Dealing with the behavioral symptoms of dementia can be a challenging and overwhelming experience, both for those affected by the condition and their loved ones. These symptoms, which can include agitation, aggression, wandering, and hallucinations, pose significant challenges to caregivers and can impact the overall well-being and quality of life for those with dementia. However, with the right strategies and approaches, it is possible to effectively manage these symptoms and create a more supportive and comfortable environment for individuals living with dementia. In this article, we will explore some practical tips and techniques that can help you navigate the complex world of behavioral symptoms in dementia, empowering you to provide the best possible care and support for your loved one.
What is Dementia?
Dementia is a term that refers to a group of diseases and conditions characterized by a decline in cognitive function, memory loss, and changes in behavior. It is not a specific disease but rather a syndrome that affects the brain, leading to problems with thinking, reasoning, and memory. Dementia can be a progressive condition, meaning it worsens over time, and it can significantly impact a person’s ability to carry out daily activities and maintain their independence.
Definition of dementia
Dementia is defined as a set of symptoms that affect the brain and hinder cognitive functioning. It is characterized by a decline in memory, thinking, and reasoning abilities, which in turn affects a person’s behavior and ability to perform daily tasks. Although dementia mainly affects older individuals, it is not a normal part of aging. It is important to understand that dementia is not a specific disease, but rather a collection of symptoms caused by various diseases and conditions.
Types of dementia
There are various types of dementia, each with its own set of characteristics and underlying causes. Some of the most common types of dementia include Alzheimer’s disease, vascular dementia, Lewy body dementia, frontotemporal dementia, and mixed dementia.
-
Alzheimer’s disease is the most common type of dementia, accounting for around 60-80% of cases. It is characterized by the accumulation of beta-amyloid plaques and tau tangles in the brain, leading to the death of brain cells and subsequent cognitive decline.
-
Vascular dementia is caused by reduced blood flow to the brain due to a series of small strokes or damage to blood vessels. It is the second most common type of dementia and often coexists with Alzheimer’s disease.
-
Lewy body dementia is characterized by the presence of abnormal protein deposits called Lewy bodies in the brain. People with Lewy body dementia may experience cognitive symptoms similar to Alzheimer’s disease, as well as visual hallucinations and fluctuations in alertness.
-
Frontotemporal dementia is a group of disorders characterized by the degeneration of the frontal and temporal lobes of the brain. It affects personality, behavior, and language abilities more prominently than memory.
-
Mixed dementia refers to a combination of different types of dementia, most commonly Alzheimer’s disease and vascular dementia.
Common Behavioral Symptoms of Dementia
Understanding behavioral symptoms
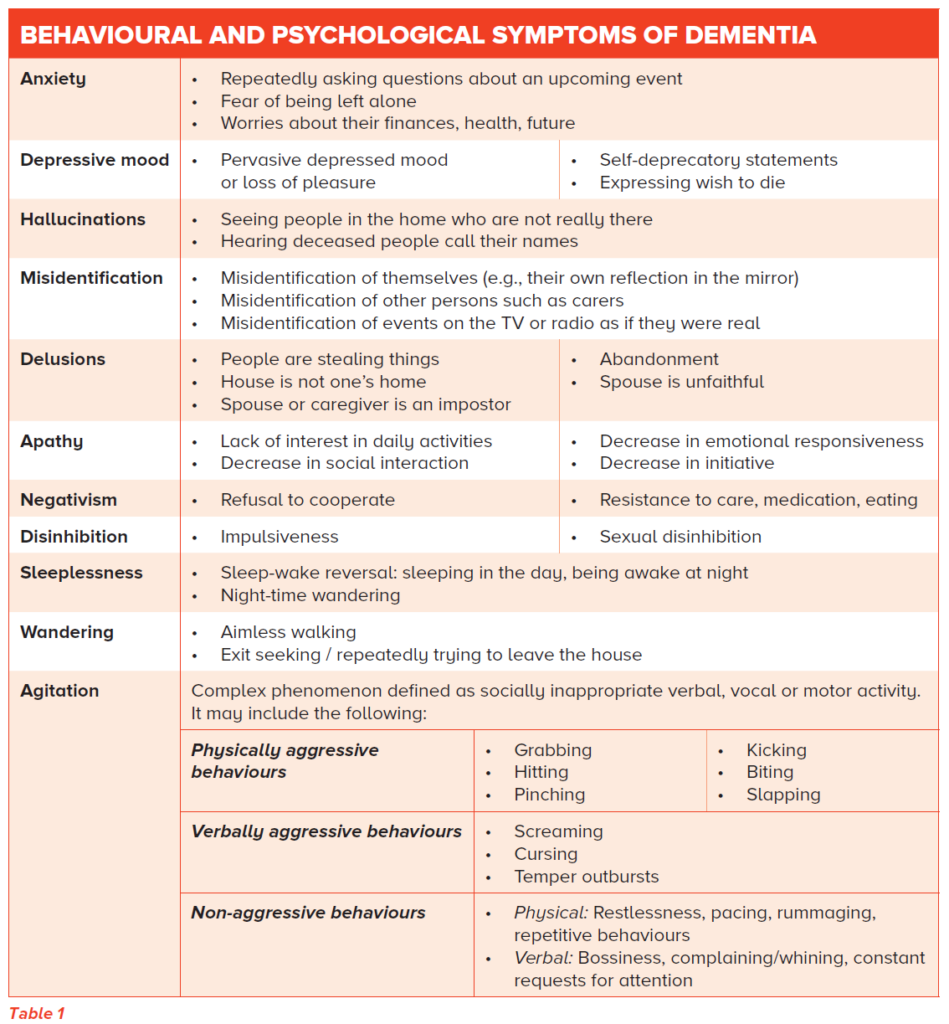
Behavioral symptoms are common among individuals with dementia and can significantly impact their quality of life and that of their caregivers. These symptoms can manifest as changes in mood, personality, and behavior. It is important to understand that these behavioral symptoms are not intentional but rather a result of the changes occurring in the brain.
Agitation
Agitation refers to a state of restlessness, anxiety, or general unease that affects individuals with dementia. It can be characterized by pacing, aggression, verbal outbursts, and difficulty in expressing oneself. Agitation can often be triggered by environmental factors, such as noise, unfamiliar surroundings, or overstimulation, and it is important to identify and address these triggers.
Aggression
Aggression is a challenging behavioral symptom of dementia that can be distressing for both the individual with dementia and their caregivers. It might manifest as physical or verbal aggression, resistance to care, or agitation escalating to aggressive behavior. Aggression can have various causes, including unmet needs, frustration, pain, or the inability to communicate effectively.
Wandering
Wandering is a behavior commonly observed in individuals with dementia, particularly in the later stages of the disease. It involves aimlessly moving around without a clear purpose or destination. Wandering can pose safety risks, as individuals may become disoriented, lost, or injured. It is crucial to ensure a secure and safe environment for individuals prone to wandering.
Sundowning
Sundowning, also known as late-day confusion, refers to a syndrome where individuals with dementia experience increased confusion, restlessness, and agitation during the late afternoon and evening hours. The exact cause of sundowning is unclear, but factors such as exhaustion, difficulty separating dreams from reality, and disruptions in the internal body clock may contribute to this phenomenon.
Delusions and hallucinations
Delusions and hallucinations can occur in individuals with dementia, particularly in the later stages of the disease or in specific types of dementia such as Lewy body dementia. Delusions are false beliefs that are firmly held and not based on reality, while hallucinations involve perceiving things that are not actually present. These symptoms can be distressing for both the individual with dementia and their caregivers, and it is important to provide reassurance and support.
Depression and anxiety
Depression and anxiety are common among individuals with dementia and can significantly impact their well-being. Changes in the brain, loss of independence, and difficulties in communication and understanding contribute to the development of these mental health conditions. Identifying and addressing depression and anxiety is crucial for ensuring the overall well-being of individuals with dementia.

Causes of Behavioral Symptoms in Dementia
Neurological changes
The behavioral symptoms observed in dementia are a result of the structural and chemical changes occurring in the brain. As brain cells are progressively damaged and die, the communication between different regions of the brain is disrupted. This leads to changes in cognitive function, behavior, and mood. The specific neurological changes vary depending on the type of dementia, but they all contribute to the manifestation of behavioral symptoms.
Environment and triggers
The environment plays a significant role in triggering and exacerbating behavioral symptoms in individuals with dementia. Factors such as noise, unfamiliar surroundings, overstimulation, lack of routine, and poor lighting can contribute to agitation, aggression, and wandering. Creating a calm, familiar, and structured environment can help minimize these triggers and reduce behavioral symptoms.
Unmet needs and communication issues
Behavioral symptoms in dementia can also arise from unmet needs and difficulties in communication. As cognitive function declines, individuals may have difficulty expressing their needs, leading to frustration and agitation. It is essential for caregivers to be attentive to non-verbal cues and find alternative forms of communication, such as using visual or tactile cues, to understand and address these needs.
Assessment and Diagnosis
Identifying behavioral symptoms
Identifying and understanding the behavioral symptoms in individuals with dementia is crucial for effective management and care. Caregivers and healthcare professionals should observe and document changes in behavior, mood, and cognition to identify patterns and triggers. This information can help in developing appropriate strategies and interventions to address these symptoms.
Medical evaluation
When behavioral symptoms become significant or impact the individual’s overall well-being, a medical evaluation by a healthcare professional specializing in the field of dementia is essential. A thorough medical evaluation will help determine the underlying cause of these symptoms and identify any treatable conditions that may be contributing to the behavioral changes.
Dementia staging and assessment tools
Dementia staging and assessment tools are used to determine the severity of cognitive decline and functional impairment in individuals with dementia. These tools, such as the Mini-Mental State Examination (MMSE) or the Clinical Dementia Rating (CDR), provide a standardized way of assessing and monitoring cognitive function over time. The results of these assessments help guide treatment decisions and care planning.

Non-Pharmacological Approaches
Person-centered care
Person-centered care is an approach that focuses on understanding and addressing the needs and preferences of individuals with dementia. It involves treating each person as an individual, respecting their autonomy, and involving them in decision-making. Person-centered care aims to enhance the individual’s well-being, maintain their dignity, and promote their independence as much as possible.
Structured routines and environmental modifications
Establishing structured routines and making environmental modifications can help reduce confusion and agitation in individuals with dementia. Consistent daily routines provide familiarity and predictability, while environmental modifications, such as removing clutter and reducing noise, create a calm and safe space. These strategies can help individuals feel more secure and reduce the risk of behavioral symptoms.
Validation therapy
Validation therapy is an approach that acknowledges and accepts the emotions and experiences expressed by individuals with dementia, even if they are not based in reality. It involves offering empathy, validation, and support rather than correcting or arguing with the individual. Validation therapy can help individuals with dementia feel heard and understood, reducing their distress and behavioral symptoms.
Reminiscence therapy
Reminiscence therapy involves encouraging individuals with dementia to recall and share their memories, experiences, and personal stories. This therapeutic approach can help improve mood, cognition, and overall well-being. Reminiscing about positive events or engaging in activities that evoke pleasant memories can be particularly beneficial in reducing behavioral symptoms.
Music and art therapy
Music and art therapy have shown to be effective in reducing behavioral symptoms in individuals with dementia. Listening to familiar music or engaging in art activities can promote relaxation, improve mood, and stimulate memories. These forms of therapy provide individuals with dementia a means of self-expression, creativity, and emotional connection.
Pet therapy
Pet therapy involves interactions with trained animals, such as dogs or cats, for therapeutic purposes. The presence of animals can provide comfort, companionship, and emotional support to individuals with dementia. Pet therapy has been shown to reduce agitation, increase social interactions, and improve overall well-being in individuals with dementia.
Recreation and physical activities
Engaging individuals with dementia in recreational and physical activities can help reduce behavioral symptoms and improve their overall well-being. Activities such as gentle exercises, walking, gardening, or participating in hobbies can provide mental and physical stimulation. These activities promote social interaction, maintain motor skills, and enhance cognitive function.
Pharmacological Approaches
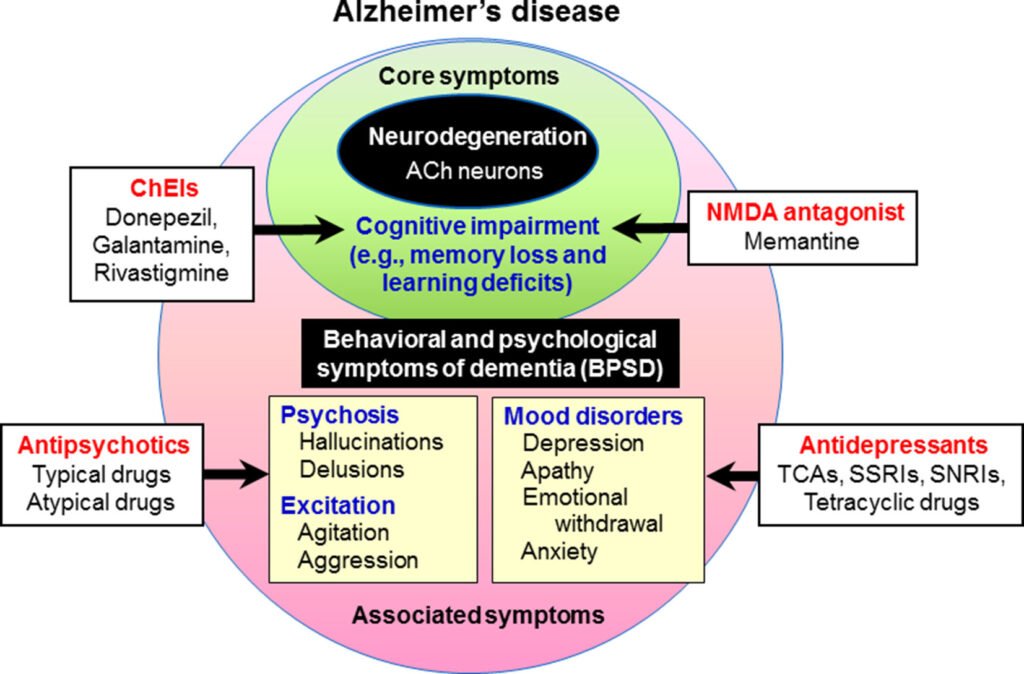
Antipsychotic medications
Antipsychotic medications may be prescribed in certain cases to manage severe behavioral symptoms, such as aggression or psychosis, in individuals with dementia. However, their use should be carefully considered due to potential side effects, particularly in older adults. Antipsychotic medications should only be used under the guidance and close supervision of a healthcare professional.
Antidepressant medications
Depression and anxiety are common in individuals with dementia, and antidepressant medications may be prescribed to manage these symptoms. Selective serotonin reuptake inhibitors (SSRIs) are often used due to their tolerability and efficacy in older adults. However, the use of antidepressant medications should be closely monitored, and individual response should be assessed regularly.
Anxiolytic medications
Anxiolytic medications, such as benzodiazepines, may be prescribed to manage severe anxiety or agitation in individuals with dementia. However, their use should be limited as they can cause sedation, confusion, and an increased risk of falls. Non-pharmacological approaches should be considered first, and the use of anxiolytic medications should be carefully monitored and evaluated.
Other medications for specific symptoms
Various other medications may be prescribed to manage specific symptoms associated with dementia. For example, cholinesterase inhibitors, such as donepezil, rivastigmine, and galantamine, are commonly used to manage cognitive symptoms in Alzheimer’s disease. Medications to manage sleep disturbances, pain, or other comorbid conditions may also be prescribed based on individual needs.
Caregiver Strategies and Support
Education and training
Caregivers of individuals with dementia require education, training, and support to effectively manage and care for their loved ones. Understanding the disease progression, behavioral symptoms, and techniques for communication and behavior management can help caregivers provide appropriate care and support. Caregiver education programs and support groups are valuable resources in providing caregivers with the necessary knowledge and skills.
Communicating effectively
Effective communication is essential when caring for individuals with dementia. Caregivers should use simple and concise language, maintain eye contact, and speak slowly and calmly. Non-verbal cues, such as facial expressions and gestures, can also facilitate communication. Creating a calm and quiet environment, free from distractions, can enhance communication and reduce misunderstandings.
Encouraging independence
Promoting independence in individuals with dementia can help maintain their sense of dignity and autonomy. Caregivers should provide opportunities for individuals to engage in tasks and activities they can still manage independently. Adjustments and adaptations should be made to support their abilities while ensuring safety and minimizing frustration.
Providing a calm and safe environment
Creating a calm and safe environment is essential in managing behavioral symptoms in individuals with dementia. Caregivers should minimize noise, clutter, and other potential triggers of agitation. Ensuring appropriate lighting, clear pathways, and access to familiar and comforting items can promote a sense of security and reduce confusion.
Managing caregiver stress and burnout
Caring for someone with dementia can be emotionally and physically challenging. Caregivers must prioritize self-care and seek support to prevent burnout. This can be achieved by taking breaks, seeking respite care, and utilizing support services available within the community. Connecting with other caregivers and accessing counseling or therapy can also provide valuable support.
Special Considerations for Hospitalized Patients
Preventing and managing behavioral symptoms in hospital settings
Hospitalization can be particularly challenging for individuals with dementia due to unfamiliar surroundings, disrupted routines, and increased stress. It is important for hospitals to have protocols in place to prevent and manage behavioral symptoms in this population. Measures such as minimizing noise, providing familiar items, and ensuring clear communication can help reduce distress and agitation.
Collaboration between dementia care team and hospital staff
Collaboration between the dementia care team and hospital staff is crucial to ensure the well-being of hospitalized patients with dementia. This collaboration involves sharing information about the individual’s needs, preferences, and behavioral symptoms. It is vital for hospital staff to receive training on dementia care and be aware of the specific challenges faced by individuals with dementia.
Ensuring patient safety and comfort
Ensuring patient safety and comfort is a priority when caring for individuals with dementia in a hospital setting. Measures such as fall prevention strategies, proper hydration and nutrition, and providing familiar items or reminiscence aids can help alleviate anxiety and promote a sense of security. Healthcare professionals should also be attentive to the individual’s pain management needs and provide appropriate intervention.
Ethical and Legal Considerations
Informed consent
Respecting the autonomy and dignity of individuals with dementia requires obtaining informed consent for medical interventions and decisions regarding their care. Informed consent involves providing individuals with information about their condition, proposed treatments or procedures, and potential risks and benefits, in a way that they can understand. Communication techniques should be adapted to meet the individual’s cognitive abilities.
Advance directives and end-of-life care
Advance directives allow individuals to express their preferences for medical care and end-of-life decisions while they are still capable of making decisions. It is important for individuals with dementia to have advance directives in place to ensure their wishes regarding medical interventions and end-of-life care are respected, even when they are no longer able to communicate or make decisions.
Guardianship and decision-making
As dementia progresses, individuals may reach a point where they are no longer able to make informed decisions or take care of their own affairs. In such cases, it may be necessary for a guardian to be appointed to make decisions on their behalf. This guardianship process should be guided by ethical principles and ensure the person’s best interests are upheld.
Promising Research and Future Directions
Non-invasive brain stimulation
Non-invasive brain stimulation techniques, such as transcranial magnetic stimulation (TMS) or transcranial direct current stimulation (tDCS), are being explored as potential therapies for individuals with dementia. These techniques aim to stimulate specific areas of the brain to enhance cognitive function and reduce behavioral symptoms. However, further research is needed to determine their efficacy and safety.
Targeted therapies for specific symptoms
Researchers are investigating targeted therapies for specific symptoms in individuals with dementia. For example, interventions targeting sleep disturbances, agitation, or depression may provide more effective and personalized treatment options. By understanding the underlying causes of these symptoms, targeted therapies can be developed to address them more effectively.
Improving care through technology
Technology has the potential to significantly improve the care and quality of life for individuals with dementia. Developments in assistive technologies, such as smart home systems or wearable devices, can assist individuals in managing their daily activities, monitoring their health, and enhancing safety and security. Technology-based interventions, such as virtual reality or cognitive training programs, may also offer therapeutic benefits.
Early detection and prevention strategies
Early detection of dementia allows for timely interventions and support, which may slow down the progression of the disease and improve outcomes. Researchers are focusing on developing better screening tools and biomarkers to identify individuals at risk of developing dementia at earlier stages. Additionally, lifestyle interventions, such as exercise, cognitive stimulation, and healthy diet, are being studied as potential strategies for preventing or delaying the onset of dementia.
In conclusion, managing behavioral symptoms in individuals with dementia requires a comprehensive and person-centered approach. Understanding the underlying causes of these symptoms and utilizing non-pharmacological approaches, such as person-centered care, environmental modifications, and therapeutic activities, can significantly improve the well-being of individuals with dementia. When necessary, pharmacological interventions should be carefully considered and monitored. Providing support and education for caregivers is crucial, and special considerations should be taken for hospitalized patients. Ethical and legal considerations, as well as promising research, offer hope for future advancements in dementia care. By implementing these strategies and staying informed about emerging research, we can improve the quality of life for individuals with dementia and support their caregivers.