If you’ve ever wondered about Hepatitis C – its causes, symptoms, and treatment – then you’ve come to the right place. In this article, we’ll shed light on this viral infection that affects the liver and provide you with a comprehensive understanding of its various aspects. From how it spreads to the signs to watch out for, and the available treatment options, we’ve got you covered. So sit back, relax, and let’s dive into the world of Hepatitis C!

Understanding Hepatitis C
Hepatitis C is a viral infection that affects the liver. It is caused by the hepatitis C virus (HCV) and can lead to serious liver damage if left untreated. In this article, we will explore the definition, prevalence, transmission, risk factors, signs and symptoms, acute and chronic hepatitis C, complications, diagnosis, and treatment of this disease.
Definition
What is Hepatitis C?
Hepatitis C is a viral infection that primarily affects the liver. It is caused by the hepatitis C virus (HCV), which is typically transmitted through blood-to-blood contact. This virus can lead to inflammation and damage to the liver over time.
How does it affect the liver?
Hepatitis C primarily targets the liver, causing inflammation and damage to its cells. The virus can multiply within the liver, leading to chronic inflammation. Over time, this chronic inflammation can progress to fibrosis (scarring), cirrhosis (advanced scarring), and even liver cancer. It is essential to diagnose and treat hepatitis C promptly to prevent long-term liver damage.
Prevalence
Global prevalence
Hepatitis C is a global health concern, with an estimated 71 million people living with chronic HCV infection worldwide. It is most prevalent in low- and middle-income countries, where access to proper healthcare and prevention measures may be limited.
Prevalence in specific countries/regions
The prevalence of hepatitis C can vary across different countries and regions. For example, Egypt has one of the highest rates of hepatitis C infection globally, primarily due to widespread unsafe medical procedures in the past. Other countries with significant HCV prevalence include Pakistan, China, and Russia. It is essential for each country to develop specific strategies to combat the spread of hepatitis C and provide necessary treatment options to those affected.
Transmission
Blood-to-blood transmission
The most common mode of hepatitis C transmission is through blood-to-blood contact. This can occur when sharing needles or other drug paraphernalia, using contaminated healthcare equipment, or receiving blood transfusions or organ transplants from infected donors.
Injection drug use
Injection drug use poses a significant risk for hepatitis C transmission. When individuals share needles, syringes, or other drug equipment, blood-to-blood contact can occur, facilitating the spread of the virus.
Needlestick injuries
Healthcare workers, such as nurses and doctors, may be at risk of contracting hepatitis C through accidental needlestick injuries. If a healthcare professional is exposed to an HCV-infected patient’s blood, the virus can enter their bloodstream and lead to infection.
Mother-to-child transmission
Pregnant women who are infected with hepatitis C can transmit the virus to their unborn child. However, the risk of transmission is relatively low, occurring in approximately 5% of cases. It is crucial for pregnant women with hepatitis C to consult with their healthcare provider to discuss appropriate measures to reduce the risk of transmission.
Unsafe medical procedures
In areas with limited resources and inadequate infection control measures, hepatitis C can be transmitted through unsafe medical procedures. Reusing contaminated needles, syringes, or other medical equipment can lead to the spread of the virus among healthcare settings.
Blood transfusions and organ transplants
Before the implementation of stringent screening measures, the hepatitis C virus could be transmitted through blood transfusions or organ transplants. However, with modern screening techniques, the risk of transmission through these procedures has been significantly reduced.
Sexual transmission
Although sexual transmission of hepatitis C is less common than blood-to-blood contact, it still poses a risk, especially in certain high-risk populations. Unprotected sexual intercourse, particularly in individuals with multiple sex partners, increases the likelihood of HCV transmission.
Sharing personal items
While the risk of hepatitis C transmission through sharing personal items is generally low, it is not entirely negligible. Sharing items such as toothbrushes or razors that may come into contact with blood poses a minimal risk of transmission.

Risk Factors
Various risk factors increase the likelihood of contracting hepatitis C. Understanding these risk factors can help individuals take appropriate preventive measures and seek early diagnosis and treatment if necessary.
Injection drug use
Injection drug use, particularly the sharing of needles and other drug paraphernalia, is a significant risk factor for hepatitis C transmission. It is essential to prioritize harm reduction strategies, such as using sterile equipment or seeking treatment for substance abuse, to minimize the risk of infection.
Unsafe medical procedures
In areas with inadequate infection control practices, receiving medical care or procedures involving contaminated equipment can increase the risk of contracting hepatitis C. It is crucial to ensure that healthcare facilities maintain strict infection control protocols to prevent the transmission of the virus.
Blood transfusions and organ transplants before 1992
People who received blood transfusions or organ transplants before 1992, when effective HCV screening was implemented, are at a higher risk of being infected with hepatitis C. However, the risk of transmission through these procedures is now extremely low, thanks to improved screening methods.
Unprotected sex with multiple partners
Engaging in unprotected sexual intercourse with multiple partners, particularly in high-risk populations, increases the chances of hepatitis C transmission. It is essential to practice safe sex by consistently using barrier methods, such as condoms, to reduce the risk of infection.
Having a sexually transmitted infection
Having a sexually transmitted infection (STI) can increase the risk of hepatitis C transmission, as STIs can cause breaks in the skin and mucous membranes, facilitating the entry of the virus. Proper treatment and prevention of other STIs can help reduce the overall risk of hepatitis C infection.
Being born to a mother with Hepatitis C
Babies born to mothers infected with hepatitis C have a chance of contracting the virus during childbirth. While the risk of transmission is relatively low, it is still important for healthcare providers to monitor and evaluate infants born to HCV-positive mothers.
Exposure to contaminated needles
Accidental needlestick injuries, particularly among healthcare workers, can lead to hepatitis C infection. Proper training in infection control practices and the use of safety measures, such as needlestick prevention devices, can help mitigate the risk in these occupational settings.
Occupational exposure in healthcare settings
Healthcare workers who frequently come into contact with blood or contaminated medical equipment are at an increased risk of hepatitis C infection. Following strict infection control protocols and using appropriate personal protective equipment can help minimize the occupational risk.
Signs and Symptoms
Acute Hepatitis C Symptoms
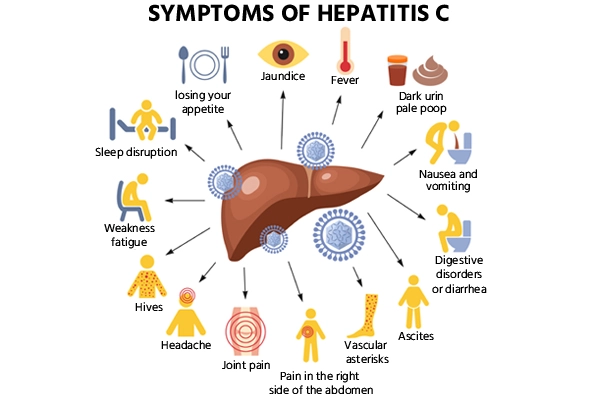
Many individuals infected with hepatitis C may not experience any symptoms during the acute phase. However, for those who do, common symptoms may include fatigue, fever, loss of appetite, nausea, vomiting, abdominal pain, dark urine, clay-colored stools, joint pain, and jaundice (yellowing of the skin and eyes).
Chronic Hepatitis C Symptoms
During the chronic phase of hepatitis C infection, most individuals remain asymptomatic for an extended period, often years or even decades. When symptoms do occur, they may include ongoing fatigue, jaundice, abdominal pain, itchy skin, dark urine, pale stools, and fluid accumulation in the legs and abdomen. If left untreated, chronic hepatitis C can lead to severe liver damage, cirrhosis, and other complications.

Acute Hepatitis C
Definition
Acute hepatitis C refers to the initial phase of HCV infection, typically occurring within six months after exposure. During this stage, the virus actively replicates in the liver, leading to inflammation and potential liver damage.
Symptoms
As mentioned earlier, many individuals with acute hepatitis C do not experience symptoms. However, those who do may notice symptoms similar to those of other viral infections, including fatigue, fever, abdominal discomfort, and jaundice. If you suspect you may have been exposed to HCV, it is essential to seek medical attention for proper diagnosis and treatment.
Timeframe
The acute phase of hepatitis C usually lasts for about six months. However, it is important to note that this timeline can vary among individuals. Some may spontaneously clear the virus within this timeframe, while others may progress to chronic infection.
Spontaneous clearance
Approximately 15-25% of individuals infected with hepatitis C will spontaneously clear the virus during the acute phase without medical intervention. This means that their immune system can successfully eliminate the virus from their body. However, it is still recommended to seek medical evaluation and follow-up, even if spontaneous clearance occurs, to ensure proper monitoring and prevention of long-term complications.
Chronic Hepatitis C
Definition
Chronic hepatitis C refers to the ongoing presence of HCV in the body for more than six months. It is characterized by persistent liver inflammation and potential long-term liver damage if left untreated.
Long-term effects
Chronic hepatitis C can have long-term effects on the liver and overall health. Without appropriate treatment and management, it can progress to advanced liver scarring (cirrhosis) and potentially lead to liver cancer or liver failure.
Liver damage and cirrhosis
Chronic inflammation caused by hepatitis C can result in the formation of scar tissue in the liver, a condition known as cirrhosis. Cirrhosis can disrupt liver function, impair blood flow, and lead to complications such as portal hypertension, ascites (accumulation of fluid in the abdomen), and hepatic encephalopathy (a decline in brain function due to liver failure).
Liver cancer
Chronic hepatitis C infection increases the risk of developing liver cancer, specifically hepatocellular carcinoma (HCC). Over time, chronic inflammation and liver cell damage can promote the development of cancerous cells. Regular monitoring and early detection of liver cancer are crucial in individuals with chronic hepatitis C.
Other complications
In addition to cirrhosis and liver cancer, chronic hepatitis C can also contribute to other complications. These may include kidney problems, immune system abnormalities, glomerulonephritis, type 2 diabetes, and cardiovascular conditions. It is important for individuals with chronic HCV infection to have regular check-ups and screenings to monitor their overall health.

Complications
Hepatitis C can lead to various complications, primarily affecting the liver. Understanding and recognizing these complications is essential for timely intervention and treatment.
Cirrhosis
As mentioned earlier, hepatitis C-induced chronic inflammation can lead to liver scarring or cirrhosis. Cirrhosis can cause significant liver dysfunction and increase the risk of severe complications, such as liver failure and liver cancer. Regular monitoring and management are crucial to prevent the progression of cirrhosis.
Liver cancer (Hepatocellular carcinoma)
Chronic hepatitis C infection significantly increases the risk of developing hepatocellular carcinoma (HCC), the most common type of liver cancer. Regular surveillance with imaging tests and other diagnostic procedures can help detect liver cancer at an early stage when treatment options are more effective.
Liver failure
In advanced cases of cirrhosis or severe liver damage, hepatitis C can lead to liver failure. Liver failure is a life-threatening condition that requires immediate medical intervention. Liver transplantation may be necessary in severe cases.
Liver transplantation
For individuals with end-stage liver disease or severe liver failure, liver transplantation may be the only treatment option. A liver transplant involves replacing the diseased liver with a healthy one from a deceased or living donor. However, access to liver transplantation may be limited due to scarcity of donor organs and other medical factors.
Diagnosis
Accurate and early diagnosis of hepatitis C is crucial for appropriate treatment and management. Healthcare providers employ various methods to diagnose hepatitis C, such as:
- Blood tests: Blood tests can detect the presence of HCV antibodies and viral RNA in the bloodstream, helping confirm the diagnosis.
- Liver function tests: These tests measure various liver enzymes and proteins that can indicate liver inflammation or damage.
- Imaging tests: Ultrasound, magnetic resonance imaging (MRI), or computed tomography (CT) scans may be used to assess the liver for signs of damage or abnormal growths.
- Liver biopsy: In certain cases, a small sample of liver tissue may be extracted for laboratory analysis to determine the extent of liver damage.
Prompt diagnosis allows individuals with hepatitis C to seek appropriate treatment and implement preventive measures to protect their liver health and reduce the risk of transmission to others.
Treatment
Effective treatment options are available for hepatitis C, offering the possibility of cure and preventing long-term liver damage. The choice of treatment depends on various factors, including the genotype of the virus, the stage of liver disease, and individual patient characteristics.
Antiviral medications
Antiviral medications are the cornerstone of hepatitis C treatment. They work by targeting and suppressing the replication of the virus, reducing its impact on liver cells. Antiviral therapy aims to achieve sustained virologic response (SVR), indicating that the virus is no longer detectable in the bloodstream.
Direct-acting antivirals (DAAs)
Direct-acting antivirals (DAAs) are a newer class of antiviral medications used to treat hepatitis C. These drugs directly target specific proteins involved in viral replication, leading to high cure rates and fewer side effects compared to older treatment regimens. DAAs are available as oral medications and are typically taken for several weeks or months, depending on the specific regimen.
Treatment duration
The duration of hepatitis C treatment can vary depending on the genotype of the virus, the individual’s overall health, and other factors. Treatment typically ranges from 8 to 12 weeks, although some cases may require longer durations. It is important to strictly adhere to the prescribed treatment regimen for optimal outcomes.
Success rates
With the advent of direct-acting antivirals, hepatitis C treatment success rates have dramatically improved. These medications have shown cure rates exceeding 95%, meaning that the virus is no longer detectable in the bloodstream six months after completing treatment. However, individual responses to treatment may vary, and close monitoring is essential to ensure treatment efficacy.
Cure for Hepatitis C
Achieving sustained virologic response (SVR) through successful antiviral treatment is considered a cure for hepatitis C. SVR means that the virus is no longer detectable in the bloodstream, indicating that the infection has been successfully eradicated. However, it is important to maintain regular medical follow-ups even after achieving SVR to monitor long-term liver health and prevent reinfection.
Liver transplant
In cases of advanced liver disease or liver failure, liver transplantation may be necessary. Liver transplantation involves replacing the diseased liver with a healthy liver from a deceased or living donor. It is a complex procedure and may not be accessible to all individuals due to limited donor organs and other medical considerations. However, for those who meet the criteria, liver transplantation can provide a new lease on life.
In conclusion, understanding hepatitis C is vital for prompt diagnosis, effective treatment, and prevention. Hepatitis C is a global health concern with significant implications for liver health. Recognizing the risk factors, signs and symptoms, and potential complications of hepatitis C can help individuals take proactive steps to protect their liver health. With advancements in antiviral therapy, hepatitis C can be successfully treated and, in many cases, cured, allowing individuals to live healthier lives. However, prevention remains critical, and efforts should focus on implementing comprehensive public health strategies to reduce the incidence and transmission of this potentially life-threatening disease.