Are you curious to learn more about Dermatitis Herpetiformis? Look no further, because this comprehensive guide has all the information you need. From understanding the symptoms and causes to exploring treatment options, we’ve got you covered. Whether you’re experiencing it yourself or simply want to be well-informed, this article will provide a friendly and engaging overview of Dermatitis Herpetiformis that will leave you satisfied and knowledgeable. So, let’s dive right in and discover everything you need to know about this skin condition.

What is Dermatitis Herpetiformis?
Dermatitis Herpetiformis (DH) is a chronic skin condition characterized by a rash that is intensely itchy and often accompanied by burning sensations. The name “dermatitis herpetiformis” is somewhat misleading, as the condition is not caused by the herpes simplex virus, but by an autoimmune reaction triggered by gluten ingestion. DH is often seen in individuals with celiac disease, and both conditions share a strong connection. It is important to understand the causes, symptoms, diagnosis, and treatment options for DH to effectively manage this condition and maintain a good quality of life.
Causes of Dermatitis Herpetiformis
Dermatitis Herpetiformis has multiple causes, including celiac disease, genetics, and immunological factors.
Celiac Disease
Celiac disease is an autoimmune disorder that affects the small intestine and is triggered by gluten consumption. Gluten is a protein found in wheat, barley, and rye. When individuals with celiac disease consume gluten, their immune system mistakenly targets the small intestine, leading to damage and inflammation. The presence of DH in individuals with celiac disease suggests a common trigger and highlights the connection between the two conditions.
Genetics
Genetics also play a significant role in the development of dermatitis herpetiformis. There is a strong association between DH and specific genetic markers, such as HLA-DQ2 and HLA-DQ8. These genetic markers are commonly found in individuals with celiac disease and DH, further emphasizing the genetic link between these conditions.
Immunological Factors
Immunological factors contribute to the development of DH. In individuals with DH, the immune system produces antibodies known as immunoglobulin A (IgA) antibodies. These antibodies bind to gluten in the small intestine, forming complexes that are then deposited under the skin, triggering the characteristic rash and associated symptoms.
Symptoms of Dermatitis Herpetiformis
Symptoms of dermatitis herpetiformis primarily affect the skin and can vary in severity from person to person. Common symptoms include a skin rash, itching and burning sensation, blisters and lesions, and scarring and hyperpigmentation.
Skin Rash
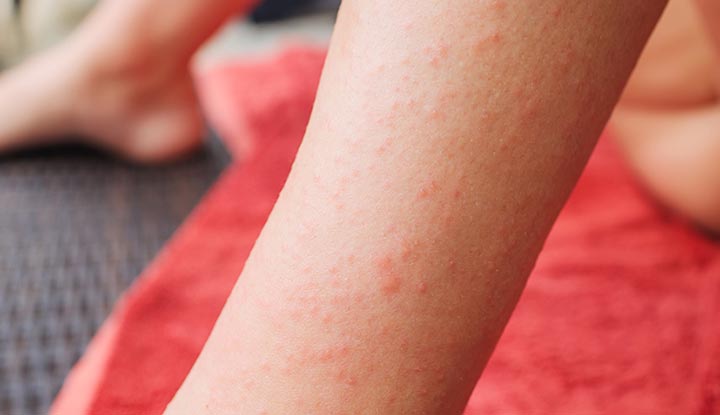
The hallmark symptom of DH is the presence of a skin rash. The rash is typically symmetrical and commonly appears on the elbows, knees, buttocks, back, or scalp. The rash consists of red raised bumps, which may be filled with fluid. Scratching the rash can cause it to become more inflamed.
Itching and Burning Sensation
DH is notorious for causing intense itching, which can be debilitating for individuals. The itchiness is often accompanied by a burning sensation, making it difficult for affected individuals to find relief. Scratching the affected areas can lead to more severe symptoms and potential scarring.
Blisters and Lesions
Blisters and lesions are common in dermatitis herpetiformis. The blisters, which are filled with clear fluid, often form symmetrically over the areas affected by the rash. These blisters can burst and form open sores, leading to a higher risk of infection if not properly cared for.
Scarring and Hyperpigmentation
If left untreated or if the rash is repeatedly scratched, DH can result in scarring and hyperpigmentation. Scarring may be permanent, and hyperpigmentation can take months or even years to fade. Proper management and treatment of DH are crucial to minimize the risk of long-term cosmetic complications.
Diagnosis of Dermatitis Herpetiformis
Diagnosing dermatitis herpetiformis involves a combination of clinical evaluation, skin biopsy, and blood tests.
Biopsy of the Skin
A skin biopsy is often the most reliable way to diagnose dermatitis herpetiformis. During a biopsy, a small piece of skin is removed and examined under a microscope to look for characteristic changes associated with DH. The presence of IgA deposits in the skin layers is a key finding in dermatitis herpetiformis.
Blood Tests
Blood tests can be helpful in supporting the diagnosis of DH. Individuals suspected of having DH often have elevated levels of IgA antibodies. Blood tests may also be used to check for other markers associated with celiac disease, such as antibodies to tissue transglutaminase (tTG) or endomysium (EMA).
IgA Antibody Measurement
Measuring IgA antibodies in the affected skin can aid in the diagnosis of dermatitis herpetiformis. A special staining technique called direct immunofluorescence (DIF) can detect the presence and distribution of IgA deposits in the skin. Biopsies taken near active lesions are often the most informative for this test.

Treatment Options for Dermatitis Herpetiformis
Treatment options for dermatitis herpetiformis primarily focus on relieving symptoms, managing the underlying autoimmune process, and preventing complications. The most common treatment measures include a gluten-free diet, dapsone medication, and topical creams and ointments.
Gluten-Free Diet
Adopting a strict gluten-free diet is the cornerstone of managing dermatitis herpetiformis. By eliminating gluten from the diet, the immune system’s response is reduced, leading to improvements in symptoms and a decrease in skin rash severity. Consultation with a registered dietitian specializing in celiac disease is recommended to ensure proper adherence to a gluten-free diet.
Dapsone Medication
Dapsone is an oral medication that is often prescribed to individuals with dermatitis herpetiformis. Dapsone helps control the skin rash and provides relief from itching and burning sensations. Regular monitoring of blood counts is necessary due to potential side effects of dapsone, such as anemia and liver toxicity.
Topical Creams and Ointments
Topical creams and ointments can provide symptomatic relief by reducing itchiness and inflammation associated with DH. Corticosteroid creams, such as hydrocortisone or betamethasone, can help reduce redness and itching. Calamine lotion or emollients may also be recommended to soothe and hydrate the skin.
Coping with Dermatitis Herpetiformis
Coping with dermatitis herpetiformis involves a multifaceted approach that includes following a gluten-free diet, managing itchiness and discomfort, and taking care of the skin.
Following a Gluten-Free Diet
Adhering to a strict gluten-free diet is essential for individuals with dermatitis herpetiformis and celiac disease. This involves avoiding all sources of gluten, including wheat, barley, rye, and certain processed foods that may contain hidden gluten. Check food labels carefully and opt for gluten-free alternatives to maintain a balanced and nutritious diet.
Managing Itchiness and Discomfort
Dealing with the intense itchiness and discomfort associated with DH can be challenging. Strategies to manage itchiness include avoiding scratching, wearing loose and breathable clothing, using cold compresses, and taking soothing baths. Over-the-counter antihistamines may also provide temporary relief.
Taking Care of Skin
Proper skincare is crucial for individuals with dermatitis herpetiformis. Gently cleanse the skin using mild, fragrance-free cleansers and lukewarm water. Avoid harsh soaps and abrasive scrubs that can further irritate the skin. Apply moisturizers regularly to prevent skin dryness and promote healing.

Dietary Considerations for Dermatitis Herpetiformis
Individuals with dermatitis herpetiformis should pay special attention to their diet and be aware of gluten-free foods, hidden sources of gluten, and cross-contamination prevention.
Gluten-Free Foods
A gluten-free diet primarily consists of whole, unprocessed foods such as fruits, vegetables, lean proteins, and gluten-free grains like rice, quinoa, and corn. It is essential to read food labels carefully, as some products may contain hidden sources of gluten, such as sauces, marinades, and seasonings.
Hidden Sources of Gluten
Gluten can be present in unexpected places. Be cautious of processed foods, including certain sauces, soups, gravies, salad dressings, and even medications or vitamin supplements. Oats may also be a concern, as they can be contaminated with gluten during processing. Opt for certified gluten-free oats if they are part of your diet.
Cross-Contamination Prevention
To prevent cross-contamination, it is crucial to maintain separate kitchen tools, cutting boards, and utensils for gluten-free cooking. Avoid using shared toasters, and thoroughly clean countertops and surfaces before preparing gluten-free meals. When dining out, communicate your dietary requirements to ensure the avoidance of cross-contamination in restaurant kitchens.
Complications of Dermatitis Herpetiformis
If left untreated or poorly managed, dermatitis herpetiformis can lead to several complications, including intestinal damage, iron deficiency anemia, and osteoporosis.
Intestinal Damage
Untreated dermatitis herpetiformis can result in ongoing damage to the small intestine, similar to celiac disease. This can lead to malabsorption of essential nutrients such as vitamins, minerals, and fats, causing deficiencies and related health problems.
Iron Deficiency Anemia
Individuals with dermatitis herpetiformis may develop iron deficiency anemia due to intestinal damage and malabsorption. Iron deficiency can lead to symptoms such as fatigue, weakness, and shortness of breath. Regular monitoring of iron levels is important to detect and manage anemia promptly.
Osteoporosis
Dermatitis herpetiformis and celiac disease are both associated with a higher risk of developing osteoporosis. Malabsorption of calcium, vitamin D, and other essential nutrients can weaken bones over time, increasing the risk of fractures. Regular bone density scans and calcium and vitamin D supplementation may be recommended to prevent the progression of osteoporosis.

Research and Future Perspectives
Ongoing research aims to improve our understanding of dermatitis herpetiformis and identify potential drug therapies for more effective treatment.
Ongoing Studies
Researchers are investigating various aspects of dermatitis herpetiformis, including the underlying immune mechanisms, genetic factors, and potential triggers. Ongoing studies may provide insights into new treatment approaches and better management strategies for this condition.
Potential Drug Therapies
Scientists are exploring several potential drug therapies for dermatitis herpetiformis. Some of these may include medications targeting specific immune pathways or alternatives to dapsone with fewer side effects. As research progresses, new treatment options may become available to improve symptom control and quality of life for individuals with DH.
Frequently Asked Questions about Dermatitis Herpetiformis
Here are some frequently asked questions about dermatitis herpetiformis, along with brief answers.
Can dermatitis herpetiformis occur without celiac disease?
Yes, dermatitis herpetiformis can occur without celiac disease, although the majority of individuals with DH also have celiac disease. Dermatitis herpetiformis can also manifest in individuals with gluten sensitivity or as an isolated condition without an underlying gluten-related disorder.
Can dermatitis herpetiformis be cured?
While there is no known cure for dermatitis herpetiformis, the condition can be effectively managed through adhering to a strict gluten-free diet and appropriate medications. With proper treatment and lifestyle adjustments, individuals with dermatitis herpetiformis can experience significant improvement and relief from symptoms.
Is dermatitis herpetiformis contagious?
No, dermatitis herpetiformis is not contagious. It cannot be spread from person to person through direct contact or any other means. The condition is solely the result of an individual’s immune system reacting to gluten ingestion and does not involve any infectious agents.