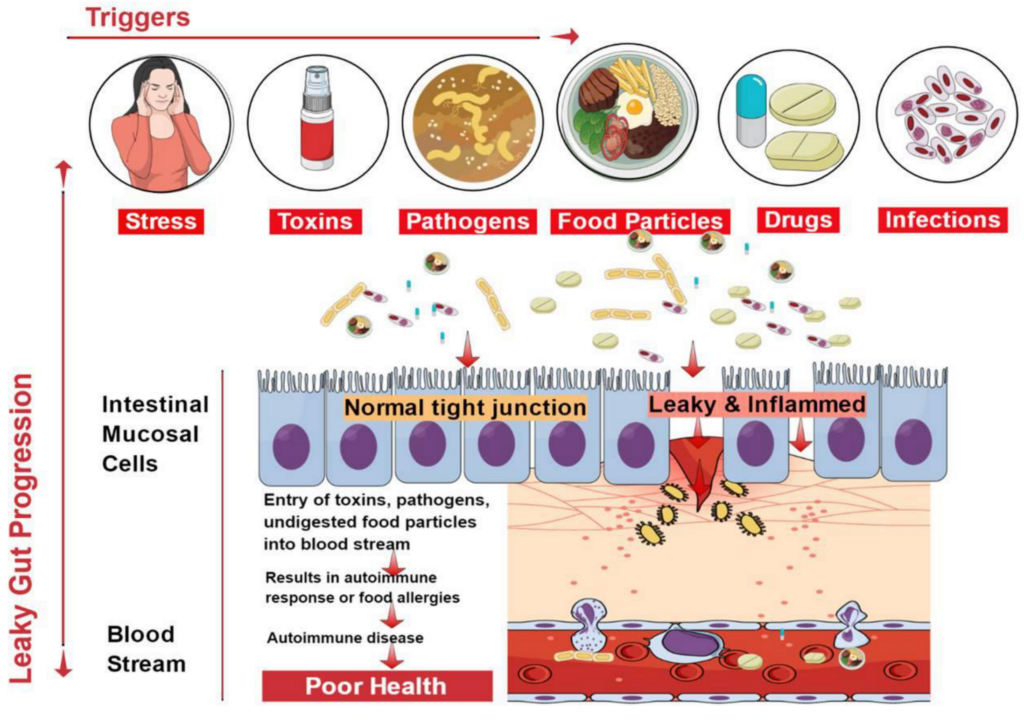
Are you familiar with Leaky Gut Syndrome? If not, don’t worry, because in this article, we will provide you with all the necessary information about this condition and the important nursing considerations that need to be taken into account. Leaky Gut Syndrome is a condition that occurs when the lining of the intestines becomes damaged, allowing toxins and other harmful substances to leak into the bloodstream. As a nurse, it is essential to understand the symptoms, diagnostic tests, and treatment options for patients with this condition. By implementing proper nursing management strategies, you can make a significant difference in the care and recovery of individuals with Leaky Gut Syndrome.

Assessment
Patient history
During the assessment process, it is crucial to gather a comprehensive patient history in order to better understand their symptoms and potential triggers of leaky gut syndrome. This includes asking about their medical history, current medications, dietary habits, and lifestyle factors. Additionally, inquiring about any previous or current GI symptoms such as abdominal pain, diarrhea, or constipation can provide valuable information for the assessment process.
Physical examination
A physical examination is an important component of the assessment for leaky gut syndrome. It allows healthcare professionals to evaluate the patient’s overall health and to identify any physical signs that may be associated with the condition. For instance, signs of malnutrition, such as poor skin turgor or muscle wasting, may be indicative of underlying nutrient deficiencies.
Laboratory tests
Laboratory tests play a critical role in the assessment of leaky gut syndrome as they can help identify potential underlying causes or complications. Blood tests, stool analysis, and allergy testing may be performed to assess for any nutrient deficiencies, evaluate gut function, and identify potential food allergies or intolerances. These tests can provide valuable information to guide treatment strategies and inform healthcare professionals about the patient’s condition.
Nutrition
Dietary modifications
Dietary modifications are a key aspect of managing leaky gut syndrome. The goal is to reduce inflammation and provide the body with the necessary nutrients to promote gut healing. It is important to educate patients on the importance of a balanced diet, which includes a variety of whole foods such as fruits, vegetables, lean proteins, and healthy fats. Avoiding processed foods, refined sugars, and artificial additives is also advised.
Supplements
Supplements may be recommended to support gut healing and address nutrient deficiencies. Including a high-quality probiotic can help restore the balance of beneficial bacteria in the gut. Additional supplements, such as omega-3 fatty acids, vitamin D, and zinc, may also be beneficial in promoting gut health and reducing inflammation.
Food allergies and intolerances
Identifying and addressing food allergies and intolerances is crucial in the management of leaky gut syndrome. Patients may be advised to eliminate certain trigger foods from their diet, such as gluten, dairy, or specific allergens identified through allergy testing. Keeping a food diary and reintroducing eliminated foods can help identify specific triggers and guide dietary adjustments.

Medication
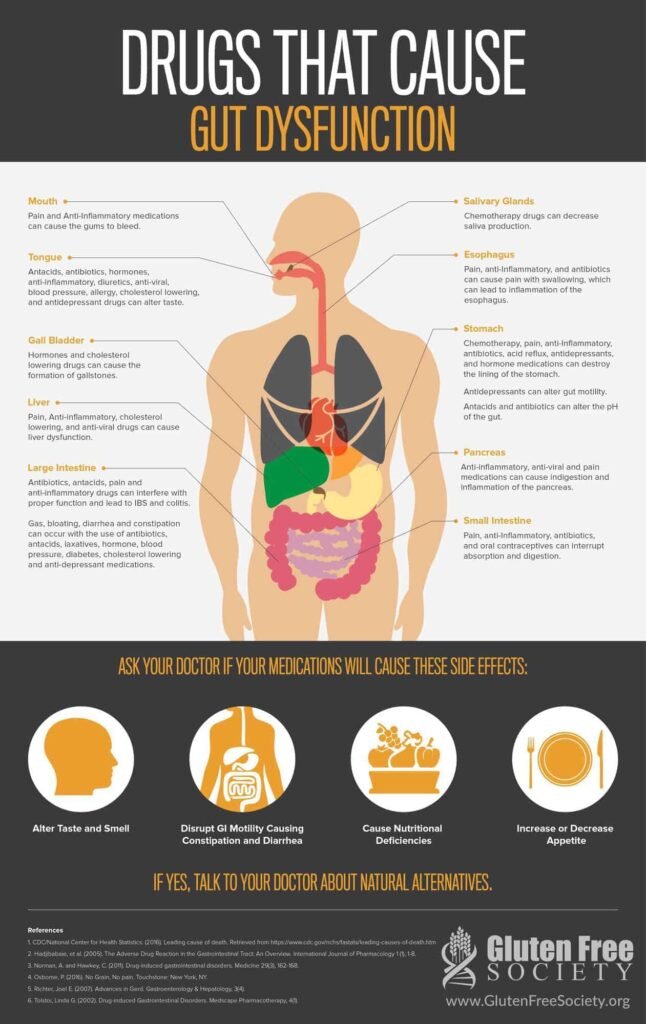
Prescription medications
Prescription medications may be utilized in the management of leaky gut syndrome, depending on the underlying causes and symptoms present. For example, if the patient has an underlying autoimmune condition, immunosuppressant medications may be prescribed to reduce inflammation and prevent further damage to the gut lining. Anti-inflammatory medications may also be considered in certain cases.
Over-the-counter medications
Over-the-counter medications such as antacids or digestive enzymes may be recommended to help manage symptoms such as heartburn or indigestion. These medications can provide temporary relief while dietary and lifestyle modifications are implemented. However, it is important to ensure patients understand the potential risks and limitations of over-reliance on these medications.
Probiotics
Understanding probiotics
Probiotics are live bacteria and yeasts that are beneficial to the gut microbiome. These “good” bacteria can help maintain a healthy balance in the gut and support gut healing. Understanding the role of probiotics in leaky gut syndrome is important in guiding patients towards appropriate treatment options.
Choosing the right probiotic
When recommending a probiotic, it is essential to consider the specific strain and dosage. Different strains of bacteria have varying benefits and may be more effective for certain conditions. It is important to choose a probiotic that is backed by scientific evidence and has undergone quality testing to ensure safety and efficacy.
Administration and monitoring
Probiotics can be administered in various forms, such as capsules, powders, or fermented foods. It is important to educate patients on proper administration techniques and discuss the importance of consistent use. Monitoring the patient’s response to probiotics and assessing any changes in symptoms or gut function is crucial to determine the effectiveness of treatment and make necessary adjustments.
Stress management
Identifying stress triggers
Stress can have a significant impact on gut health and exacerbate symptoms of leaky gut syndrome. As part of the nursing management, it is important to help patients identify their stress triggers. This may involve encouraging open communication and active listening to understand the unique stressors that may be present in their lives.
Relaxation techniques
Teaching patients relaxation techniques can be helpful in managing stress and promoting overall well-being. Techniques such as deep breathing exercises, guided imagery, and mindfulness meditation can help alleviate stress, reduce inflammation, and promote gut healing. Encouraging patients to incorporate these techniques into their daily routine can have a positive impact on their overall health.
Supportive counseling
Providing supportive counseling to patients with leaky gut syndrome can help address any emotional or psychological challenges they may be facing. Exploring coping mechanisms, stress reduction strategies, and providing a safe space for patients to express their concerns can be beneficial in their overall management of the condition.
Treatment of underlying causes
Identifying and addressing infections
In some cases, leaky gut syndrome may be caused by underlying infections such as bacterial or fungal overgrowth in the gut. Identifying and treating these infections is crucial in achieving gut healing. This may involve performing diagnostic tests, such as stool cultures or breath tests, to identify the specific pathogen and guiding treatment with appropriate antimicrobial agents.
Managing autoimmune conditions
Autoimmune conditions, such as Crohn’s disease or celiac disease, can contribute to leaky gut syndrome. Management of these conditions may involve medication regimens, dietary modifications, and close monitoring of symptoms. Collaborating with healthcare professionals specializing in autoimmune diseases is vital to ensure comprehensive and effective management of these underlying conditions.
Addressing nutrient deficiencies
Nutrient deficiencies can further contribute to the dysfunction of the gut lining and delay healing. Identifying and addressing these deficiencies is essential in supporting gut healing. This may involve supplementation with specific vitamins or minerals, as well as dietary adjustments to ensure an adequate intake of essential nutrients.
Education and counseling
Patient education on leaky gut syndrome
Providing patients with education on leaky gut syndrome is important in empowering them to actively participate in their own care. This may involve explaining the pathophysiology of the condition, discussing potential triggers and aggravating factors, and clarifying treatment goals and expectations. Education should be tailored to the patient’s individual needs and delivered in a clear and understandable manner.
Lifestyle modifications
In addition to dietary modifications, lifestyle changes can play a significant role in managing leaky gut syndrome. This may include stress reduction strategies, regular exercise, and adequate sleep. Educating patients on the importance of these lifestyle modifications and providing guidance on how to incorporate them into their daily routine can have a positive impact on both gut health and overall well-being.
Support groups and resources
Connecting patients with support groups and additional resources can further enhance their management of leaky gut syndrome. Support groups provide a safe space for patients to share experiences, seek advice, and find understanding. Additionally, providing patients with reputable sources of information, such as reputable websites or educational materials, can help them in their journey of self-management.
Collaborative care
Working with other healthcare professionals
Collaboration with other healthcare professionals, including physicians, dietitians, and mental health professionals, is essential in providing comprehensive care for patients with leaky gut syndrome. By working together, healthcare professionals can exchange knowledge, assess treatment effectiveness, and develop individualized care plans that address the multifaceted aspects of the condition.
Referrals to specialists
Leaky gut syndrome may require additional specialized care based on the underlying causes or associated conditions. Referring patients to specialists, such as gastrointestinal specialists, allergists, or rheumatologists, can ensure that their specific needs are met and appropriate treatment is provided. Regular communication and coordination with these specialists are important for optimal patient outcomes.
Interdisciplinary care plans
Developing interdisciplinary care plans involving all relevant healthcare professionals is essential in managing leaky gut syndrome. These care plans should outline the roles and responsibilities of each team member, as well as establish clear communication channels to facilitate effective collaboration. Regular team meetings and case discussions can help ensure that all aspects of the patient’s care are addressed and monitored effectively.

Monitoring and evaluation
Assessing treatment effectiveness
Regular monitoring and evaluation of treatment effectiveness are crucial in managing leaky gut syndrome. This may involve assessing the patient’s symptoms, performing follow-up laboratory tests, and evaluating their response to dietary modifications or medication regimens. Adjustments to the treatment plan may be necessary based on the patient’s progress or any new findings.
Monitoring for complications
While leaky gut syndrome itself is not considered a life-threatening condition, it can lead to complications if left untreated or poorly managed. Monitoring for potential complications, such as infections, nutrient deficiencies, or worsening gastrointestinal symptoms, is vital in preventing further damage to the gut and promoting optimal patient outcomes.
Regular follow-up
Regular follow-up appointments are important in ensuring ongoing support and management of leaky gut syndrome. These appointments provide an opportunity to assess the patient’s progress, address any concerns or questions they may have, and make any necessary adjustments to their treatment plan. By maintaining open lines of communication, healthcare professionals can provide ongoing guidance and support to patients on their journey towards gut healing.
Patient advocacy
Ensuring patient rights and needs
As a healthcare professional, it is important to advocate for the rights and needs of patients with leaky gut syndrome. This involves ensuring that their voices are heard, their questions are answered, and their concerns are addressed. Empowering patients to actively participate in their care and making sure their needs are met can contribute to better patient outcomes and improved overall experience.
Advocating for appropriate care
Advocating for appropriate care involves ensuring that patients receive evidence-based treatments, have access to necessary resources, and are supported in their journey towards gut healing. This may involve collaborating with other healthcare professionals, providing education and resources, and advocating for necessary referrals or treatments as needed.
Empowering patients
Empowering patients with leaky gut syndrome involves providing them with the knowledge, tools, and confidence to take an active role in their own care. By fostering a therapeutic relationship built on trust and mutual respect, healthcare professionals can empower patients to make informed decisions, implement lifestyle modifications, and actively participate in their treatment plan.