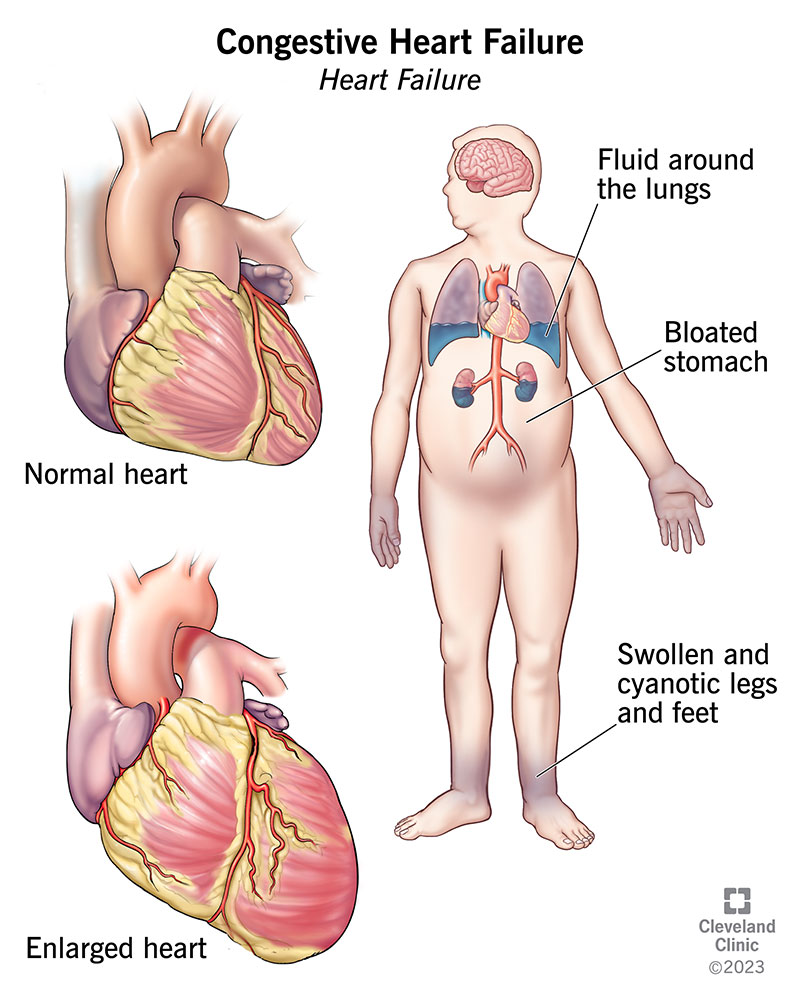
You’re about to learn all about the diagnosis of Congestive Heart Failure (CHF). It’s a condition that affects millions of people worldwide, causing symptoms such as shortness of breath, fatigue, and swelling in the legs. In this article, you’ll discover the various diagnostic tools and tests that healthcare professionals use to identify CHF, including physical examinations, imaging studies, and blood tests. By understanding the process of diagnosing CHF, you’ll be better equipped to recognize the signs and seek appropriate medical care if needed. So, let’s dive right in and explore the world of diagnosing Congestive Heart Failure!
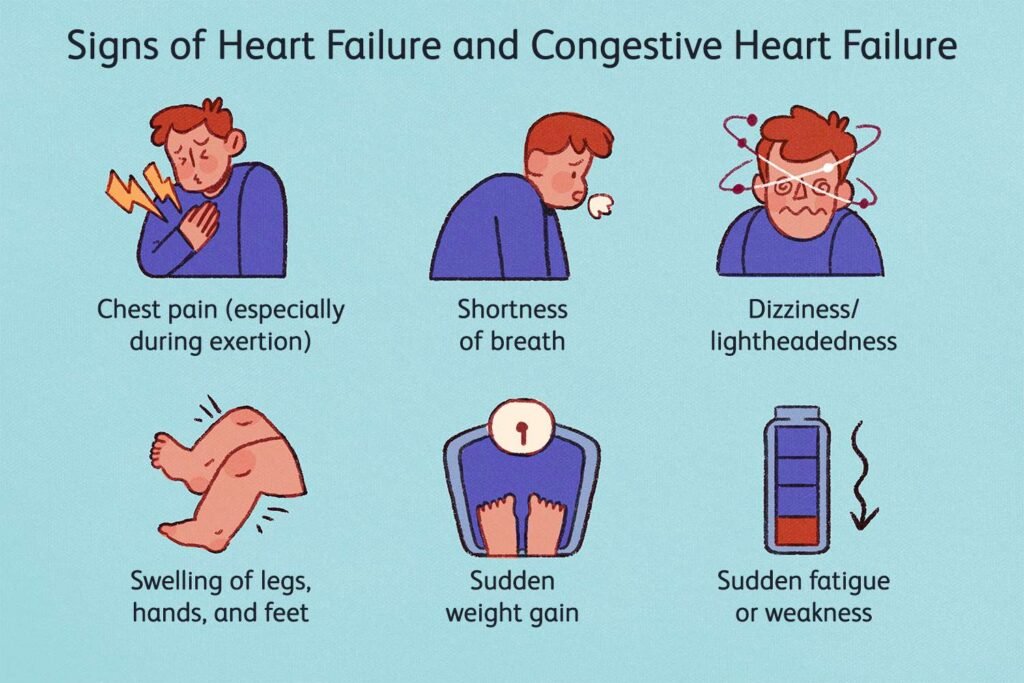
Signs and Symptoms
Shortness of breath
One of the most common signs of congestive heart failure is experiencing shortness of breath, also known as dyspnea. This symptom occurs when excess fluid builds up in the lungs, making it difficult for you to breathe properly. You may feel like you can’t catch your breath even during normal activities or while lying down. It’s important to pay attention to any changes in your breathing pattern and seek medical attention if you notice persistent shortness of breath.
Fatigue
Feeling tired and lacking energy is another common symptom of congestive heart failure. When your heart doesn’t pump efficiently, your organs and muscles may not receive enough oxygenated blood, leading to fatigue. If you find yourself becoming easily exhausted or struggling to perform everyday tasks, it could be a sign that your heart is not functioning properly.
Swelling in the legs, ankles, and feet
Congestive heart failure can cause fluid to accumulate in your body, leading to swelling in the legs, ankles, and feet. This condition is known as peripheral edema. You may notice that your shoes feel tighter or that there are visible indentations on your skin when you remove your socks. It’s essential to monitor any swelling and notify your healthcare provider if it persists or worsens over time.
Rapid or irregular heartbeat
Changes in your heart rate may indicate congestive heart failure. You might experience a rapid or irregular heartbeat, also known as palpitations. This symptom can be unsettling and may be accompanied by a feeling of fluttering or pounding in your chest. It’s essential to discuss any irregularities in your heart rate with your doctor, as they may require further evaluation and management.
Coughing with pink or white phlegm
A persistent cough that produces pink or white phlegm can be a telling symptom of congestive heart failure. This type of cough is often referred to as a “frothy” cough and occurs due to fluid accumulation in the lungs. If you notice this symptom, it’s crucial to seek medical attention, as it may indicate fluid overload in your body.
Physical Examination
Listening to the heart and lungs
During a physical examination for congestive heart failure, your healthcare provider will use a stethoscope to listen to your heart and lungs. They will pay attention to any abnormal sounds, such as murmurs, irregular rhythms, or crackling sounds in your lungs. These findings can provide essential clues about the functioning of your heart and lungs.
Checking blood pressure
Measuring your blood pressure is a routine part of a congestive heart failure evaluation. High blood pressure can contribute to the development of heart failure and is an important risk factor to consider. Your healthcare provider will assess both your systolic and diastolic blood pressure to determine if they fall within the normal range or require further management.
Examining the abdomen and extremities
During the physical examination, your healthcare provider may palpate your abdomen and extremities to assess for any signs of fluid retention. Swelling, tenderness, or an enlarged liver may suggest the presence of congestive heart failure or related complications. Additionally, they will check your pulses in various locations to evaluate the blood flow to your extremities.
Assessing skin color and temperature
The color and temperature of your skin can provide valuable information about your heart function. Pale or bluish skin may indicate inadequate oxygenation, while a flushed appearance might suggest a different underlying cause. Your healthcare provider will carefully observe your skin during the physical examination to help determine the severity and impact of congestive heart failure.

Diagnostic Tests
Electrocardiogram (ECG)
One of the initial diagnostic tests for congestive heart failure is an electrocardiogram (ECG). This non-invasive test measures the electrical activity of your heart and can detect abnormalities in rhythm or structure. An ECG can help identify underlying heart conditions that may contribute to congestive heart failure.
Chest X-ray
A chest X-ray is commonly performed to assess the condition of your heart and lungs. It can reveal signs of fluid buildup or an enlarged heart. This imaging test provides your healthcare provider with valuable information about the size, shape, and position of your heart and lungs, assisting in the diagnosis of congestive heart failure.
Echocardiogram
An echocardiogram is a key diagnostic test for congestive heart failure. This ultrasound examination uses sound waves to create images of your heart’s structure and function. It allows your healthcare provider to evaluate the pumping ability of your heart and assess the overall health of its valves and chambers.
Blood tests
Blood tests can provide valuable information about your overall health and any potential underlying causes of congestive heart failure. These tests may include a complete blood count, blood chemistry panel, thyroid function tests, and specific markers to assess heart function and damage. They help your healthcare provider determine the appropriate treatment plan and address any underlying conditions contributing to your symptoms.
Stress test
A stress test, also known as an exercise tolerance test, evaluates how well your heart functions during physical exertion. During this test, you’ll be asked to walk on a treadmill or ride a stationary bicycle while your heart rate, blood pressure, and electrocardiogram are monitored. It helps determine if your heart can handle the increased demand of physical activity and can identify any potential underlying issues contributing to congestive heart failure.
Coronary angiography
Coronary angiography is an invasive diagnostic test that allows your healthcare provider to visualize the blood vessels supplying your heart muscle. A contrast dye is injected into the arteries, and X-ray images are taken to identify any blockages or narrowing of the vessels. This test helps determine if coronary artery disease is a contributing factor to your congestive heart failure.
Medical History and Risk Factors
Discussing symptoms and their duration
When evaluating congestive heart failure, your healthcare provider will discuss your symptoms in detail. They will inquire about how long you’ve been experiencing symptoms and whether there have been any notable changes over time. Understanding the duration and progression of your symptoms helps guide the diagnostic process and determine the appropriate treatment plan.
Reviewing past medical conditions
A thorough review of your past medical conditions is crucial when assessing congestive heart failure. Your healthcare provider will inquire about any previous heart conditions, such as prior heart attacks, heart valve problems, or arrhythmias. They will also review any other underlying medical conditions, such as diabetes, hypertension, or kidney disease, which may contribute to the development of congestive heart failure.
Assessing family history of heart disease
Family history can play a significant role in determining your risk for congestive heart failure. Your healthcare provider will ask about any family members who have been diagnosed with heart disease or experienced heart-related conditions. This information helps assess your genetic predisposition and understand any potential inherited factors that may contribute to your condition.
Identifying risk factors
Your healthcare provider will identify and evaluate various risk factors associated with congestive heart failure. These risk factors may include obesity, smoking, sedentary lifestyle, high blood pressure, high cholesterol levels, and a family history of heart disease. Recognizing and addressing these risk factors is crucial for managing and preventing future complications.
Inquiring about lifestyle choices
Understanding your lifestyle choices is essential when assessing congestive heart failure. Your healthcare provider will inquire about your diet, physical activity level, alcohol and tobacco use, and stress management. Lifestyle modifications, such as following a heart-healthy diet and engaging in regular exercise, can play a significant role in managing congestive heart failure and improving overall heart health.

Evaluating Heart Function
Ejection fraction measurement
Ejection fraction (EF) is a critical measurement of heart function. It assesses the percentage of blood pumped out of the heart’s left ventricle with each heartbeat. A normal ejection fraction is typically between 50% and 70%. A reduced ejection fraction may suggest heart failure with reduced systolic function. Ejection fraction measurement helps determine the severity and classification of congestive heart failure.
Cardiac catheterization
Cardiac catheterization is an invasive procedure used to diagnose and assess congestive heart failure. A thin tube, called a catheter, is inserted into your blood vessels and advanced to your heart. Contrast dye is then injected, allowing for X-ray visualization of the heart’s blood vessels and chambers. This test provides detailed information about the structure and function of your heart.
Nuclear stress test
A nuclear stress test is a diagnostic tool used to evaluate how well your heart performs under stress. During this test, a small amount of a radioactive tracer is injected into your bloodstream, which allows for the visualization of blood flow to your heart muscle. This test can help identify areas of reduced blood flow and assess the overall functioning of your heart.
Differentiating from Other Conditions
Pulmonary edema
Pulmonary edema is a condition that results from fluid accumulation in the lungs and shares several symptoms with congestive heart failure. However, pulmonary edema is considered a medical emergency caused by severe heart failure or acute lung injury. Distinguishing between congestive heart failure and pulmonary edema is crucial as the treatment approaches may differ.
Asthma
Asthma is a chronic respiratory condition that shares some symptoms with congestive heart failure. Wheezing, shortness of breath, and coughing can be present in both conditions. However, asthma is primarily characterized by airway inflammation and bronchoconstriction, while congestive heart failure is related to heart dysfunction. Proper evaluation and diagnostic tests can help differentiate between these two conditions.
Chronic obstructive pulmonary disease (COPD)
Chronic obstructive pulmonary disease (COPD) is a progressive lung disease that can coexist with congestive heart failure. Symptoms such as shortness of breath, chronic cough, and wheezing can be present in both conditions. A comprehensive evaluation by a healthcare provider, including pulmonary function tests and imaging studies, can help differentiate between congestive heart failure and COPD.
Pneumonia
Pneumonia is an infection of the lungs that can present with symptoms similar to congestive heart failure, such as coughing and shortness of breath. However, pneumonia is caused by a bacterial or viral infection, whereas congestive heart failure results from compromised heart function. Medical history, physical examination findings, and diagnostic tests are vital in distinguishing between the two conditions.
Pleural effusion
Pleural effusion is the buildup of fluid between the layers of tissue lining the lungs and chest cavity. This condition can cause symptoms similar to congestive heart failure, such as shortness of breath and chest discomfort. However, pleural effusion occurs due to various underlying causes, including congestive heart failure. Diagnostic tests, such as imaging studies and analysis of the fluid, help differentiate pleural effusion from congestive heart failure.
Anemia
Anemia is a condition characterized by a low level of red blood cells or hemoglobin in the blood. It can cause symptoms similar to congestive heart failure, such as fatigue and shortness of breath. Anemia can coexist with heart failure or be an underlying cause. Blood tests measuring hemoglobin levels help evaluate the presence of anemia in congestive heart failure patients.
Hypothyroidism
Hypothyroidism is an underactive thyroid condition that can contribute to the development or exacerbation of congestive heart failure. Symptoms such as fatigue, weight gain, and swelling are common in both conditions. Blood tests measuring thyroid hormone levels help assess the presence of hypothyroidism and its potential impact on congestive heart failure.
Classification of Congestive Heart Failure
Systolic heart failure
Systolic heart failure, also known as heart failure with reduced ejection fraction, occurs when the left ventricle of the heart fails to contract effectively, resulting in reduced pumping ability. This leads to a decreased ejection fraction and inefficient blood flow throughout the body. Systolic heart failure is one of the most common classifications of congestive heart failure.
Diastolic heart failure
Diastolic heart failure, also known as heart failure with preserved ejection fraction, occurs when the left ventricle of the heart has difficulty relaxing and filling with blood during the resting phase of the cardiac cycle. This results in a preserved ejection fraction but impaired filling. Diastolic heart failure is typically seen in individuals with stiff or thickened heart muscle.
Left-sided heart failure
Left-sided heart failure occurs when the left ventricle is unable to effectively pump blood out to the body. This leads to a backup of fluid in the lungs, causing symptoms such as shortness of breath, fatigue, and coughing. Left-sided heart failure is a common classification of congestive heart failure and can be caused by various underlying conditions.
Right-sided heart failure
Right-sided heart failure occurs when the right ventricle of the heart is unable to effectively pump blood into the lungs to receive oxygen. This leads to fluid retention throughout the body, resulting in swelling in the legs, ankles, and abdomen. Right-sided heart failure is often caused by left-sided heart failure, but can also be caused by other conditions affecting the right side of the heart.
Treatments and Management
Medications
Medications play a crucial role in the treatment and management of congestive heart failure. They can help reduce fluid retention, improve heart function, and manage associated risk factors. Common medications used in the treatment of congestive heart failure include diuretics, ACE inhibitors, beta-blockers, and angiotensin receptor blockers.
Lifestyle modifications
Lifestyle modifications are essential for managing congestive heart failure and improving overall heart health. These modifications include following a heart-healthy diet low in sodium and saturated fat, engaging in regular exercise as recommended by your healthcare provider, quitting smoking, and managing stress levels. Making these changes can help improve symptoms, increase heart function, and prevent future complications.
Surgical interventions
In some cases, surgical interventions may be required to treat congestive heart failure. Procedures such as coronary artery bypass grafting (CABG) or percutaneous coronary intervention (PCI) may be necessary to improve blood flow to the heart muscle. Additionally, valve repair or replacement surgeries can be performed to address any underlying valve-related abnormalities contributing to congestive heart failure.
Implantable devices
Implantable devices are often used in the management of congestive heart failure. These devices can help regulate heart rhythm, improve heart function, and monitor fluid levels in the body. Common implantable devices include pacemakers, implantable cardioverter-defibrillators (ICDs), and cardiac resynchronization therapy (CRT) devices.

Prognosis and Complications
Survival rates
The prognosis for individuals with congestive heart failure varies depending on several factors, including the underlying cause, severity, and overall health of the patient. It’s important to note that congestive heart failure is a chronic condition that requires ongoing management. With appropriate treatment, adherence to lifestyle modifications, and regular medical follow-up, many individuals with congestive heart failure can live fulfilling lives.
Causes of mortality
Congestive heart failure can lead to several complications that can contribute to mortality. These complications may include arrhythmias, heart attacks, pulmonary embolism, kidney failure, and stroke. Addressing and managing these complications are crucial for improving survival rates and overall outcomes.
Potential complications
Congestive heart failure can give rise to various complications that can impact your overall health and quality of life. These complications may include fluid buildup in the lungs (pulmonary edema), kidney damage, liver congestion, and peripheral artery disease. Regular medical monitoring and adherence to treatment plans can help minimize the risk and impact of these complications.
Impact of treatment
Proper treatment and management can significantly impact the outcomes and quality of life for individuals with congestive heart failure. By effectively managing symptoms, reducing fluid buildup, optimizing heart function, and addressing underlying causes, treatment can help improve survival rates, reduce hospitalizations, and enhance overall well-being.
Quality of life
Living with congestive heart failure can significantly impact your quality of life. Symptoms such as shortness of breath, fatigue, and limited physical abilities may affect everyday activities and emotional well-being. However, with proper medical care, lifestyle modifications, and support, individuals with congestive heart failure can still lead fulfilling and meaningful lives. Building a strong support network, participating in cardiac rehabilitation programs, and staying proactive in managing your health can contribute to an improved quality of life.