Thrombocytopenia, a condition characterized by low blood platelet count, can present unique challenges to nurses in their daily practice. This article will provide an overview of nursing considerations and management strategies for thrombocytopenia, aimed at promoting patient safety and optimal outcomes. By understanding the key aspects of this condition and implementing appropriate nursing interventions, you can play a vital role in ensuring the well-being of patients with thrombocytopenia.

Assessment
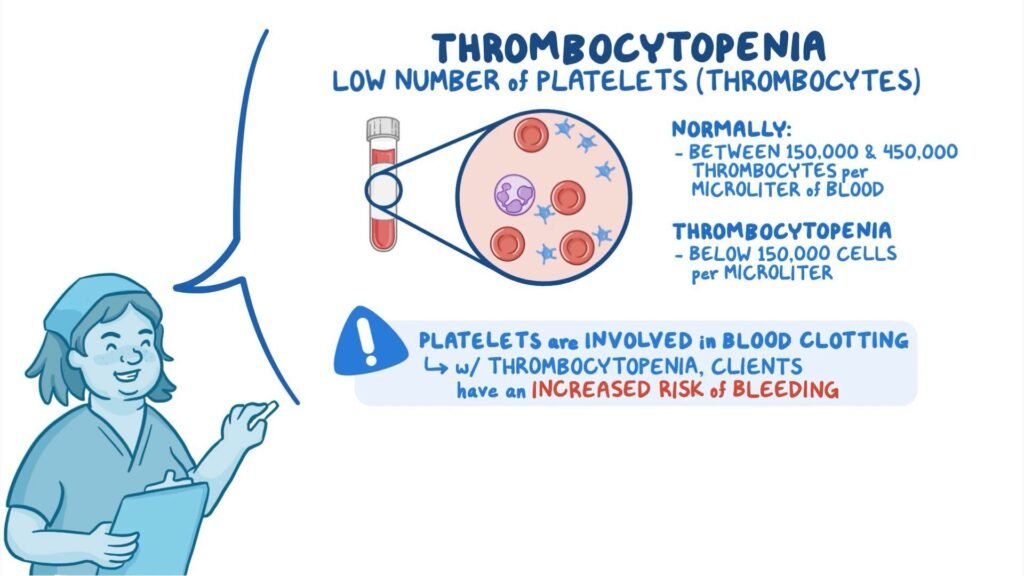
Thrombocytopenia is a condition characterized by a low platelet count, which can lead to an increased risk of bleeding and other complications. As a nurse, it is essential to perform a thorough assessment to gather relevant information about the patient’s history, physical condition, and laboratory results.
Patient history
When assessing a patient with thrombocytopenia, it is crucial to obtain a detailed patient history. This includes information about any previous diagnoses or medical conditions, such as liver disease or leukemia, as these can contribute to the development of thrombocytopenia. Additionally, inquire about any recent surgeries, injuries, or infections, as these may have caused platelet depletion.
Physical examination
A comprehensive physical examination is necessary to assess the patient’s overall physical condition and identify any signs of bleeding or other complications. Pay close attention to the skin for evidence of petechiae, purpura, or other indications of bleeding. Observe mucous membranes, such as the gums and nose, for signs of spontaneous bleeding. Assess vital signs, paying special attention to blood pressure and heart rate, as low platelet counts can lead to elevated bleeding risk.
Laboratory tests
Laboratory tests play a crucial role in the assessment of thrombocytopenia. A complete blood count (CBC) with differential is performed to determine the platelet count, as well as other blood cell parameters. Additionally, coagulation studies, such as prothrombin time (PT) and activated partial thromboplastin time (aPTT), may be ordered to assess the patient’s clotting ability. These tests provide valuable information to guide treatment decisions and monitor the patient’s progress.
Complications
Thrombocytopenia puts patients at an increased risk of several complications, including bleeding and infection. It is essential to be aware of these potential complications and take appropriate measures to prevent and manage them effectively.
Bleeding
Bleeding is a significant concern in patients with thrombocytopenia due to the decreased platelet count. The nurse must closely monitor the patient for any signs of bleeding, such as petechiae, ecchymosis, or prolonged bleeding from minor cuts or wounds. Promptly report any signs of active bleeding to the healthcare provider. Implement measures to prevent bleeding, such as using gentle techniques during patient care, avoiding unnecessary invasive procedures, and providing soft-bristle toothbrushes for oral care.
Hemorrhage
Hemorrhage refers to uncontrolled bleeding that can be life-threatening in severe cases. It is crucial for the nurse to assess the patient for signs of internal bleeding, such as melena (black, tarry stools) or hematemesis (vomiting blood). Instruct the patient to report any unusual bruising, dizziness, or weakness promptly. Collaborate with the healthcare team to manage bleeding episodes effectively, which may include platelet transfusions or other interventions.
Infection
Thrombocytopenia makes patients more susceptible to infections. Low platelet counts can impair the body’s immune response, making it harder to fight off infections. Therefore, it is essential to closely monitor the patient for signs of infection, such as fever, chills, or increased respiratory rate. Promote infection control measures, such as hand hygiene and a clean environment, to minimize the risk of infection. Educate the patient and their caregivers about the importance of proper hygiene and avoiding contact with sick individuals.
Prevention
Prevention plays a crucial role in managing thrombocytopenia and reducing the risk of bleeding and other complications. As a nurse, you can implement various strategies to help prevent adverse outcomes for patients with thrombocytopenia.
Platelet transfusions
Platelet transfusions are often necessary to increase the patient’s platelet count and prevent bleeding. Nurses play a vital role in ensuring safe and effective platelet transfusions. This includes verifying the correct blood product, checking for compatibility, and administering the transfusion according to established protocols. Regularly assess the patient for any signs of transfusion reactions, such as fever, chills, or itching, and promptly report any adverse events to the healthcare provider.
Medication management
Medication management is essential for patients with thrombocytopenia, as certain medications can further increase bleeding risk. As a nurse, it is crucial to review the patient’s medication list and identify any medications that may interfere with platelet function or cause bleeding. Collaborate with the healthcare team to adjust the patient’s medication regimen if necessary, and provide education to the patient and their caregivers about the importance of medication adherence and potential side effects to watch for.
Bleeding precautions
Implementing bleeding precautions is essential to minimize the risk of bleeding in patients with thrombocytopenia. Educate the patient and their caregivers about the importance of gentle handling and avoiding activities that may increase the risk of injury or bleeding, such as contact sports or using sharp objects. Provide assistive devices, such as non-slip footwear or walking aids, to promote safety and reduce the risk of falls. Regularly assess the patient’s environment for potential hazards and take appropriate steps to minimize the risk of injury.
Patient Education
Empowering patients with knowledge about their condition is vital in managing thrombocytopenia effectively. As a nurse, it is essential to provide comprehensive patient education that covers various aspects of thrombocytopenia.
Understanding thrombocytopenia
Start by explaining what thrombocytopenia is and why it occurs. Use simple, non-medical terminology to ensure the patient understands the condition. Discuss potential causes and risk factors, such as underlying medical conditions or recent surgeries. Provide information about the importance of regular blood tests to monitor platelet counts and how low platelet counts can increase the risk of bleeding.
Self-care measures
Educate the patient about self-care measures they can take to minimize the risk of bleeding and reduce complications. Stress the importance of practicing good oral hygiene with a soft-bristle toothbrush and prompt reporting of any bleeding from the gums. Instruct the patient to use a stool softener or increase dietary fiber intake to prevent constipation, as straining during bowel movements can lead to bleeding. Encourage the patient to avoid activities that may increase the risk of injury or contact with infectious individuals.
Signs and symptoms to report
Inform the patient and their caregivers about signs and symptoms that require immediate medical attention. These may include sudden or severe bruising, unexplained bleeding, or hypotension. Emphasize the importance of promptly reporting any signs of infection, such as fever or chills, as these can quickly progress in patients with thrombocytopenia. Provide clear instructions on who to contact if any concerning symptoms arise and ensure the patient has access to emergency contact numbers.

Collaborative Care
Collaboration with other healthcare professionals is essential in providing optimal care for patients with thrombocytopenia. Effective teamwork and communication are crucial for managing the complex needs of these patients.
Hematologist consultation
Consulting with a hematologist is often necessary in the care of patients with thrombocytopenia. Hematologists specialize in blood disorders, including thrombocytopenia, and can provide valuable insights and recommendations. Collaborate with the hematologist to develop an individualized care plan for the patient, considering their specific needs and underlying conditions.
Interdisciplinary team involvement
Thrombocytopenia management often requires input from various healthcare professionals, including nurses, physicians, pharmacists, and dietitians. Each team member plays a crucial role in ensuring safe and effective care. Collaborative meetings and discussions are essential to review the patient’s progress, adjust treatment plans, and address any concerns or challenges.
Collaboration with pharmacy
Pharmacists are vital in managing medication therapy for patients with thrombocytopenia. Collaborate with the pharmacy team to ensure accurate medication orders, review potential interactions or contraindications, and optimize medication regimens. Pharmacists can provide valuable insights into appropriate dosages, monitoring parameters, and potential adverse reactions to watch for. Regular communication with the pharmacy team is essential for safe and effective medication management.
Medication Management
Medication management is a critical aspect of caring for patients with thrombocytopenia. As a nurse, you play a key role in ensuring patients receive appropriate medications and monitoring for any adverse reactions.
Prescribing appropriate medications
Ensure that the patient’s medication regimen is appropriate for their thrombocytopenia and any underlying conditions. Collaborate with the healthcare provider to review all prescribed medications and determine if any adjustments are necessary. Some medications, such as certain anticoagulants or NSAIDs, may need to be avoided or used with caution in patients with low platelet counts due to their increased bleeding risk.
Monitoring for adverse reactions
Regularly assess the patient for any signs of adverse reactions to medications. This can include symptoms such as easy bruising or persistent bleeding, gastrointestinal upset, or allergic reactions. Educate the patient and their caregivers about the potential side effects of prescribed medications and when to seek medical attention. Promptly report any concerning symptoms or medication-related issues to the healthcare provider.
Dosage adjustments
In some cases, dosage adjustments may be necessary for medications that can affect platelet function or increase bleeding risk. Collaborate with the healthcare provider to determine appropriate dosages based on the patient’s platelet count and individual needs. Regularly monitor the patient’s response to medication therapy and communicate any changes or concerns to the healthcare team.
Transfusion Therapy
Transfusion therapy is often necessary in patients with thrombocytopenia to increase platelet counts and manage bleeding. As a nurse, you play a crucial role in ensuring safe and effective transfusion therapy.
Assessing for transfusion reactions
Before initiating a platelet transfusion, assess the patient for any signs of transfusion reactions. These can include fever, chills, itching, rash, or respiratory distress. Start the transfusion slowly and monitor closely for any adverse reactions during the procedure. Promptly report any signs of a reaction to the healthcare provider for further evaluation and immediate intervention.
Administering transfusions safely
Ensure proper identification of the patient and the blood product before initiating the transfusion. Follow established protocols for the administration of blood products, including verifying compatibility and using appropriate infusion equipment. Monitor the patient closely during the transfusion for any signs of adverse reactions or complications. Record all relevant information accurately, including the time started and completed, vital signs, and any transfusion events.
Monitoring for therapeutic response
After a platelet transfusion, it is essential to monitor the patient for a therapeutic response. Regularly assess the patient’s platelet counts and clotting function to evaluate the effectiveness of the transfusion. Collaborate with the healthcare provider to determine the desired platelet count range and adjust treatment plans if needed.
Dietary Considerations
Diet plays a significant role in managing thrombocytopenia and promoting overall health. As a nurse, you can provide valuable guidance to patients regarding dietary considerations.
Encouraging consumption of high-nutrient foods
A diet rich in essential nutrients can support the production of healthy platelets and overall well-being. Encourage the patient to consume foods that are high in iron, folate, and vitamin B12, as these nutrients are essential for healthy blood cell production. Examples of nutrient-rich foods include lean meats, leafy green vegetables, eggs, citrus fruits, and legumes. Collaborate with a dietitian to create a personalized dietary plan that meets the patient’s specific nutritional needs.
Restricting certain foods
In some cases, it may be necessary to restrict certain foods that can interfere with platelet function or increase bleeding risk. Foods that contain high levels of salicylates, such as aspirin or certain fruits and vegetables, may need to be limited. Collaborate with the healthcare provider and dietitian to determine appropriate dietary restrictions based on the patient’s individual needs and platelet count.
Managing dietary restrictions
Ensure that the patient understands and follows any necessary dietary restrictions. Provide education about alternative food choices that can still meet their nutritional needs. Collaborate with the dietitian to provide regular dietary counseling and support to the patient. Regularly assess the patient’s adherence to dietary restrictions and address any concerns or challenges they may face in following the recommended diet.

Psychosocial Support
Thrombocytopenia can have a significant impact on a patient’s emotional well-being and quality of life. As a nurse, you can provide valuable psychosocial support to patients dealing with this condition.
Addressing anxiety and fear
Thrombocytopenia can cause significant anxiety and fear about bleeding or other complications. Take the time to listen to the patient’s concerns and provide reassurance and emotional support. Offer clear and concise explanations about the condition, potential complications, and the steps taken to ensure their safety. Encourage open communication and create a safe environment for the patient to express their fears and anxieties.
Promoting coping strategies
Assist the patient in developing healthy coping strategies to manage their stress and anxiety related to thrombocytopenia. Encourage relaxation techniques, such as deep breathing exercises or mindfulness meditation, to promote a sense of calm. Provide information about support resources, such as support groups or counseling services, that can help the patient navigate their emotional journey and connect with others facing similar challenges.
Referring to support groups or counseling
Thrombocytopenia can be a lifelong condition, and patients may benefit from ongoing support. Refer patients to support groups or counseling services where they can connect with others who share similar experiences. These resources provide an opportunity for patients to exchange information, seek advice, and gain emotional support. Collaborate with social workers or case managers to ensure appropriate referrals are made and follow-up is provided.
Safety Measures
Patient safety is paramount in the care of individuals with thrombocytopenia. Implementing safety measures can reduce the risk of complications and ensure optimal outcomes for patients.
Fall prevention
Low platelet counts can increase the risk of bleeding, making fall prevention a crucial aspect of care. Assess the patient’s mobility and environmental hazards that may contribute to falls. Implement measures to minimize fall risk, such as keeping the patient’s environment free of tripping hazards, ensuring appropriate lighting, and providing assistive devices as needed. Educate the patient about the importance of moving slowly and taking precautions to avoid falls.
Infection control
Thrombocytopenia can weaken the immune response, making patients more susceptible to infections. Implement stringent infection control measures to prevent the spread of pathogens. This includes adhering to proper hand hygiene protocols, using personal protective equipment when necessary, and maintaining a clean environment. Educate the patient and their caregivers about infection control practices, such as proper handwashing and avoiding contact with individuals who are sick.
Medication safety
Medication safety is crucial in patients with thrombocytopenia, as certain medications can increase bleeding risk. Ensure proper medication storage and administration practices to minimize the risk of errors. Follow established protocols for medication reconciliation and verification to prevent medication-related adverse events. Educate the patient and their caregivers about the importance of medication adherence, potential side effects, and the need to promptly report any concerning symptoms or medication-related issues.
