In this article, we will explore essential nursing considerations for managing pressure ulcers. From understanding the causes and stages of pressure ulcers to implementing effective prevention strategies and treatments, we will cover all the important aspects of nursing management in this specialized area. Whether you are a new nurse looking to expand your knowledge or a seasoned professional seeking a refresher, this article will provide you with valuable insights and practical tips to enhance your care for patients with pressure ulcers. So, let’s dive right in and explore the world of pressure ulcer management together!
Assessment of Pressure Ulcers
Pressure ulcers, also known as bedsores or pressure sores, can cause significant pain and discomfort for individuals who are immobile or spend long periods in one position. Proper assessment of pressure ulcers is essential in order to develop appropriate treatment and prevention strategies.
Risk assessment
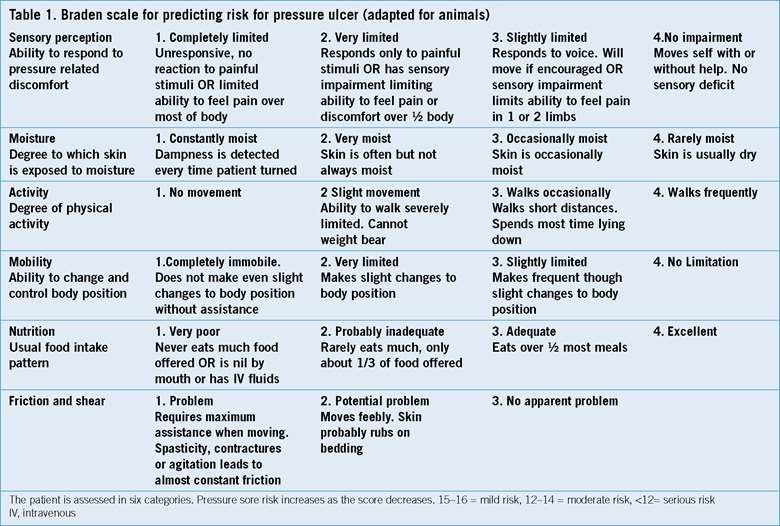
The first step in pressure ulcer assessment is identifying individuals who are at risk of developing pressure ulcers. Factors such as immobility, advanced age, poor nutrition, and incontinence can increase the risk. Regular risk assessments should be conducted to determine the level of risk for each individual. This assessment may include the use of tools such as the Braden Scale or Norton Scale, which evaluate various factors such as skin moisture, mobility, and sensory perception.
Clinical assessment
Once a risk assessment has been completed and identified individuals at risk, a thorough clinical assessment of the skin is necessary. This involves inspecting the skin for any signs of damage, discoloration, or changes in texture. The assessment should also include palpation of the affected area to check for pain, warmth, or swelling. Documentation of the assessment findings is essential for monitoring changes over time and for determining appropriate treatment interventions.
Staging of pressure ulcers
Pressure ulcers are classified into stages based on their severity. The stages range from stage I, which is the least severe, to stage IV, which is the most severe. Each stage has specific characteristics and treatment considerations. Staging is important in order to determine the appropriate course of action and to track the progress of the ulcer. It is important to note that pressure ulcers can worsen over time if not properly managed, making accurate staging crucial for effective treatment.
Prevention Strategies
Prevention is key in managing pressure ulcers, as they can be difficult to heal once they have developed. Implementing preventive measures is essential in reducing the incidence of pressure ulcers.
Skin inspection and monitoring
Regular skin inspection and monitoring are crucial in preventing pressure ulcers. Careful examination of the skin should be conducted, paying special attention to areas that are prone to pressure ulcers, such as the heels, sacrum, and hips. Any changes in the skin, such as redness, discoloration, or breaks in the skin, should be promptly addressed. It is important to ensure that the skin remains clean, dry, and moisturized, as excessive moisture can increase the risk of skin breakdown.
Patient repositioning
Repositioning patients regularly is an effective strategy for preventing pressure ulcers. This involves changing the patient’s position at least every two hours to relieve pressure on vulnerable areas. The use of assistive devices, such as pillows, foam wedges, or specialized seating cushions, can help redistribute pressure and reduce the risk of developing pressure ulcers.
Use of pressure redistribution surfaces
Another preventive strategy is the use of pressure redistribution surfaces, which are specifically designed to distribute weight and reduce pressure on vulnerable areas. These surfaces include specialized mattresses, overlays, and cushions that help relieve pressure and promote better blood flow. The selection of the appropriate pressure redistribution surface should be based on the individual’s risk assessment and clinical assessment findings.

Wound Care and Dressing Selection
Once a pressure ulcer has developed, proper wound care and dressing selection are essential for promoting healing and preventing further complications.
Wound cleansing
The first step in wound care is cleansing the wound. This involves using a gentle cleanser or saline solution to remove any debris or bacteria from the wound. It is important to avoid using harsh or irritating substances, as they can further damage the delicate tissue. Careful attention should be given to ensuring aseptic technique during wound cleansing to minimize the risk of infection.
Choosing appropriate dressings
The selection of appropriate dressings is crucial in facilitating wound healing. The choice of dressing depends on various factors, including the stage and characteristics of the pressure ulcer, the amount of exudate present, and the individual’s overall health status. Dressings can range from simple non-adherent dressings for shallow, non-infected wounds to specialized dressings such as hydrocolloids or foams for deeper or infected wounds.
Debridement techniques
Debridement, the removal of dead or necrotic tissue from the wound, may be necessary in some cases to promote healing. There are several techniques for debridement, including surgical debridement, enzymatic debridement, mechanical debridement, and autolytic debridement. The choice of debridement technique depends on the characteristics of the wound and the individual’s overall health status. Proper assessment and consultation with wound care specialists are essential in determining the appropriate debridement approach.
Nutritional Considerations
Nutrition plays a crucial role in pressure ulcer management, as proper nutrition promotes tissue repair and wound healing.
Assessing nutritional status
Assessing the individual’s nutritional status is an important step in managing pressure ulcers. Malnutrition can significantly impair the healing process, making it essential to identify any nutritional deficiencies. This assessment may include evaluating the individual’s body mass index (BMI), assessing dietary intake, and considering laboratory values such as albumin and pre-albumin levels.
Providing adequate protein and calorie intake
Protein and calorie intake are important factors in promoting wound healing. Adequate protein intake is vital for tissue repair and the formation of new skin. Calorie intake should be sufficient to meet the individual’s energy needs, especially during times of increased metabolic demands. Nutritional support, such as oral supplementation or enteral feeding, may be necessary to ensure that the individual receives adequate nutrition for wound healing.
Fluid management
Proper fluid management is essential for maintaining adequate hydration and supporting wound healing. Dehydration can impair tissue repair and increase the risk of pressure ulcers. It is important to monitor the individual’s fluid intake and output and ensure that they are well-hydrated. Collaboration with a registered dietitian or nutritionist can help formulate a proper fluid management plan based on the individual’s specific needs.
Pain Management
Pain management is an important aspect of pressure ulcer care, as pressure ulcers can be extremely painful and can significantly affect an individual’s quality of life.
Assessing and documenting pain
Assessing and documenting pain is essential in order to provide appropriate pain management interventions. Pain assessments should include asking the individual about their pain levels, using pain scales, and observing their behavior for signs of discomfort. It is important to document pain assessments accurately and regularly to monitor changes in pain levels over time.
Choosing appropriate analgesics
The choice of analgesics for pain management depends on the individual’s pain severity and response to previous interventions. Non-opioid analgesics, such as nonsteroidal anti-inflammatory drugs (NSAIDs) or acetaminophen, may be sufficient for mild to moderate pain. For severe pain, opioid analgesics may be necessary. It is important to monitor the individual’s response to analgesics and adjust the dosage as needed to achieve adequate pain relief while minimizing side effects.
Non-pharmacologic pain management techniques
In addition to analgesics, non-pharmacologic pain management techniques can be employed to alleviate pressure ulcer-related pain. These techniques may include the use of heat or cold therapy, massage, relaxation techniques, or distraction methods. Each individual may respond differently to these techniques, so it is important to assess their effectiveness and tailor the interventions to the individual’s preferences and needs.
Infection Control
Infection control is a critical component of pressure ulcer management, as pressure ulcers can become infected and lead to serious complications.
Hand hygiene and aseptic technique
Proper hand hygiene and aseptic technique are essential in preventing the spread of infection. Healthcare professionals should perform hand hygiene before and after every wound assessment or dressing change. Aseptic technique should be followed during wound care procedures to minimize the risk of introducing bacteria into the wound. This includes using sterile gloves, sterile dressings, and sterile solutions when necessary.
Managing wound infections
Prompt identification and management of wound infections are crucial in preventing further complications. Signs of wound infection may include increased pain, redness, warmth, swelling, or purulent drainage. If an infection is suspected, appropriate cultures should be obtained, and antimicrobial therapy may be necessary. Close monitoring of the wound and regular assessment for signs of infection are essential for early intervention.
Isolation precautions
In certain cases, isolation precautions may be necessary to prevent the spread of infection. This may include implementing contact precautions, such as wearing gloves and gowns, when caring for individuals with infected pressure ulcers. It is important to follow facility-specific protocols and guidelines for infection control to minimize the risk of cross-contamination.

Psychosocial Support
Psychosocial support is vital in pressure ulcer management, as individuals with pressure ulcers may experience emotional distress and isolation.
Assessing patient’s emotional well-being
Assessing the patient’s emotional well-being is an important aspect of holistic care. Individuals with pressure ulcers may experience feelings of frustration, sadness, or anxiety. A thorough assessment should include discussing the individual’s emotional state, identifying coping mechanisms, and referring them to appropriate resources or support services if needed.
Providing psychological support
Providing psychological support can help individuals cope with the emotional challenges associated with pressure ulcers. This may involve offering empathetic listening, providing information about the healing process, or referring individuals to counseling services. Creating a supportive and empathetic environment can greatly contribute to the individual’s overall well-being.
Facilitating social interactions
Pressure ulcers can sometimes limit an individual’s ability to participate in social activities and interact with others. Facilitating social interactions and maintaining a sense of connectedness can greatly enhance the individual’s quality of life. Encouraging visits from family and friends, providing opportunities for engagement and recreation, and promoting activities that match the individual’s abilities can help combat feelings of isolation and improve overall well-being.
Collaborative Teamwork
Effective collaboration among healthcare professionals is crucial in providing comprehensive care for individuals with pressure ulcers.
Effective communication among healthcare professionals
Clear and effective communication among healthcare professionals is essential for coordinated care. This includes sharing relevant information, such as assessment findings, wound care plans, and response to interventions. Regular team meetings, interdisciplinary rounds, and electronic documentation systems can facilitate communication and ensure that everyone involved in the individual’s care is informed and working together towards common goals.
Multidisciplinary approach to care
A multidisciplinary approach to care involves the collaboration of various healthcare professionals with different areas of expertise. This may include nurses, wound care specialists, dietitians, physical therapists, and occupational therapists, among others. Each discipline brings unique knowledge and skills to the table, allowing for a comprehensive and individualized approach to pressure ulcer management. Regular interdisciplinary meetings and shared care plans can promote effective collaboration.
Collaborating with other departments
In addition to the healthcare team, collaboration with other departments within the healthcare facility is important for optimal pressure ulcer management. This may involve working closely with the facility’s nutrition services to ensure adequate nutritional support, consulting with the pharmacy for appropriate medication management, or coordinating with the materials management department for the procurement of specialized wound care supplies. Collaboration with other departments can help ensure that all aspects of care are addressed and integrated into the individual’s overall plan of care.

Patient Education
Patient education is essential in pressure ulcer management to empower individuals and promote active involvement in their own care.
Educating patients about pressure ulcer prevention
Educating patients about pressure ulcer prevention is a crucial step in reducing the incidence of pressure ulcers. This may include teaching individuals about the importance of regular repositioning, proper skin care, maintaining good nutrition, and avoiding habits that can increase the risk of pressure ulcers, such as smoking or excessive alcohol consumption. Providing written materials or visual aids can reinforce the education and serve as a reference for individuals.
Teaching self-care techniques
Teaching individuals self-care techniques can help them actively participate in their own wound care. This may include demonstrating proper wound cleansing techniques, explaining the importance of maintaining a clean and moist wound environment, and guiding individuals in correctly applying dressings. By empowering individuals with the knowledge and skills to care for their own wounds, they become active participants in their care and can contribute to better outcomes.
Importance of follow-up care
Emphasizing the importance of follow-up care is essential for successful pressure ulcer management. Regular follow-up appointments help monitor the progress of wound healing, identify and address any complications, and adjust treatment interventions if necessary. It is important to educate individuals about the need for regular follow-up visits and encourage them to promptly report any changes in their condition between appointments.
Documentation
Accurate and timely documentation is crucial in pressure ulcer management for communication, continuity of care, and legal purposes.
Accurate and timely documentation of wound assessments
Accurate and timely documentation of wound assessments is essential for monitoring changes in the pressure ulcer and evaluating the effectiveness of interventions. Detailed descriptions, measurements, and photographs of the wound should be recorded. Any changes in wound characteristics, such as size, depth, odor, or drainage, should be documented accurately and promptly. This documentation serves as a reference for healthcare professionals involved in the individual’s care and provides a baseline for future assessments.
Recording interventions and outcomes
Recording interventions and outcomes is important for evaluating the effectiveness of the care provided. This includes documenting the specific wound care techniques used, the type of dressings applied, any debridement procedures performed, and the response of the wound to these interventions. If any complications or adverse events occur, they should be documented and reported according to facility protocols.
Communication of information to other healthcare providers
Effective communication of information to other healthcare providers is critical for continuity of care. This may involve sharing wound assessment findings, treatment plans, and progress notes with other members of the healthcare team, including physicians, wound care specialists, and therapists. Clear and concise documentation ensures that everyone involved in the individual’s care has access to the necessary information to make informed decisions and provide appropriate interventions.
In conclusion, managing pressure ulcers requires a comprehensive approach that includes risk assessment, clinical assessment, prevention strategies, wound care and dressing selection, nutritional considerations, pain management, infection control, psychosocial support, collaborative teamwork, patient education, and documentation. By addressing each aspect of care, healthcare professionals can provide the best possible management for individuals with pressure ulcers.
