Are you ready to dive into the world of nursing considerations for kidney disease? With this article, we will explore the important role that nurses play in the management and care of patients with kidney disease. From monitoring vital signs to administering medications, nurses are vital in ensuring the well-being of these patients. Join us as we explore the various aspects of nursing considerations and management for kidney disease, providing insights and tips for providing the best possible care. So, put on your nursing cap and let’s get started!

Assessment
General Assessment
When it comes to managing kidney disease, a thorough assessment is crucial in order to provide the best possible care. In the general assessment, various factors need to be taken into consideration. This includes assessing the patient’s medical history, identifying any risk factors for kidney disease, and evaluating their lifestyle habits such as smoking and alcohol consumption. Additionally, it is important to assess the patient’s overall physical and mental well-being, as kidney disease can have significant impacts on both aspects of health.
Physical Assessment
A physical assessment is an integral part of caring for patients with kidney disease. This involves examining the patient’s vital signs, including blood pressure, heart rate, and temperature, in order to monitor any changes that may indicate worsening kidney function. Physical assessments also include evaluating the presence of edema, which often occurs in kidney disease due to fluid retention. It is important to check for signs of fluid overload, such as swelling in the legs and ankles.
Psychosocial Assessment
In addition to the physical aspects of kidney disease, it is essential to assess the patient’s psychosocial well-being. Chronic kidney disease can have a significant emotional impact on patients, leading to anxiety, depression, and other mental health concerns. By conducting a thorough psychosocial assessment, healthcare providers can identify any underlying emotional issues that may need to be addressed. Understanding the patient’s emotional state allows for the provision of appropriate counseling, emotional support, and patient education to help them cope with their disease.
Diagnosis
Laboratory Tests
Laboratory tests play a vital role in diagnosing and monitoring kidney disease. These tests include blood tests to measure levels of various substances, such as creatinine and urea, which can indicate kidney function. Urinalysis is also important, as it can detect the presence of abnormal levels of protein, blood, or other substances in the urine. These tests provide valuable information to healthcare providers and help guide further treatment decisions.
Imaging Tests
Imaging tests are often necessary to visualize the kidneys and assess their structure and function. Common imaging tests used in the diagnosis of kidney disease include ultrasound, which uses sound waves to create images of the kidneys, and computed tomography (CT) scans, which provide detailed cross-sectional images. These tests enable healthcare providers to identify any structural abnormalities or blockages that may be contributing to the patient’s kidney disease.

Medication Administration
Understanding Medications for Kidney Disease
Proper understanding of medications is essential for managing kidney disease effectively. Medications commonly prescribed for kidney disease include angiotensin-converting enzyme (ACE) inhibitors and angiotensin receptor blockers (ARBs), which help to lower blood pressure and protect the kidneys from further damage. Diuretics may also be prescribed to help control fluid retention. It is important for patients to understand the rationale behind their medications, their potential side effects, and the importance of adhering to the prescribed dosage.
Dosage and Administration Considerations
Administering medications for kidney disease requires careful consideration of the patient’s kidney function. Dosage adjustments are often necessary, as impaired kidney function can affect how medications are metabolized and eliminated from the body. Close monitoring of renal function is important to ensure that appropriate adjustments are made to medication dosages. Additionally, healthcare providers must educate patients on the importance of adhering to their prescribed medication regimen and provide clear instructions on how and when to take their medications.
Fluid and Electrolyte Balance
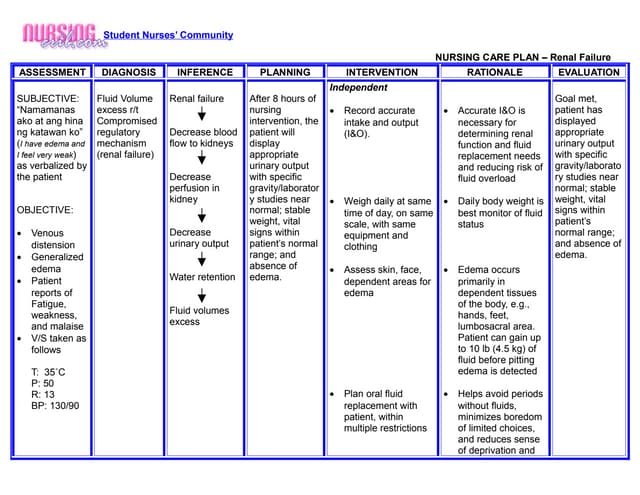
Monitoring Fluid Intake and Output
Maintaining a proper fluid balance is crucial for patients with kidney disease. Monitoring fluid intake and output is essential to prevent fluid overload or dehydration, both of which can have negative consequences on kidney function. Healthcare providers must closely monitor the patient’s fluid intake, including drinking habits and any intravenous fluids administered. Measuring urine output is also important to assess the kidneys’ ability to effectively filter waste products.
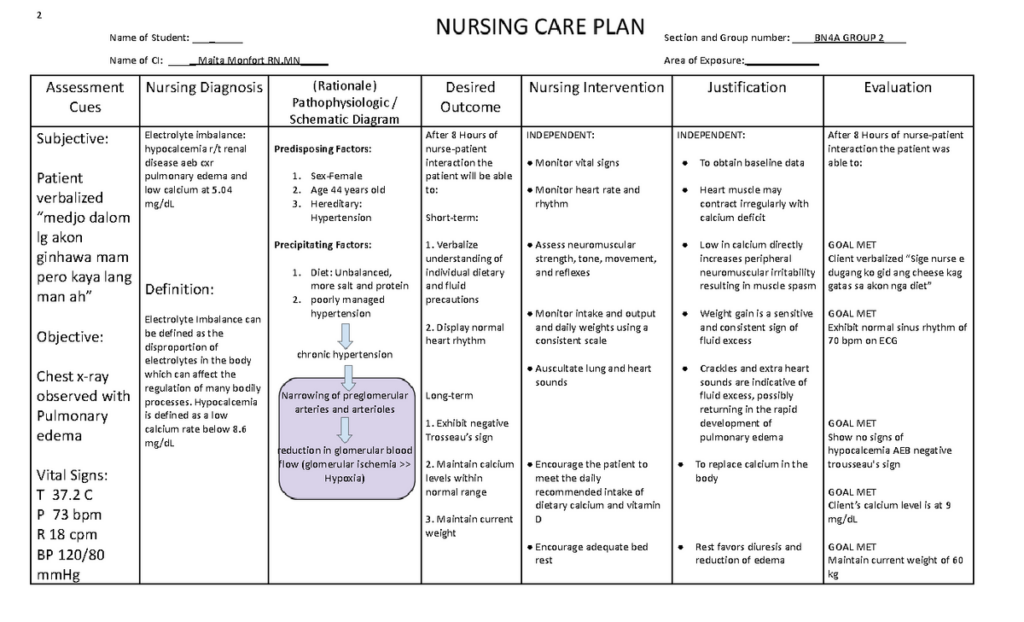
Managing Electrolyte Imbalance
Kidney disease often leads to electrolyte imbalances, such as high potassium levels (hyperkalemia) or low calcium levels (hypocalcemia). Monitoring electrolyte levels regularly is important to detect any imbalances promptly. In cases of hyperkalemia, dietary modifications and medication adjustments may be necessary to regulate potassium levels. In cases of hypocalcemia, calcium supplements or vitamin D may be prescribed. Maintaining proper electrolyte balance is essential for overall health and effective management of kidney disease.
Nutritional Support
Dietary Modification
Dietary modifications are an integral part of managing kidney disease. It is important to work closely with a registered dietitian to develop an individualized meal plan that meets the specific nutritional needs of each patient. In general, a kidney-friendly diet involves limiting the intake of sodium, phosphorus, and potassium, as well as controlling fluid intake. This typically means avoiding processed foods, high-sodium condiments, and foods rich in phosphorus and potassium, such as dairy products and certain fruits and vegetables.
Supplemental Nutrition
In some cases, patients with kidney disease may require supplemental nutrition to ensure they are getting adequate nutrients. This can be due to poor appetite, dietary restrictions, or other factors that may limit their ability to meet their nutritional needs through food alone. Nutritional supplements, such as protein shakes or drinks, may be recommended to supplement the patient’s diet and prevent malnutrition.
Monitoring Dietary Compliance
Monitoring dietary compliance is crucial to ensure that patients are adhering to their prescribed meal plans. Regular follow-ups with a registered dietitian can help identify any challenges or areas of non-compliance and provide appropriate education and support. It is important for patients to understand the impact of their dietary choices on their kidney health and the importance of following dietary guidelines to prevent further complications.
Dialysis
Hemodialysis
Hemodialysis is a common treatment option for patients with end-stage renal disease. During hemodialysis, blood is filtered outside the body through a dialysis machine, removing waste products and excess fluid. Nursing care during hemodialysis involves closely monitoring vital signs, ensuring the patient’s comfort and safety, and monitoring for potential complications such as hypotension or infection. Additionally, education regarding dialysis procedures and self-care at home is crucial for patients receiving hemodialysis.
Peritoneal Dialysis
Peritoneal dialysis is another option for patients with kidney disease. It involves using the lining of the abdomen (peritoneum) as a natural filter to remove waste products and excess fluid. Nursing care during peritoneal dialysis includes teaching patients how to perform the procedure correctly, ensuring proper catheter care, and monitoring for potential complications such as infection or peritonitis. Ongoing education and support are essential to help patients successfully manage peritoneal dialysis at home.
Nursing Care during Dialysis
Whether patients undergo hemodialysis or peritoneal dialysis, nursing care during dialysis is crucial. This includes close monitoring of vital signs, assessing for any signs of complications or adverse reactions, and ensuring the patient’s comfort and safety throughout the procedure. Additionally, providing emotional support and addressing any concerns or anxieties that patients may have is an important aspect of nursing care during dialysis.
Preventing Infection
Hand Hygiene
Preventing infection is a top priority when caring for patients with kidney disease. Hand hygiene is one of the simplest and most effective ways to prevent the spread of infections. Nurses must emphasize the importance of proper hand hygiene to patients and caregivers, educating them on the proper technique for washing hands with soap and water or using alcohol-based hand sanitizers.
Aseptic Techniques
In addition to hand hygiene, maintaining aseptic techniques is crucial when providing care to patients with kidney disease. This includes ensuring that all medical equipment and supplies used during procedures are sterile and properly cleaned. Nurses must adhere to strict aseptic techniques to prevent any potential sources of infection.
Education for Patients and Caregivers
Education plays a vital role in preventing infections in patients with kidney disease. Nurses must provide comprehensive education to patients and their caregivers on infection prevention strategies, including proper wound care techniques, recognizing signs of infection, and when to seek medical attention. By empowering patients and caregivers with the necessary knowledge and skills, the risk of infections can be significantly reduced.
Pain Management
Assessment and Documentation of Pain
Pain is a common symptom experienced by patients with kidney disease, and effective pain management is essential to improve their quality of life. Nurses must conduct a thorough assessment of the patient’s pain, including its location, intensity, and any aggravating or alleviating factors. Accurate documentation of pain assessments is crucial in evaluating the effectiveness of pain management interventions and ensuring that appropriate interventions are implemented.
Non-pharmacological Interventions
In addition to medications, non-pharmacological interventions can be effective in managing pain for patients with kidney disease. These include techniques such as relaxation exercises, heat or cold therapy, and distraction techniques. Nurses can provide education and support to help patients incorporate these non-pharmacological interventions into their daily routine and manage their pain more effectively.
Medication Administration for Pain Relief
In cases where non-pharmacological interventions are not sufficient, medications may be necessary to provide adequate pain relief. Nurses must have a thorough understanding of the medications commonly used for pain management and their potential side effects. It is important to carefully assess the patient’s pain level before administering medication and to closely monitor their response to the medication to ensure optimal pain relief.
Psychosocial Support
Addressing Anxiety and Depression
Patients with kidney disease often experience high levels of anxiety and depression due to the challenges and lifestyle changes that come with their condition. Nurses play a crucial role in addressing these psychosocial concerns. By providing empathetic and supportive care, nurses can help alleviate anxiety and depression symptoms. Referring patients to mental health professionals or support groups can also provide additional support in managing their emotional well-being.
Counseling and Emotional Support
Counseling and emotional support are essential components of psychosocial support for patients with kidney disease. Nurses can provide counseling and education to help patients and their families understand and cope with the emotional impact of the disease. Additionally, providing emotional support and actively listening to patients’ concerns can help them feel understood and supported throughout their healthcare journey.
Patient Education
Patient education is a crucial aspect of psychosocial support for patients with kidney disease. By providing comprehensive education on their condition, treatment options, and self-care, nurses can empower patients to actively participate in their own healthcare. Education can include information on medication management, dietary modifications, and lifestyle changes. Ensuring that patients have the knowledge and skills to effectively manage their condition can greatly improve their overall well-being.
End-of-Life Care
Palliative Care
End-of-life care is an important aspect of nursing considerations for patients with kidney disease. Palliative care focuses on providing comfort and alleviating suffering for patients with life-limiting illnesses. This includes managing symptoms such as pain, nausea, and shortness of breath to improve the patient’s quality of life. Nurses play a vital role in coordinating and providing palliative care, ensuring that patients receive comprehensive and compassionate end-of-life support.
Patient and Family Support
Supporting patients and their families during end-of-life care is essential for providing a holistic approach to care. Nurses must provide emotional support and guidance, helping patients and their families navigate the emotional and logistical challenges that may arise. This can include facilitating difficult conversations about advanced care planning and offering grief support services to family members following the loss of a loved one.
Ethical Considerations
End-of-life care for patients with kidney disease often involves complex ethical considerations. Nurses must be knowledgeable about ethical principles, such as autonomy, beneficence, and non-maleficence, and their application in end-of-life decision-making. This includes respecting patients’ wishes regarding resuscitation, artificial hydration, and the use of life-sustaining treatments. Nurses must advocate for the patient’s best interests while also honoring their autonomy and ensuring their comfort and dignity during the end-of-life journey.
