Breaking Down The Types Of Diabetes Mellitus
Diabetes Mellitus is a term that encompasses a group of metabolic disorders characterized by high blood sugar levels over a prolonged period. If you’ve found yourself navigating the complex world of diabetes, you’re not alone. Understanding the different types of diabetes is essential for effectively managing the condition and improving your quality of life. Each type has its unique characteristics, treatment approaches, and implications for your health, so let’s break down diabetes mellitus into its core types.

What is Diabetes Mellitus?
While it’s essential to dive into the specific types of diabetes, it’s also crucial to grasp what diabetes mellitus means in a broader sense. When you have diabetes, your body either doesn’t produce enough insulin, doesn’t use insulin effectively, or both. Insulin is the hormone responsible for regulating blood sugar levels, allowing your cells to utilize glucose for energy. Without adequate insulin function, glucose remains in your bloodstream, leading to various health complications if left unmanaged.
Living with diabetes requires vigilance and understanding. Lifestyle changes, including diet and exercise, can significantly impact your blood sugar levels. By understanding diabetes mellitus, you empower yourself to make informed choices about your health.
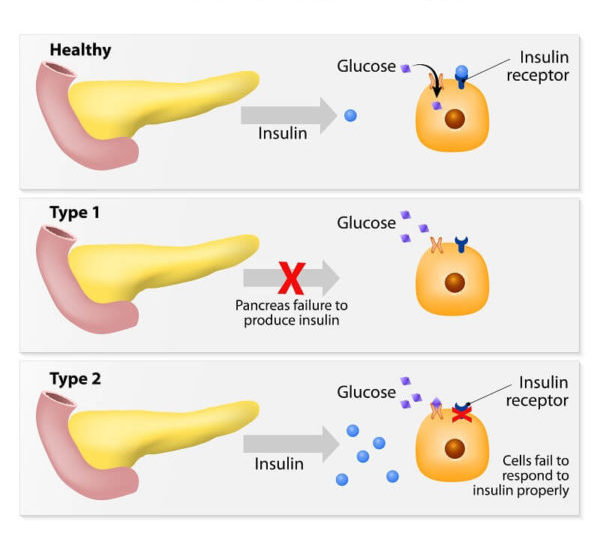
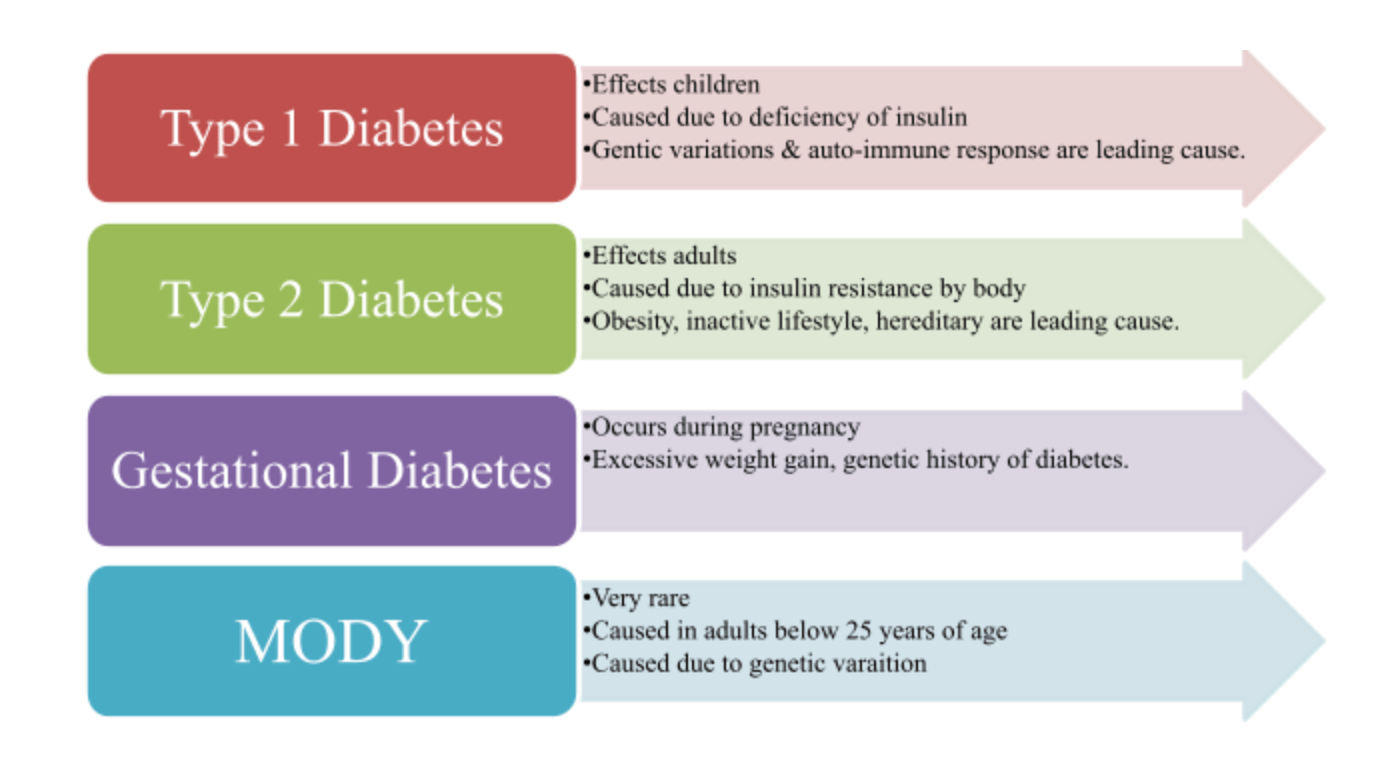
Type 1 Diabetes
Type 1 Diabetes is often referred to as juvenile diabetes or insulin-dependent diabetes. This type arises when your immune system mistakenly attacks the insulin-producing beta cells in your pancreas. The exact cause is still not fully understood, but it is thought to involve a combination of genetic and environmental factors. When your body can no longer produce insulin, your blood sugar levels rise to dangerous heights, necessitating immediate management.
If you or a child you know has been diagnosed with Type 1 Diabetes, take heart; you’re not alone. Managing this type involves regular insulin injections or the use of an insulin pump, alongside careful monitoring of blood sugar levels. It can be incredibly overwhelming, but creating a supportive network of healthcare providers and loved ones can ease the burden. Furthermore, education is key; the more you know about Type 1 diabetes, the more empowered you feel in daily management.
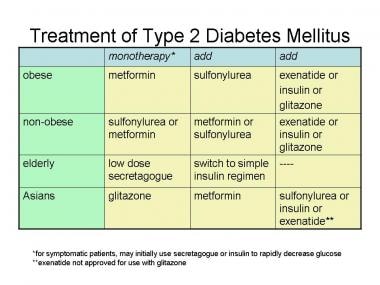
Type 2 Diabetes
Type 2 Diabetes is the most common form of the condition, affecting millions worldwide. Unlike Type 1, where insulin is not produced at all, Type 2 Diabetes results from insulin resistance, where your body doesn’t use insulin effectively. This resistance forces your pancreas to produce more insulin to compensate, putting a strain on your body over time. Eventually, the pancreas may not be able to keep up, leading to higher blood sugar levels.
There are several risk factors associated with developing Type 2 Diabetes, including obesity, sedentary lifestyle, poor diet, and genetic predisposition. If you’ve been diagnosed with Type 2 diabetes, know that lifestyle modifications such as healthier eating, increased physical activity, and weight loss can make a significant difference. In many cases, Type 2 can be managed or even reversed with all these efforts. It’s important to work closely with your healthcare provider to devise a personalized plan that fits your lifestyle.
Gestational Diabetes
Gestational Diabetes is a form of diabetes that occurs during pregnancy. It usually develops around the 24th week and tends to resolve after the delivery of the baby. The body goes through numerous hormonal changes during pregnancy, which can lead to insulin resistance. If your body can’t produce enough insulin to overcome this resistance, you may develop gestational diabetes.
While gestational diabetes can be concerning, you can take proactive steps to manage it. Monitoring blood sugar levels, maintaining a healthy diet, and staying physically active are key strategies. Your healthcare provider will also likely keep a close eye on your pregnancy to ensure both you and your baby remain healthy. Often, women who experience gestational diabetes are at a higher risk of developing Type 2 diabetes later in life, so being vigilant about your health after pregnancy is crucial.
Other Specific Types of Diabetes
Besides the main types, diabetes can also manifest in other forms, which are often grouped under “Other Specific Types.” These can include:
-
Monogenic Diabetes: A rare form of diabetes caused by a change in a single gene. It is distinct from the more common forms of diabetes and often requires specialized treatment.
-
Secondary Diabetes: This type occurs as a result of other medical conditions or treatments, such as chronic pancreatitis or hormonal disorders, that affect insulin production or function.
The nuances of these specific types are essential to understand, as they may require different management strategies. It’s important for you to consult a healthcare professional for a precise diagnosis and individualized treatment plan if you fall under these categories.
How Diabetes Affects Your Daily Life
Living with diabetes doesn’t just impact your health; it intricately weaves into every facet of your life. You might find yourself adjusting your food choices, establishing medication routines, and monitoring your blood sugar levels multiple times a day. All these practices can feel time-consuming and burdensome, and it’s perfectly normal to feel overwhelmed.
However, many people with diabetes learn to integrate management into their daily routines seamlessly. Meal planning, engaging in regular physical activity, and finding enjoyable activities can all help ease the burden. Additionally, connecting with others who share similar experiences can provide emotional support and encouragement. Remember, you’re not alone on this journey; many other individuals navigate similar hurdles daily.
The Importance of Monitoring Blood Sugar Levels
Blood sugar monitoring is one of the cornerstones of diabetes management. If you’re managing Type 1 or Type 2 diabetes, you might be using a glucose meter to check your blood sugar levels regularly. Keeping track of your glucose levels helps you make informed decisions regarding meals, physical activity, and medication. It allows you to recognize patterns and adjust your management strategies accordingly.
Nevertheless, it’s essential to remember that numbers don’t tell the whole story. Sometimes, you might feel great even if your numbers aren’t ideal or might feel unwell despite seemingly normal readings. Striking a balance between data-driven decisions and intuition about your well-being is key. Over time, you’ll develop a better understanding of how your body responds to different foods, activities, and medications.
Nutrition and Diabetes Management
Nutrition plays a vital role in managing diabetes effectively. A well-balanced, nutrient-dense diet can help control your blood sugar levels while also providing the necessary energy and nutrients for your body. If you’re newly diagnosed, you might feel daunted by dietary restrictions, but with the right guidance, you can find delicious and satisfying meals that fit your needs.
Understanding carbohydrates, especially their types and how they affect your blood sugar, is essential. Choosing complex carbohydrates, such as whole grains, vegetables, and legumes, over simple carbohydrates can help prevent blood sugar spikes. Furthermore, incorporating lean proteins and healthy fats can contribute positively to your overall health. Collaborating with a registered dietitian can help you find a nutrition plan that works for your lifestyle and preferences.
Physical Activity and Diabetes Management
Regular physical activity is another crucial element of diabetes management. Exercise helps improve your body’s insulin sensitivity, which means your cells can use glucose more effectively. Whether it’s a brisk walk, a dance class, or a structured workout, finding an activity you enjoy makes it easier to stick with it.
Setting realistic fitness goals is vital, especially if you’re starting from a sedentary lifestyle. Begin with activities that fit into your routine, aiming for at least 150 minutes of moderate-intensity aerobic exercise each week, as recommended by health experts. Remember to consult your healthcare provider before starting any new exercise routine, particularly if you have other health concerns.
Emotional Well-Being and Diabetes
Managing diabetes can take a toll on your emotional health. The daily reality of living with diabetes often comes with stress and anxiety, and it’s crucial to acknowledge these feelings. You might feel overwhelmed by the demands of self-management, lifestyle changes, or the fear of complications.
Seeking support from healthcare professionals, support groups, or therapy can be immensely beneficial. You’re not alone; many individuals face similar emotional challenges. Engaging in stress-reducing activities such as mindfulness, meditation, or hobbies can provide positive outlets for your feelings and improve your overall well-being.

Advances in Diabetes Technology
Thanks to advancements in technology, life with diabetes is becoming more manageable. Continuous Glucose Monitors (CGMs) and insulin pumps have revolutionized diabetes management, allowing you to track your blood sugar levels continuously and administer insulin more effectively. These technologies can provide real-time data, giving you the power to make more informed decisions throughout your day.
Additionally, various mobile applications can support your diabetes journey, enabling you to log your meals, monitor your physical activity, and track your blood sugar levels easily. As technology continues to evolve, keeping yourself informed about new options can empower you to take charge of your health in exciting ways.
Collaborating with Your Healthcare Team
Working closely with your healthcare team is vital for effective diabetes management. This team can include doctors, nurses, dietitians, and diabetes educators who can provide tailored advice and support. Regular appointments will allow you to discuss changes in your health, review your blood sugar levels, and adjust treatment plans as necessary.
Don’t hesitate to ask questions and voice concerns during your appointments; you are your best advocate. A collaborative approach will help ensure you’re well-equipped to manage your diabetes, leading to better outcomes and a more satisfying life.
Conclusion
Navigating life with diabetes mellitus may seem challenging at times, but understanding the different types of diabetes empowers you to be an active participant in your health journey. Whether it’s making dietary changes, increasing physical activity, or utilizing technology, countless strategies can help you manage your condition effectively.
The key is to stay informed, remain proactive, and never hesitate to seek support when needed. By doing so, you cultivate a lifestyle that not only manages your diabetes but allows you to thrive despite it.
If you found this article helpful, please clap, leave a comment, and subscribe to my Medium newsletter for more updates. Let’s navigate this journey together!