Vaginitis is a common condition that many women may experience at some point in their lives. In this article, we will explore the nursing considerations and management strategies for vaginitis. From understanding the different types of vaginitis to implementing effective interventions, we will provide you with a comprehensive overview to help you navigate this condition with confidence and provide optimal care for your patients. So, grab a cup of tea and let’s dive into the world of nursing considerations for vaginitis together!
Assessment
Patient history
In order to effectively assess and manage vaginitis, it is important to obtain a thorough patient history. This includes gathering information about the patient’s age, sexual history, hygiene practices, previous diagnoses of vaginitis, and any current symptoms or discomfort they may be experiencing. Understanding the patient’s medical history, including any underlying health conditions or surgeries, can also provide valuable insight into the potential causes and treatment options for their vaginitis.
Symptoms
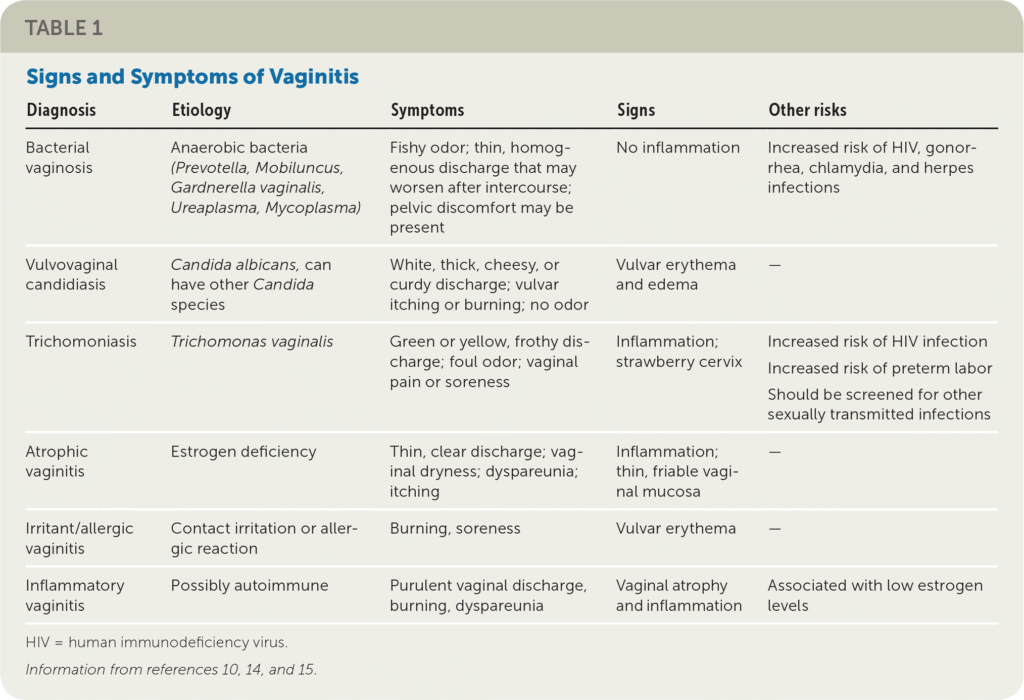
The symptoms of vaginitis can vary depending on the underlying cause, but common symptoms include itching, burning, irritation, abnormal vaginal discharge, and pain during sexual intercourse or urination. It is important to ask the patient about the severity and duration of their symptoms, as well as any factors that may worsen or alleviate them. Additionally, assess for the presence of any other symptoms that may indicate a more serious condition, such as fever or lower abdominal pain.
Physical examination
A physical examination can provide important clues regarding the cause and severity of vaginitis. During the examination, inspect the external genitalia for any redness, swelling, or lesions. Palpate the inguinal lymph nodes to check for any enlargement or tenderness. A speculum examination may also be performed to visualize the vaginal walls and cervix, and to assess the color, consistency, and odor of any vaginal discharge.
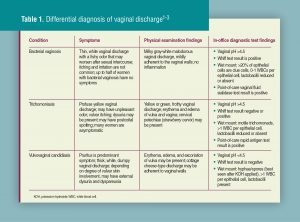
Diagnostic tests
To confirm the diagnosis and determine the specific cause of vaginitis, various diagnostic tests may be ordered. These tests can include a microscopic examination of a vaginal swab to identify the presence of bacteria, yeast, or parasites. Cultures may also be performed to identify the specific organism responsible for the infection. In some cases, a biopsy may be necessary to rule out other underlying conditions. Additionally, blood tests may be ordered to check for any hormonal imbalances or underlying medical conditions that may be contributing to the vaginitis.
Types of Vaginitis
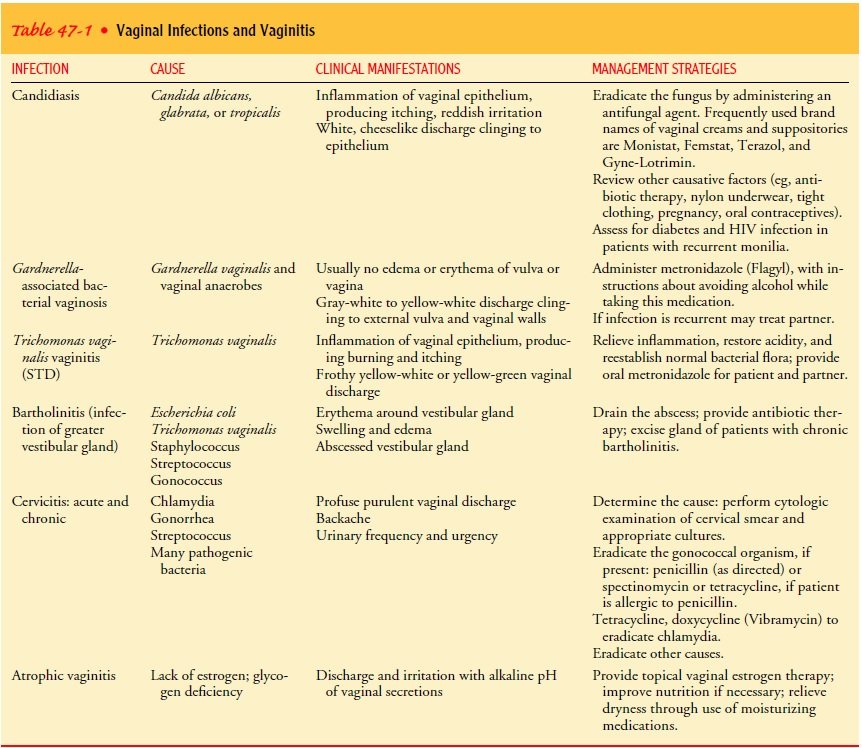
Bacterial vaginosis
Bacterial vaginosis is a common cause of vaginitis that occurs when there is an overgrowth of certain types of bacteria in the vagina. It is often characterized by a thin, grayish-white discharge with a noticeable fishy odor. Bacterial vaginosis can result from factors such as douching, multiple sexual partners, or an imbalance in the vaginal microbiome.
Yeast infection (Candidiasis)
Yeast infection, or candidiasis, occurs when there is an overgrowth of the fungus Candida in the vagina. It can cause symptoms such as intense itching, thick white discharge that resembles cottage cheese, and redness or swelling of the vulva. Yeast infections are commonly associated with factors such as antibiotic use, hormonal changes, diabetes, or a weakened immune system.
Trichomoniasis
Trichomoniasis is a sexually transmitted infection caused by the parasite Trichomonas vaginalis. It can cause symptoms such as itching, burning, a frothy yellow-green vaginal discharge, and a strong fishy odor. Trichomoniasis is typically transmitted through sexual contact and can be easily treated with medications.
Atrophic vaginitis
Atrophic vaginitis is a type of vaginitis that occurs due to a decrease in estrogen levels, often associated with menopause. It can cause symptoms such as vaginal dryness, itching, irritation, and pain during sexual intercourse. Treatment for atrophic vaginitis typically involves hormone therapy to restore estrogen levels and alleviate symptoms.
Other types
There are other less common types of vaginitis, including non-infectious vaginitis, which can result from allergic reactions or irritants, and mixed vaginitis, which occurs when there are multiple types of infections present simultaneously.
Causes and Risk Factors
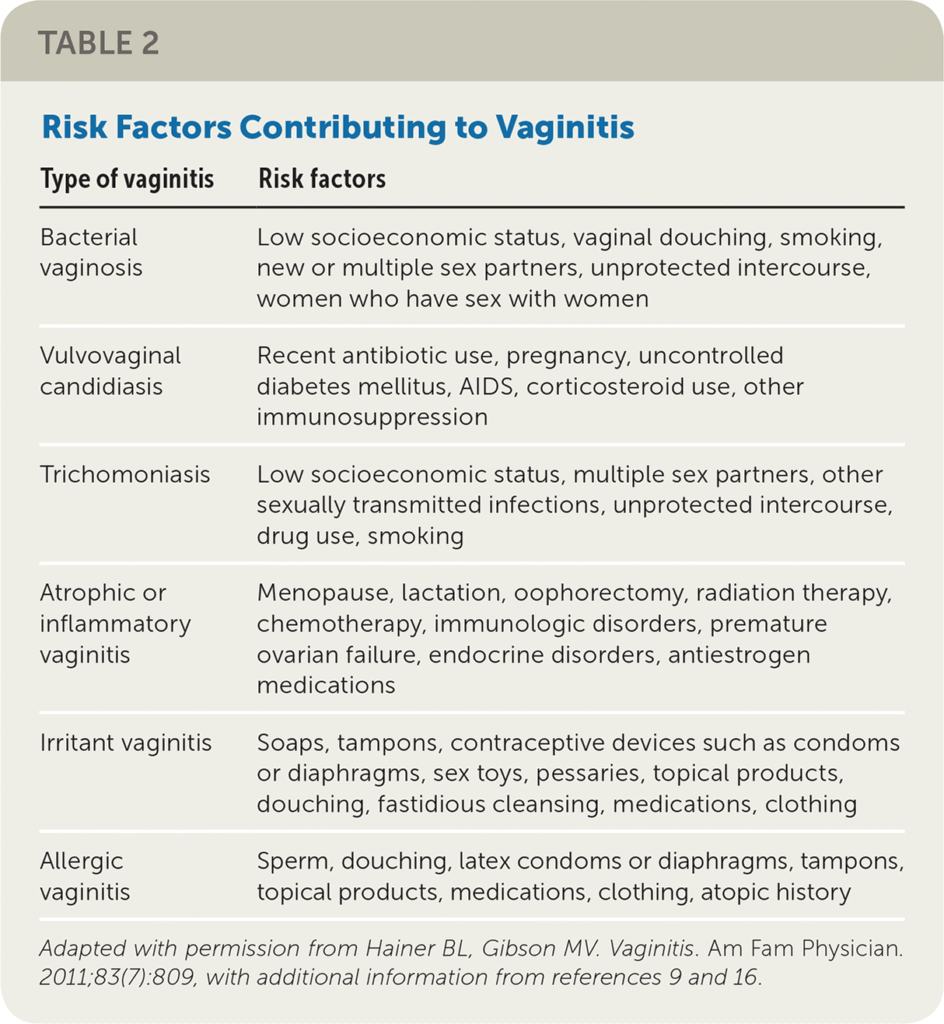
Microbial imbalances
An imbalance in the vaginal microbiome is a common cause of vaginitis. Factors such as douching, using harsh soaps or hygiene products, or taking antibiotics can disrupt the natural balance of bacteria and yeast in the vagina, leading to an overgrowth of harmful organisms.
Sexual activity
Sexual activity, especially with multiple partners or a new partner, can increase the risk of developing vaginitis. This is particularly true for trichomoniasis and sexually transmitted infections, which can be transmitted through sexual contact.
Hormonal changes
Hormonal changes, such as those that occur during pregnancy, menopause, or the menstrual cycle, can alter the vaginal environment and increase the risk of developing vaginitis. Estrogen plays a particularly important role in maintaining the health and balance of the vaginal tissues.
Antibiotic use
Taking antibiotics can disrupt the natural balance of bacteria in the vagina, increasing the risk of developing vaginitis. Antibiotics kill both harmful and beneficial bacteria, creating an environment that is more susceptible to infections.
Poor hygiene
Poor hygiene practices, such as not properly cleaning the genital area or wearing tight, non-breathable clothing, can contribute to the development of vaginitis. This is because these factors can create a moist, warm environment that promotes the growth of harmful microorganisms.
Allergies or irritants
Exposure to certain allergens or irritants, such as certain types of soaps, detergents, or perfumes, can cause an allergic reaction or irritation in the vaginal area, leading to vaginitis.
Weakened immune system
A weakened immune system can make an individual more susceptible to infections, including vaginitis. Conditions such as HIV/AIDS, diabetes, and certain autoimmune disorders can compromise the immune system’s ability to fight off infections.
Patient Education
Explanation of condition
When providing patient education about vaginitis, it is important to explain the underlying causes, symptoms, and treatment options. Help the patient understand that vaginitis is a common condition that can be caused by a variety of factors, and that it is not necessarily indicative of poor hygiene or any personal failure.
Self-care measures
Encourage the patient to practice good hygiene by washing the genital area with mild soap and water. Advise them to avoid douching, using scented hygiene products, or wearing tight, non-breathable clothing, as these can further irritate the vaginal tissues. Additionally, recommend the use of cotton underwear and avoiding the use of panty liners or pads unless necessary.
Prevention strategies
Educate the patient on preventive measures to reduce the risk of developing vaginitis. This can include practicing safe sexual behaviors, such as using condoms and limiting the number of sexual partners. It is also important for the patient to understand the importance of maintaining a healthy lifestyle, including eating a balanced diet, managing stress, and getting regular exercise to support a strong immune system.
Importance of medication adherence
If the patient is prescribed medication to treat their vaginitis, stress the importance of adherence to the prescribed treatment regimen. Help the patient understand the potential consequences of not following the treatment plan, including the possibility of recurrent or chronic vaginitis.
Follow-up care
Explain the importance of follow-up care to monitor the effectiveness of the treatment and address any remaining or new symptoms. Encourage the patient to reach out if they have any questions or concerns, and provide them with appropriate contact information to seek further assistance if needed.
Medical Treatments
Antibiotics
For bacterial vaginosis or certain types of vaginitis caused by bacterial infections, antibiotics may be prescribed. These medications help to eliminate the overgrowth of harmful bacteria and restore the balance in the vaginal microbiome.
Antifungals
Antifungal medications, such as antifungal creams or suppositories, are commonly used to treat yeast infections. These medications help to eliminate the overgrowth of Candida fungus and relieve the associated symptoms.
Antiparasitics
In the case of trichomoniasis, antiparasitic medications are prescribed to eliminate the Trichomonas vaginalis parasite. These medications can be administered orally or as a vaginal gel.
Hormone therapy
Hormone therapy, such as estrogen creams or vaginal rings, may be prescribed to treat atrophic vaginitis. These medications help to restore estrogen levels, alleviate symptoms, and promote the health of the vaginal tissues.
Topical treatments
Topical treatments, such as creams or gels, can provide relief from symptoms such as itching, burning, or irritation. These medications may contain ingredients such as hydrocortisone or lidocaine, which help to reduce inflammation and discomfort.
Alternative medicine
Some individuals may seek alternative or complementary treatments for vaginitis, such as herbal remedies or probiotics. While research on the effectiveness of these treatments is limited, it is important for healthcare providers to be aware of any alternative treatments the patient may be using and to provide appropriate guidance and support.
Nursing Interventions
Promoting comfort and hygiene
Nurses play a crucial role in promoting comfort and hygiene for patients with vaginitis. This includes providing education on good hygiene practices, such as proper cleansing techniques and avoiding irritants. Additionally, nurses can provide guidance on ways to alleviate discomfort, such as using ice packs or warm sitz baths.
Administering prescribed medications
Nurses are responsible for ensuring that prescribed medications are administered correctly and on time. This includes providing education on how to properly use medications, such as antifungal creams or suppositories, and addressing any concerns or questions the patient may have.
Ensuring patient safety
Patient safety is paramount in the nursing care of individuals with vaginitis. Nurses should ensure that infection prevention measures are followed, such as proper hand hygiene and the use of personal protective equipment when necessary. Additionally, nurses should monitor patients for any signs of complications or adverse reactions to medications.
Educating patient on medication side effects
It is important for nurses to educate patients about the potential side effects of the medications they are prescribed for vaginitis. This includes providing information on common side effects, such as gastrointestinal upset or allergic reactions, as well as any specific precautions or warning signs they should be aware of.
Assisting with self-care measures
Nurses can provide guidance and support to patients in implementing self-care measures to manage their vaginitis. This can include helping the patient develop a personalized hygiene routine, providing education on proper use of hygiene products, or offering resources for additional support or counseling if needed.

Complications
Pelvic inflammatory disease
Untreated or recurrent vaginitis can sometimes lead to pelvic inflammatory disease (PID), a serious infection that affects the female reproductive organs. PID can cause symptoms such as lower abdominal pain, fever, and painful intercourse. Prompt treatment of vaginitis can help prevent the development of PID.
Urinary tract infections
In some cases, vaginitis can lead to urinary tract infections (UTIs). This can occur when the infection spreads from the vagina to the urethra and bladder. Patients with vaginitis should be educated on the signs and symptoms of UTIs, such as frequent urination, burning during urination, and lower abdominal pain, and encouraged to seek medical attention if they suspect a UTI.
Pregnancy complications
Vaginitis during pregnancy can increase the risk of complications such as preterm birth or low birth weight. Pregnant individuals with vaginitis should be closely monitored and treated promptly to reduce the risk of adverse outcomes.
Increased risk of sexually transmitted infections
Having untreated or recurrent vaginitis can increase the risk of acquiring or transmitting sexually transmitted infections (STIs). This is especially true for individuals with trichomoniasis or other STIs. Education on safe sexual practices, including condom use and regular STI testing, can help reduce the risk of STIs.
Chronic or recurrent vaginitis
In some cases, vaginitis can become chronic or recurrent, requiring ongoing treatment and management. Chronic vaginitis is often caused by underlying factors such as hormonal imbalances or immune system disorders. It is important for healthcare providers to work closely with patients to identify and address these underlying factors to effectively manage chronic or recurrent vaginitis.
Collaborative Care
Consulting with healthcare team
Nurses should collaborate with other members of the healthcare team, including physicians, nurse practitioners, and other specialized healthcare providers, to ensure comprehensive and coordinated care for patients with vaginitis. This includes sharing information, seeking guidance, and collaborating on treatment plans.
Referral to specialists
In some cases, referral to specialists may be necessary for further evaluation or management of vaginitis. This can include gynecologists, infectious disease specialists, or reproductive endocrinologists, depending on the underlying cause and complexity of the condition.
Coordinating care with other providers
Nurses play an important role in coordinating care for patients with vaginitis. This includes communicating with other healthcare providers involved in the patient’s care, such as primary care physicians or dermatologists, and ensuring that all necessary information is shared to provide comprehensive and seamless care.
Providing continuity of care
Continuity of care is essential in the management of vaginitis. Nurses can help ensure that patients receive consistent and ongoing care by providing education and support, scheduling follow-up appointments, and facilitating communication between the patient and the healthcare team.
Preventive Measures
Promoting good hygiene practices
One of the key preventive measures for vaginitis is promoting good hygiene practices. Nurses can educate patients on the importance of proper cleansing techniques, avoiding irritants, and maintaining a healthy vaginal environment. This may include recommending gentle cleansing with mild soap and water, avoiding douching or using scented products, and wearing breathable cotton underwear.
Encouraging safe sexual practices
Safe sexual practices can help reduce the risk of vaginitis and sexually transmitted infections. Nurses can provide education on the use of condoms, limiting the number of sexual partners, and regular testing for STIs. It is also important to address any concerns or misconceptions the patient may have about safe sexual practices.
Educating patients on preventive measures
Education is key in preventing vaginitis. Nurses should provide information on risk factors and preventive measures, such as maintaining a healthy lifestyle, managing chronic conditions, and avoiding known triggers or irritants. This can include providing resources and support to help patients make informed decisions and develop healthy habits.
Regular screening and check-ups
Regular screenings and check-ups can help identify any early signs or symptoms of vaginitis and provide prompt treatment. Nurses can help facilitate regular check-ups and ensure that patients are aware of the importance of routine screenings for vaginal infections, especially for individuals with recurrent or chronic vaginitis.
Documentation and Reporting
Accurate and detailed documentation
Accurate and detailed documentation is essential in the care of patients with vaginitis. Nurses should document the patient’s medical history, symptoms, physical examination findings, diagnostic test results, medications administered, and any interventions or education provided. This documentation not only helps ensure continuity of care but also serves as a legal record of the patient’s healthcare journey.
Reporting abnormal findings
If any abnormal or concerning findings are observed during the assessment or treatment of a patient with vaginitis, it is important to promptly report these findings to the appropriate healthcare providers. This may include notifying the primary care physician, gynecologist, or other healthcare professionals involved in the patient’s care.
Communication with healthcare team
Effective communication with the healthcare team is crucial in providing comprehensive and coordinated care for patients with vaginitis. Nurses should communicate any relevant information, such as changes in symptoms or treatment plans, to ensure that all members of the healthcare team are informed and involved in the patient’s care.
Maintaining patient confidentiality
Nurses must adhere to strict standards of patient confidentiality when documenting and reporting on patients with vaginitis. This includes ensuring that all electronic and paper records are securely stored and that patient information is only shared with authorized healthcare providers involved in the patient’s care. Respecting patient confidentiality builds trust and maintains the integrity of the nurse-patient relationship.
In conclusion, nursing considerations for vaginitis encompass a comprehensive assessment, awareness of the different types and causes of vaginitis, patient education, provision of appropriate medical treatments, implementation of nursing interventions, identification and management of potential complications, collaborative care with the healthcare team, promotion of preventive measures, accurate documentation and reporting, and adherence to patient confidentiality. By taking a holistic and patient-centered approach, nurses can play a vital role in effectively managing vaginitis and providing compassionate care to individuals experiencing this condition.
