Imagine this: You’re going about your day, feeling perfectly fine, when suddenly you notice blood in your urine. It’s a startling discovery, to say the least. You’re left wondering what could be causing this and how serious it might be. Well, fear not, because in this comprehensive guide, we’ll walk you through everything you need to know about hematuria – the medical term for blood in the urine. From the various causes and types of hematuria to the diagnostic tests and treatment options available, this article will provide you with the knowledge and guidance you need to navigate this potentially concerning symptom. So, let’s dive in and unravel the mysteries of hematuria together!
Definition
Hematuria, also known as blood in the urine, is a condition characterized by the presence of red blood cells in the urine. It can be categorized into two types: gross hematuria and microscopic hematuria.
Gross Hematuria
Gross hematuria refers to the visible presence of blood in the urine, leading to a pink, red, or brownish color. It can be alarming to see, as the urine may appear to be heavily stained with blood. However, the actual amount of blood loss may not always be significant.
Microscopic Hematuria
Microscopic hematuria, on the other hand, is not visible to the naked eye and can only be detected through laboratory tests. Even though the blood is not apparent, the presence of red blood cells in the urine indicates an underlying issue that needs further investigation.
Types
Hematuria can be further classified into specific types based on the source of the bleeding. These types include glomerular hematuria, nonglomerular hematuria, urological hematuria, and non-urological hematuria.
Glomerular Hematuria
Glomerular hematuria occurs when there is bleeding within the glomeruli, which are tiny blood vessels in the kidneys responsible for filtering waste products from the blood. Conditions such as glomerulonephritis and lupus nephritis can lead to glomerular hematuria.
Nonglomerular Hematuria
Nonglomerular hematuria occurs when the bleeding is derived from sources outside the glomeruli. This type of hematuria can result from issues in the urinary tract, such as urinary tract infections (UTIs), kidney stones, or bladder or kidney infections.
Urological Hematuria
Urological hematuria refers to bleeding caused by problems within the urinary tract, including the kidneys, ureters, bladder, and urethra. Conditions such as bladder or kidney cancer, urinary tract obstructions, and injury to the urinary tract can lead to urological hematuria.
Non-Urological Hematuria
Non-urological hematuria involves bleeding that originates from outside the urinary tract. This can be caused by disorders such as blood disorders or inherited conditions like sickle cell disease or hemophilia.

Causes
There are various factors and underlying conditions that can lead to the development of hematuria. Understanding these causes is crucial in diagnosing and managing the condition effectively.
Kidney Stones
Kidney stones, which are solid mineral and acid salts that form in the kidneys, can cause irritation and damage to the urinary tract. As a result, they can lead to blood in the urine.
Urinary Tract Infection
Urinary tract infections, particularly those affecting the bladder or urethra, can cause inflammation and subsequent bleeding in the urinary tract, resulting in hematuria.
Bladder or Kidney Infections
Infections specifically targeting the bladder or kidneys, such as cystitis or pyelonephritis, respectively, can cause hematuria due to the inflammation and damage they cause to the urinary tract.
Injury to the Urinary Tract
Trauma or injury to the urinary tract, such as from a fall or accident, can result in blood in the urine. Blunt force trauma or penetrating injuries can cause visible hematuria.
Kidney Disease
Certain kidney diseases, such as glomerulonephritis or polycystic kidney disease, can lead to glomerular hematuria. These conditions affect the filtering ability of the glomeruli, leading to blood leakage into the urine.
Inherited Disorders
Inherited disorders that affect the blood or organs involved in the urinary system can contribute to the development of hematuria. Examples include sickle cell disease, which affects the shape and function of red blood cells, and Alport syndrome, which causes kidney abnormalities.
Bladder or Kidney Cancer
Cancerous growths in the bladder or kidneys can cause bleeding, resulting in hematuria. It is important to rule out cancer as a cause of hematuria, especially in older individuals or those with risk factors.
Urinary Tract Obstruction
Blockages or obstructions in the urinary tract, such as from an enlarged prostate or urinary stones, can lead to urinary tract infections and subsequent hematuria.
Enlarged Prostate
An enlarged prostate, a condition known as benign prostatic hyperplasia (BPH), can cause urinary symptoms and increase the risk of bladder infections, ultimately leading to hematuria.
Blood Disorders
Certain blood disorders, such as hemophilia or clotting disorders, can increase the likelihood of bleeding and hematuria. These conditions disrupt the body’s ability to form blood clots properly.
Risk Factors
Several factors can increase an individual’s risk of developing hematuria. Recognizing these risk factors is important in identifying those who may be more susceptible to the condition.
Age and Gender
Men over the age of 50 are at a higher risk of experiencing hematuria due to factors such as an enlarged prostate. Women may also experience hematuria due to factors like menopause or urinary tract infections.
Certain Medications
Some medications, such as blood thinners, anti-inflammatory drugs, or antibiotics, can increase the likelihood of experiencing hematuria. These medications can affect blood clotting or irritate the urinary tract.
Family History
A family history of kidney disease, kidney stones, or certain inherited disorders increases the risk of developing hematuria. There may be genetic predispositions that cause abnormalities in the urinary system.
Exposure to Chemicals
Exposure to certain chemicals or toxins, such as those found in certain industries or occupations, can irritate the urinary tract and potentially lead to hematuria.
Smoking
Smoking increases the risk of developing bladder cancer, which can cause hematuria. The chemicals in tobacco smoke can also irritate the urinary tract and contribute to the development of hematuria.
Urinary Tract Infections
Individuals who frequently experience urinary tract infections are at a higher risk of developing hematuria. These infections can cause inflammation and damage to the urinary tract.
Kidney Stones
A history of kidney stones increases the risk of future occurrences, which can lead to hematuria.
Kidney or Bladder Infections
Recurrent kidney or bladder infections can cause damage to the urinary tract and increase the likelihood of hematuria.
Strenuous Exercise
Engaging in intense physical activities or exercises that put a strain on the body can increase the risk of developing hematuria. This is more commonly observed in athletes or individuals participating in high-impact sports.

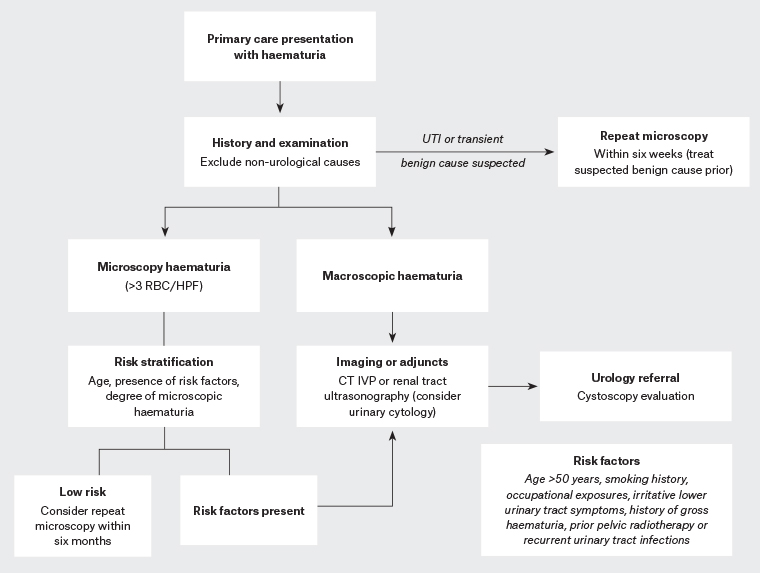
Diagnosis
When hematuria is suspected, a comprehensive diagnostic approach is necessary to determine the underlying cause and guide appropriate management. The following steps are typically involved in the diagnostic process:
Medical History
Your healthcare provider will inquire about your medical history, including any previous episodes of hematuria, known medical conditions, medications, and family history. This helps provide valuable insight into potential causes or associated risk factors.
Physical Examination
A physical examination may be conducted to assess your overall health and identify any visible signs or symptoms. This may include an examination of the abdomen, urinary system, and certain organs.
Urine Tests
Urine tests, such as a urinalysis or urine culture, are crucial in diagnosing hematuria. These tests help identify the presence of red blood cells, assess urine color and clarity, and detect any signs of infection or abnormalities.
Imaging Tests
Imaging tests, such as ultrasound, computed tomography (CT) scan, or magnetic resonance imaging (MRI), may be recommended to visualize the urinary tract and identify any structural abnormalities, tumors, or kidney stones.
Cystoscopy
Cystoscopy involves using a thin, flexible tube with a camera (cystoscope) to examine the inside of the bladder and urethra. This allows the healthcare provider to visually inspect these structures for any signs of bleeding or abnormalities.
Biopsy
In certain cases, a biopsy may be required to obtain a sample of tissue from the urinary tract or kidneys for further analysis. This is typically done using minimally invasive techniques and can provide important information about the underlying cause of hematuria if other tests are inconclusive.
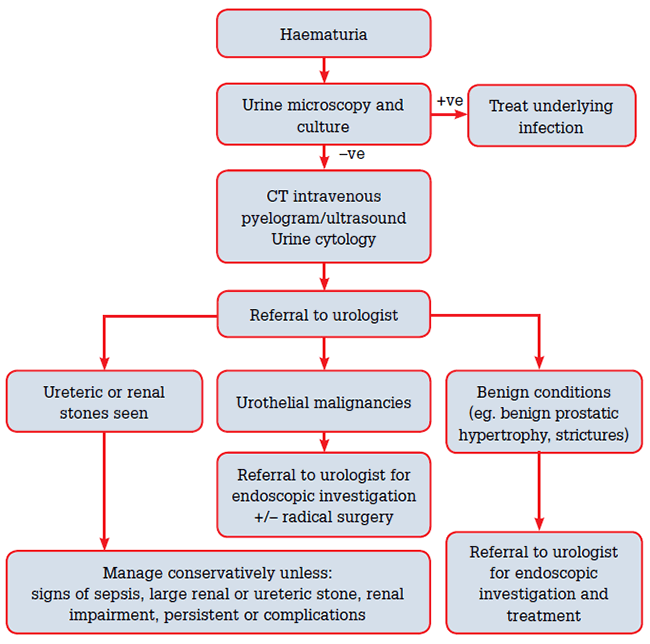
Management
The appropriate management of hematuria depends on the underlying cause and the severity of the condition. Here are some common approaches to managing hematuria:
Treating Underlying Causes
Addressing the underlying cause of hematuria is of utmost importance. This may involve treating urinary tract infections with antibiotics, removing kidney stones, or managing kidney diseases or disorders through medication or other therapies.
Medications
Depending on the specific condition causing hematuria, medications may be prescribed to alleviate symptoms, manage inflammation, or slow the progression of kidney disease or other underlying conditions.
Surgical Interventions
In some cases, surgical interventions may be necessary to remove obstructions, tumors, or cancerous growths contributing to hematuria. Procedures such as lithotripsy, cryotherapy, or laser surgery may be employed to address kidney stones or certain types of cancer.
Lifestyle Changes
Making lifestyle modifications can significantly impact the management and prevention of hematuria. This may include adopting a healthy diet, staying hydrated, avoiding smoking or exposure to toxins, and practicing good hygiene.
Regular Monitoring
Regular check-ups and monitoring are essential for individuals with a history of hematuria or those at risk of developing the condition. This allows healthcare providers to detect any changes or new symptoms, ensuring early intervention and appropriate management.

Complications
While hematuria itself is not always a dire condition, it can lead to several potential complications if left untreated or unmanaged. These complications may include:
Anemia
Chronic or recurrent hematuria can result in anemia, a condition characterized by low levels of red blood cells. Anemia can cause fatigue, weakness, and shortness of breath, among other symptoms.
Kidney Damage
Repeated episodes of hematuria, particularly if associated with underlying kidney diseases or conditions, can lead to kidney damage or impairment. This can affect kidney function and overall health.
Urinary Tract Infections
Hematuria can increase the risk of urinary tract infections, as inflammation and damage to the urinary tract provide an ideal environment for bacterial growth. Recurrent infections can cause further complications, such as kidney infections.
Cancer
In some cases, hematuria may be a sign of underlying bladder or kidney cancer. Early detection and prompt treatment are crucial to improving prognosis and increasing the chances of successful treatment.
Emotional Impact
Experiencing hematuria can be emotionally distressing for individuals, particularly if the cause is unknown or if they have a family history of cancer or kidney disease. Anxiety, fear, and stress may arise, highlighting the significance of emotional support during the diagnostic and management process.
Prevention
While some causes of hematuria may not be preventable, adopting certain lifestyle habits and practices can minimize the risk of developing the condition. Here are some key preventive measures:
Maintaining a Healthy Lifestyle
Eating a balanced diet, exercising regularly, and maintaining a healthy weight can reduce the risk of developing underlying conditions such as kidney disease or obesity-related complications that contribute to hematuria.
Hydration
Staying adequately hydrated helps dilute urine and prevents the formation of kidney stones or concentrated urine, which can irritate the urinary tract and lead to hematuria. Aim to drink plenty of water throughout the day.
Regular Exercise
Engaging in regular exercise promotes overall health and can reduce the risk of certain conditions that contribute to hematuria, such as obesity, high blood pressure, or diabetes.
Personal Hygiene
Practicing good personal hygiene, particularly when it comes to the genital area, can significantly reduce the risk of urinary tract infections and subsequent hematuria. This includes regular and thorough cleaning, especially before and after sexual activity.
Medical Check-ups
Undergoing regular medical check-ups allows healthcare providers to monitor your overall health and identify any potential risk factors or developing conditions. Regular screenings may include urine tests and blood work to detect any early signs of blood in the urine.
When to Seek Medical Help
Although hematuria can sometimes be harmless, certain circumstances call for immediate medical attention. Contact your healthcare provider if you experience any of the following:
Presence of Blood Clots in Urine
The presence of blood clots in the urine suggests significant bleeding and should not be ignored. Seek medical help promptly to evaluate the cause and initiate appropriate management.
Persistent Hematuria
If you are consistently noticing blood in your urine or experiencing recurrent episodes of hematuria, it is essential to consult with a healthcare professional. Persistent hematuria may indicate a more serious underlying condition that requires further evaluation and treatment.
Abdominal Pain
The presence of severe or persistent abdominal pain along with hematuria should not be overlooked. This may be a sign of a urinary tract infection, kidney stones, or other conditions requiring medical attention.
Frequent Urinary Tract Infections
If you experience recurrent urinary tract infections along with hematuria or notice changes in your urinary patterns, such as increased frequency or urgency, it is important to seek medical help. Frequent infections can lead to complications and may be indicative of an underlying issue.
Conclusion
Hematuria can be a concerning symptom, but with proper diagnosis and management, the underlying causes can be identified and treated. It is important to consult with a healthcare professional if you experience blood in your urine or have any associated symptoms. By understanding the different types, causes, risk factors, and complications of hematuria, you can take the necessary steps to maintain a healthy urinary system and overall well-being. Regular check-ups, healthy lifestyle habits, and open communication with your healthcare provider can help ensure early detection and appropriate management of any underlying conditions. Remember, your health is a priority, and seeking medical advice is always recommended when faced with unusual symptoms or concerns.