Whether you’ve recently been diagnosed with a germ cell tumor or are seeking information about the diagnosis and treatment options, this article is here to help you understand the complexities of this condition. Germ cell tumors may sound daunting, but with the right diagnosis and proper treatment, the chances of successful recovery are high. In this article, we will explore the various methods used to accurately diagnose germ cell tumors and the multiple treatment options available, enabling you to approach this challenging journey with confidence.
Diagnosis and Treatment of Germ Cell Tumors

Overview of Germ Cell Tumors
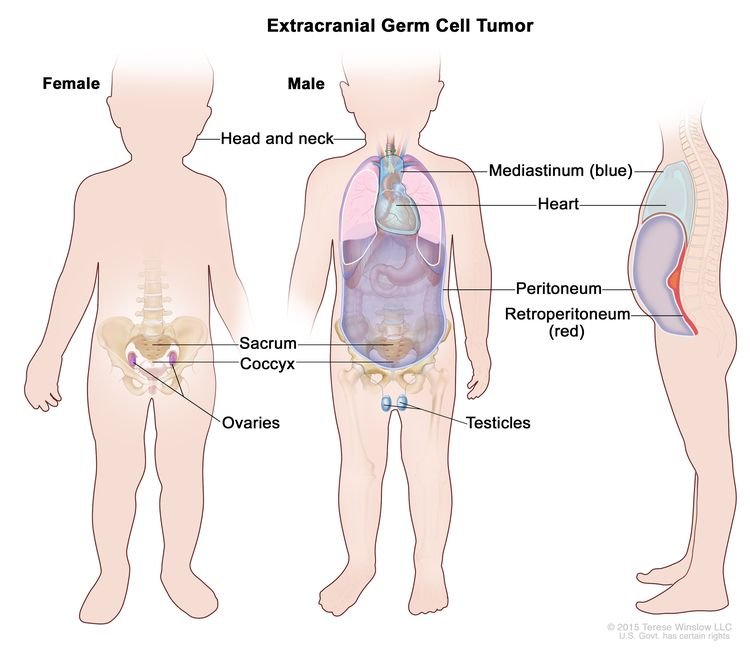
Germ cell tumors are a form of cancer that originates in the cells that develop into sperm or eggs. These tumors can occur in various locations, including the testicles, ovaries, and other sites within the body where these cells are present. Germ cell tumors can be classified into two main types: seminomas and nonseminomas. Seminomas are typically slower growing and more responsive to radiation therapy, while nonseminomas tend to grow more quickly and require chemotherapy for treatment.
Diagnosis of Germ Cell Tumors
1.1 Physical Examination
During the diagnosis process, a thorough physical examination is essential. The healthcare provider will carefully examine the affected area, such as the testicles or ovaries, to check for any signs of abnormal growths or lumps. In the case of testicular germ cell tumors, the physician will feel the testicles for any masses or changes in size. For ovarian germ cell tumors, a pelvic examination may be performed to assess the ovaries.
1.2 Imaging Studies
Imaging studies play a vital role in the diagnosis of germ cell tumors. The following imaging techniques are commonly used:
1.2.1 Ultrasound
Ultrasound uses high-frequency sound waves to create images of the internal organs. This non-invasive procedure can provide detailed images of the testicles, ovaries, and surrounding structures, allowing healthcare providers to identify any abnormal growths or tumors present.
1.2.2 Computed Tomography (CT)
Computed tomography, also known as CT scanning, combines multiple X-ray images to create cross-sectional images of the body. CT scans are commonly used to determine the size and location of a tumor and to assess its spread to nearby lymph nodes or other organs.
1.2.3 Magnetic Resonance Imaging (MRI)
MRI uses a powerful magnetic field and radio waves to generate detailed images of the body’s internal structures. This imaging technique is particularly useful in evaluating the extent of tumor involvement, especially in the brain and spinal cord.
1.3 Blood Tests
Blood tests can help detect certain substances in the blood that may indicate the presence of a germ cell tumor. The following blood tests are commonly used for diagnosis:
1.3.1 Alpha-fetoprotein (AFP)
Elevated levels of alpha-fetoprotein in the blood may suggest the presence of a nonseminoma tumor, particularly in the testicles. Serial measurement of AFP levels can also be used to monitor treatment response and assess for recurrence.
1.3.2 Human Chorionic Gonadotropin (HCG)
Human chorionic gonadotropin is another hormone that can be elevated in the blood of patients with germ cell tumors, particularly nonseminomas. Similar to AFP, HCG levels can be monitored during treatment and follow-up.
1.3.3 Lactate Dehydrogenase (LDH)
LDH is an enzyme that may be elevated in the blood of patients with germ cell tumors. However, it is less specific than AFP or HCG and is often used in conjunction with other markers for diagnosis and monitoring.
Staging and Classification of Germ Cell Tumors
2.1 Stages of Germ Cell Tumors
Staging is an important aspect of diagnosing germ cell tumors as it helps determine the extent of the disease and guides treatment decisions. Germ cell tumors are staged based on various factors, including the size of the tumor, involvement of lymph nodes, and presence of distant metastasis. The stages of germ cell tumors are as follows:
2.1.1 Stage 1
In stage 1, the tumor is limited to the organ of origin, such as the testicles or ovaries, and has not spread to nearby lymph nodes or distant sites.
2.1.2 Stage 2
Stage 2 germ cell tumors involve spread to nearby lymph nodes, but still remain confined to the organ of origin.
2.1.3 Stage 3
In stage 3, the tumor has spread beyond the organ of origin and may involve multiple lymph nodes or adjacent structures.
2.1.4 Stage 4
Stage 4 germ cell tumors indicate metastasis to distant organs, such as the lungs, liver, or brain.
2.2 Classification of Germ Cell Tumors
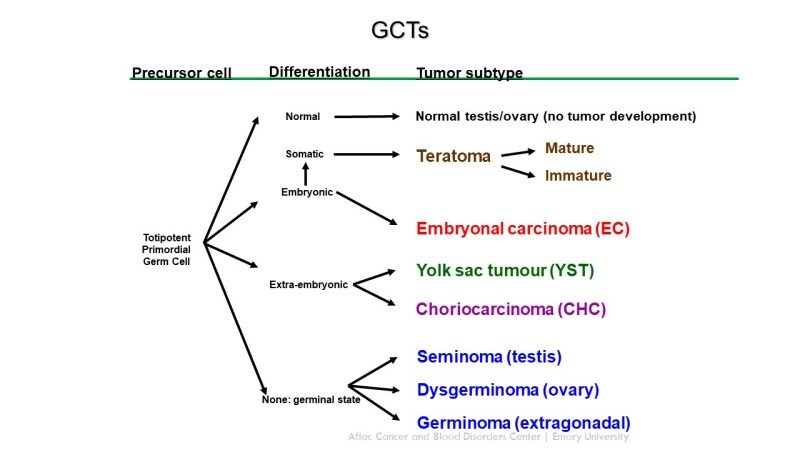
In addition to staging, germ cell tumors are classified into two main types: seminomas and nonseminomas.
2.2.1 Seminomas
Seminomas are germ cell tumors that originate in the cells that produce sperm. They are typically slower growing and less invasive than nonseminomas. Seminomas are more common in older individuals and have a higher likelihood of responding to radiation therapy.
2.2.2 Nonseminomas
Nonseminomas, on the other hand, are faster growing and more aggressive than seminomas. They contain a mixture of different cell types and are further classified into subtypes such as embryonal carcinoma, yolk sac tumor, teratoma, and choriocarcinoma. Nonseminomas are generally more common in younger individuals and often require chemotherapy for optimal treatment.
Treatment Options for Germ Cell Tumors
3.1 Surgery
Surgery is often the primary treatment for both seminomas and nonseminomas, and the specific procedure depends on the tumor type and stage.
3.1.1 Radical Inguinal Orchiectomy
For testicular germ cell tumors, a radical inguinal orchiectomy is usually performed. This surgical procedure involves the removal of the affected testicle through a small incision in the groin area. In some cases, a prosthetic testicle may be inserted for cosmetic purposes.
3.1.2 Retroperitoneal Lymph Node Dissection (RPLND)
RPLND is a surgical procedure used to remove lymph nodes in the retroperitoneal area (located behind the abdominal cavity) for patients with testicular germ cell tumors. It is typically performed to remove cancerous lymph nodes or as a preventive measure to remove potentially cancerous nodes.
3.1.3 Orchidectomy with Preservation of Testicular Blood Supply
In select cases, such as when the affected testicle appears unaffected by cancerous cells on imaging studies, orchidectomy with preservation of the testicular blood supply may be considered. This procedure aims to preserve fertility by removing only the tumor nodules while sparing the healthy tissue.
3.2 Chemotherapy
Chemotherapy is a systemic treatment approach that uses powerful drugs to destroy cancer cells throughout the body. It is an important component of treatment for both seminomas and nonseminomas.
3.2.1 BEP Regimen
The BEP regimen is a commonly used chemotherapy combination for germ cell tumors. It consists of three drugs: bleomycin, etoposide, and cisplatin. This combination has shown high efficacy and a good response rate in treating these types of tumors.
3.2.2 VIP Regimen
Another chemotherapy regimen used for the treatment of germ cell tumors is the VIP regimen, which includes three drugs: etoposide, ifosfamide, and cisplatin. This combination is often used as an alternative for patients who cannot tolerate bleomycin.
3.3 Radiation Therapy
Radiation therapy utilizes high-energy X-rays or other forms of radiation to destroy cancer cells and shrink tumors.
3.3.1 External Beam Radiation Therapy (EBRT)
EBRT is the most commonly used form of radiation therapy for germ cell tumors. It involves targeting high-energy X-rays to the affected area from outside the body to destroy cancer cells.
3.3.2 Brachytherapy
Brachytherapy is a type of radiation therapy where radioactive sources are placed directly near or inside the tumor. It is less commonly used for germ cell tumors but may be considered in certain cases.
3.4 High-dose Chemotherapy and Stem Cell Transplant
For patients with refractory or relapsed germ cell tumors, high-dose chemotherapy followed by a stem cell transplant may be recommended. This intensive treatment approach aims to eradicate any remaining cancer cells and replace the damaged bone marrow with healthy stem cells.
3.5 Surveillance and Follow-up
After the completion of treatment, regular surveillance and follow-up visits are crucial to monitor the patient’s response, detect any recurrence, and manage potential long-term side effects. Imaging studies, blood tests, and physical examinations are typically performed at specific intervals to ensure optimal management and early detection of any recurrence.
In conclusion, the diagnosis and treatment of germ cell tumors involve various procedures and modalities. A multidisciplinary approach, incorporating surgery, chemotherapy, radiation therapy, and close surveillance, is essential for optimal outcomes in patients with these types of tumors. Early detection, accurate staging, and appropriate treatment selection play a vital role in improving the prognosis for individuals affected by germ cell tumors.