You may have heard of Keratosis Pilaris, a common skin condition that causes small bumps on the skin. But did you know that nurses play an important role in providing care and management for those with this condition? From educating patients about self-care strategies to offering support and guidance, nurses are an integral part of the treatment journey for individuals with Keratosis Pilaris. In this article, we will explore the key nursing considerations and management techniques for Keratosis Pilaris, shedding light on the invaluable contributions nurses make in improving the lives of those affected.
Overview of Keratosis Pilaris
Keratosis Pilaris (KP) is a common skin condition characterized by small, rough bumps on the skin, typically on the upper arms, thighs, cheeks, or buttocks. It often presents as a mild, non-inflammatory condition, but can sometimes cause itchiness or discomfort. In some cases, KP may also be associated with dry skin or other dermatological conditions. The condition is estimated to affect up to 50% of adolescents and approximately 40% of adults.
Definition and Prevalence
Keratosis Pilaris is a benign, hereditary condition that results in the accumulation of keratin around the hair follicles. This buildup forms small, red or flesh-colored bumps that have a rough texture. These bumps are caused by the inflammation of the hair follicles and can sometimes be mistaken for acne or other skin conditions. While KP can occur at any age, it is most commonly seen in children, adolescents, and young adults. It is also more prevalent in individuals with dry skin or those with a family history of the condition.
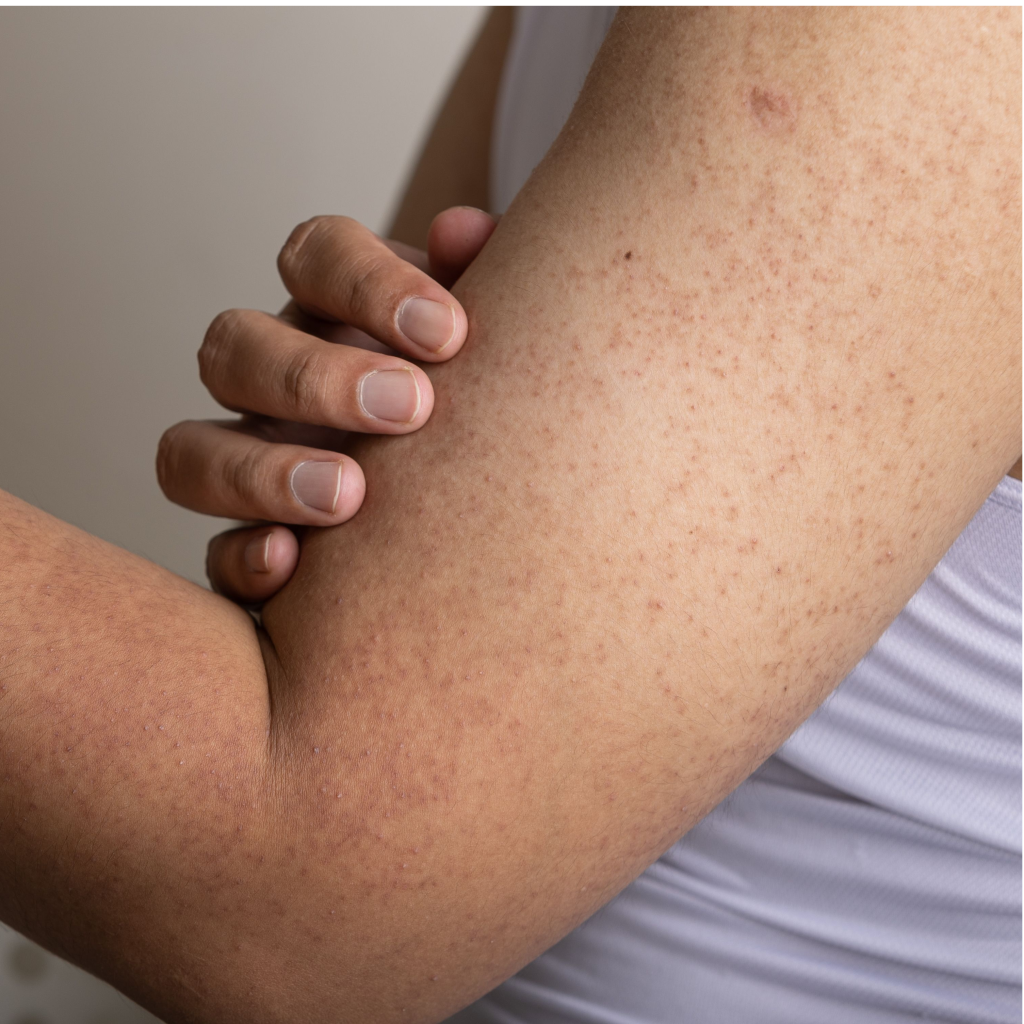
Etiology and Risk Factors
The exact cause of Keratosis Pilaris is not fully understood, but both genetic and environmental factors are believed to contribute to its development. The condition is thought to be associated with an overproduction of keratin, a protein that helps protect the skin. When this keratin builds up around the hair follicles, it leads to the formation of the characteristic bumps seen in KP. In addition to genetic factors, certain skin conditions such as eczema or dry skin can make individuals more susceptible to developing KP. Other risk factors include a history of atopic dermatitis, obesity, and a family history of the condition.
Clinical Presentation
Keratosis Pilaris typically presents as small, rough bumps that are often described as feeling like “goosebumps” or “sandpaper.” These bumps are usually painless and may have a red or flesh-colored appearance. The most common sites for KP include the upper arms, thighs, buttocks, and cheeks. The condition is generally non-inflammatory, but in some cases, the affected areas may become itchy or inflamed. KP is usually asymptomatic, but its appearance can often cause emotional distress or self-consciousness, especially in individuals with more severe cases.
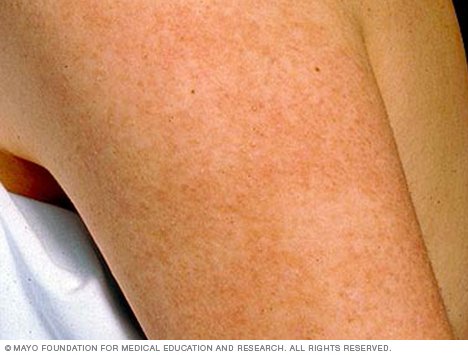
Assessment and Diagnosis
Physical Examination
Diagnosing Keratosis Pilaris is usually based on a physical examination of the affected areas. A healthcare professional will evaluate the appearance of the bumps, as well as the distribution and symmetry of the lesions. The skin may be gently palpated to assess for any signs of inflammation or tenderness. It is important to differentiate KP from other similar skin conditions, such as acne or folliculitis. Additionally, healthcare providers may assess for any associated dryness or signs of atopic dermatitis, as these can help confirm the diagnosis of KP.
Differential Diagnosis
The differential diagnosis for Keratosis Pilaris includes conditions such as acne vulgaris, folliculitis, and eczema. Acne vulgaris is characterized by the presence of comedones (whiteheads and blackheads) and inflammatory papules and pustules. Folliculitis, on the other hand, results from inflammation or infection of the hair follicles and presents as small, red bumps filled with pus. Eczema, or atopic dermatitis, is a chronic inflammatory condition characterized by dry, itchy skin and may also manifest with rough bumps. Distinguishing these conditions from KP is important for proper management and treatment.
Diagnostic Tests
In most cases, diagnostic tests are not necessary to confirm the diagnosis of Keratosis Pilaris. However, in rare instances where the presentation is atypical or there is diagnostic uncertainty, a skin biopsy may be performed. This involves the removal of a small sample of the affected skin for microscopic examination. A biopsy can help rule out other skin conditions and assist in confirming the diagnosis of KP. It is important to note that this procedure is generally reserved for cases where a definitive diagnosis cannot be reached through physical examination alone.
Patient Education and Counseling
Explaining Keratosis Pilaris
When providing patient education about KP, it is essential to explain the nature of the condition and its benign nature. Patients should understand that KP is a common and harmless condition that does not pose any significant health risks. It is important to reassure individuals that the bumps associated with KP are not contagious and do not result from poor hygiene. Educating patients about the prevalence of KP and its hereditary nature can help reduce any feelings of embarrassment or self-consciousness.
Managing Expectations
It is crucial to manage patient expectations regarding the treatment outcomes for Keratosis Pilaris. While there is no cure for KP, various treatment options can help improve the appearance and texture of the skin. However, it is important to note that the effectiveness of these treatments may vary depending on the individual. Setting realistic expectations and discussing the potential for recurrence or periods of exacerbation can prevent patients from becoming disillusioned or frustrated with the management of their condition.
Treatment Options
There are several treatment options available for managing Keratosis Pilaris. The choice of treatment will depend on the severity of the condition, the patient’s preferences, and the presence of any associated symptoms. Some common treatment modalities include topical creams and lotions, oral medications, lifestyle modifications, and nutritional considerations. Patient counseling should involve discussing the benefits, risks, and expected outcomes of each treatment option to help patients make informed decisions that align with their individual goals and preferences.

Skin Care Management
Moisturization
One of the key aspects of managing Keratosis Pilaris is maintaining optimal skin hydration. Regular and adequate moisturization can help prevent the buildup of dry skin cells around the hair follicles, thereby reducing the severity of KP. Emollient creams and lotions that contain humectants, such as urea or glycerin, can be applied to the affected areas. It is advisable to apply moisturizers immediately after bathing, when the skin is still slightly damp, to maximize absorption and effectiveness.
Exfoliation
Gentle exfoliation can be beneficial in managing the rough texture associated with Keratosis Pilaris. However, it is important to avoid excessive scrubbing or harsh exfoliants, as these can irritate the skin and potentially worsen KP. Physical exfoliation with a soft washcloth or a gentle scrub can help remove dead skin cells and promote a smoother skin texture. Additionally, chemical exfoliation with alpha-hydroxy acids or salicylic acid can help to break down the keratin plugs and improve the appearance of the affected areas.
Cleansing
Proper cleansing practices are essential for individuals with Keratosis Pilaris. It is important to use mild, non-drying cleansers that are free from harsh chemicals or fragrances. Harsh soaps or cleansers can strip the skin of its natural moisture, leading to dryness and potentially exacerbating KP. Moreover, hot water should be avoided, as it can further dry out the skin and increase the risk of irritation. Gently patting the skin dry after washing is preferable over rubbing, as excessive friction can irritate the already sensitive areas.
Pharmacological Interventions
Topical Creams and Lotions
Topical creams and lotions can play a significant role in the management of Keratosis Pilaris. These products often contain ingredients such as urea, lactic acid, or ammonium lactate, which help to moisturize the skin and promote gentle exfoliation. These ingredients work by softening and loosening the keratin plugs, thereby reducing the appearance of the bumps associated with KP. It is important to educate patients on the correct application technique, frequency, and potential side effects (such as mild skin irritation) of these topical treatments.
Oral Medications
In more severe cases or when topical treatments have not provided satisfactory results, oral medications may be considered. Oral retinoids, such as isotretinoin, can help regulate skin cell turnover and reduce the production of keratin. However, these medications are typically reserved for more severe cases of KP and require close monitoring due to their potential side effects. Patients prescribed oral medications should be educated about the risks and benefits, as well as the need for regular follow-up appointments to monitor treatment response and any adverse effects.

Non-Pharmacological Interventions
Lifestyle Modifications
Certain lifestyle modifications can help manage and prevent flare-ups of Keratosis Pilaris. It is important to avoid picking or scratching at the affected areas, as this can lead to further inflammation or infection. Additionally, wearing loose-fitting clothing made from breathable fabrics can help reduce friction and irritation. Regular exercise and maintaining a healthy diet can also contribute to overall skin health, as these practices can help improve circulation and provide essential nutrients to the skin.
Nutritional Considerations
While there is no specific diet that can cure or prevent Keratosis Pilaris, maintaining a balanced and nutritious diet can support overall skin health. A diet rich in vitamins, minerals, and antioxidants can help strengthen the skin and reduce the likelihood of dryness or inflammation. Encouraging individuals with KP to consume foods high in omega-3 fatty acids, such as fatty fish or flaxseeds, may also be beneficial, as these nutrients have anti-inflammatory properties that can potentially improve the appearance of the skin.
Psychosocial Support
The impact of Keratosis Pilaris on an individual’s emotional well-being should not be underestimated. The condition, particularly when it affects visible areas of the body, can result in self-consciousness, embarrassment, or social anxiety. Providing psychosocial support to individuals with KP is essential in helping them cope with the emotional aspects of the condition. Encouraging open communication, offering reassurance, and providing resources for support groups or counseling can help individuals develop strategies to manage any negative emotions associated with their skin appearance.
Monitoring and Evaluation
Assessing Treatment Response
Regular monitoring and evaluation are important in determining the effectiveness of the chosen treatment modalities for Keratosis Pilaris. Patients should be advised to track any changes in the appearance or texture of their skin and report these findings to their healthcare provider. Comparing photographs taken before and during treatment can assist in objectively assessing treatment response. Additionally, patients should be regularly assessed for any associated symptoms, such as itchiness or inflammation, to ensure that the chosen treatment is adequately managing the condition.
Monitoring for Complications
While Keratosis Pilaris is generally a benign condition, monitoring for potential complications is still important, especially in severe or persistent cases. Individuals with KP may be at a higher risk for developing secondary skin infections, such as cellulitis or impetigo, due to scratching or picking at the affected areas. Regular skin assessments should be conducted to evaluate for any signs of infection, such as redness, warmth, swelling, or pus. Prompt recognition and treatment of any complications can help prevent further complications and promote skin healing.
Collaborative Management
Consultations and Referrals
Collaborative management of Keratosis Pilaris may involve consultations or referrals to other healthcare professionals, depending on the specific needs of the patient. Dermatologists can provide specialized expertise in the diagnosis and management of skin conditions, including Keratosis Pilaris. Additionally, individuals with severe or refractory cases of KP may benefit from consultation with a dermatologist to explore further treatment options, such as laser therapy or prescription-strength medications. Collaboration with a mental health professional may also be beneficial for individuals experiencing significant psychological distress associated with their skin appearance.
Interdisciplinary Care
Interdisciplinary care involving various healthcare professionals can contribute to comprehensive management of Keratosis Pilaris. Nurses can play a pivotal role in providing patient education, counseling, and monitoring treatment response. Pharmacists can provide expertise in medication management, addressing any concerns or potential drug interactions. Collaborative care involving nurses, dermatologists, pharmacists, and other healthcare professionals can ensure a holistic approach to the management of KP, taking into account both the physical and emotional aspects of the condition.
Quality Improvement
Standardizing Care Protocols
Standardizing care protocols for the assessment, diagnosis, and management of Keratosis Pilaris can contribute to improved patient outcomes and satisfaction. Developing standardized guidelines or algorithms for healthcare professionals can help ensure consistency in the evaluation and treatment of KP. These protocols can include recommendations for the use of specific diagnostic criteria, treatment algorithms, and follow-up schedules. Regular review and updating of these protocols based on the latest evidence can help optimize care and promote best practices for individuals with Keratosis Pilaris.
Patient Outcomes and Satisfaction
Monitoring patient outcomes and satisfaction is crucial in evaluating the effectiveness of the provided care for Keratosis Pilaris. Collecting and analyzing data on patient-reported outcomes, such as changes in the severity of symptoms or emotional well-being, can help measure the impact of interventions. Patient satisfaction can be assessed through surveys or feedback questionnaires, allowing healthcare providers to identify areas for improvement or address any concerns. Regularly evaluating patient outcomes and satisfaction can guide quality improvement initiatives and the delivery of patient-centered care.
Ethical Considerations
Informed Consent
Respecting the principles of autonomy and informed consent is essential when managing Keratosis Pilaris. Healthcare providers should obtain informed consent from patients before initiating any diagnostic or treatment interventions. This involves providing patients with clear and accurate information about the nature of their condition, the available treatment options, and any potential risks or side effects. Ensuring patients have access to comprehensive information allows them to make informed decisions regarding their care and actively participate in the management of their condition.
Patient Confidentiality
Maintaining patient confidentiality is a fundamental ethical consideration when managing Keratosis Pilaris. Personal health information should be handled with the utmost care and stored securely to prevent unauthorized access or disclosure. Healthcare providers have a legal and professional obligation to safeguard patient information and adhere to applicable privacy laws. Respecting patient privacy and confidentiality helps foster trust and ensures that individuals can disclose sensitive skin concerns without fear of judgment or breach of confidentiality.
In conclusion, Keratosis Pilaris is a common and typically benign skin condition characterized by small, rough bumps on the skin. It can cause physical discomfort and emotional distress for many individuals. Nursing considerations for Keratosis Pilaris involve a comprehensive approach that includes patient education and counseling, skin care management, pharmacological and non-pharmacological interventions, as well as monitoring and evaluation. Collaborative management and a focus on quality improvement ensure the provision of patient-centered care. Ethical considerations, such as informed consent and patient confidentiality, are also essential to uphold throughout the management of Keratosis Pilaris. By implementing these nursing considerations, healthcare professionals can effectively support individuals with Keratosis Pilaris in managing their condition and improving their overall well-being.