Are you a nurse navigating the world of plantar warts? Look no further! In this article, we will explore nursing considerations and management techniques specifically tailored for plantar warts. From identifying symptoms to implementing effective treatments, we’ve got you covered. So grab a cup of tea and let’s dive into the fascinating world of plantar warts!
Assessment
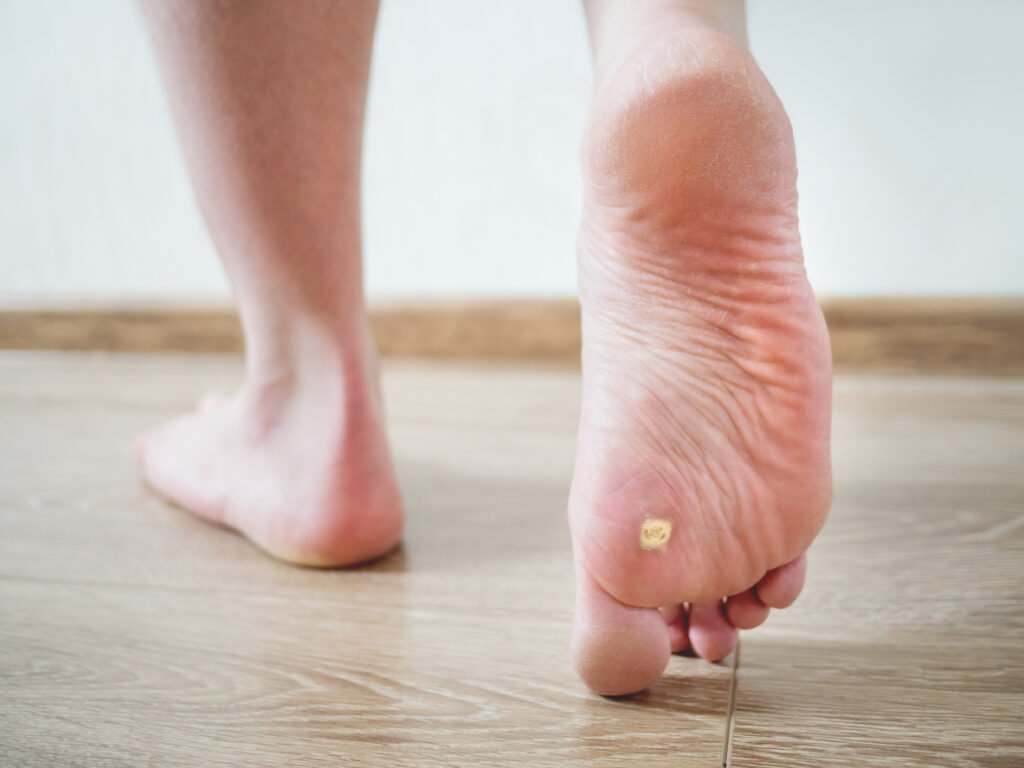
Identifying the presence of plantar warts
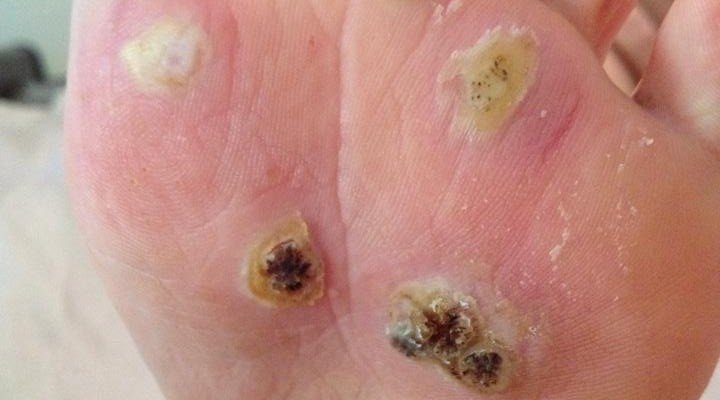
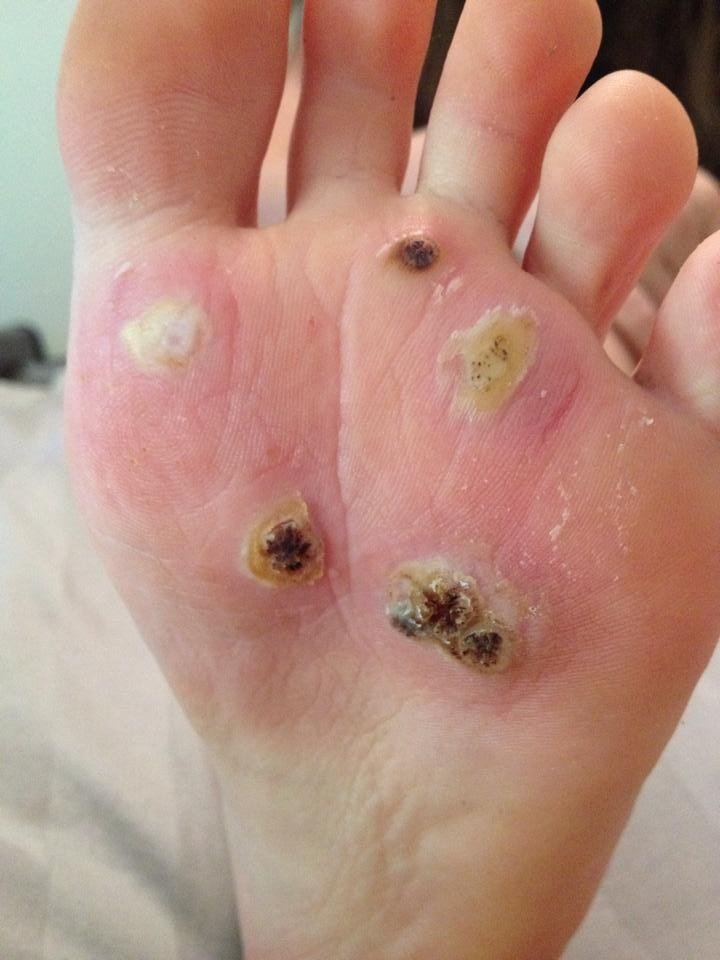
To begin the assessment, it is important to gather information about the patient’s symptoms and medical history. Ask the patient if they have noticed any small, raised bumps on the soles of their feet or experienced any discomfort while walking or standing. Plantar warts are usually flesh-colored or gray, with a rough texture and tiny black dots on the surface. These dots are actually small blood vessels which are responsible for nourishing the wart. They may also be painful or tender to the touch.
Assessing the severity and extent of plantar warts
During the assessment, it is crucial to assess the severity and extent of the plantar warts. Note the number of warts and their size, as some warts may be solitary while others may be present in clusters. Evaluate the size and depth of each wart, as larger and deeper warts may require different treatment approaches. Additionally, observe if the warts are interfering with the patient’s daily activities or causing significant pain.
Assessing the patient’s medical history and risk factors
The assessment should also include a review of the patient’s medical history and risk factors that may increase their susceptibility to plantar warts. Inquire about the patient’s current health conditions, such as immunosuppression or diabetes, as these can impact the effectiveness of treatment and overall healing process. Additionally, ask about the patient’s lifestyle habits, such as communal swimming pool usage or walking barefoot in public places, which can increase the risk of contracting plantar warts.
Diagnosis
Conducting thorough physical examination
A thorough physical examination is vital in diagnosing plantar warts accurately. Start by examining the affected area, paying close attention to the soles of the feet. Look for any raised bumps that match the description of plantar warts, noting their size, color, and texture. Take note if the warts are surrounded by calloused or thickened skin. It is important to differentiate between plantar warts and other foot conditions, such as calluses or corns, as the treatment approaches may differ.
Performing a visual inspection of the affected area
After the physical examination, a visual inspection of the affected area can provide valuable clues about the nature and severity of the plantar warts. Take note of any signs of bleeding or inflammation around the warts, as this may indicate an infection. Look for signs of itching or scratching, as excessive scratching can damage the skin and increase the risk of secondary infections. Additionally, assess the patient’s overall foot hygiene and cleanliness.
Using diagnostic aids like dermoscopy
In some cases, a dermoscopy may be used as a diagnostic aid to help visualize the plantar warts more clearly. Dermoscopy involves using a handheld device with magnification and lighting to examine the skin’s surface. This technique can help identify characteristic features of plantar warts, such as the presence of blood vessels or specific patterns. Dermoscopy can be particularly useful when dealing with challenging cases or when there is uncertainty in the clinical diagnosis.
Prevention and Education
Educating patients about the transmission and risk factors
One of the core aspects of nursing care for patients with plantar warts is education. It is crucial to provide patients with knowledge about the transmission and risk factors associated with plantar warts. Explain that plantar warts are caused by the human papillomavirus (HPV) and are highly contagious. Emphasize the importance of avoiding direct contact with warts, as well as sharing personal items such as towels or shoes. Educate patients on the risk factors, such as walking barefoot in public areas or having a weakened immune system, and discuss strategies to minimize their exposure.
Encouraging proper foot hygiene practices
To prevent the spread of plantar warts, it is essential to encourage patients to maintain proper foot hygiene. Instruct patients to wash their feet daily with mild soap and warm water, ensuring thorough cleansing of the affected areas. Remind them to dry their feet thoroughly, especially between the toes, as moisture can create an environment conducive to wart growth. Additionally, advise patients to regularly inspect their feet for any changes or signs of new warts.
Promoting the use of protective footwear
Another preventive measure against plantar warts is promoting the use of protective footwear. Encourage patients to wear comfortable, properly fitting shoes that provide adequate support and cushioning. Discourage the habit of walking barefoot in public areas, especially in places where the risk of exposure to HPV may be higher. For individuals who are particularly prone to plantar warts, suggest the use of over-the-counter foot pads or silicone sleeves to provide additional protection to vulnerable areas.
Treatment Options
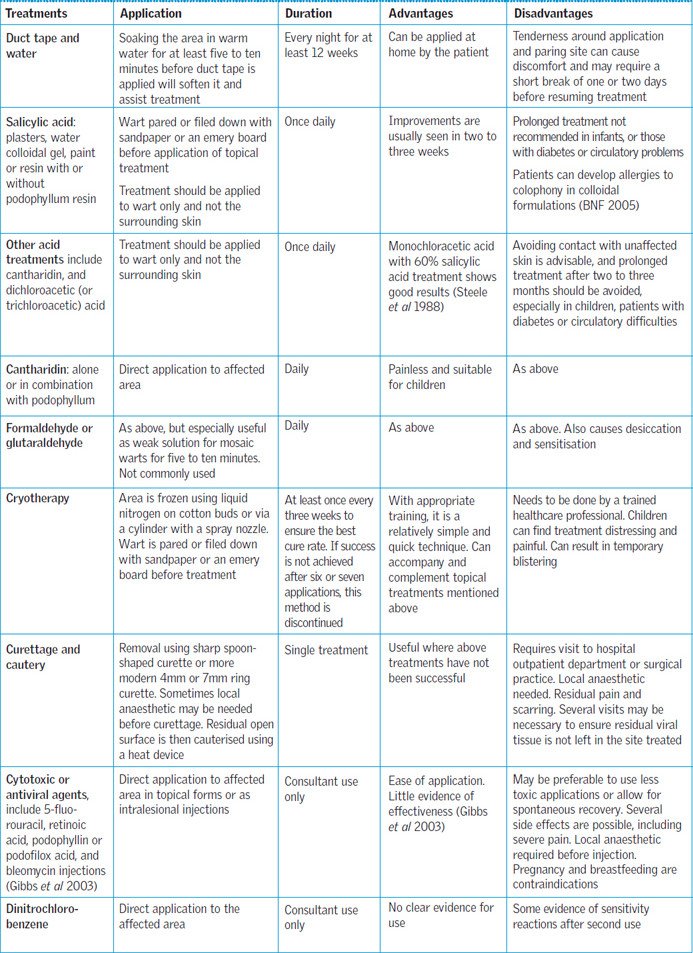
Topical treatments
Topical treatments are commonly used as the initial line of treatment for plantar warts. These treatments usually contain salicylic acid, which works by gradually breaking down the wart tissue. Instruct patients on the proper application of the topical medication, ensuring they clean and dry the affected area before treatment. Emphasize the importance of consistency, as daily application for several weeks or months may be necessary. Additionally, educate patients on common side effects, such as local skin irritation, and when to seek medical advice.
Cryotherapy
Cryotherapy involves freezing the wart tissue using liquid nitrogen or other freezing agents. The freezing temperature causes the wart to die and eventually fall off. Explain the procedure to patients, including the potential discomfort or pain during the treatment. Instruct patients to follow any necessary pre-procedure guidelines, such as avoiding aspirin or other blood-thinning medications. After the procedure, educate patients about the expected post-procedure care, including the possibility of blister formation and proper wound care.
Electrosurgery
Electrosurgery, also known as electrocautery, is a treatment option for patients with larger or more resistant plantar warts. This procedure involves using an electrically heated probe to destroy the wart tissue. Inform patients about the process, including the use of local anesthesia to numb the area. Discuss any potential risks or complications associated with electrosurgery, such as scarring or infection. After the procedure, provide detailed instructions for wound care, avoidance of excessive pressure on the treated area, and signs of possible infection.
Laser therapy
Laser therapy is a less common but effective treatment option for plantar warts that are resistant to other treatments. The laser delivers focused beams of light to destroy the wart tissue. Educate patients on the mechanism of action and expectations of the procedure. Discuss the possibility of discomfort or mild pain during the procedure, and inform patients about the necessary precautions, such as eye protection. After laser therapy, provide instructions for wound care and follow-up appointments, as multiple sessions may be required for optimal results.
Immunotherapy
Immunotherapy involves stimulating the patient’s immune system to fight against the wart-causing virus. Commonly used immunotherapy options for plantar warts include the use of immune-boosting medications or the application of immune-response modifiers directly to the warts. Educate patients about the potential benefits and limitations of immunotherapy, including the possibility of local skin reactions or flu-like symptoms. Highlight the importance of compliance with the treatment regimen and regular follow-up appointments.
Surgical excision
In some cases, surgical excision may be deemed necessary, especially if other treatment options have been unsuccessful or if the warts are causing significant pain and impairment. During surgical excision, the plantar warts are surgically removed by cutting them out or shaving them off. Inform patients about the procedure, including the need for local anesthesia and potential post-surgical care requirements. Emphasize the importance of proper wound care and the possible risks of scarring or infection.

Patient Care
Providing comfort measures for pain relief
Plantar warts can be painful, especially when they interfere with walking or standing. As a nurse, it is essential to provide patients with comfort measures to alleviate their pain. This may include suggesting over-the-counter pain relievers, applying ice packs to the affected area to reduce inflammation, or recommending the use of cushioned insoles or pads to minimize pressure on the warts.
Assisting in the application of topical treatments
Topical treatments are a common part of plantar wart treatment. As a nurse, you can assist patients by providing step-by-step instructions for the proper application of these medications. Guide patients on cleaning the affected area thoroughly, applying the medication, and covering the wart if necessary. Address any questions or concerns they may have about the treatment process or potential side effects.
Performing wound care and dressing changes
After certain treatments, such as cryotherapy or surgical excision, patients may require wound care and dressing changes. As a nurse, it is part of your role to perform these tasks and ensure proper healing. Teach patients how to clean the wound, properly apply dressings, and when to seek medical attention for signs of infection or delayed healing. Provide them with any necessary supplies and emphasize the importance of adherence to the wound care regimen.
Educating patients on self-care
Empower patients by educating them on self-care practices for plantar wart management. Teach them about proper foot hygiene, including the importance of regular washing and thorough drying, as well as avoiding picking or scratching the warts. Instruct patients on how to inspect their feet for any changes or signs of new warts. Encourage them to wear comfortable shoes with adequate support and cushioning, and advise against sharing personal items that come into contact with the feet.
Monitoring the progress of treatment
Throughout the course of treatment, it is important to monitor the progress and effectiveness of the interventions. Regularly assess the size and appearance of the warts, noting any changes or improvements. Observe if the patient’s symptoms, such as pain or discomfort, have reduced. Document any side effects or adverse reactions to treatments. Communicate any significant findings to the healthcare team, as adjustments to the treatment plan may be necessary.
Infection Control
Implementing standard precautions
When caring for patients with plantar warts, it is essential to implement standard precautions to prevent the spread of the virus. Adhere to proper hand hygiene guidelines, such as washing hands with soap and water or using alcohol-based hand sanitizers before and after coming into contact with the warts or their surrounding area. Wear gloves when performing any procedures that may involve direct contact with the warts or any potentially contaminated materials.
Practicing proper hand hygiene
Hand hygiene is crucial in infection control. Encourage patients to practice proper hand hygiene as well, especially after touching or treating their warts. Teach them the correct technique for handwashing, including using soap and water and thoroughly lathering all surfaces of the hands for at least 20 seconds. Reinforce the importance of hand hygiene in reducing the risk of infection and spreading the virus to other areas of the body or to other individuals.
Using personal protective equipment
When performing certain procedures, such as cryotherapy or electrosurgery, it may be necessary to use personal protective equipment (PPE) to minimize the risk of exposure to infectious materials. Explain the importance of wearing gloves, masks, goggles, or face shields as appropriate. Instruct patients on the proper use, storage, and disposal of PPE if they are performing self-treatments at home.
Disinfecting contaminated surfaces
As part of infection control measures, it is important to regularly disinfect any surfaces or objects that may come into contact with the plantar warts or their secretions. Use appropriate disinfectants and follow manufacturer instructions for dilution, contact time, and safety precautions. Emphasize the need for routine cleaning of shared surfaces, such as bathroom floors or shower mats, which may contribute to the transmission of the virus.
Complications
Identifying potential complications
Although plantar warts are generally harmless, certain complications may arise in certain situations. Promptly identify and assess these potential complications to ensure timely intervention. Some possible complications include infection, cellulitis, ulceration, or nerve compression. Monitor patients for signs of redness, increased pain, swelling, warmth, pus, or an unhealed wound. Report any concerning findings to the healthcare provider.
Managing secondary infections
If a secondary infection occurs, it is essential to promptly manage and treat it to prevent further complications. Take appropriate cultures or swabs from infected areas to identify the causative organism and guide antibiotic therapy if needed. Administer prescribed antibiotics as instructed and provide education on the importance of completing the full course of treatment. In addition to antibiotics, implement wound care measures to promote healing and prevent the spread of infection.
Ensuring proper wound healing
Proper wound healing is crucial in preventing complications and promoting optimal outcomes. Educate patients on wound care best practices, including cleaning the wound with mild soap and water, applying appropriate dressings, and avoiding excessive pressure on the healing area. Reinforce the importance of keeping the wound clean and dry, and instruct patients on the signs of delayed wound healing or infection. Encourage a healthy diet, adequate hydration, and good overall self-care practices to support proper wound healing.
Patient Follow-up
Scheduling regular appointments for monitoring
After initiating treatment, schedule regular follow-up appointments to monitor the patient’s progress and make any necessary adjustments to the treatment plan. The frequency of follow-up visits will depend on the severity of the warts and the chosen treatment modalities. During these appointments, assess the size and appearance of the warts, evaluate any changes in symptoms, and document the patient’s satisfaction with the treatment outcomes.
Assessing treatment outcomes
During follow-up appointments, it is important to assess the effectiveness of the chosen treatment options. Evaluate if there has been a reduction in the size and number of warts, as well as any improvements in symptoms such as pain or discomfort. Discuss any side effects or complications that may have occurred during the treatment process. Based on these assessments, collaborate with the healthcare team to determine whether to continue the current treatment or explore alternative options.
Providing ongoing education and support
Throughout the entire treatment journey, provide ongoing education and support to patients regarding their plantar wart management. Answer any questions or concerns they may have and clarify any misconceptions about the condition or treatment options. Reinforce preventive measures and self-care practices to minimize the risk of recurrence. Offer emotional support and encourage patients to reach out if they experience any challenges or need further guidance.
Collaborative Care
Consulting with dermatologists or podiatrists for specialized treatment
In complex or challenging cases, it may be necessary to consult with dermatologists or podiatrists for specialized treatment options. Collaborate closely with these professionals to ensure comprehensive and individualized care for the patients. Consultations may be needed for cases that do not respond to standard treatments, require more invasive procedures, or involve asymptomatic patients. Share relevant patient information, treatment history, and progress to facilitate a coordinated and unified approach.
Coordinating care with other healthcare providers
Patients with plantar warts may have underlying health conditions or require additional healthcare services. As a nurse, coordinate care with other healthcare providers involved in the patient’s overall management. Collaborate with primary care physicians, infectious disease specialists, or immunologists to ensure optimal care and address any underlying factors that may impede or complicate the treatment of plantar warts. Maintain open lines of communication to promote continuity of care.
Patient Advocacy
Ensuring patients receive appropriate and timely treatment
As a patient advocate, it is important to ensure that patients receive appropriate and timely treatment for their plantar warts. Advocate for patients by promptly reporting any concerning changes or complications to the healthcare team. Help patients understand their treatment options, potential risks, and benefits. Collaborate with healthcare providers to address any barriers to treatment or access to specialized care, and assist patients in navigating the healthcare system to receive the care they need.
Advocating for necessary interventions and resources
In addition to treatments, some patients may require additional interventions or resources to support their plantar wart management. This may include psychological support for patients who experience significant distress or anxiety related to the condition. Advocate for necessary interventions, such as counseling services or support groups, to help patients cope with the psychological impact of plantar warts. Work closely with social workers or other relevant professionals to connect patients with community resources or financial assistance programs if needed.
In summary, as a nurse caring for patients with plantar warts, your role is multifaceted. You play a crucial role in conducting assessments, providing education and support, implementing appropriate treatments, and ensuring infection control practices. By following a comprehensive approach to care, you can contribute to the effective management of plantar warts and improve patient outcomes.