You have just been assigned a patient with a lipoma, a common benign tumor made up of fat cells. As a nurse, it is important to understand the nursing considerations and management strategies for lipoma. This article will provide you with essential information on how to care for and support your patient with a lipoma, ensuring their comfort and well-being throughout their journey.

Definition and Overview of Lipoma
Definition of Lipoma
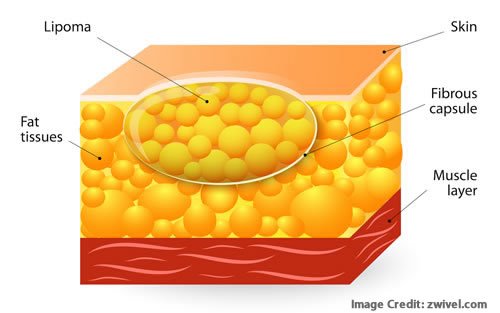
A lipoma is a benign tumor composed of fatty tissue that grows slowly under the skin. It is the most common type of soft tissue tumor, with a characteristic soft, rubbery texture. Lipomas are usually painless and can occur anywhere on the body, but they are most commonly found on the neck, shoulders, back, and arms. These tumors are typically small, ranging from a few millimeters to several centimeters in size. While lipomas are generally harmless, they can cause discomfort or concern due to their appearance.
Clinical Presentation
Lipomas are usually detected by the patient or healthcare provider as a soft, movable lump under the skin. They are typically painless but can sometimes cause tenderness, especially if they grow larger or press on nearby structures. Lipomas can vary in size, shape, and consistency, but they are generally well-defined and encapsulated. In some cases, multiple lipomas may be present, a condition known as familial multiple lipomatosis. In rare instances, lipomas can become larger and deeper, requiring further evaluation to rule out more serious conditions.
Causes of Lipoma
The exact cause of lipomas is not fully understood, but there are several factors that may contribute to their development. Genetic predisposition may play a role, as certain families have been found to have a higher incidence of lipomas. Trauma to the affected area has also been reported as a potential trigger for lipoma formation. Additionally, hormonal imbalances and metabolic disorders, such as adiposis dolorosa and Madelung’s disease, have been associated with lipoma development. However, for the majority of cases, the cause remains unknown.
Prevalence
Lipomas are common, occurring in approximately 1% of the population. They can develop at any age but are most frequently seen in middle-aged and older adults. Lipomas are slightly more common in men than in women. While lipomas can occur in people of any race or ethnicity, some studies suggest a higher prevalence in certain populations, such as those of European descent. Overall, lipomas are considered benign tumors and do not pose a significant health risk.
Nursing Assessment for Lipoma
Patient History
When assessing a patient with a lipoma, it is important to gather a comprehensive patient history. This includes information on the duration and characteristics of the lipoma, any changes in size or appearance, and any associated symptoms or discomfort. It is also essential to inquire about the patient’s medical history, including any previous surgeries, family history of lipomas or other tumors, and any underlying medical conditions that may be related to the lipoma. Additionally, the nurse should ask about the patient’s feelings and concerns related to the lipoma to provide appropriate emotional support.
Physical Examination
A thorough physical examination is crucial when assessing a lipoma. The nurse should inspect and palpate the lipoma, noting its size, shape, texture, and mobility. It is important to assess for any signs of inflammation, redness, warmth, or tenderness, which may indicate an infection or other complications. The nurse should also evaluate the surrounding skin and assess for any changes or abnormalities. Additionally, a full body examination should be performed to identify any other lipomas or potential signs of syndromes associated with multiple lipomas.
Diagnostic Tests
In most cases, lipomas can be diagnosed based on their characteristic appearance and physical examination findings. However, if there are any concerns about the lipoma or if it presents atypically, further diagnostic tests may be performed. These tests may include imaging studies, such as ultrasound or magnetic resonance imaging (MRI), which can help differentiate the lipoma from other tumors or structures. A biopsy may also be considered if there is uncertainty about the diagnosis or if there are features that raise suspicion for a more serious condition. The decision for further testing should be made in consultation with the healthcare provider.

Psychosocial Considerations
Patient Education and Counseling
When caring for a patient with a lipoma, it is important to provide education and counseling about the condition. This includes explaining the benign nature of the tumor and reassuring the patient that it is not cancerous. Providing information on the common presentation, growth pattern, and treatment options can help alleviate any concerns or anxiety the patient may have. It is also essential to address any questions or misconceptions the patient may have and provide resources for further information or support.
Body Image Concerns
Lipomas, especially when located in visible areas, can sometimes cause body image concerns for patients. They may feel self-conscious or worry about how the lipoma affects their appearance. As nurses, it is crucial to address these concerns empathetically and provide support and reassurance. Patients can be encouraged to express their feelings and emotions regarding the lipoma, and counseling or referral to a mental health professional may be appropriate if body image concerns significantly impact the patient’s well-being.
Impact on Quality of Life
Although lipomas are generally benign and do not cause significant health problems, they can still impact a patient’s quality of life. Patients may experience discomfort, limited range of motion, or interference with daily activities, especially if the lipoma is large or located in a sensitive area. It is important for nurses to assess and address these impacts on the patient’s quality of life and provide appropriate interventions or referrals as needed. Physical therapy, pain management techniques, or support from occupational therapists may be beneficial for certain patients.
Potential Complications
Rapid Growth or Size Increase
Most lipomas grow slowly over time, but in rare cases, they may experience rapid growth or increase in size. This sudden change in the lipoma’s characteristics may raise concerns about malignancy or infection. It is important for nurses to be alert to any changes in the lipoma’s appearance and promptly report them to the healthcare provider. Further evaluation, such as biopsy or imaging studies, may be necessary to rule out any underlying pathology.
Pain or Discomfort
While lipomas are typically painless, they can cause discomfort if they grow larger or press on nearby tissues or nerves. Patients may experience dull aching, tenderness, or limited mobility in the affected area. It is important for nurses to assess and manage any pain or discomfort associated with the lipoma. This may involve providing pain medications, advising the patient on positioning or activities that alleviate discomfort, or referring the patient to a pain management specialist if necessary.
Cosmetic Concerns
The appearance of a lipoma can sometimes cause cosmetic concerns for patients, especially if it is located in a visible area or grows to a larger size. Patients may feel self-conscious or uncomfortable with their appearance, impacting their self-esteem and confidence. Nurses can provide emotional support and offer resources or referrals to address these cosmetic concerns. This may include consultation with a plastic surgeon or discussion of treatment options such as surgical removal or liposuction.
Malignant Transformation
While lipomas are benign tumors, there have been rare reports of lipomas transforming into malignant tumors, such as liposarcoma. These cases are extremely uncommon, but it is important for healthcare providers and nurses to be aware of the possibility. Any changes in the lipoma’s characteristics, rapid growth, or new symptoms should be promptly evaluated to rule out malignancy. Collaboration with the healthcare team is crucial in determining the appropriate course of action and ensuring timely and appropriate management.

Medical Management of Lipoma
Watchful Waiting
In most cases, lipomas do not require treatment and can be managed through watchful waiting. This approach involves monitoring the lipoma’s size and characteristics over time and assessing for any changes or complications. Regular follow-up visits with the healthcare provider can help ensure the lipoma remains stable and does not cause any significant problems. Educating the patient about the need for ongoing monitoring and addressing any concerns can help alleviate anxiety and promote patient engagement in self-care.
Surgical Removal
Surgical removal, also known as excision, is a common treatment option for lipomas that cause symptoms, discomfort, or cosmetic concerns. It involves removing the entire lipoma and its capsule through an incision in the skin. The surgery is usually performed under local anesthesia, and the patient can typically go home the same day. Surgical removal is generally considered safe and effective, with low rates of recurrence. Patients should be educated about the procedure, potential risks, and expected recovery to make informed decisions about their treatment options.
Liposuction
Liposuction is a minimally invasive technique that can be used to remove lipomas. It involves inserting a thin tube, called a cannula, into the lipoma and using suction to remove the fatty tissue. Liposuction is particularly useful for larger lipomas or lipomas located in delicate or difficult-to-reach areas. It generally results in smaller incisions, less scarring, and faster recovery compared to surgical excision. However, liposuction may not be appropriate for all lipomas, and the decision to use this technique should be made in consultation with the healthcare provider and surgeon.
Other Treatment Options
In some cases, alternative treatment options may be considered for lipomas that are not amenable to surgical removal or liposuction. These can include steroid injections to reduce the lipoma’s size or symptoms, radiation therapy to shrink the lipoma, or cryolipolysis (freezing therapy) to destroy the fatty tissue. However, it is essential to note that these alternative treatments have limited evidence and may carry the risk of complications or side effects. Close collaboration with the healthcare provider and a thorough understanding of the risks and benefits are necessary when exploring these options.
Nursing Interventions for Lipoma
Providing Emotional Support
Caring for a patient with a lipoma entails providing emotional support throughout the diagnosis, treatment, and management process. Patients may experience anxiety, worry, or fear related to the lipoma’s appearance, potential complications, or impact on their daily lives. Nurses can offer a listening ear, validate the patient’s concerns, and provide reassurance and encouragement. Engaging in empathetic communication can help alleviate patient anxiety and promote a trusting relationship that fosters patient empowerment and engagement in self-care.
Assisting with Decision-Making
When a patient is faced with treatment options for their lipoma, nurses play a crucial role in assisting with informed decision-making. This involves providing detailed explanations of the available treatment options, discussing the benefits, risks, and potential outcomes, and addressing any questions or concerns the patient may have. The nurse can help the patient weigh the pros and cons of each option and provide support throughout the decision-making process. Shared decision-making can foster a collaborative relationship between the nurse and the patient, ensuring that the chosen treatment aligns with the patient’s preferences and goals.
Monitoring for Complications
While lipomas are generally benign, it is important to monitor for any potential complications or changes in the lipoma’s characteristics. Nurses should regularly assess the lipoma during follow-up visits, noting any new symptoms, rapid growth, or signs of infection. Any concerning findings should be promptly reported to the healthcare provider for further evaluation and appropriate management. By staying vigilant and proactive, nurses can contribute to early detection and timely intervention, minimizing the risk of complications associated with lipomas.
Educating the Patient about Self-Care
Patient education is vital in promoting self-care and empowering patients to actively participate in managing their lipomas. Nurses can provide information on how to monitor the lipoma for any changes and when to seek further medical attention. Patients should be educated on proper wound care if they undergo surgical removal, including dressing changes, signs of infection, and regular follow-up visits. Additionally, patients can be advised on lifestyle modifications, such as maintaining a healthy weight and staying physically active, which may help prevent the development or growth of new lipomas.
Post-Operative Nursing Care
Assessment of Surgical Site
After surgical removal of a lipoma, nurses play a crucial role in assessing the surgical site for any signs of complications or infection. The nurse should monitor the incision for redness, swelling, drainage, or separation, which may indicate an infection or delayed wound healing. In addition to visual assessment, the nurse should also assess the patient’s pain level and comfort, noting any changes that may require further intervention or pain management.
Wound Care
Proper wound care is essential to promote healing and prevent complications after lipoma removal surgery. Nurses should provide instructions to the patient on how to care for the incision site, including keeping the area clean and dry, applying prescribed dressings or ointments, and avoiding any activities that may disrupt the wound. Patients should also be educated on signs of infection or delayed wound healing and instructed to report any concerning symptoms to the healthcare provider. Regular follow-up visits with the nurse or healthcare provider can help ensure proper wound healing and detect any complications early.
Pain Management
Pain management is an integral part of post-operative nursing care for patients who undergo lipoma removal surgery. Nurses should assess the patient’s pain level using appropriate pain assessment tools and administer prescribed pain medications as needed. Non-pharmacological pain management techniques, such as relaxation exercises or positioning, can also be utilized to help alleviate the patient’s discomfort. Educating the patient about pain management strategies and providing ongoing support can contribute to a more comfortable recovery experience for the patient.
Complication Monitoring
Although complications after lipoma removal surgery are uncommon, it is important for nurses to monitor for any signs of infection, bleeding, or other complications. Regular assessments of the surgical site, vital signs, and overall patient condition are necessary to detect any concerning changes. Nurses should educate patients on the signs and symptoms of potential complications and encourage them to report any abnormalities promptly. Collaboration with the healthcare provider is crucial to ensure timely intervention and appropriate management of any post-operative complications.
Promoting Self-Care and Coping Strategies
Educating the Patient about Post-Operative Care
After lipoma removal surgery, nurses play a vital role in educating the patient about post-operative care and promoting self-care. Patients should be informed about activities to avoid during the recovery period, such as heavy lifting or strenuous exercise, to prevent wound disruption or complications. Nurses should provide detailed instructions on wound care, dressing changes, and signs of infection, emphasizing the importance of proper hygiene and following the healthcare provider’s recommendations. By providing clear and concise information, nurses can empower patients to actively participate in their own recovery process.
Encouraging Physical Activity
Physical activity is an important component of overall health and well-being, and it can also play a role in preventing the development or growth of new lipomas. Nurses can encourage patients to engage in regular physical activity, such as walking or aerobic exercises, to maintain a healthy weight and reduce the risk of lipoma formation or recurrence. By promoting physical activity, nurses can support patients in adopting a healthy lifestyle and contribute to their long-term well-being.
Discussing Body Image Concerns
Patients with lipomas, especially those located in visible areas, may have body image concerns that can impact their self-esteem and psychological well-being. Nurses can provide a safe and supportive environment for patients to discuss their feelings and concerns about body image. By actively listening, showing empathy, and offering validation, nurses can help patients cope with these concerns and develop strategies to enhance their self-image. Referral to mental health professionals or support groups specializing in body image issues may be appropriate for patients who require additional support.
Referring to Support Groups or Resources
Support groups or resources can play a valuable role in helping patients cope with lipoma-related concerns and challenges. Nurses can provide information and referrals to support groups or online forums where patients can connect with others who have experienced similar experiences. These resources can provide emotional support, guidance, and a sense of community for patients. By connecting patients with support resources, nurses play a pivotal role in enhancing the patient’s overall well-being and promoting a sense of empowerment and resilience.

Collaboration with other Healthcare Professionals
Consultation with Surgeons
Collaboration with surgeons is essential in the assessment and management of lipomas. Nurses can work closely with surgeons to ensure a comprehensive evaluation of the lipoma and determine the most appropriate treatment options for the patient. By communicating and sharing information effectively, nurses can contribute to a multidisciplinary approach that optimizes patient outcomes.
Referral to Plastic Surgeon
For patients with lipomas that cause significant cosmetic concerns or are located in aesthetically sensitive areas, referral to a plastic surgeon may be appropriate. Plastic surgeons specialize in techniques that can minimize scarring, improve cosmetic outcomes, and address any concerns related to body image. Nurses can facilitate the referral process, educate patients on the potential benefits of plastic surgery, and provide ongoing support and information throughout the patient’s journey.
Involvement of Mental Health Professionals
Patients with lipomas, particularly those with body image concerns or significant psychological distress, may benefit from the involvement of mental health professionals. Psychologists or counselors can provide additional emotional support, assist patients in developing coping strategies, and address any underlying psychological issues. Nurses can collaborate with mental health professionals to ensure a holistic approach to patient care and to promote the patient’s overall well-being.
Coordination with Patient’s Primary Care Provider
Coordination with the patient’s primary care provider is essential in providing comprehensive care for patients with lipomas. Nurses can communicate with the primary care provider to ensure continuity of care, share relevant information, and update the patient’s medical records. This collaboration supports effective management of the lipoma and any underlying medical conditions or comorbidities, ensuring that the patient’s overall health is appropriately addressed.
Evidence-Based Practice and Research
Current Recommendations for Lipoma Management
The management of lipomas is primarily based on clinical experience and expert opinion, as there is a limited amount of high-quality research in this area. Current recommendations for lipoma management focus on watchful waiting for asymptomatic lipomas and surgical removal for symptomatic lipomas, significant cosmetic concerns, or lipomas causing functional impairment. However, further research is needed to assess the effectiveness of alternative treatments and to optimize the management of lipomas in specific populations or clinical scenarios.
Ongoing Research and Future Directions
Research on lipomas is currently limited but growing. Ongoing studies aim to improve the understanding of the underlying mechanisms of lipoma formation, identify potential risk factors or genetic markers, and explore novel treatment modalities. Future research endeavors may focus on the development of targeted therapies that can selectively shrink or eliminate lipomas without the need for surgical intervention. Additionally, studies investigating the long-term outcomes and recurrence rates of lipoma management strategies may help refine current guidelines and improve patient care.
In conclusion, lipomas are benign tumors composed of fatty tissue that typically grow slowly under the skin. They are common and usually present as soft, movable lumps that are often asymptomatic. However, lipomas can cause discomfort or concern due to their size, location, or impact on body image. Nursing assessment for lipoma includes obtaining a comprehensive patient history, performing a thorough physical examination, and considering diagnostic tests if necessary. Psychosocial considerations, potential complications, and medical and nursing management strategies should be addressed to provide holistic and patient-centered care. Collaboration with other healthcare professionals, promoting self-care and coping strategies, and staying informed about evidence-based practice and ongoing research are crucial in delivering the best possible care for patients with lipomas.