In this article, you will learn about common types of blood disorders that can affect your health. Understanding these conditions is crucial as they can impact your overall well-being. From anemia to leukemia, the various disorders discussed here shed light on their causes, symptoms, and available treatments. Whether you want to educate yourself or seek support for a loved one, this comprehensive guide will provide valuable insights into the different blood disorders that may affect you. So, read on to broaden your knowledge and be better equipped to navigate the world of blood disorders.

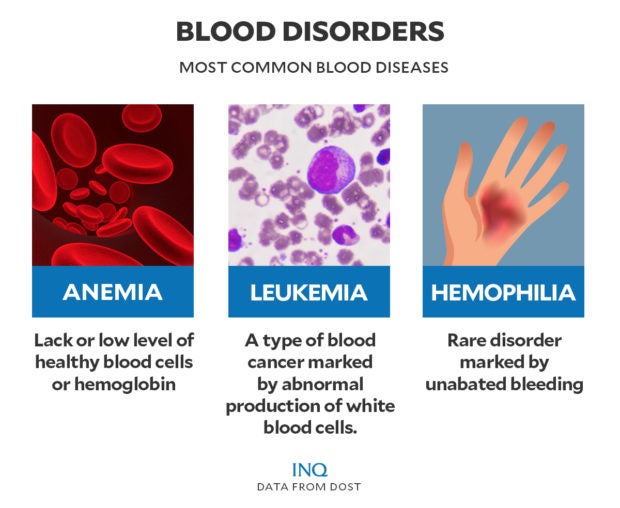
Anemia
Anemia is a common blood disorder that occurs when the body doesn’t have enough healthy red blood cells to carry oxygen to the tissues and organs. This can lead to fatigue, weakness, and a variety of other symptoms. There are several different types of anemia, each with its own causes and treatments. In this article, we will explore the different types of anemia and provide an overview of each.
Iron-deficiency anemia
Iron-deficiency anemia is the most common type of anemia and occurs when the body doesn’t have enough iron to produce adequate amounts of hemoglobin, the protein that carries oxygen in the blood. This can be caused by a lack of dietary iron, poor absorption of iron by the body, or chronic blood loss. Symptoms of iron-deficiency anemia can include fatigue, weakness, pale skin, shortness of breath, and difficulty concentrating. Treatment usually involves iron supplements and dietary changes to increase iron intake.
Vitamin-deficiency anemia
Vitamin-deficiency anemia occurs when the body doesn’t have enough of certain vitamins, such as vitamin B12 or folate, to produce healthy red blood cells. This can be caused by a poor diet that doesn’t provide enough of these vitamins, malabsorption of vitamins due to certain medical conditions, or an increased need for vitamins during pregnancy or breastfeeding. Symptoms of vitamin-deficiency anemia can include fatigue, weakness, shortness of breath, and swollen tongue. Treatment usually involves vitamin supplements and dietary changes.
Hemolytic anemia
Hemolytic anemia is a type of anemia that occurs when the red blood cells are destroyed faster than the body can replace them. This can be caused by inherited conditions, such as sickle cell disease or thalassemia, or by certain medications, infections, or autoimmune disorders. Symptoms of hemolytic anemia can vary depending on the underlying cause but may include fatigue, jaundice, pale skin, and an enlarged spleen. Treatment usually involves addressing the underlying cause and, in some cases, medication or blood transfusions.
Sickle cell anemia
Sickle cell anemia is an inherited form of hemolytic anemia that affects the shape of red blood cells. Instead of being round and flexible, the red blood cells are crescent-shaped and prone to getting stuck in blood vessels, leading to a reduced oxygen supply to the tissues and organs. Common symptoms of sickle cell anemia include pain, fatigue, infections, delayed growth, vision problems, and jaundice. Treatment often involves managing symptoms and complications, such as pain medications, blood transfusions, and hydroxyurea.
Aplastic anemia
Aplastic anemia is a rare and serious type of anemia that occurs when the bone marrow doesn’t produce enough red blood cells, white blood cells, and platelets. This can be caused by radiation or chemotherapy, certain medications, infections, autoimmune disorders, or inherited conditions. Symptoms of aplastic anemia can include fatigue, shortness of breath, increased susceptibility to infections, and easy bruising or bleeding. Treatment often involves blood transfusions, medications to stimulate the production of blood cells, and, in some cases, stem cell transplantation.
Thalassemia
Thalassemia is a genetic blood disorder that affects the production of hemoglobin. It results in the body producing abnormal forms of hemoglobin, leading to a reduced ability to carry oxygen. There are two main types of thalassemia: alpha thalassemia and beta thalassemia. Symptoms of thalassemia can vary from mild to severe and may include fatigue, weakness, pale skin, delayed growth and development, and abnormal bone structure. Treatment options for thalassemia may include blood transfusions, medications, and, in severe cases, stem cell transplantation.
Hemophilia
Hemophilia is a rare inherited bleeding disorder that impairs the body’s ability to form blood clots, leading to prolonged and excessive bleeding. It is caused by a deficiency or dysfunction of specific clotting factors in the blood. Hemophilia primarily affects males, although females can be carriers of the gene. There are three main types of hemophilia: Hemophilia A, Hemophilia B, and Hemophilia C.
Hemophilia A
Hemophilia A is the most common type of hemophilia and is caused by a deficiency of clotting factor VIII. The severity of Hemophilia A can vary depending on the level of factor VIII in the blood. Symptoms of Hemophilia A include easy bruising, prolonged bleeding, joint pain and swelling, and, in severe cases, spontaneous bleeding. Treatment often involves replacing the missing clotting factor through regular infusions.
Hemophilia B
Hemophilia B, also known as Christmas disease, is caused by a deficiency of clotting factor IX. It is less common than Hemophilia A but shares similar symptoms and treatment options. The severity of Hemophilia B can also vary, with individuals experiencing varying degrees of bleeding and joint problems.
Hemophilia C
Hemophilia C is the least common type of hemophilia and is caused by a deficiency of clotting factor XI. It is typically less severe than Hemophilia A and Hemophilia B and often goes undiagnosed until a significant bleeding event occurs. Symptoms of Hemophilia C can include easy bruising, prolonged bleeding after injuries or surgeries, and nosebleeds.

Leukemia
Leukemia is a type of cancer that affects the blood and bone marrow, leading to the overproduction of abnormal white blood cells. It can be acute or chronic and is classified based on the specific type of white blood cell affected and the rate of disease progression.
Acute lymphocytic leukemia (ALL)
Acute lymphocytic leukemia, also known as acute lymphoblastic leukemia, is a cancer of the lymphocytes, a type of white blood cell. It primarily affects children but can also occur in adults. Symptoms of ALL may include fatigue, fever, frequent infections, easy bruising or bleeding, swollen lymph nodes, and bone or joint pain. Treatment often involves chemotherapy, radiation therapy, and stem cell transplantation.
Acute myeloid leukemia (AML)
Acute myeloid leukemia is a cancer of the myeloid cells, another type of white blood cell. It can occur at any age but is most common in older adults. Symptoms of AML may include fatigue, frequent infections, easy bruising or bleeding, shortness of breath, and bone pain. Treatment often involves chemotherapy, targeted therapy, and stem cell transplantation.
Chronic lymphocytic leukemia (CLL)
Chronic lymphocytic leukemia is a cancer of the lymphocytes that typically progresses slowly and is most common in older adults. Many people with CLL show no symptoms in the early stages of the disease, and it is often diagnosed through routine blood tests. Symptoms of CLL may include swollen lymph nodes, fatigue, weight loss, night sweats, and frequent infections. Treatment options for CLL may include watchful waiting, chemotherapy, targeted therapy, and stem cell transplantation.
Chronic myeloid leukemia (CML)
Chronic myeloid leukemia is a cancer of the myeloid cells that typically progresses slowly in the initial chronic phase but can accelerate to a more aggressive phase called the blast crisis. It primarily affects adults and is rarely seen in children. Symptoms of CML may include fatigue, rapid weight loss, night sweats, fever, and abdominal pain. Treatment often involves targeted therapy, such as tyrosine kinase inhibitors, and stem cell transplantation.
Hairy cell leukemia
Hairy cell leukemia is a rare type of chronic leukemia that affects B cells, a type of white blood cell. It gets its name from the appearance of the abnormal cells under a microscope, which have fine hair-like projections on their surface. Symptoms of hairy cell leukemia may include fatigue, enlarged spleen, frequent infections, easy bruising or bleeding, and a weak immune system. Treatment options for hairy cell leukemia may include chemotherapy, targeted therapy, and splenectomy.
Thrombocytopenia
Thrombocytopenia is a condition characterized by a low platelet count in the blood, which can increase the risk of bleeding and result in prolonged bleeding after injuries or surgeries. There are different types of thrombocytopenia, each with its own causes and treatment approaches.
Immune thrombocytopenia (ITP)
Immune thrombocytopenia, also known as idiopathic thrombocytopenic purpura, occurs when the body’s immune system mistakenly attacks and destroys its own platelets. This can lead to a low platelet count and an increased risk of bleeding. Symptoms of ITP may include easy bruising, petechiae (small purple or red spots on the skin), nosebleeds, and prolonged bleeding. Treatment options for ITP may include medications to suppress the immune system, platelet transfusions, and surgery in rare cases.
Drug-induced thrombocytopenia
Drug-induced thrombocytopenia is a condition in which certain medications can cause a decrease in platelet count. This can result from an immune reaction to the medication or from direct toxicity to the bone marrow, where platelets are produced. Symptoms can range from mild to severe, depending on the extent of platelet reduction. Treatment involves discontinuation of the offending medication and supportive care.
Thrombotic thrombocytopenic purpura (TTP)
Thrombotic thrombocytopenic purpura is a rare blood disorder characterized by the formation of blood clots within small blood vessels throughout the body. This can lead to a decrease in platelet count and damage to organs and tissues. Symptoms of TTP may include purpura (red or purple discolorations on the skin), fever, headache, confusion, and kidney or heart problems. Treatment typically involves plasma exchange therapy to remove antibodies and replenish normal plasma components.
Hemochromatosis
Hemochromatosis is a genetic disorder that results in excessive absorption and accumulation of iron in the body. Over time, this excess iron can damage various organs, including the liver, heart, and pancreas. There are two main types of hemochromatosis.
Primary hemochromatosis
Primary hemochromatosis, also known as hereditary hemochromatosis, is caused by a mutation in the HFE gene, which regulates iron absorption in the body. It is usually inherited in an autosomal recessive pattern. Symptoms of primary hemochromatosis may include fatigue, joint pain, weight loss, and abdominal pain. Treatment often involves regular phlebotomy (blood removal) to lower iron levels and prevent organ damage.
Secondary hemochromatosis
Secondary hemochromatosis occurs as a result of another underlying condition or factor, such as chronic alcoholism, certain blood disorders, or repeated blood transfusions. The excessive iron accumulation in secondary hemochromatosis can have similar consequences as primary hemochromatosis, and treatment often involves addressing the underlying cause and managing iron levels through phlebotomy or iron-chelation therapy.
Von Willebrand Disease
Von Willebrand Disease is an inherited bleeding disorder caused by a deficiency or dysfunction of von Willebrand factor, a protein that plays a crucial role in blood clotting. There are three main types of Von Willebrand Disease.
Type 1 Von Willebrand Disease
Type 1 Von Willebrand Disease is the mildest and most common form of the disorder. It is characterized by reduced levels of von Willebrand factor in the blood. Symptoms of Type 1 Von Willebrand Disease can include easy bruising, nosebleeds, and heavy or prolonged menstrual periods in women. Treatment may involve desmopressin (a medication that stimulates the release of von Willebrand factor) or von Willebrand factor replacement therapy.
Type 2 Von Willebrand Disease
Type 2 Von Willebrand Disease is characterized by normal or reduced levels of von Willebrand factor, but with functional defects that impair clotting. There are several subtypes of Type 2 Von Willebrand Disease, each with its own specific characteristics and treatment approaches. Symptoms can range from mild to severe and may include spontaneous bleeding, mucocutaneous bleeding, and bleeding after surgeries or injuries.
Type 3 Von Willebrand Disease
Type 3 Von Willebrand Disease is the most severe form of the disorder and is characterized by the complete absence of von Willebrand factor in the blood. Symptoms of Type 3 Von Willebrand Disease can include severe and spontaneous bleeding, joint bleeds, and life-threatening hemorrhages. Treatment often involves regular infusions of von Willebrand factor concentrate and careful monitoring to prevent and manage bleeding episodes.
Polycythemia Vera
Polycythemia Vera is a rare blood disorder that results in the overproduction of red blood cells by the bone marrow. This excessive production can lead to thickening of the blood and increased risk of blood clots. There are two main types of polycythemia vera.
Primary polycythemia vera
Primary polycythemia vera is the most common form of the disorder and occurs due to a mutation in the JAK2 gene, which controls the production of red blood cells. Symptoms of primary polycythemia vera can include fatigue, headache, itching, shortness of breath, and an increased risk of blood clots. Treatment often involves phlebotomy to lower red blood cell count and medications to manage symptoms and reduce the risk of complications.
Secondary polycythemia
Secondary polycythemia, also known as acquired polycythemia, occurs as a result of another underlying condition or factor that stimulates the production of red blood cells. This can include chronic lung diseases, such as chronic obstructive pulmonary disease (COPD), certain tumors, and high altitude. Treatment involves addressing the underlying cause and managing symptoms, which may include phlebotomy or medication.
Idiopathic thrombocytopenic purpura (ITP)
Idiopathic thrombocytopenic purpura (ITP) is a bleeding disorder characterized by a low platelet count in the blood. It is an autoimmune condition in which the immune system mistakenly attacks and destroys platelets. ITP can be divided into two main subtypes: acute ITP and chronic ITP.
Acute ITP
Acute ITP typically occurs in children after a viral infection and is a self-limiting condition that tends to resolve on its own within a few weeks or months. It is characterized by a sudden onset of low platelet count and symptoms of bleeding, such as petechiae, easy bruising, and nosebleeds. Treatment for acute ITP may involve close monitoring and, in severe cases, medication or platelet transfusions.
Chronic ITP
Chronic ITP is a long-term condition that persists for more than six months and is more commonly seen in adults. It is characterized by a persistent low platelet count and an increased risk of bleeding. Symptoms of chronic ITP can include easy bruising, prolonged bleeding after injuries or surgeries, and heavy menstrual periods in women. Treatment options for chronic ITP may include medications to suppress the immune system, platelet transfusions, and splenectomy in some cases.
Malaria
Malaria is a serious and potentially life-threatening tropical disease caused by parasitic infection transmitted through the bite of infected mosquitoes. There are several species of the Plasmodium parasite that cause malaria, each with its own unique characteristics and geographic distribution.
Plasmodium falciparum malaria
Plasmodium falciparum is the most deadly species of the malaria parasite and is responsible for the majority of malaria-related deaths globally. It can cause severe symptoms, such as high fever, chills, headache, and organ damage. Treatment of Plasmodium falciparum malaria usually involves a combination of antimalarial medications, with prompt diagnosis and medical intervention critical for a successful outcome.
Plasmodium vivax malaria
Plasmodium vivax is the most common species of the malaria parasite found outside of Africa. It can cause relapsing malaria, in which the parasite remains dormant in the liver and reactivates periodically, leading to recurrent bouts of illness. Symptoms of Plasmodium vivax malaria are similar to other types of malaria and may include fever, chills, headache, and body aches. Treatment typically involves antimalarial medications to eliminate the parasite from the body.
Plasmodium malariae malaria
Plasmodium malariae is a less common species of the malaria parasite but can cause chronic infection that persists for many years if left untreated. Symptoms of Plasmodium malariae malaria are generally milder and may include fever, headache, and fatigue. Treatment involves antimalarial medications to clear the parasite from the body and prevent complications.
Plasmodium ovale malaria
Plasmodium ovale is a rare species of the malaria parasite but shares similarities with Plasmodium vivax in terms of its ability to cause relapsing malaria. Symptoms of Plasmodium ovale malaria are similar to other types of malaria and may include fever, chills, headache, and muscle pain. Treatment involves antimalarial medications to eliminate the parasite from the body.
Sepsis
Sepsis is a serious and potentially life-threatening condition that occurs in response to an infection. It can lead to widespread inflammation throughout the body and organ dysfunction. Disseminated intravascular coagulation (DIC) is a complication of sepsis that affects blood clotting and can result in excessive bleeding or abnormal blood clots.
Understanding these common types of blood disorders is crucial for recognizing their symptoms, diagnosing them accurately, and providing appropriate treatment. If you suspect you may be experiencing any signs or symptoms related to these conditions, it is important to consult with a healthcare professional for a proper evaluation and management plan. With early diagnosis and effective treatment, many individuals with blood disorders can lead healthy and fulfilling lives.