Are you familiar with the potential risks and complications that can arise from acute cholecystitis? In this article, we will explore the various problematic outcomes that can occur as a result of this condition and how recognizing and addressing them in a timely manner is crucial for effective treatment. From gallbladder perforation to bile duct obstruction, understanding these complications is essential for healthcare professionals and patients alike. So, let’s dive into the world of acute cholecystitis and uncover the challenges that may arise along the way.

Complications of Acute Cholecystitis
Acute cholecystitis is a condition characterized by inflammation of the gallbladder, typically caused by the presence of gallstones. While it can be a painful and bothersome condition on its own, there are also several potential complications that may arise as a result. Understanding these complications is crucial in order to recognize their signs and symptoms, and to take appropriate action to address them.
Understanding Acute Cholecystitis
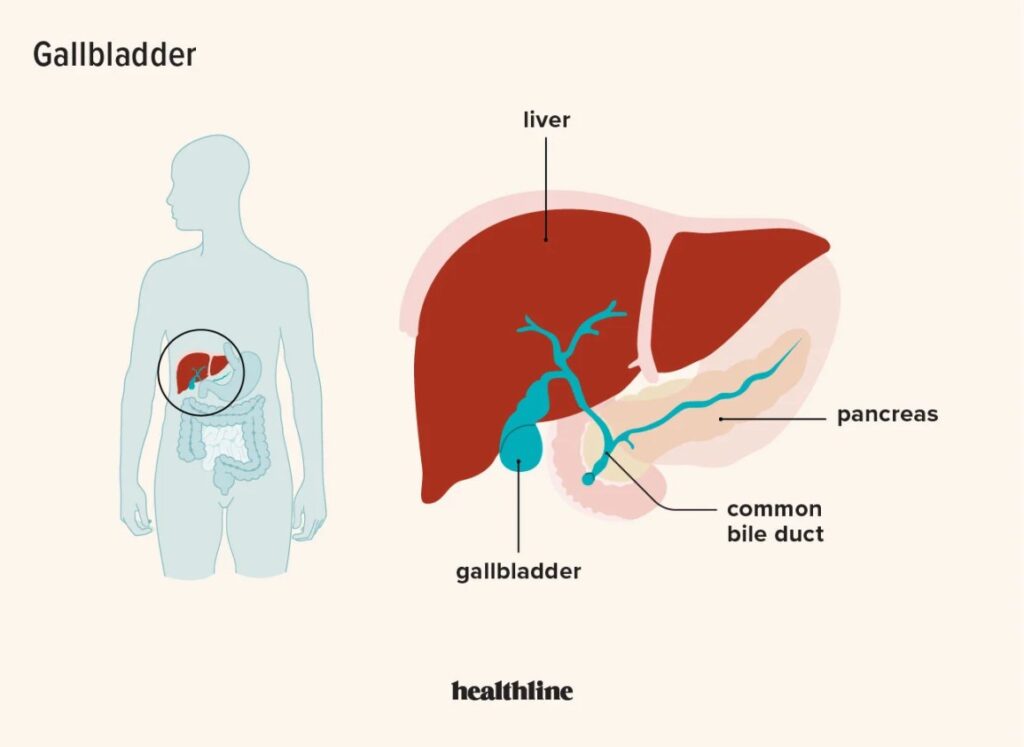
Before delving into the complications, it is important to have a clear understanding of acute cholecystitis itself. Acute cholecystitis refers to the sudden inflammation of the gallbladder, which is a small organ located beneath the liver. The gallbladder plays a crucial role in the digestion of fat by storing and concentrating bile produced by the liver. When the flow of bile is blocked, usually by gallstones, the gallbladder becomes inflamed, leading to acute cholecystitis.
Prevalence and Risk Factors
Acute cholecystitis is a fairly common condition, affecting millions of people worldwide each year. Certain factors increase the risk of developing this condition. Age and gender play a role, as women and individuals over the age of 40 are more likely to experience acute cholecystitis. Additionally, obesity and a sedentary lifestyle have been associated with an increased risk, as excess weight and inactivity can contribute to the formation of gallstones.
Dietary habits can also influence the development of acute cholecystitis. A high-fat diet, for example, can increase the risk by promoting the production of cholesterol, a key component of gallstones. Other risk factors include a family history of gallstones, certain medical conditions such as diabetes, and the use of medications that reduce the flow of bile.
Identification and Diagnosis
To properly address the complications of acute cholecystitis, it is necessary to accurately identify and diagnose the condition. Clinical assessment is an important component of this process, as it involves evaluating a patient’s medical history, symptoms, and physical examination findings. Laboratory tests, such as blood tests and liver function tests, can provide valuable information pertaining to the function and health of the gallbladder.
Imaging techniques, such as ultrasound and computed tomography (CT) scans, are commonly used to aid in diagnosis by visualizing the gallbladder and detecting any abnormalities. These imaging modalities can help identify the presence of gallstones, inflammation, and other potential complications.
However, diagnosing acute cholecystitis can sometimes present challenges. The symptoms can be similar to other conditions, such as peptic ulcer disease or pancreatitis, making it important to differentiate between them. In some cases, a diagnosis may require further investigation or the use of additional diagnostic tools, such as a hepatobiliary iminodiacetic acid (HIDA) scan or magnetic resonance cholangiopancreatography (MRCP).
Complications Overview
While acute cholecystitis itself can be uncomfortable and painful, there are several complications that may arise if the condition is left untreated or if it becomes more severe. These complications can range from mild to life-threatening, and understanding their manifestations is crucial for prompt recognition and appropriate management.
One complication of acute cholecystitis is gangrenous cholecystitis, which refers to the death of the gallbladder tissue. This occurs when the inflammation and blockage of blood flow become severe, leading to tissue necrosis. Another potential complication is the development of an empyema, which refers to the collection of pus within the gallbladder. This can occur when the inflammation progresses and results in the accumulation of infected fluid.
Gallbladder perforation is another complication that can occur, wherein the gallbladder wall becomes so inflamed and distended that it ruptures. This can lead to the leakage of bile into the abdominal cavity, causing severe pain and potentially leading to infection and peritonitis. Biliary fistula, which is an abnormal connection between the gallbladder and another organ, can also develop as a complication of acute cholecystitis.
Other potential complications include gallstone ileus, where a gallstone becomes lodged in the small intestine and causes a blockage, as well as Mirizzi syndrome, which involves the obstruction of the common bile duct due to external compression. Abscess formation, sepsis, jaundice, and even acute pancreatitis can also occur as complications of acute cholecystitis.
Understanding the symptoms and manifestations of these complications is crucial in order to provide appropriate care and prevent further complications from arising. Prompt diagnosis and treatment are essential to address these complications effectively and minimize the potential risk to the patient.
Gangrenous Cholecystitis
Definition and Etiology
Gangrenous cholecystitis is a severe complication of acute cholecystitis, characterized by the death of the gallbladder tissue due to severe inflammation and compromised blood supply. It occurs when the inflammation becomes so severe that it leads to tissue necrosis. This can be caused by various factors, with the most common being the presence of gallstones that obstruct the cystic duct, leading to the accumulation of bile and subsequent irritation and inflammation.
In some cases, gangrenous cholecystitis can also be caused by ischemia, which refers to a lack of blood flow to the gallbladder. This can occur when the blood vessels supplying the gallbladder become blocked or constricted, reducing the oxygen and nutrient supply to the tissue.
Clinical Features
Gangrenous cholecystitis presents with several distinct clinical features that differentiate it from uncomplicated acute cholecystitis. Patients may experience more severe abdominal pain that is constant and localized to the right upper quadrant. The pain may be accompanied by a fever, increased heart rate, and general malaise.
Physical examination findings may also reveal tenderness and guarding upon palpation of the abdomen, as well as signs of inflammation, such as redness or swelling. In severe cases, there may be evidence of peritonitis, which is the inflammation of the membrane lining the abdominal cavity.
Management and Treatment
The management and treatment of gangrenous cholecystitis focus on eliminating the source of infection and addressing the necrotic tissue. In many cases, surgical intervention is necessary to remove the gallbladder entirely. This procedure, called cholecystectomy, can be performed as an open surgery or as a minimally invasive laparoscopic procedure.
During the surgery, the necrotic tissue and any associated pus or fluid may be drained, and the affected area is thoroughly cleaned to prevent the spread of infection. Antibiotics are also commonly administered to combat infection and prevent further complications.
Recovery from gangrenous cholecystitis typically involves a hospital stay and a period of post-operative care. Pain management, infection control, and monitoring for complications are important aspects of the recovery process. With timely and appropriate intervention, the prognosis for patients with gangrenous cholecystitis can be favorable, although the condition can be life-threatening if left untreated.
Overall, gangrenous cholecystitis serves as a reminder of the importance of recognizing and addressing the complications of acute cholecystitis. By understanding the etiology, clinical features, and appropriate management of this severe complication, healthcare providers can ensure that patients receive the necessary care and treatment to improve their outcomes.

Watch This Video Below
Related Terms About Complications of Acute Cholecystitis
A Complication Of Acute Cholecystitis, Complications Of Acute Calculous Cholecystitis, Complications Of Acute Cholecystitis, Complications Of Acute Cholecystitis Pdf, Complications Of Acute Cholecystitis Radiology, Complications Of Laparoscopic Cholecystectomy For Acute Cholecystitis, Does This Patient Have Acute Cholecystitis, Most Common Complication Of Acute Cholecystitis, Most Common Complication Of Cholecystitis, What Are The Complications Of Acute Cholecystitis