, you can identify areas of concern and provide appropriate support and referral to a mental health professional if needed.
Providing counseling and emotional support
Providing counseling and emotional support is a fundamental aspect of nursing management for individuals with heart disease. As a nurse, you can offer a listening ear, provide empathy, and encourage open communication. This may involve discussing the patient’s fears and concerns, exploring coping strategies, and providing encouragement and reassurance. By actively engaging with patients and their families, you can help alleviate emotional distress and promote a positive psychosocial environment.
Referring to appropriate mental health professionals
In some cases, individuals with heart disease may require specialized mental health support. As a nurse, it is important to be knowledgeable about available resources and referral options. This includes collaborating with social workers, psychologists, or psychiatrists who can provide additional counseling or therapy services. By advocating for comprehensive mental health care, you can ensure that individuals with heart disease receive the support they need to navigate the emotional challenges associated with their condition.
In conclusion, nursing considerations and nursing management for heart disease encompass various aspects of care. From assessment and physical examination to medication management, dietary modifications, lifestyle changes, patient education, pain management, managing comorbidities, monitoring vital signs, infection prevention, and psychosocial support, the role of the nurse is crucial in promoting optimal outcomes for individuals with heart disease. By providing comprehensive and patient-centered care, nurses contribute significantly to the overall well-being and quality of life of patients with heart disease.
