Hey there! Have you ever wondered what exactly arthritis is and how it affects millions of people around the world? Well, look no further! In this article, we’ll take a deep dive into the world of arthritis, exploring its causes, symptoms, and available treatment options. Whether you’re experiencing joint pain yourself or simply curious to learn more about this common condition, we’ve got you covered. So, let’s get started on unraveling the mysteries of arthritis together!
Causes of Arthritis
Genetic Factors
One of the causes of arthritis is believed to be genetic factors. Research has shown that certain genes can make individuals more susceptible to developing arthritis. If there is a family history of arthritis, especially in close relatives such as parents or siblings, there is a higher likelihood of developing the condition.
Age
Another common cause of arthritis is age. As we grow older, the cartilage in our joints naturally starts to wear down. This can lead to joint pain, stiffness, and inflammation, which are all characteristic symptoms of arthritis. As age increases, so does the risk of developing arthritis.
Injury
Injury is another factor that can contribute to the development of arthritis. Injuries to the joints, such as fractures or dislocations, can lead to post-traumatic arthritis. This type of arthritis can develop years after the initial injury and can cause chronic pain and joint damage.
Obesity
Obesity is known to be a risk factor for arthritis, particularly osteoarthritis. Excess weight puts additional pressure on the joints, especially in weight-bearing areas such as the knees and hips. Over time, this increased stress can cause the cartilage to break down and lead to the development of arthritis.
Infections
In some cases, certain infections can trigger the development of arthritis. Bacterial or viral infections can cause the immune system to go into overdrive, leading to joint inflammation and damage. Examples of infections that have been associated with arthritis include Lyme disease and certain gastrointestinal infections.
Types of Arthritis
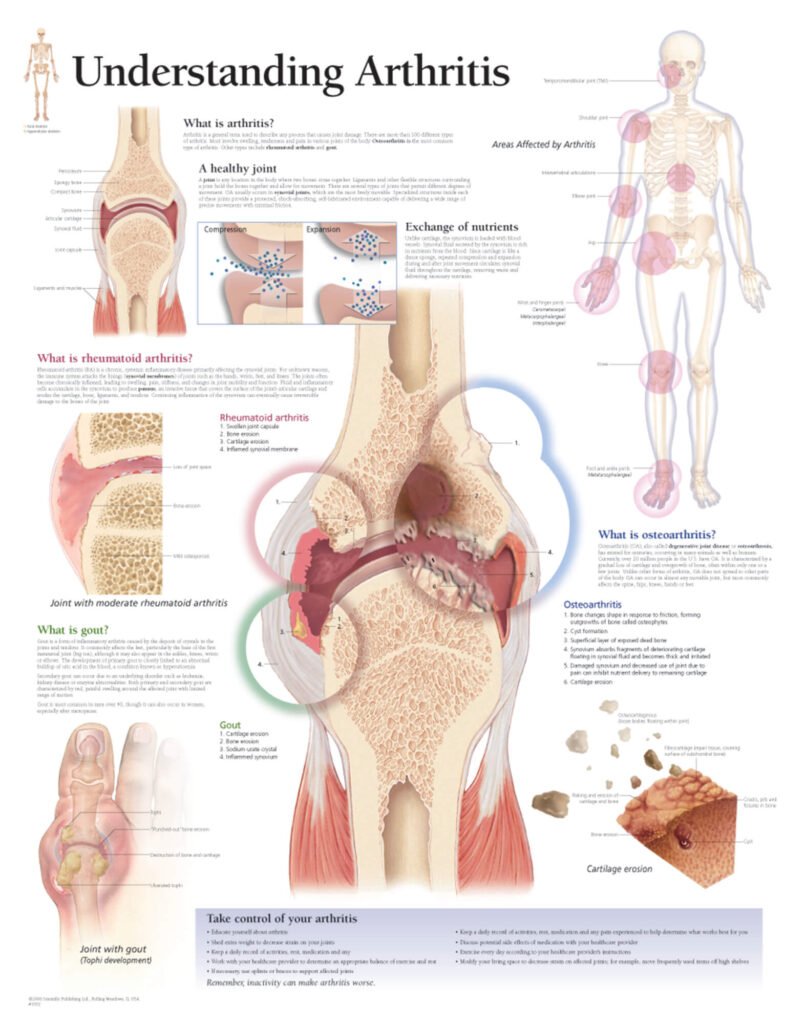
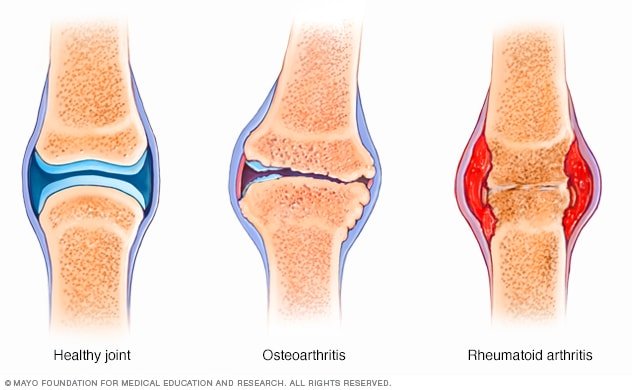
Osteoarthritis
Osteoarthritis is the most common type of arthritis. It occurs when the protective cartilage that cushions the ends of the bones wears down over time. Osteoarthritis typically affects the joints in the hands, knees, hips, and spine. Symptoms include joint pain, stiffness, and limited range of motion.
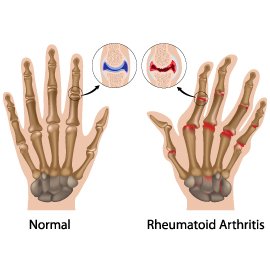
Rheumatoid Arthritis
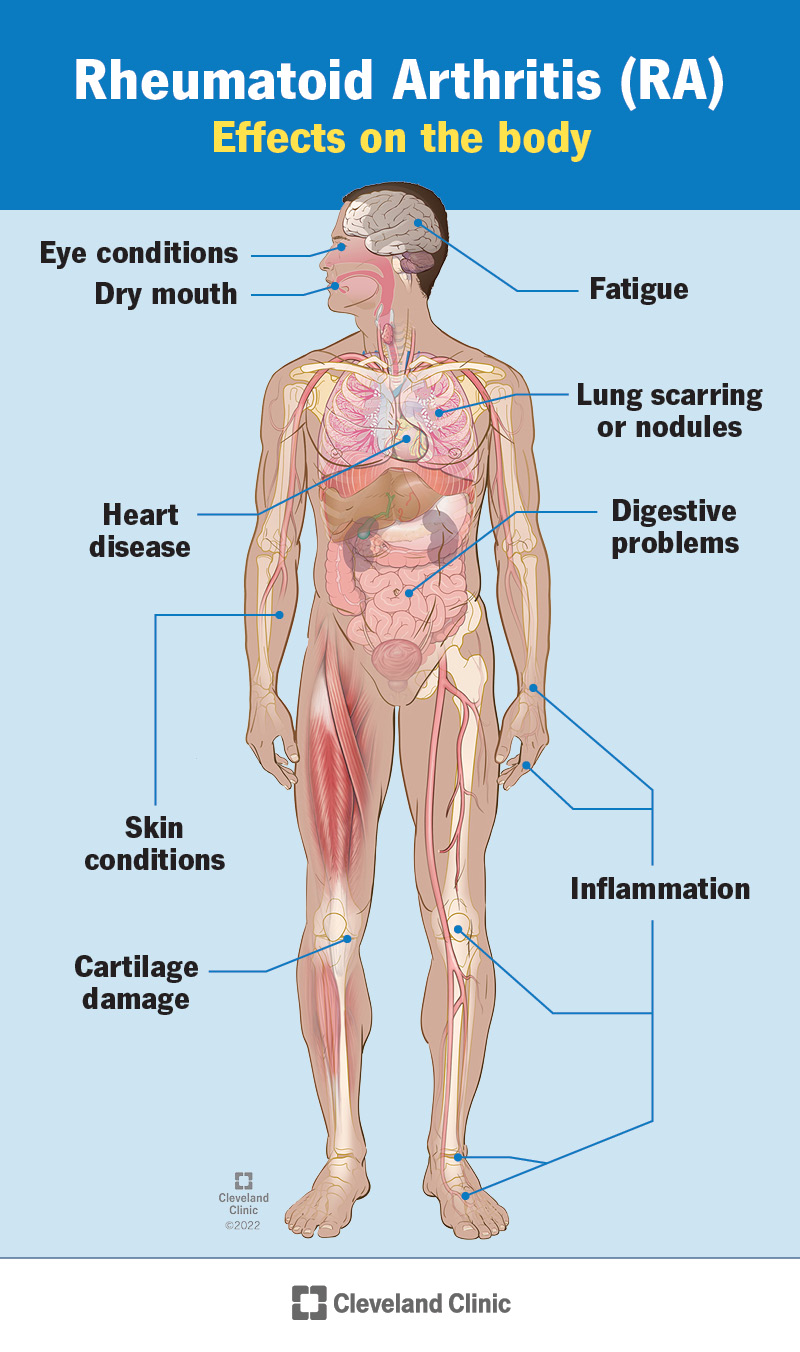
Rheumatoid arthritis is an autoimmune disease that causes chronic inflammation of the joints. It occurs when the immune system mistakenly attacks the tissues that line the joints, leading to pain, swelling, and joint deformity. Rheumatoid arthritis can also affect other organs in the body.
Psoriatic Arthritis
Psoriatic arthritis is a type of arthritis that develops in individuals who have psoriasis, a skin condition characterized by red, scaly patches. Psoriatic arthritis causes joint pain, stiffness, and swelling. It can also lead to nail changes and dactylitis, which is the swelling of an entire finger or toe.
Gout
Gout is a form of arthritis that develops due to the buildup of uric acid crystals in the joints. It commonly affects the big toe, but can also involve other joints such as the ankle, knee, or wrist. Gout causes sudden, intense pain, swelling, and redness in the affected joint.
Ankylosing Spondylitis
Ankylosing spondylitis is a type of arthritis that primarily affects the spine. It causes inflammation of the sacroiliac joints, which are located in the lower back. Over time, ankylosing spondylitis can lead to the fusion of the spinal vertebrae, causing stiffness and limited mobility.
Signs and Symptoms of Arthritis
Joint Pain and Stiffness
One of the most common signs of arthritis is joint pain and stiffness. The pain can range from mild to severe and may worsen with movement. Stiffness is often more pronounced in the morning or after periods of inactivity.
Swelling and Redness
Inflamed joints can become swollen and tender to the touch. The affected area may also appear red and feel warm. Swelling and redness are common symptoms of many types of arthritis, including rheumatoid arthritis and gout.
Limited Range of Motion
As arthritis progresses, it can cause a decrease in the range of motion of affected joints. This can make it difficult to perform everyday tasks, such as bending or reaching. In severe cases, joint deformities may develop, further restricting movement.
Fatigue
Fatigue is a common symptom experienced by individuals with arthritis. The constant pain and inflammation can take a toll on the body, leading to feelings of exhaustion and a lack of energy. Fatigue can also be a side effect of certain medications used to manage arthritis.
Fever
In some cases, arthritis can be accompanied by a low-grade fever. This is more commonly seen in individuals with rheumatoid arthritis, as it is an inflammatory condition. Fever may occur during flare-ups or periods of increased disease activity.
Diagnosing Arthritis
Medical History and Physical Examination
To diagnose arthritis, your healthcare provider will start by taking a detailed medical history and performing a physical examination. They will ask about your symptoms, family history of arthritis, and any previous injuries or infections. During the physical examination, they will assess your joints for signs of inflammation, swelling, and limited mobility.
Imaging Tests
Imaging tests such as X-rays, CT scans, and MRIs may be ordered to get a closer look at the affected joints. These tests can help to visualize the extent of joint damage and rule out other conditions that may be causing your symptoms.
Laboratory Tests
Laboratory tests can be helpful in diagnosing certain types of arthritis, such as rheumatoid arthritis or infectious arthritis. Blood tests can detect specific antibodies or markers of inflammation that are associated with these conditions. Joint fluid analysis may also be performed to check for signs of infection or crystals, as seen in gout.
Traditional Treatments for Arthritis
Medications
Medications are commonly used to manage the symptoms of arthritis and slow down the progression of the disease. Nonsteroidal anti-inflammatory drugs (NSAIDs) can help to reduce pain and inflammation. Disease-modifying antirheumatic drugs (DMARDs) and biologic agents are often prescribed for individuals with rheumatoid arthritis or other autoimmune forms of arthritis.
Physical Therapy
Physical therapy is an essential component of arthritis treatment. A physical therapist can teach you exercises and stretches to improve joint flexibility, strengthen muscles, and reduce pain. They may also use modalities such as heat or ice therapy to help alleviate symptoms.
Occupational Therapy
Occupational therapy focuses on helping individuals with arthritis maintain independence and perform daily tasks. An occupational therapist can recommend adaptations or assistive devices to make activities easier and less painful.
Assistive Devices
Assistive devices such as canes, walkers, or braces may be recommended to help support and protect the affected joints. These devices can help reduce pain and improve mobility, making daily activities more manageable.
Surgery
In severe cases of arthritis, surgery may be required to repair or replace damaged joints. Joint replacement surgery, such as a hip or knee replacement, can help improve mobility and relieve pain. Other surgical options include joint fusion or joint resurfacing.
Lifestyle Changes to Manage Arthritis
Regular Exercise
Regular exercise is crucial for managing arthritis and maintaining joint health. Low-impact exercises such as walking, swimming, or biking can help strengthen the muscles around the joints and improve flexibility. It is important to work with a healthcare professional or physical therapist to develop an exercise program that is safe and suitable for your specific needs.
Weight Management
Maintaining a healthy weight is important for individuals with arthritis, especially those with osteoarthritis. Excess weight puts more stress on the joints and can exacerbate symptoms. Weight loss can help alleviate pain and improve mobility.
Proper Nutrition
A well-balanced diet can help support overall joint health. Foods rich in omega-3 fatty acids, such as fatty fish, nuts, and seeds, may help reduce inflammation. Antioxidant-rich fruits and vegetables can also provide benefits for individuals with arthritis.
Hot and Cold Therapy
Hot and cold therapy can provide temporary relief for joint pain and stiffness. Applying a heating pad or warm towel to the affected area can help relax muscles and increase blood flow. Cold packs or ice packs can help numb the area and reduce inflammation.
Stress Management
Stress can worsen arthritis symptoms, so it is important to find healthy ways to manage stress. Relaxation techniques such as deep breathing, meditation, or yoga can help reduce stress levels and promote overall well-being.
Alternative Treatments for Arthritis
Acupuncture
Acupuncture is a traditional Chinese medicine practice that involves inserting thin needles into specific points on the body. Some individuals with arthritis find acupuncture helpful in reducing pain and improving joint function.
Massage Therapy
Massage therapy can help relax muscles, reduce pain, and improve circulation. Techniques such as Swedish massage or deep tissue massage may be beneficial for individuals with arthritis.
Herbal Supplements
Certain herbal supplements, such as turmeric or ginger, have anti-inflammatory properties and may provide relief for arthritis symptoms. However, it is important to consult with a healthcare professional before starting any herbal supplements, as they may interact with medications or have potential side effects.
Mind-Body Techniques
Mind-body techniques such as meditation, guided imagery, or biofeedback can help individuals with arthritis manage pain and reduce stress. These techniques focus on the connection between the mind and body and can promote relaxation and overall well-being.
Homeopathy
Homeopathy is a form of alternative medicine that uses highly diluted substances to stimulate the body’s natural healing processes. Some individuals with arthritis may find relief with homeopathic remedies. However, scientific evidence supporting the effectiveness of homeopathy for arthritis is limited.
Managing Arthritis with Self-Care
Pain and Symptom Management
Self-care plays a vital role in managing arthritis symptoms. This can include taking over-the-counter pain relievers as recommended by your healthcare provider, using hot or cold therapy, and resting when needed.
Joint Protection
Protecting your joints from further damage is crucial in managing arthritis. This can be done by using proper body mechanics, avoiding repetitive motions or activities that put stress on the joints, and using assistive devices or adaptive equipment to decrease joint strain.
Balanced Rest and Activity
Balancing rest and activity is important for individuals with arthritis. It is essential to listen to your body and take breaks when needed, but also to engage in regular physical activity to maintain joint flexibility and strength.
Supportive Footwear
Wearing supportive and cushioned footwear can help reduce the impact on your joints, especially when walking or standing for long periods. Shoes with good arch support and shock-absorbing soles are typically recommended for individuals with arthritis.
Avoiding Trigger Foods
Some individuals with arthritis may experience worsened symptoms after consuming certain foods. Keeping a food diary can help identify trigger foods and make necessary dietary adjustments. Common trigger foods include processed foods, red meat, and foods high in sugar or saturated fats.

Prevention and Risk Reduction of Arthritis
Maintaining a Healthy Weight
Maintaining a healthy weight is one of the key ways to prevent or reduce the risk of developing arthritis, particularly osteoarthritis. By keeping your weight within a healthy range, you can lessen the stress on your joints and decrease the likelihood of joint damage.
Stay Physically Active
Regular physical activity is not only important for managing arthritis but also for preventing its onset. Engaging in exercises that strengthen muscles, improve flexibility, and support joint health can help reduce the risk of arthritis.
Protect Joints from Injury
Taking precautions to protect your joints from injury can help reduce the risk of developing arthritis. This includes using proper body mechanics, wearing protective gear during sports or physical activities, and avoiding repetitive motions that may strain the joints.
Quit Smoking
Smoking is not only harmful to overall health but also increases the risk of developing rheumatoid arthritis. Quitting smoking can not only lower the risk of arthritis but also improve overall joint health and reduce inflammation.
Manage Stress
Stress can worsen inflammation and contribute to arthritis symptoms. Finding healthy ways to manage stress, such as through exercise, relaxation techniques, or hobbies, can help reduce the impact of stress on your joints.
Support and Resources for Arthritis
Arthritis Support Groups
Arthritis support groups can provide a valuable source of emotional support and practical advice for individuals living with arthritis. These groups allow individuals to connect with others who are facing similar challenges and share their experiences.
Patient Education and Self-Management Programs
Patient education programs and self-management programs can provide individuals with valuable information about arthritis and its management. These programs often include workshops, classes, or online resources that cover topics such as symptom management, medication adherence, and coping strategies.
Arthritis Foundations and Organizations
Arthritis foundations and organizations are dedicated to raising awareness about arthritis and providing support to individuals and their families. These organizations often offer educational materials, resources, and advocacy for individuals living with arthritis.
Online Communities
Online communities and forums provide a platform for individuals with arthritis to connect with others, share their experiences, and seek advice. These communities can be especially helpful for individuals who may not have access to local support groups or who prefer online interactions.
Financial Assistance Programs
Managing arthritis can be costly, with expenses such as medications, doctor visits, and assistive devices. Financial assistance programs, such as patient assistance programs or grants, may be available to help individuals with the financial burden associated with arthritis.
Arthritis is a complex condition with various causes, types, and treatment options. By understanding the causes, recognizing the signs and symptoms, and exploring the different treatment approaches, you can work with your healthcare provider to effectively manage your arthritis and improve your quality of life. Remember, it is essential to consult with a healthcare professional for proper diagnosis and personalized treatment recommendations. With the right support and resources, you can navigate the challenges posed by arthritis and regain control over your health.