In this article, we will explore the symptoms and treatment options for hernias. A hernia occurs when an organ or tissue pushes through a weak spot in the muscles or connective tissues. It can cause discomfort and pain, affecting your daily activities. By understanding the common signs of a hernia and the available treatments, you can equip yourself with knowledge to tackle this condition head-on. So let’s dive into this informative piece and discover how to identify and treat hernias effectively.

Definition of a Hernia
What is a hernia?
A hernia is a medical condition that occurs when an organ or tissue protrudes through a weak spot in the surrounding muscle or connective tissue. It usually appears as a bulge or lump and can cause pain and discomfort. Hernias can develop in various parts of the body, most commonly in the abdomen, groin, or diaphragm. While hernias can occur in people of all ages, they are more commonly found in males and the elderly.
Types of hernias
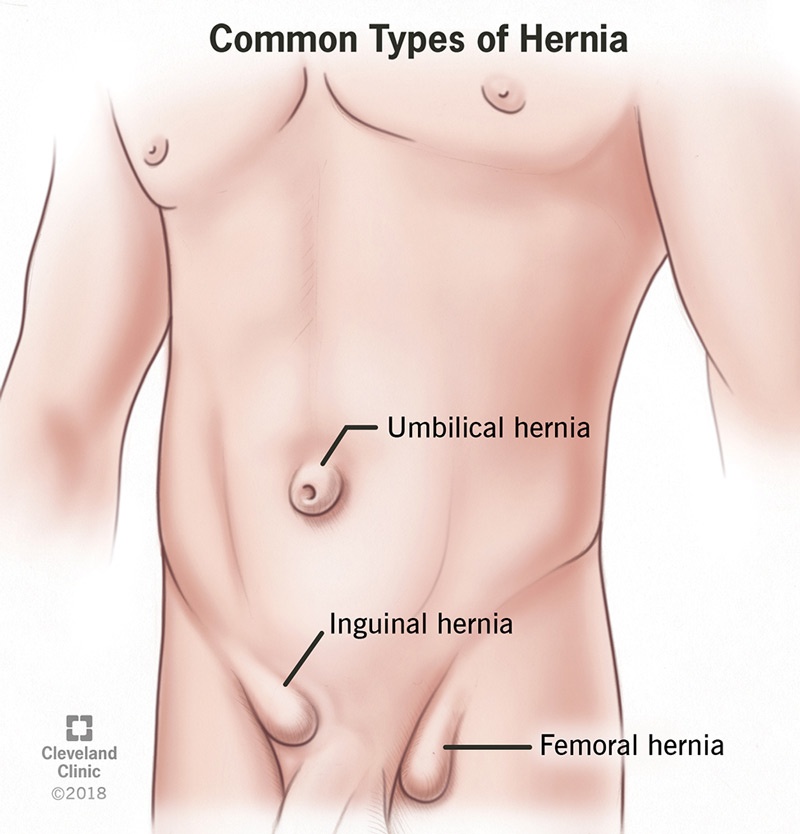
There are several types of hernias that can occur in different areas of the body. The most common types include:
-
Inguinal Hernia: This is the most common type of hernia and occurs when the intestines or bladder protrude through a weak spot in the lower abdominal wall or groin.
-
Umbilical Hernia: This type of hernia occurs when the intestines protrude through a weakened area near the belly button.
-
Hiatal Hernia: This occurs when a portion of the stomach pushes through the diaphragm and into the chest cavity.
-
Incisional Hernia: This type of hernia occurs at the site of a previous abdominal surgery, where the intestines or other organs push through the weakened scar tissue.
-
Femoral Hernia: Less common than inguinal hernias, femoral hernias occur when the intestines push through a weak spot near the groin and upper thigh area.
It’s important to note that hernias may be asymptomatic, meaning they do not cause any noticeable symptoms, or they may cause discomfort and pain. It is essential to seek medical attention for a proper diagnosis and appropriate treatment.
Causes of Hernias
Weakness in the muscle wall
Hernias often occur due to a weakness in the muscle wall or connective tissue. This weakness can be caused by a variety of factors, including:
-
Congenital Weakness: Some people are born with a naturally weak muscle wall, making them more prone to developing hernias.
-
Aging: As we age, our muscles and tissues naturally weaken, increasing the risk of hernias.
-
Chronic Coughing or Sneezing: Frequent bouts of coughing or sneezing can strain the muscles and increase the likelihood of hernias.
-
Obesity: Excess weight and pressure on the abdomen can weaken the muscles and lead to hernias.
Increased pressure in the abdomen
Another common cause of hernias is increased pressure in the abdomen, which can force organs or tissues to protrude through weak spots. Factors that can contribute to increased abdominal pressure include:
-
Lifting heavy objects: Straining while lifting heavy objects can increase the pressure in the abdomen and potentially cause a hernia.
-
Chronic Constipation: Frequent straining during bowel movements can put pressure on the abdominal muscles, leading to hernias.
-
Pregnancy: The growing uterus can put pressure on the abdominal muscles and contribute to the development of hernias.
It’s important to be mindful of these risk factors and take necessary precautions to prevent hernias. Maintaining a healthy weight, avoiding heavy lifting, and practicing proper body mechanics while lifting can help reduce the risk of hernias.
Common Symptoms of Hernias
Visible bulge or lump
One of the most common symptoms of a hernia is the appearance of a visible bulge or lump in the affected area. This bulge may be more prominent when you stand or strain and may disappear when you lie down. The size and appearance of the bulge can vary depending on the type and severity of the hernia. In some cases, the bulge may be painless and reduce on its own, while in others, it may cause discomfort or pain.
Pain or discomfort
Hernias can cause varying degrees of pain or discomfort. The pain can range from mild to severe and may worsen during activities that increase abdominal pressure, such as lifting, coughing, or sneezing. The discomfort may be localized to the hernia site or radiate to surrounding areas. It’s important to note that not all hernias cause pain, and some may be asymptomatic.
Weakness or pressure in the abdomen
People with hernias may experience a general feeling of weakness or pressure in the abdomen, even if there is no visible bulge or lump. This sensation may be present even when not engaged in strenuous activities and can be a sign of a hernia. It’s important to pay attention to these symptoms and seek medical evaluation for a proper diagnosis.
Complications of Hernias
Incarceration
If a hernia becomes incarcerated, it means that the organ or tissue that is protruding becomes trapped and cannot be pushed back into place. This can lead to severe pain and discomfort and requires immediate medical attention. Incarceration can interfere with blood flow to the trapped organ or tissue, leading to more serious complications.
Strangulation
Strangulation is a potentially life-threatening complication of hernias. It occurs when the blood supply to the trapped organ or tissue is completely cut off, leading to tissue death. Strangulated hernias can cause intense pain, fever, and nausea. This is a medical emergency, and immediate surgical intervention is necessary to restore blood flow and prevent further complications.

Diagnosis of Hernias
Physical examination
A thorough physical examination is usually the first step in diagnosing a hernia. Your doctor will carefully examine the affected area and look for any visible bulges or lumps. They may also ask you to cough or strain during the examination to see if the hernia becomes more prominent. In some cases, the hernia may be easily diagnosed through a physical exam. However, additional tests may be required for a more accurate diagnosis.
Imaging tests
In some cases, your doctor may order imaging tests to further evaluate the hernia. Ultrasound, X-ray, or CT scan may be performed to get a detailed view of the area affected by the hernia. These tests can help determine the size, location, and severity of the hernia and guide the appropriate treatment plan.
Specialized tests
In certain instances, specialized tests may be necessary to diagnose and evaluate specific types of hernias, such as hiatal hernias. These tests may include an upper endoscopy or a barium swallow test, which allow for a better visualization of the affected area in the upper digestive tract.
It’s essential to undergo a proper medical evaluation and diagnostic tests to accurately diagnose a hernia and guide the most appropriate treatment plan.
Non-surgical Treatment of Hernias
Watchful waiting
In some cases, if a hernia is small and not causing significant symptoms, your doctor may recommend a watchful waiting approach. This means monitoring the hernia regularly to ensure it does not worsen or cause complications. Lifestyle modifications, such as avoiding heavy lifting and managing underlying conditions like chronic constipation, may be suggested to prevent the hernia from worsening.
Lifestyle changes
Making certain lifestyle changes can be beneficial in managing hernias. Maintaining a healthy weight, eating a high-fiber diet to avoid constipation, and avoiding activities that strain the abdominal muscles, such as heavy lifting, can help prevent the hernia from worsening. Engaging in regular exercise and strengthening the core muscles can also provide added support to the weakened area.
Use of trusses or belts
For some individuals with inguinal hernias, the use of trusses or belts may provide temporary relief and support. These devices are designed to hold the hernia in place and reduce discomfort. However, they are not a permanent solution and should be used under the guidance of a healthcare professional.
It’s important to note that non-surgical treatment methods may only be suitable for certain types and sizes of hernias. Your doctor will guide you in determining the most appropriate treatment option based on your specific condition.

Surgical Treatment of Hernias
Open hernia repair
Open hernia repair is a surgical procedure where an incision is made near the hernia site, and the protruding organ or tissue is pushed back into place. The weakened muscle wall is then reinforced with sutures or a synthetic mesh to prevent future hernias. Open hernia repair is often performed under general anesthesia and may require a hospital stay.
Laparoscopic hernia repair
Laparoscopic hernia repair is a minimally invasive surgical procedure that involves making several small incisions in the abdomen. A laparoscope, a thin tube with a camera, is inserted through one of the incisions to guide the surgeon. Special surgical instruments are used to repair the hernia from within the abdomen. This approach offers a shorter recovery time and less post-operative pain compared to open hernia repair.
Robotic-assisted hernia repair
Robotic-assisted hernia repair is a newer surgical technique that utilizes robotic technology to perform the procedure. The surgeon operates the robotic system, controlling the robotic arms and instruments from a console. This approach provides enhanced precision and visualization during the surgery. Like laparoscopic hernia repair, robotic-assisted surgery offers a shorter recovery time and less post-operative pain compared to open hernia repair.
The choice of surgical technique will depend on various factors, including the type and size of the hernia, your overall health, and the surgeon’s expertise.
Preparing for Hernia Surgery
Medical evaluation
Before undergoing hernia surgery, you will need to undergo a thorough medical evaluation. This may include blood tests, urine tests, and other routine tests to ensure you are in good overall health for the procedure. Your healthcare team will review your medical history, current medications, and any underlying medical conditions to ensure the surgery is safe for you.
Pre-operative instructions
Your surgeon will provide specific pre-operative instructions to follow before your scheduled surgery. This may include guidelines on fasting before the procedure, any necessary medication adjustments, and restrictions on certain activities or medications.
Discussing anesthesia options
During the pre-operative evaluation, you will have the opportunity to discuss anesthesia options with your anesthesiologist. The different options include general anesthesia, which renders you completely unconscious during the surgery, or local/regional anesthesia, which numbs the surgical area while allowing you to remain awake. The choice of anesthesia will depend on your individual circumstances and the surgeon’s recommendation.
It’s important to follow all pre-operative instructions and communicate any concerns or questions you may have with your healthcare team to ensure a smooth surgical experience.

Recovery after Hernia Surgery
Hospital stay
The length of your hospital stay will depend on various factors, including the type and extent of the hernia repair, your overall health, and your surgeon’s recommendations. Open hernia repairs typically require a longer hospital stay compared to laparoscopic or robotic-assisted repairs. Your healthcare team will monitor your recovery and provide appropriate pain management during this time.
Pain management
Pain management is an essential part of the recovery process after hernia surgery. Your healthcare team will provide you with appropriate pain medications to manage any discomfort. It’s important to follow the prescribed medication regimen and communicate any concerns about pain with your healthcare team.
Resuming normal activities
The recovery timeline after hernia surgery can vary from person to person. It’s important to follow your surgeon’s post-operative instructions regarding activity restrictions, wound care, and follow-up visits. While it is essential to rest and avoid strenuous activities during the initial recovery phase, gradually increasing your activity level as tolerated under the guidance of your healthcare team is crucial for a successful recovery.
Prognosis and Follow-up
Hernia recurrence
Hernia recurrence is a possibility, even after successful surgical repair. Factors such as smoking, obesity, chronic coughing, and previous hernia repairs can increase the risk of recurrence. It’s important to follow the lifestyle recommendations provided by your healthcare team and attend regular follow-up visits to monitor for any signs of hernia recurrence.
Regular check-ups
Regular check-ups with your healthcare provider are an essential part of post-operative care. These visits allow your doctor to monitor your recovery progress, assess any complications, and ensure the long-term success of the hernia repair. It’s important to attend all scheduled visits and promptly report any concerning symptoms or issues to your healthcare team.
In conclusion, hernias are a common medical condition that can cause discomfort and pain. Understanding the symptoms, causes, and treatment options for hernias is crucial for timely diagnosis and appropriate management. Seeking medical attention for a thorough evaluation is essential in determining the most suitable treatment approach. Whether non-surgical or surgical, treatment options aim to provide relief, prevent complications, and promote a successful recovery. By following the recommended guidelines and maintaining regular follow-up visits, individuals can effectively manage their hernias and minimize the risk of recurrence.