You’re about to embark on a journey into the fascinating world of Functional Neurological Disorder (FND). In this article, we’ll delve into the causes behind this complex condition that affects the nervous system. FND can manifest as a wide range of physical symptoms, such as muscle weakness, paralysis, and seizures, without any underlying structural or biochemical abnormalities. Through exploring the underlying causes, you will gain a deeper understanding of this intriguing disorder and the impact it has on the lives of those affected. So, let’s embark on this journey together and uncover the mysteries of FND!

Introduction
Welcome to this comprehensive article on Functional Neurological Disorder (FND). In this article, we will explore the definition of FND, its prevalence, risk factors, biological mechanisms, psychological factors, social and cultural factors, diagnostic challenges, and treatment approaches. We will also look into future directions in the field of FND research and treatment. Whether you are seeking information for yourself or a loved one, this article aims to provide a friendly and informative overview of the topic.
Definition of Functional Neurological Disorder
Functional Neurological Disorder, also known as FND, is a condition characterized by neurological symptoms that cannot be explained by an underlying organic or structural disorder. These symptoms are real and often disabling, affecting various parts of the body, such as movement, sensory perception, or cognition. FND can have a significant impact on an individual’s quality of life and daily functioning.
Prevalence of Functional Neurological Disorder
Global Prevalence
The global prevalence of FND is still not well understood due to the complexity of the condition and the lack of standardized diagnostic criteria. Estimates suggest that FND affects around 2 to 31 per 100,000 individuals. However, it is important to note that these numbers might vary depending on the populations studied and the diagnostic methods used.
Gender and Age Differences
Research indicates that FND may be more common in women than men, with a higher prevalence observed in females across various age groups. However, FND can affect individuals of any age, including children and older adults. The reasons behind these gender and age differences are still under investigation.
Risk Factors
Physical Trauma
Physical trauma, such as motor vehicle accidents or falls, has been identified as a potential risk factor for developing FND. In some cases, the onset of FND symptoms can be traced back to a traumatic event. However, it is essential to understand that not everyone who experiences physical trauma will develop FND.
Psychological Trauma
Psychological trauma, including experiences such as abuse, neglect, or emotional distress, has also been associated with the development of FND. Research suggests that the stress and emotional burden resulting from traumatic experiences may contribute to the manifestation of FND symptoms. It is vital to address and treat underlying psychological trauma in FND patients.
Genetic Factors
While the exact genetic factors contributing to FND are still unclear, studies have indicated a potential role of genetic susceptibility in the development of the disorder. Family history and genetic predisposition may increase the likelihood of developing FND, but further research is needed to fully understand the complex interplay between genetics and FND.
Environmental Factors
Certain environmental factors, such as exposure to toxins or infectious agents, have been proposed as potential triggers for FND. While the precise mechanisms by which these factors influence the development of FND are not fully known, they highlight the importance of exploring the interaction between the environment and the nervous system.

Biological Mechanisms
Brain Connectivity
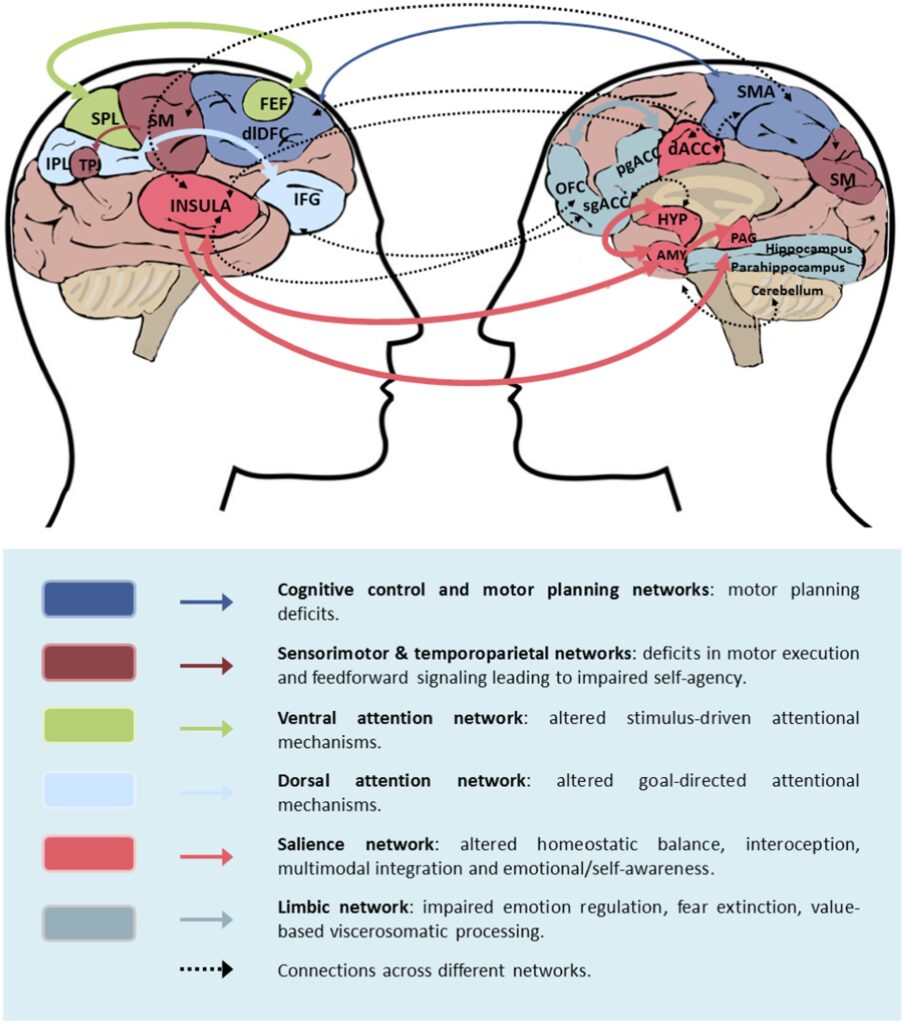
Research suggests that alterations in brain connectivity may play a role in the development of FND. Functional imaging studies have revealed abnormalities in the connections between different brain regions in individuals with FND. These altered patterns of connectivity may contribute to the generation of FND symptoms, providing insights into the underlying mechanisms of the disorder.
Neurotransmitter Imbalances
Imbalances in neurotransmitters, the chemical messengers of the brain, have also been implicated in FND. Disruptions in the delicate balance of neurotransmitters, such as dopamine and serotonin, can affect various neurological functions and potentially contribute to the manifestation of FND symptoms. Further research is needed to fully understand the specific neurotransmitter dysregulation in FND.
Abnormal Brain Activation
Studies using functional imaging techniques have shown abnormal patterns of brain activation in individuals with FND. These altered activation patterns suggest that certain brain regions may be overactive or underactive in individuals with FND, further supporting the hypothesis of dysfunctional brain mechanisms. Understanding these abnormal brain activation patterns may lead to more targeted treatment approaches for FND.
Psychological Factors
Stress and Trauma
Stress and trauma, both acute and chronic, have been recognized as significant psychological factors in FND. The complex relationship between mental and physical health highlights the importance of addressing emotional well-being in the management of FND. Stress management techniques, therapy, and support can help individuals with FND cope with their symptoms and improve their overall quality of life.
Personality Traits
Certain personality traits have been associated with an increased risk of developing FND. Traits such as neuroticism, perfectionism, and somatic focusing may contribute to the vulnerability to FND. Understanding the interplay between personality traits and FND can aid in the development of personalized treatment approaches and strategies.
Maladaptive Coping Strategies
Individuals with FND may resort to maladaptive coping strategies to manage their symptoms, such as excessive avoidance or dependence on healthcare professionals. These unconscious behaviors can reinforce the symptoms and perpetuate the cycle of disability. Identifying and addressing these maladaptive coping strategies through therapy and counseling are essential for improving functional outcomes in FND.
Social and Cultural Factors
Socioeconomic Status
Socioeconomic status can influence the development, course, and outcome of FND. Limited access to healthcare, financial stress, and lower educational attainment may contribute to the persistence and severity of FND symptoms. Addressing these social determinants of health is crucial for promoting equitable care and improving outcomes in individuals with FND.
Cultural Beliefs and Stigma
Cultural beliefs and stigmatization surrounding neurological disorders can impact the experiences of individuals with FND. Misunderstandings about the nature of FND may lead to skepticism and dismissiveness, further exacerbating the challenges faced by those affected. Promoting awareness, education, and supportive cultural attitudes are vital in reducing the stigma associated with FND.
Diagnostic Challenges
Overlap with Other Disorders
One of the diagnostic challenges in FND is the overlap with other neurological and psychiatric disorders. The symptoms of FND can mimic those of various conditions, such as epilepsy, multiple sclerosis, and conversion disorder. Careful clinical assessment and collaboration among different healthcare professionals are necessary to differentiate FND from other disorders accurately.
Subjectivity of Symptoms
The subjective nature of FND symptoms poses another diagnostic challenge. FND symptoms are often self-reported by the individual, making objective assessment difficult. Clinicians must rely on patient history, thorough examination, and collaboration with multidisciplinary teams to arrive at a diagnosis and rule out other potential explanations for the symptoms.
Lack of Reliable Biomarkers
Currently, there are no reliable biomarkers for FND diagnosis. Biomarkers, such as blood tests or imaging techniques, play a crucial role in many medical conditions, aiding in diagnosis and treatment decisions. The absence of objective biomarkers for FND emphasizes the need for further research to identify reliable indicators of the disorder.

Treatment Approaches
Psychotherapy
Psychotherapy, including cognitive-behavioral therapy and psychodynamic therapy, has shown promise in the treatment of FND. Addressing underlying psychological factors, enhancing coping skills, and promoting emotional well-being can help individuals with FND manage their symptoms and improve their overall functioning.
Physical Therapy
Physical therapy interventions, focusing on graded exercise programs, movement rehabilitation, and functional restoration, can be beneficial for individuals with FND. This multidisciplinary approach aims to improve physical functioning, reduce disability, and enhance overall quality of life.
Medication
Medication management is often individualized for each person with FND and depends on the specific symptoms and associated conditions. Various medications, such as antidepressants or antiepileptic drugs, may be prescribed to target specific symptoms or address comorbidities. Close monitoring and collaboration with healthcare professionals are essential for finding the most effective medication regimen.
Neurostimulation
Emerging research has explored the use of neurostimulation techniques, such as transcranial magnetic stimulation (TMS) and deep brain stimulation (DBS), as potential treatment options for FND. These techniques aim to modulate brain activity and restore normal neural functioning, providing new avenues for therapeutic interventions in FND.
Future Directions
Advancements in Neuroimaging Techniques
Continued advancements in neuroimaging techniques, such as functional magnetic resonance imaging (fMRI) and electroencephalography (EEG), hold promise for unraveling the biological mechanisms underlying FND. By further understanding the brain abnormalities associated with FND, researchers can develop more targeted treatments and improve diagnostic accuracy.
Targeted Treatment Strategies
With a better understanding of the complex interplay of genetic, environmental, psychological, and social factors in FND, future treatment strategies can be developed to target specific mechanisms and individualized needs. Personalized medicine approaches, including genetics-based therapies and precision psychiatry, may revolutionize the field of FND management.
In conclusion, Functional Neurological Disorder is a complex condition with a range of factors contributing to its development and manifestation. By recognizing the various risk factors, understanding the underlying biological and psychological mechanisms, and acknowledging the impact of social and cultural factors, we can strive towards improved diagnostic accuracy and personalized treatment approaches for individuals with FND. With ongoing research and advancements in the field, there is hope for better outcomes and increased understanding of this often misunderstood disorder.
