Are you a nurse looking to expand your knowledge on nonallergic rhinitis? Look no further! In this article, we will discuss the nursing considerations and management strategies for nonallergic rhinitis. Nonallergic rhinitis is a condition characterized by symptoms similar to allergies, such as a runny or stuffy nose, sneezing, and nasal congestion, but it is not triggered by allergens. As a nurse, understanding the specific considerations and management techniques for nonallergic rhinitis is essential in providing effective care and support to your patients. So, let’s dive into the world of nonallergic rhinitis and explore the nursing considerations that can greatly impact patient outcomes.
Assessment
History of symptoms
In order to effectively manage nonallergic rhinitis, a thorough assessment of the patient’s history of symptoms is essential. By understanding the timeline and characteristics of the symptoms, healthcare professionals can better tailor the treatment plan to meet the specific needs of the individual. It is important to inquire about the frequency and duration of symptoms such as nasal congestion, sneezing, and postnasal drip. Additionally, asking about the presence of any triggers, such as environmental factors or certain activities, can provide valuable insights into the underlying causes of the symptoms.
Physical examination
After obtaining a comprehensive history of symptoms, a physical examination is necessary to assess the nasal passages and surrounding structures. During the examination, healthcare professionals will evaluate the presence of nasal congestion, redness, and swelling. They may also use a nasal speculum to inspect the nasal cavity for any abnormalities or signs of inflammation. Taking note of these findings will aid in determining the severity and impact of nonallergic rhinitis on the patient’s overall health and well-being.
Allergy testing
Although nonallergic rhinitis is not caused by an allergic response, it is important to rule out any underlying allergies that may be contributing to the symptoms. Allergy testing can help identify specific allergens that trigger allergic reactions, which can often present with similar symptoms to nonallergic rhinitis. Skin prick tests and blood tests are commonly used to identify allergens such as pollen, dust mites, and pet dander. By differentiating between allergic and nonallergic triggers, healthcare professionals can provide more targeted treatment plans.
Identifying triggers
Identifying the triggers that exacerbate nonallergic rhinitis symptoms is crucial for effective management. Triggers can vary from person to person, but common culprits include strong odors, tobacco smoke, air pollution, temperature changes, and certain foods. It is important for healthcare professionals to guide patients in identifying their individual triggers through meticulous assessment and patient education. By gaining insight into these triggers, healthcare professionals can advise patients on appropriate lifestyle modifications and assist them in minimizing exposure to these triggers.
Education
Explaining nonallergic rhinitis
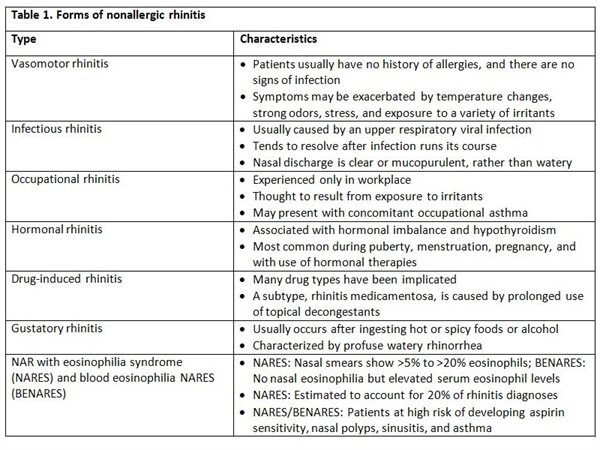
When working with patients diagnosed with nonallergic rhinitis, it is vital to educate them about the nature of their condition. Nonallergic rhinitis is a chronic inflammatory disorder that is not caused by allergens but can present with similar symptoms to allergic rhinitis. It is important to emphasize that nonallergic rhinitis is not an allergic response and therefore, will not respond to traditional allergy treatments. By providing this clear explanation, patients can better understand their condition and avoid unnecessary treatments.
Reviewing symptoms and triggers
To effectively manage nonallergic rhinitis, patients must be able to recognize their symptoms and identify triggers that worsen these symptoms. By reviewing the symptoms associated with nonallergic rhinitis, healthcare professionals can ensure patients are accurately able to recognize their condition. Additionally, discussing triggers and how they can contribute to symptom exacerbation is crucial. Patients should be encouraged to keep track of their symptoms and triggers, which will aid healthcare professionals in developing an appropriate treatment plan.
Discussing treatment options
Engaging patients in a discussion about treatment options is essential to ensure they are actively involved in their healthcare journey. When discussing treatment options for nonallergic rhinitis, healthcare professionals should explain various pharmacological and non-pharmacological interventions. Pharmacological options may include antihistamines, nasal decongestants, nasal corticosteroids, and leukotriene modifiers. Non-pharmacological interventions can include lifestyle modifications, environmental considerations, symptom relief techniques, and emotional support. By presenting a range of treatment options, healthcare professionals can individualize the care plan and promote patient adherence.
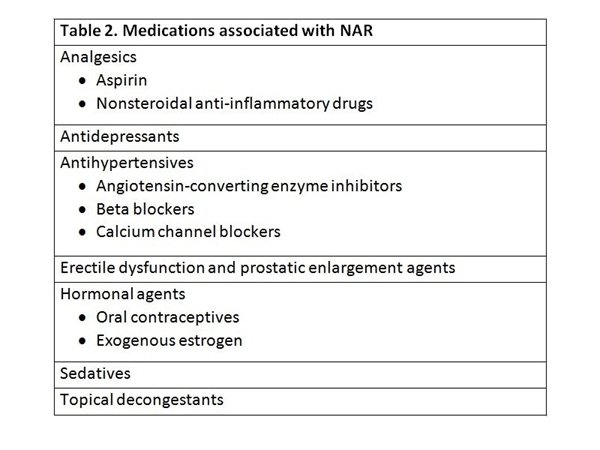
Medication Management
Antihistamines
Antihistamines are commonly used in treating allergic rhinitis, but they can also provide relief for certain symptoms of nonallergic rhinitis. These medications work by blocking the histamine receptors in the body, reducing the symptoms associated with inflammation and allergic reactions. While antihistamines may be less effective in managing nonallergic rhinitis compared to allergic rhinitis, they can still provide relief for symptoms such as sneezing and itching. Healthcare professionals should educate patients about the potential side effects of antihistamines, such as drowsiness, and guide them in choosing the most appropriate over-the-counter or prescription options.
Nasal decongestants
Nasal decongestants are another class of medications commonly used in managing nonallergic rhinitis. These medications work by constricting blood vessels in the nasal passages, reducing swelling and congestion. Nasal decongestants can provide temporary relief, particularly for nasal congestion, and are available in both oral and nasal spray forms. However, they should be used with caution, as prolonged or excessive use can lead to rebound congestion. Healthcare professionals should educate patients on the appropriate use of nasal decongestants and encourage them to limit usage to prevent dependency.
Nasal corticosteroids
Nasal corticosteroids are considered one of the most effective treatment options for nonallergic rhinitis. These medications reduce inflammation in the nasal passages, providing relief for symptoms such as congestion, sneezing, and nasal itching. Nasal corticosteroids are available as sprays and are typically used on a daily basis for optimal results. It is important for healthcare professionals to educate patients about the correct administration technique and potential side effects, such as nasal dryness or irritation. Patients should also be informed that it may take several weeks of regular use before experiencing the full benefits of this medication.
Leukotriene modifiers
Leukotriene modifiers are medications that work by blocking the action of leukotrienes, inflammatory chemicals involved in various allergic and inflammatory conditions. While their role in treating nonallergic rhinitis is still being researched, they may be considered as an option for patients who do not respond well to other treatments. It is important for healthcare professionals to discuss with patients the potential benefits and limitations of leukotriene modifiers, as well as any potential side effects. Individualized treatment plans should be developed based on patient preferences and responses to medications.
Lifestyle Modifications
Avoidance of triggers
One of the key aspects of managing nonallergic rhinitis is identifying and avoiding triggers that worsen symptoms. Healthcare professionals should educate patients on common triggers such as strong odors, air pollution, and temperature changes. By providing guidance on how to minimize exposure to these triggers, healthcare professionals can help patients proactively manage their symptoms. For example, patients can avoid using scented products, ensure proper ventilation in their living spaces, and dress appropriately for weather changes.
Humidification
Humidification can be a helpful strategy for individuals with nonallergic rhinitis, especially those who experience dry nasal passages. By increasing moisture in the air, the nasal passages can remain adequately hydrated, reducing the risk of nasal irritation. Healthcare professionals can advise patients to use humidifiers in their homes, particularly in bedrooms, to maintain a comfortable humidity level. However, it is important to remind patients to clean humidifiers regularly to prevent the growth of mold or bacteria.
Nasal irrigation
Nasal irrigation, also known as nasal douching or nasal lavage, involves flushing the nasal passages with a saline solution. This technique can help remove allergens, irritants, and excess mucus from the nasal passages, providing symptom relief for individuals with nonallergic rhinitis. Healthcare professionals can instruct patients on how to perform nasal irrigation safely and effectively using products such as neti pots or nasal irrigation kits. It is important to emphasize the importance of using distilled or sterilized water to prevent the introduction of harmful microorganisms.
Regular exercise
Regular exercise can play a significant role in managing nonallergic rhinitis. Engaging in physical activity helps improve overall cardiovascular health and immune function, potentially reducing the frequency and severity of symptoms. Healthcare professionals should encourage patients to incorporate regular exercise into their daily routines, taking care to choose activities that do not aggravate their symptoms. It is important to educate patients about the potential benefits of exercise and promote its inclusion as part of a comprehensive treatment plan.
Environmental Considerations
Reducing dust and allergens
Reducing exposure to dust and other allergens can greatly benefit individuals with nonallergic rhinitis. Healthcare professionals should provide guidance on strategies to minimize allergens in the home environment. Examples of such strategies include implementing regular cleaning routines, using allergen-proof covers on mattresses and pillows, vacuuming with high-efficiency particulate air (HEPA) filters, and removing carpeting. By minimizing exposure to these triggers, healthcare professionals can contribute to symptom reduction and improved quality of life for their patients.
Proper ventilation
Proper ventilation is essential in promoting optimal air quality and reducing the concentration of allergens and irritants in indoor spaces. Healthcare professionals can educate patients on the importance of opening windows to allow fresh air circulation and avoiding activities that contribute to poor ventilation, such as smoking indoors. Additionally, the use of air purifiers or filters can help remove allergens from the air, contributing to a healthier indoor environment.
Maintaining cleanliness
Maintaining cleanliness in living spaces can help reduce the buildup of allergens and irritants that can worsen nonallergic rhinitis symptoms. Healthcare professionals should emphasize the importance of regular dusting, cleaning of surfaces, and vacuuming to prevent the accumulation of allergens. Furthermore, ensuring that bedding and linens are cleaned regularly can also contribute to a cleaner environment and alleviate symptoms.
Avoiding smoke exposure
Exposure to smoke, whether from tobacco or wood-burning sources, can exacerbate symptoms of nonallergic rhinitis. Healthcare professionals should educate patients on the risks associated with smoke exposure and encourage them to avoid smoking or being around smokers. Additionally, individuals who have wood-burning fireplaces or stoves should be advised to take appropriate precautions, such as proper ventilation or the use of alternative heating sources, to minimize smoke exposure.
Symptom Relief Techniques
Breathing exercises
Breathing exercises can provide relief for nonallergic rhinitis symptoms by promoting nasal passage clearance and reducing congestion. Healthcare professionals can teach patients various breathing techniques, such as deep breathing exercises or alternate nostril breathing, to enhance nasal airflow and alleviate symptoms. By incorporating regular breathing exercises into their daily routines, patients can experience improved nasal function and enhanced well-being.
Steam inhalation
Steam inhalation is a simple and effective method for relieving congestion and moisturizing the nasal passages. Healthcare professionals can advise patients to inhale steam from a bowl of hot water or use a facial steamer or humidifier for more targeted steam therapy. The warm, moist air can help loosen mucus and soothe irritated nasal passages. However, caution should be exercised to prevent burns or scalds.
Use of saline nasal sprays
Saline nasal sprays can provide temporary relief by moisturizing the nasal passages and helping to flush out irritants and excess mucus. Healthcare professionals can recommend over-the-counter saline sprays or demonstrate how to prepare homemade saline solutions for patients to use. It is important to emphasize the importance of using sterile water and proper technique to avoid introducing additional irritants or causing further nasal irritation.
Warm compresses
Application of warm compresses to the face can help alleviate symptoms of nonallergic rhinitis. Healthcare professionals can recommend using a warm washcloth or a microwaveable compress on the sinus areas of the face, such as the forehead, cheeks, and bridge of the nose. The warmth can help ease nasal congestion and reduce facial pressure. It is essential to remind patients to use warm, not hot, compresses to prevent burns.

Monitoring and Evaluation
Assessing symptoms regularly
Regular assessment of symptoms is crucial for monitoring the effectiveness of treatment interventions and making necessary adjustments. Healthcare professionals should encourage patients to keep track of their symptoms, either through written documentation or the use of symptom-tracking apps. By reviewing symptoms during follow-up appointments, healthcare professionals can assess the impact of treatment strategies and determine if any modifications are needed.
Monitoring medication response
For patients who are prescribed medications as part of their nonallergic rhinitis treatment, healthcare professionals should closely monitor their response to the prescribed drugs. It is important to assess if the medications are providing symptomatic relief, or if they are causing any adverse effects. Monitoring medication response allows healthcare professionals to optimize treatment plans and consider alternative medications or dosages if necessary.
Evaluating adherence to treatment plan
Patient adherence to the recommended treatment plan is essential for achieving successful management of nonallergic rhinitis. Healthcare professionals should regularly assess patient adherence and discuss any barriers or challenges that may impede compliance. Open and non-judgmental communication between healthcare professionals and patients can help identify strategies to enhance adherence and promote optimal outcomes.
Multidisciplinary Approach
Collaboration with allergists
In complex cases of nonallergic rhinitis, collaboration with allergists can provide invaluable expertise and insights. Allergists specialize in the diagnosis and management of allergies and allergic rhinitis, which can present with similar symptoms to nonallergic rhinitis. By working together, nurses and allergists can ensure a comprehensive and accurate assessment of the patient’s symptoms and triggers, leading to more tailored treatment plans.
Communication with respiratory therapists
Respiratory therapists play a vital role in managing respiratory conditions, including nonallergic rhinitis. By collaborating with respiratory therapists, nurses can enhance patient education and provide additional support in managing symptoms. Respiratory therapists can provide guidance on breathing exercises, assist in the selection and use of respiratory devices, and assess lung function to optimize treatment outcomes. Effective communication between respiratory therapists and nurses is crucial for providing holistic care to patients with nonallergic rhinitis.
Coordinating care with otolaryngologists
Otolaryngologists, also known as ear, nose, and throat (ENT) specialists, focus on the diagnosis and treatment of conditions affecting the head and neck. In certain cases of nonallergic rhinitis, coordination with otolaryngologists may be necessary to explore potential anatomical or structural causes that contribute to the symptoms. Collaboration between nurses and otolaryngologists ensures comprehensive care and allows for a multidisciplinary approach to address the needs of patients with nonallergic rhinitis.

Emotional Support
Providing emotional support
Living with nonallergic rhinitis can be challenging and may impact a patient’s emotional well-being. Nurses have a crucial role in providing emotional support to these individuals. By empathetically listening to their concerns, fears, and frustrations, nurses can validate their experiences and offer reassurance. Creating a supportive and safe space for patients to express their emotions can contribute to their overall well-being and help them navigate through the challenges associated with their condition.
Addressing patient concerns
Patients with nonallergic rhinitis may have various concerns related to their symptoms, treatment options, and the impact of their condition on their daily lives. Nurses should actively address these concerns and provide clear explanations and information to alleviate any uncertainties. By addressing patient concerns, nurses can empower patients to actively participate in their care and make informed decisions regarding their treatment.
Referring to support groups
Support groups can provide valuable resources and a sense of community for individuals with nonallergic rhinitis. Nurses should be knowledgeable about local support groups or online communities focused on nonallergic rhinitis and be prepared to provide relevant referrals. Connecting patients with these support networks can help them access additional information, gain insight from others who share similar experiences, and receive emotional support from their peers.
Promoting self-care practices
Encouraging patients with nonallergic rhinitis to engage in self-care practices is an important aspect of their holistic care. Nurses can educate patients about self-care strategies, such as stress management techniques, proper sleep hygiene, and maintaining a balanced diet. Promoting self-care practices empowers patients to take a proactive role in managing their symptoms and enhances their overall well-being.
Follow-up and Continuity of Care
Scheduling regular follow-up appointments
Regular follow-up appointments are essential for monitoring the progress of patients with nonallergic rhinitis and adjusting treatment plans as needed. Nurses should establish a follow-up schedule that is tailored to the individual patient’s needs and goals. During these appointments, healthcare professionals can assess symptom management, discuss any concerns or challenges, update medication prescriptions, and reinforce patient education. Scheduling regular follow-up appointments ensures continuity of care and ongoing support for patients with nonallergic rhinitis.
Ensuring proper medication refills
To promote medication adherence and continuity of care, nurses should ensure that patients have access to the necessary medications for managing nonallergic rhinitis. This includes monitoring medication supplies and arranging for timely refills. Nurses can provide education on appropriate medication storage and disposal and emphasize the importance of adhering to prescribed dosages. Proactive management of medication refills contributes to the overall effectiveness of treatment plans and patient satisfaction.
Maintaining continuity of care
Maintaining continuity of care is crucial for optimal management of nonallergic rhinitis. Nurses should collaborate with other healthcare providers involved in the patient’s care, such as primary care physicians, specialists, and respiratory therapists. Clear and effective communication among healthcare professionals ensures that patients receive consistent and coordinated care. Nurses play a vital role in facilitating this continuity of care by ensuring the seamless transfer of information and promoting a patient-centered approach throughout the healthcare journey.
