You may have heard of Hepatitis B, but do you truly understand what it is? In this article, we will shed light on this viral infection and its impact on the body. From its symptoms and transmission to prevention and treatment, we aim to provide you with a comprehensive understanding of Hepatitis B. So, let’s get started and uncover the facts about this often misunderstood disease.

Overview
What is Hepatitis B?
Hepatitis B is a viral infection that primarily affects the liver. It is caused by the hepatitis B virus (HBV), which can lead to both acute and chronic forms of the disease. HBV is transmitted through contact with the blood, semen, or other body fluids of an infected person.
Causes of Hepatitis B
The main cause of Hepatitis B is the hepatitis B virus, which belongs to the family of Hepadnaviridae. The virus is highly contagious and can be transmitted through various means, including sexual contact, sharing needles or syringes, and from an infected mother to her child during childbirth. It can also be transmitted through contaminated blood transfusions or medical procedures.
Symptoms of Hepatitis B
The symptoms of Hepatitis B can vary from mild to severe and may include fatigue, nausea, vomiting, loss of appetite, abdominal pain, dark urine, clay-colored stools, and jaundice (yellowing of the skin and eyes). Some individuals may not experience any symptoms, while others may develop chronic infection, which can lead to long-term liver damage or even liver cancer if left untreated.
Transmission of Hepatitis B
Hepatitis B can be transmitted through various means, including sexual contact, sharing needles or syringes, and from an infected mother to her child during childbirth. It can also be transmitted through contaminated blood transfusions or medical procedures. The virus is highly contagious and can survive outside the body for up to seven days, making it important to take precautions to prevent its transmission.
Prevention of Hepatitis B
The best way to prevent Hepatitis B is through vaccination. The hepatitis B vaccine is safe and effective, and it is recommended for all infants, children, and adults who have not been previously vaccinated. Other preventive measures include practicing safe sex, avoiding sharing needles or other drug paraphernalia, and ensuring the use of sterile equipment for medical procedures. Additionally, pregnant women should be tested for hepatitis B, and if necessary, receive appropriate antiviral treatment to prevent mother-to-child transmission.
Diagnosis
Blood Tests for Hepatitis B
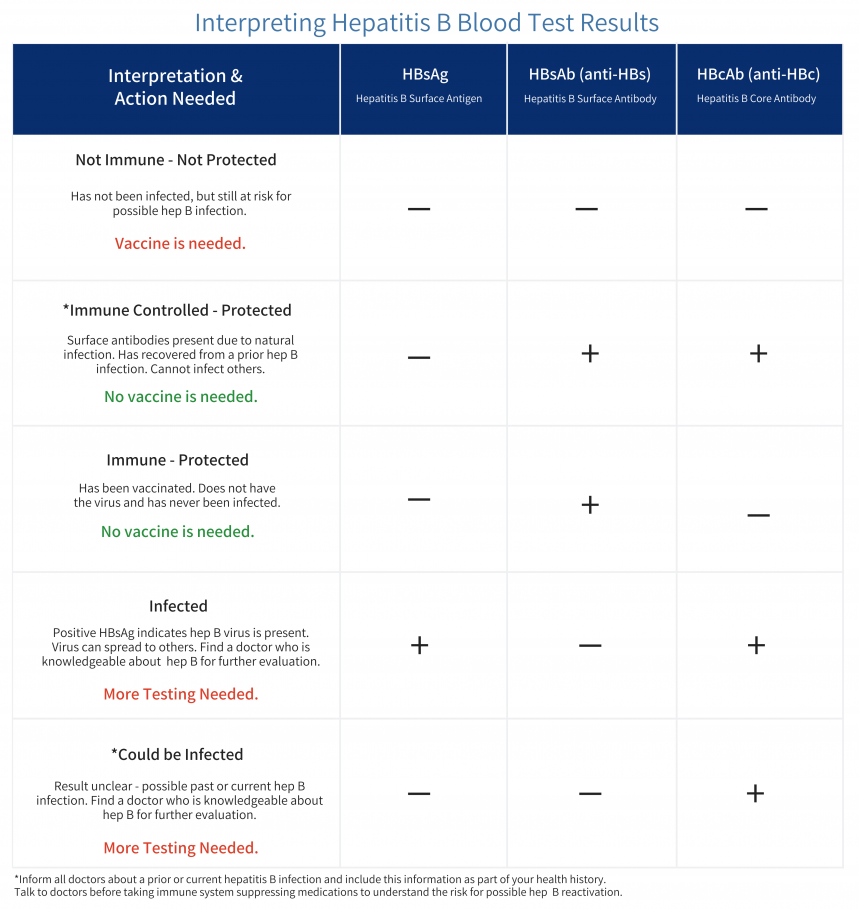
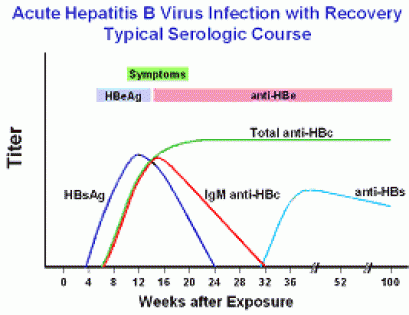
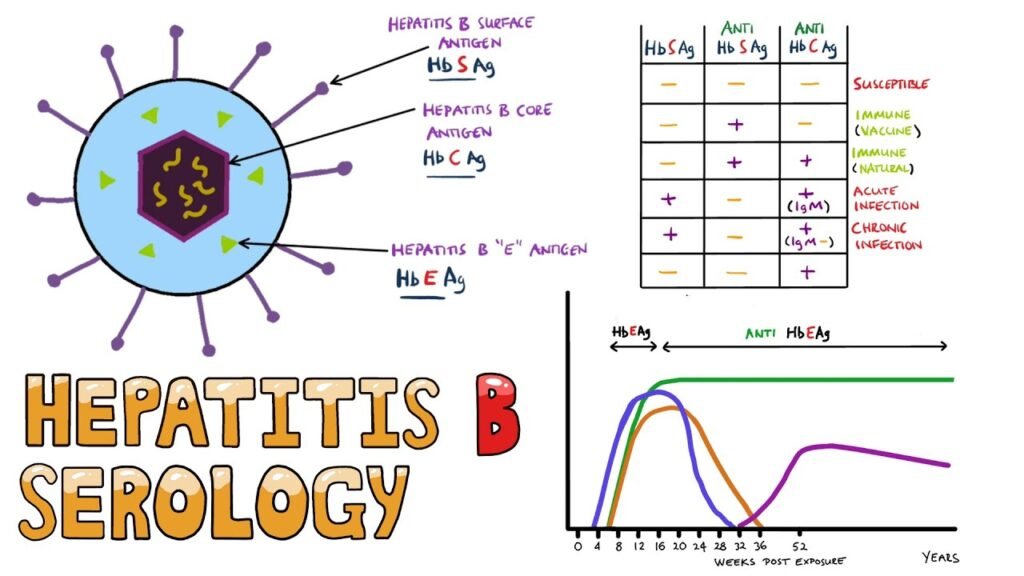
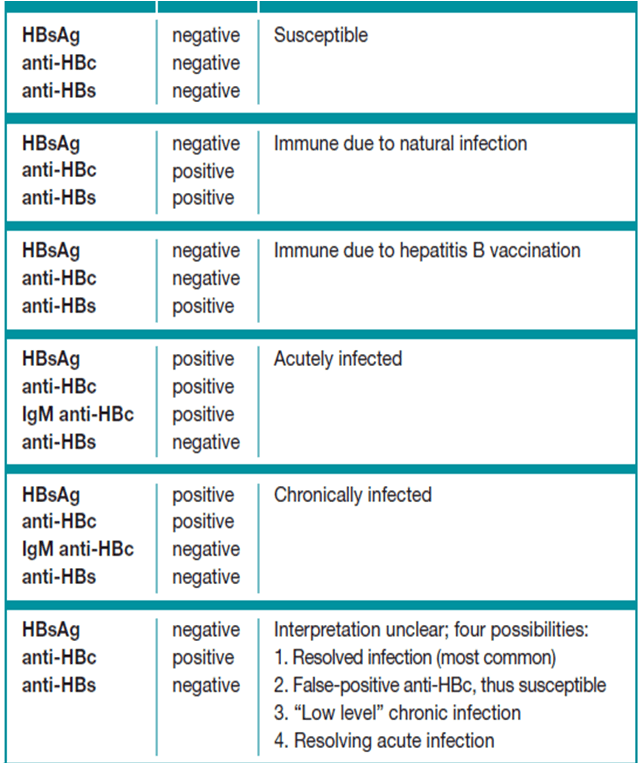
Blood tests are commonly used to diagnose Hepatitis B. These tests detect the presence of specific hepatitis B antigens and antibodies in the blood, which indicate whether a person has been infected with the virus. Some of the common blood tests for Hepatitis B include the hepatitis B surface antigen (HBsAg), hepatitis B core antibody (anti-HBc), and hepatitis B surface antibody (anti-HBs) tests. These tests help determine if a person has acute or chronic hepatitis B infection.
Other Diagnostic Methods
In addition to blood tests, other diagnostic methods may be used to evaluate the extent of liver damage and assess any complications associated with Hepatitis B. These methods include imaging tests such as ultrasound, CT scan, or MRI, which can provide detailed pictures of the liver, and liver biopsy, which involves removing a small sample of liver tissue for examination under a microscope.
Complications
Acute Hepatitis B Complications
Most cases of acute hepatitis B resolve on their own without complications. However, in some cases, acute hepatitis B can lead to severe liver inflammation (fulminant hepatitis), liver failure, or even death. Acute hepatitis B can also progress to become chronic hepatitis B, which may further increase the risk of liver cirrhosis or liver cancer.
Chronic Hepatitis B Complications
Chronic hepatitis B infection can cause ongoing liver inflammation, leading to liver damage and an increased risk of developing liver cirrhosis. Cirrhosis is a condition in which scar tissue replaces healthy liver tissue, impairing liver function. If left untreated, chronic hepatitis B can also increase the risk of developing liver cancer or liver failure.
Treatment
Antiviral Medications
Antiviral medications are commonly used to manage chronic hepatitis B infection and reduce the risk of liver damage and complications. These medications, such as entecavir or tenofovir, help suppress the replication of the hepatitis B virus in the body, which can lead to improved liver function and decreased liver inflammation. However, these medications may need to be taken long-term, as stopping treatment can result in the reactivation of the virus.
Monitoring and Management
Regular monitoring of liver function and viral load, as well as periodic imaging tests, is important in the management of chronic hepatitis B. This helps healthcare providers assess treatment effectiveness and identify any progression of liver disease. It is also essential to adopt a healthy lifestyle, including maintaining a balanced diet, avoiding excessive alcohol consumption, and avoiding exposure to other liver-damaging substances.
Liver Transplantation
In severe cases of chronic hepatitis B with advanced liver disease or liver failure, liver transplantation may be necessary. This involves replacing the diseased liver with a healthy liver from a deceased or living donor. Liver transplantation can be costly and may require lifelong immunosuppressive medications to prevent organ rejection.
Prevention
Vaccination
Vaccination is the most effective way to prevent Hepatitis B. The hepatitis B vaccine is administered through a series of shots and is recommended for all infants, children, and adults who have not been previously vaccinated. It is especially important for individuals at high risk of infection, such as healthcare workers, people with multiple sexual partners, and individuals who inject drugs.
Taking Precautions
Taking precautions to prevent the transmission of Hepatitis B is crucial. This includes practicing safe sex by using barrier methods such as condoms, avoiding sharing needles or other drug paraphernalia, and ensuring the use of sterile equipment for medical procedures. It is also important to use precautions when handling blood or other body fluids, such as wearing gloves and other protective gear.
Preventing Mother-to-Child Transmission
Pregnant women with Hepatitis B should be identified and managed appropriately to reduce the risk of mother-to-child transmission. This involves testing pregnant women for hepatitis B early in pregnancy and administering antiviral medications, such as tenofovir, to reduce the risk of viral transmission to the baby. In addition, newborns of mothers with Hepatitis B should receive both the hepatitis B vaccine and hepatitis B immune globulin shortly after birth.
Epidemiology
Global Prevalence of Hepatitis B
Hepatitis B is a global health problem, with an estimated 257 million people living with chronic hepatitis B infection worldwide. Regions with high prevalence include sub-Saharan Africa, the Western Pacific, and parts of Asia. Despite advancements in prevention and treatment, Hepatitis B continues to be a major public health concern.
High-Risk Populations
Certain populations are at higher risk of acquiring Hepatitis B, including individuals with unprotected sex, intravenous drug users, healthcare workers who are at risk of occupational exposure, and individuals born to mothers infected with hepatitis B. It is important to target these high-risk populations with preventive measures and healthcare interventions to reduce the burden of Hepatitis B.
Hepatitis B and Co-Infections
Hepatitis B infection can have a significant impact on individuals co-infected with other viruses, such as hepatitis C or HIV. Co-infections can complicate the prognosis and management of Hepatitis B and may require specialized healthcare interventions. It is essential to screen for co-infections and provide appropriate care to individuals affected by multiple viral infections.
Impact on Public Health
Healthcare Burden
Hepatitis B places a substantial burden on healthcare systems worldwide. The management of acute and chronic hepatitis B infections requires medical resources, including diagnostic tests, antiviral medications, liver transplantation, and regular monitoring. The cost of providing healthcare services and interventions for hepatitis B can be significant, highlighting the importance of prevention and early detection.
Effect on Quality of Life
Hepatitis B can have a significant impact on the quality of life of affected individuals. The symptoms and complications associated with hepatitis B, such as fatigue, abdominal pain, and liver cirrhosis, can limit physical activity, impair daily functioning, and cause emotional distress. The stigma associated with the disease can also contribute to social isolation and discrimination.
Economic Impact
Hepatitis B has a significant economic impact, both on individuals and society as a whole. The costs associated with healthcare services, including diagnostic tests, antiviral medications, and liver transplantation, can be substantial. In addition, the loss of productivity due to illness and disability caused by hepatitis B can have a significant economic burden on individuals, families, and communities.
Risks and Complications for Specific Populations
Hepatitis B in Children
Children who acquire hepatitis B infection at a young age are at higher risk of developing chronic infection compared to adults. Chronic hepatitis B in children can lead to long-term liver damage, including liver cirrhosis and an increased risk of liver cancer. Vaccination of infants and children is critical in preventing hepatitis B transmission and reducing the burden of the disease in this population.
Hepatitis B in Pregnant Women
Hepatitis B in pregnant women can pose a risk of mother-to-child transmission. It is important to identify pregnant women with hepatitis B early in pregnancy and initiate appropriate interventions to reduce the risk of transmission. Antiviral medications, such as tenofovir, can help reduce viral replication and the chance of vertical transmission. Timely administration of the hepatitis B vaccine and hepatitis B immune globulin to newborns further reduces the risk.
Hepatitis B in People with HIV/AIDS
Hepatitis B and HIV co-infection can have serious health implications. Individuals co-infected with hepatitis B and HIV have a higher risk of developing liver disease and liver-related complications. The management of hepatitis B in people with HIV/AIDS requires specialized medical care, including antiretroviral therapy and close monitoring of liver function.
Stigma and Discrimination
Social Stigma
Hepatitis B is often associated with social stigma and discrimination, primarily due to misconceptions about its transmission and the perception that it is a sexually transmitted disease. This stigma can lead to social isolation, restricted opportunities for education and employment, and impact individuals’ mental health and well-being. Addressing stigma and raising awareness about hepatitis B is crucial in promoting acceptance and support for affected individuals.
Legal Protection and Advocacy
Legal protection and advocacy efforts are necessary to combat stigma and discrimination associated with hepatitis B. Laws and policies should be in place to protect individuals with hepatitis B from discrimination in areas such as employment, education, healthcare, and housing. Advocacy organizations play a vital role in raising awareness, promoting education, and advocating for the rights of individuals affected by hepatitis B.
Future Directions
Research and Development
Investment in research and development is crucial to advance our understanding of hepatitis B and develop new prevention strategies, diagnostics, and treatments. Ongoing research aims to improve the effectiveness of vaccines, develop novel antiviral therapies, and explore potential curative approaches such as the use of gene therapies or immune modulators.
Improved Access to Care
Ensuring equitable access to healthcare services and interventions for hepatitis B is essential. This includes increasing access to hepatitis B vaccination, blood tests for diagnosis and monitoring, antiviral medications, and specialized care for individuals with chronic infection. Efforts should be made to address barriers to care, including financial constraints, lack of awareness, and limited healthcare infrastructure in certain regions.
Public Health Strategies
Public health strategies are crucial in the prevention and control of hepatitis B. These strategies include comprehensive vaccination programs, targeted testing and management of high-risk populations, implementing infection control practices in healthcare settings, and raising public awareness about hepatitis B transmission and prevention. Collaborative efforts between governments, healthcare systems, advocacy organizations, and the community are essential in reducing the global burden of hepatitis B.
In conclusion, Hepatitis B is a significant global health concern that can cause acute and chronic liver disease, liver cirrhosis, and liver cancer if left untreated. Preventive measures such as vaccination, safe sex practices, and avoiding sharing needles are vital in reducing the transmission of hepatitis B. Early diagnosis through blood tests and appropriate management can help mitigate the risks and complications associated with this viral infection. Continued research, access to healthcare, and awareness campaigns are essential in improving the outcomes for individuals affected by hepatitis B and reducing its burden on public health.