Imagine a world where your smile is as confident and bright as ever, no hint of discomfort, pain, or gum disease. Sounds incredible, doesn’t it? Well, understanding gum disease is the first step towards achieving and maintaining that perfect smile. From its causes to the telltale symptoms and the various treatment options available, this article aims to equip you with the necessary knowledge to combat gum disease effectively. So, let’s dive into this informative journey together and uncover everything you need to know about this common dental issue.
Understanding Gum Disease
Gum disease, also known as periodontal disease, is a common dental condition that affects the gums, the tissues surrounding the teeth, and the bone that supports them. It is a progressive condition that starts with inflammation and can lead to tooth loss if left untreated. Understanding gum disease is crucial for maintaining good oral health and preventing serious complications.
What is gum disease?
Gum disease is an infection of the tissues surrounding the teeth. It begins with the buildup of plaque, a sticky film of bacteria that forms on the teeth. If not removed through proper oral hygiene practices, plaque hardens and forms tartar. This leads to irritation and inflammation of the gums, known as gingivitis. If gingivitis is not treated, it can progress to more severe stages of gum disease, such as periodontitis and advanced periodontitis.
Prevalence of gum disease
Gum disease is a prevalent oral health condition, affecting a significant portion of the population. According to the Centers for Disease Control and Prevention (CDC), nearly half of adults in the United States aged 30 or older have some form of gum disease. The prevalence increases with age, with approximately 70% of adults over the age of 65 having gum disease. These statistics highlight the importance of understanding and addressing gum disease to maintain optimal oral health.
Complications of gum disease
If left untreated, gum disease can lead to various complications beyond oral health issues. It can increase the risk of tooth loss, as the infection weakens the supporting structures of the teeth. Gum disease has also been linked to jawbone deterioration, which can result in changes to facial structure and difficulties with chewing and speaking. Additionally, research has shown a connection between gum disease and systemic diseases such as heart disease, diabetes complications, and respiratory problems. Understanding these potential complications reinforces the need for early detection and treatment of gum disease.
Causes of Gum Disease
Gum disease develops as a result of various factors and habits. Understanding the causes can help individuals take preventive measures and maintain good oral health.
Plaque and tartar buildup
The primary cause of gum disease is the accumulation of plaque and its hardened form, tartar, on the teeth and along the gumline. Plaque contains harmful bacteria that produce toxins, irritating the gums and leading to inflammation.
Poor oral hygiene
Inadequate oral hygiene practices, such as infrequent brushing and flossing, allow plaque to build up, increasing the risk of gum disease. Proper oral hygiene, including regular brushing, flossing, and mouthwash use, is essential in preventing gum disease.
Smoking and tobacco use
Smoking and using tobacco products significantly increase the risk of gum disease. These habits reduce blood flow to the gums, impair the immune system’s ability to fight infections, and hinder the healing process, making gum disease more severe and difficult to treat.
Hormonal changes
Hormonal changes, such as those experienced during puberty, pregnancy, and menopause, can make gums more sensitive and prone to inflammation. This hormonal imbalance can contribute to the development and progression of gum disease.
Genetic predisposition
Some individuals may have a genetic predisposition to gum disease. If there is a family history of gum disease, it is essential for these individuals to be vigilant about their oral health and seek professional dental care regularly.
Certain medications
Certain medications, such as anticonvulsants and oral contraceptives, can increase the risk of gum disease. These medications may alter the oral environment, leading to gum inflammation and an increased likelihood of gum disease.

Symptoms of Gum Disease
Recognizing the symptoms of gum disease is crucial for early detection and prompt treatment. By being aware of these signs, individuals can seek professional help and prevent the condition from progressing further.
Gum inflammation
One of the early signs of gum disease is red, swollen, and tender gums. Healthy gums should appear firm and pale pink, so any signs of inflammation should not be ignored.
Bleeding gums
Gums that bleed easily, especially during brushing or flossing, can be an indication of gum disease. Bleeding gums are a result of the infection and inflammation caused by the buildup of plaque along the gumline.
Persistent bad breath
Halitosis, or bad breath, is a common symptom of gum disease. Bacteria present in the infected gums produce foul-smelling gases, resulting in persistent bad breath that cannot be eliminated by regular brushing, flossing, or using mouthwash.
Receding gumline
As gum disease progresses, the gums may start to recede, creating an elongated appearance of the teeth. This can make the teeth appear longer and can expose the tooth roots, leading to tooth sensitivity.
Sensitive teeth
Gum disease can cause the gum tissue to recede, exposing the roots of the teeth. When the roots are exposed, it can lead to tooth sensitivity, particularly to hot and cold temperatures.
Loose or shifting teeth
As gum disease advances, the infection weakens the supporting structures of the teeth, leading to loose or shifting teeth. If left untreated, this can eventually result in tooth loss.
Stages of Gum Disease
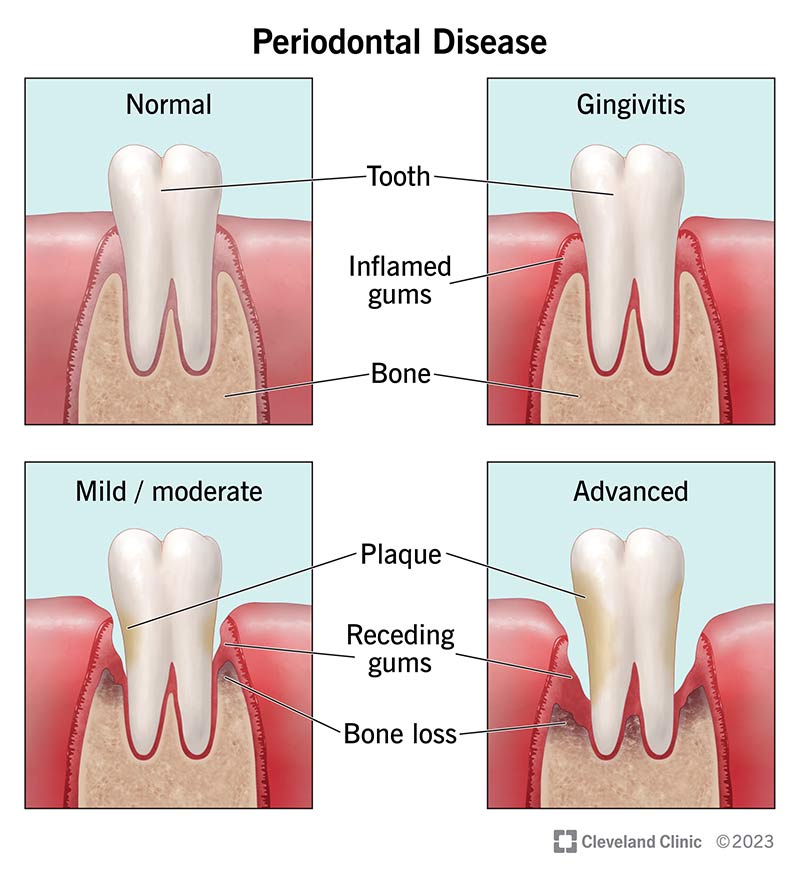
Gum disease progresses through different stages, each with its own characteristics and level of severity. Understanding the stages of gum disease can help individuals and dental professionals determine appropriate treatments and interventions.
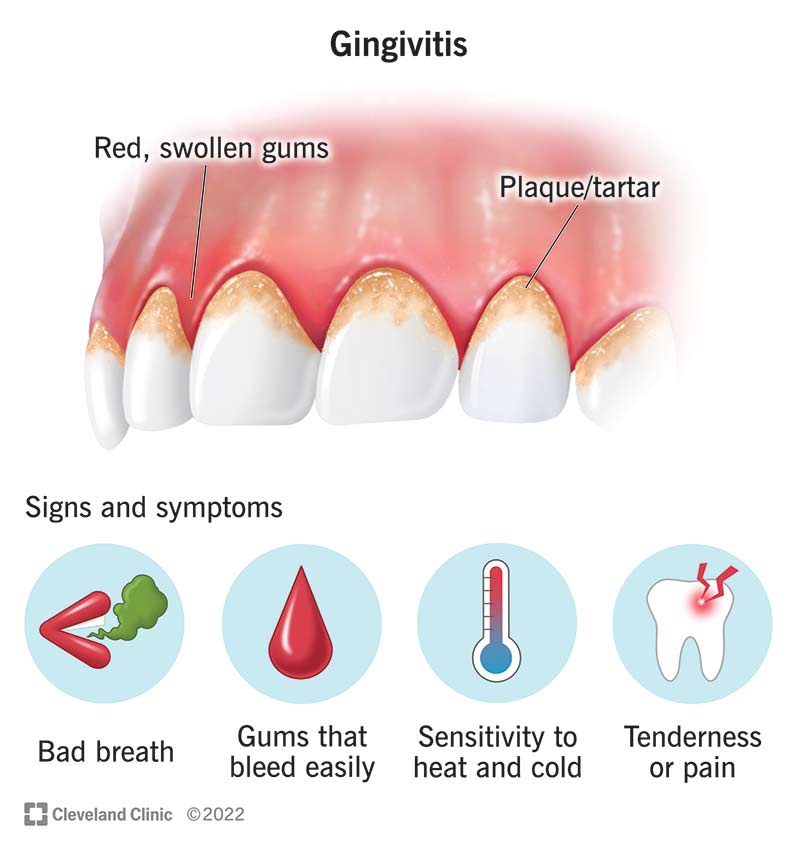
Gingivitis
Gingivitis is the earliest stage of gum disease and is characterized by swollen, red, and bleeding gums. At this stage, the infection is limited to the gum tissue and has not yet affected the underlying bone structure. With prompt treatment and proper oral hygiene, gingivitis can be reversed.
Periodontitis
If gingivitis is left untreated, it can progress to periodontitis, a more severe form of gum disease. In periodontitis, the infection spreads beyond the gum tissue and starts to attack the supporting bone and fibers that hold the teeth in place. This can lead to tooth loss and requires more extensive treatment to control the infection and prevent further damage.
Advanced periodontitis
Advanced periodontitis is the most severe stage of gum disease. At this stage, the infection has caused significant damage to the gums, bone, and fibers supporting the teeth. Tooth loss, changes in facial structure, and difficulties with basic oral functions, such as chewing and speaking, may occur. Advanced periodontitis requires aggressive treatment and, in some cases, surgical interventions.
Diagnosing Gum Disease
Diagnosing gum disease involves a comprehensive evaluation of the patient’s oral health. Dental professionals use various methods to assess the presence and severity of gum disease, allowing them to develop an appropriate treatment plan.
Visual examination
A visual examination is one of the first steps in diagnosing gum disease. The dentist or dental hygienist will inspect the gums for signs of inflammation, bleeding, recession, and other indications of gum disease.
Probing of gum pockets
Probing of gum pockets involves using a dental instrument called a probe to measure the depth of the space between the gums and teeth. Deep pocket depths indicate the presence of gum disease and the severity of the infection.
X-rays
X-rays, such as periapical or bitewing radiographs, may be taken to assess the condition of the bone supporting the teeth. X-rays can reveal bone loss, which is a significant indicator of advanced gum disease.
Periodontal charting
Periodontal charting involves recording measurements of the gum pockets and other relevant information about the condition of the gums. This comprehensive charting aids in tracking the progress of gum disease and determining the appropriate treatment approach.
Preventing Gum Disease
Prevention plays a crucial role in maintaining optimal oral health and preventing the development of gum disease. By implementing simple preventive measures, individuals can significantly reduce the risk of gum disease.
Brushing and flossing
Regular and thorough brushing and flossing are key to preventing gum disease. Individuals should brush their teeth at least twice a day using a fluoride toothpaste and floss daily to remove plaque and prevent its buildup.
Regular dental check-ups
Regular dental check-ups are essential for early detection and treatment of gum disease. Dental professionals can assess the condition of the gums, remove any plaque or tartar buildup, and provide guidance on proper oral hygiene practices.
Healthy diet and lifestyle
Adopting a healthy diet and lifestyle can contribute to good gum health. A diet rich in fruits, vegetables, and whole grains provides essential nutrients for gum tissue integrity. Avoiding sugary foods and drinks can also help minimize the development of plaque.
Avoiding smoking and tobacco use
Smoking and using tobacco products have detrimental effects on gum health and overall oral health. Quitting smoking and avoiding tobacco use significantly reduce the risk of gum disease and its complications.

Treating Gum Disease
The treatment of gum disease depends on the stage and severity of the condition. Dental professionals can develop personalized treatment plans to address the specific needs of each patient.
Professional dental cleaning
Professional dental cleaning, also known as prophylaxis, is an essential part of gum disease treatment. During a cleaning, the dentist or dental hygienist will carefully remove plaque and tartar from the teeth, including below the gumline.
Scaling and root planing
Scaling and root planing is a non-surgical procedure used to treat gum disease. It involves deep cleaning below the gumline to remove bacterial colonies, plaque, and tartar. This procedure aims to smoothen the tooth roots, allowing the gums to reattach to the teeth and prevent further progression of the disease.
Antibiotic therapy
In some cases, antibiotic therapy may be prescribed to control the infection and reduce inflammation. Antibiotics can be taken orally or applied directly to the affected areas, depending on the severity of the gum disease.
Surgical interventions
Advanced stages of gum disease may require surgical interventions to effectively treat the infection and restore oral health. Surgical procedures, such as flap surgery or bone grafting, can address severe gum recession, bone loss, and deep gum pockets.
Gum grafting
In cases of significant gum recession, gum grafting may be performed. This procedure involves taking tissue from another area of the mouth or using synthetic materials to cover exposed tooth roots, improve aesthetics, and protect the vulnerable areas.
Laser therapy
Laser therapy is a minimally invasive treatment option for gum disease. It involves using a dental laser to remove infected tissue, kill bacteria, and promote gum healing. Laser therapy can effectively treat gum disease while minimizing discomfort and recovery time.
Complications of Untreated Gum Disease
Untreated gum disease can lead to various complications beyond the oral cavity. Understanding these potential complications emphasizes the importance of early detection and prompt treatment.
Tooth loss
Gum disease is one of the main causes of tooth loss in adults. As the infection progresses, it weakens the supporting structures of the teeth, leading to tooth mobility and eventual loss.
Jawbone deterioration
Advanced gum disease can result in the deterioration of the jawbone, leading to changes in facial structure and difficulties with basic oral functions, such as chewing and speaking. Restoring the jawbone health may require extensive treatments and interventions.
Heart disease
Research suggests a possible link between gum disease and heart disease. The bacteria present in gum infections can enter the bloodstream and contribute to the development of cardiovascular problems, including heart disease and stroke.
Diabetes complications
Gum disease can have adverse effects on individuals with diabetes. Poorly controlled blood sugar levels can worsen gum disease, and untreated gum disease can make it more challenging to manage diabetes. It is crucial for individuals with diabetes to maintain good oral health and manage their blood sugar levels effectively.
Respiratory problems
The bacteria associated with gum disease can be inhaled into the lungs, potentially causing respiratory problems, such as pneumonia or worsened chronic obstructive pulmonary disease (COPD). Maintaining good oral hygiene and seeking early treatment for gum disease can help prevent these complications.

Gum Disease and Overall Health
Gum disease is not only a dental issue but also has implications for overall health and well-being. Understanding the relationship between gum disease and various systemic diseases is important for individuals to prioritize their oral health and seek appropriate treatment.
Links to systemic diseases
Research has established links between gum disease and systemic diseases such as heart disease, diabetes, and respiratory problems. The presence of gum disease can potentially worsen or contribute to the development of these conditions, highlighting the need for comprehensive oral care.
Impact on pregnancy
Maintaining good oral health during pregnancy is crucial for both the mother and the baby. Gum disease has been linked to adverse pregnancy outcomes, including preterm birth and low birth weight. Pregnant individuals should seek regular dental care and maintain proper oral hygiene to minimize these risks.
Association with diabetes
Gum disease and diabetes have a two-way relationship. Individuals with diabetes are more prone to gum disease due to impaired immune function, and untreated gum disease can make it harder to control blood sugar levels. Managing gum disease effectively is essential for individuals with diabetes to maintain overall health.
Seeking Professional Help
When it comes to gum disease, seeking professional help is key to proper diagnosis, treatment, and prevention. Dental professionals play a vital role in guiding individuals through their oral health journey.
When to see a dentist
It is recommended to see a dentist regularly for routine dental check-ups, which typically occur every six months. However, if any symptoms of gum disease are present, such as red, swollen gums or bleeding during brushing, an immediate dental visit is necessary for proper evaluation and treatment.
The role of dental specialists
For advanced stages of gum disease or complex cases, individuals may be referred to a dental specialist called a periodontist. Periodontists specialize in diagnosing and treating gum disease and can provide advanced treatments and interventions to control and manage the infection.
Treatment costs and insurance coverage
The cost of treating gum disease can vary depending on the severity of the condition, the recommended treatments, and the geographic location. Dental insurance typically covers a portion of the costs, but it is important to check the specifics of the insurance plan for coverage details. Some dental offices may offer payment plans or financing options to make treatment more affordable for patients.
In conclusion, understanding gum disease is essential for maintaining good oral health and overall well-being. By recognizing the causes, symptoms, and stages of gum disease, individuals can take preventive measures, seek timely professional help, and ultimately prevent serious complications. Good oral hygiene, regular dental check-ups, a healthy lifestyle, and avoidance of harmful habits are the keys to preventing and managing gum disease. With appropriate treatment, gum disease can be controlled, oral health can be restored, and long-term complications can be minimized.