In this article, you will discover the essential nursing considerations for patients experiencing eye floaters and eye flashes. These visual disturbances can be distressing for individuals, and as a nurse, it is crucial to possess the knowledge and understanding to provide appropriate care and support. By incorporating effective nursing management strategies, you can help alleviate concerns, educate patients, and ensure their overall well-being. Join us as we explore the important role nurses play in addressing eye floaters and eye flashes, and learn the key considerations to enhance patient care.

Anatomy and Physiology of the Eye
Structure of the Eye
The eye is a complex organ that allows you to see and perceive the world around you. It consists of several structures working together to capture and process visual information. The main parts of the eye include the cornea, pupil, iris, lens, retina, and optic nerve. The cornea is the clear, dome-shaped front part of the eye that helps to focus light onto the retina. The pupil is the opening in the center of the iris, which controls the amount of light entering the eye. The iris is the colored part of the eye that regulates the size of the pupil. The lens is located behind the iris, and its main function is to focus light onto the retina. The retina is a thin layer of tissue at the back of the eye that contains the cells responsible for detecting light and sending visual signals to the brain. The optic nerve connects the retina to the brain, allowing the transmission of visual information.
Function of the Eye
The primary function of the eye is vision, which is the ability to perceive and interpret visual stimuli. The process of vision begins with light entering the eye through the cornea and pupil. The iris adjusts the size of the pupil to control the amount of light entering the eye, ensuring optimal vision in various lighting conditions. The lens then focuses the incoming light onto the retina. The cells in the retina, called photoreceptors, detect the light and convert it into electrical signals. These signals are then transmitted to the brain via the optic nerve, where they are interpreted as visual images. The brain processes these images, allowing you to see and comprehend the world around you.
Role of Vitreous Humor
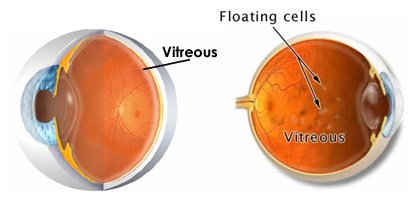
The vitreous humor is a gel-like substance that fills the space between the lens and the retina. It helps to maintain the shape of the eyeball and plays a crucial role in the transmission of light to the retina. The vitreous humor also helps to protect the retina and provide nutrients to its cells. As we age, the vitreous humor can undergo changes, leading to the formation of floaters and flashes, which can affect vision and require management and treatment.
Understanding Eye Floaters
Definition of Eye Floaters
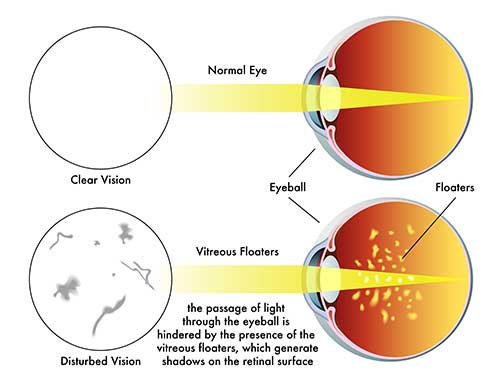
Eye floaters, also known as vitreous floaters, are tiny specks or strings that appear in your field of vision. They are actually shadows cast by tiny clumps of gel or cells in the vitreous humor as they move within the eye. Floaters may appear as dark dots, lines, or cobweb-like shapes, and they can be more noticeable when looking at a bright background or in well-lit environments.
Causes of Eye Floaters
Eye floaters are primarily caused by changes in the vitreous humor that occur with age. As the vitreous humor becomes more liquid and less gel-like, small particles can clump together and cast shadows on the retina, resulting in floaters. Other factors that can contribute to the development of floaters include eye inflammation or injury, retinal tears or detachments, and certain medical conditions such as diabetes or nearsightedness.
Diagnosis of Eye Floaters
Diagnosing eye floaters typically involves a comprehensive eye examination performed by an eye care professional. The examination may include a review of your medical history, a visual acuity test to assess your ability to see clearly, and a dilated fundus examination to examine the internal structures of the eye. This examination allows the eye care professional to determine the cause and severity of the floaters and recommend appropriate management options.
Management of Eye Floaters
In most cases, eye floaters are harmless and do not require treatment. However, if they become bothersome or significantly affect your vision, there are treatment options available. One option is laser therapy, where a laser is used to break up the floaters into smaller fragments, making them less noticeable. Another option is a surgical procedure called vitrectomy, where the vitreous humor is removed and replaced with a saline solution. Both of these treatments should be discussed with a qualified ophthalmologist to determine the best approach for your specific condition.

Recognizing Eye Flashes
Definition of Eye Flashes
Eye flashes, also known as photopsia, are brief bursts of light that appear in your visual field. They can appear as flickering lights, lightning-like streaks, or flashes of color. Unlike floaters, eye flashes are not caused by shadows cast on the retina, but rather by mechanical or biochemical stimulation of the retina or the optic nerve.
Causes of Eye Flashes
Eye flashes can have various causes, including the normal aging process of the eye, which can cause the gel-like vitreous humor to shrink and pull away from the retina. This process, known as vitreous detachment, can stimulate the retina and result in the perception of flashes. Other potential causes of eye flashes include trauma or injury to the eye, retinal tears or detachments, migraines, and certain medical conditions such as diabetic retinopathy or ocular migraines.
Diagnosis of Eye Flashes
If you experience eye flashes, it is essential to seek medical attention promptly. An eye care professional will conduct a thorough examination to determine the cause and severity of the flashes. This may include a visual acuity test, a dilated fundus examination, and additional diagnostic tests such as an optical coherence tomography (OCT) scan or a fluorescein angiography. These tests help to evaluate the condition of the retina and identify any underlying factors contributing to the flashes.
Management of Eye Flashes
The management of eye flashes depends on the underlying cause. If the flashes are a result of a harmless condition, such as vitreous detachment, no specific treatment may be required, and the flashes may gradually decrease or disappear over time. However, if the flashes are due to a more serious condition, such as a retinal tear or detachment, immediate intervention is necessary to prevent further vision loss. Treatment options may include laser therapy, cryotherapy, or vitrectomy surgery, which should be performed by a qualified ophthalmologist based on the individual’s specific needs.
Assessment and Observation Techniques
Taking Patient History
When assessing a patient’s eye health, it is crucial to obtain a comprehensive patient history. This includes asking about any current eye symptoms, such as floaters or flashes, as well as any history of eye conditions or surgeries. It is also important to inquire about any systemic health conditions, medications, or lifestyle factors that may impact eye health, such as diabetes, hypertension, or smoking. Gathering this information helps to identify any potential risk factors or underlying conditions that may contribute to eye floaters or flashes.
Visual Acuity Test
A visual acuity test is a standard assessment used to measure the sharpness and clarity of a patient’s vision. This test typically involves reading a series of letters or numbers on an eye chart from a specific distance. The results of the visual acuity test provide valuable information about a patient’s overall visual function and can help identify any refractive errors or visual impairments that may be affecting their vision.
Slit-Lamp Examination
A slit-lamp examination is a non-invasive procedure that allows for a detailed examination of the structures at the front of the eye, including the cornea, iris, and lens. This examination is performed using a specialized microscope called a slit lamp, which emits a thin beam of light that can be adjusted to illuminate different parts of the eye. By examining the front structures of the eye under magnification, the eye care professional can identify any abnormalities or signs of disease that may contribute to eye floaters or flashes.
Dilated Fundus Examination
A dilated fundus examination involves the use of dilating eye drops to widen the pupil and allow for a more thorough examination of the retina and optic nerve. This examination is crucial in evaluating the health of the internal structures of the eye and identifying any signs of retinal tears, detachments, or other retinal abnormalities that may be causing floaters or flashes. It provides a comprehensive view of the retina, allowing for a more accurate diagnosis and treatment plan.
Amsler Grid Test
The Amsler grid test is a simple tool used to detect and monitor changes in central vision. The grid consists of straight lines forming a square pattern, with a dot in the center. Patients are instructed to focus on the dot and report any distortions or missing areas in their peripheral vision. This test is particularly useful in detecting and monitoring changes associated with macular degeneration, which can cause visual distortions and impair central vision.
Patient Education and Support
Explaining Eye Floaters
Patient education plays a vital role in helping individuals understand eye floaters and manage their condition effectively. It is important to explain to patients that eye floaters are a common occurrence, particularly as we age, and are generally harmless. Providing information about the anatomy of the eye and the causes of floaters can help patients better comprehend why they are experiencing these symptoms. Furthermore, discussing the potential management options, including observation versus treatment, allows patients to make informed decisions and actively participate in their care.
Addressing Patient Concerns
Patients experiencing eye floaters or flashes may have concerns about their vision and overall eye health. It is essential to address these concerns empathetically and provide reassurance. Assuring patients that floaters are typically harmless and exploring any specific worries they may have can help alleviate anxiety and promote a sense of trust. Patients should also be encouraged to seek prompt medical attention if their symptoms worsen or if they experience any sudden changes in vision, as this may indicate a more serious underlying condition.
Providing Information on Self-Care
In addition to medical management, patients can benefit from self-care strategies to cope with eye floaters or flashes. Educating patients about lifestyle modifications, such as managing stress, maintaining a healthy diet, and protecting their eyes from excessive UV exposure, can help promote overall eye health. Additionally, providing guidance on self-monitoring for changes in symptoms or vision, and encouraging regular eye examinations, allows patients to actively participate in their eye care and take necessary precautions to maintain optimal visual health.
Supporting Emotional Well-being
Experiencing eye floaters or flashes can have a significant impact on a patient’s emotional well-being. It is essential to provide emotional support and validate their concerns. Active listening and empathy can help patients feel understood and supported during their journey. Encouraging open and honest communication, and providing appropriate resources for additional emotional support, such as counseling services or support groups, can further enhance the patient’s overall well-being and help them cope with any emotional challenges related to their eye condition.
Referral to Ophthalmologist
In some cases, the management of eye floaters or flashes may require the expertise of an ophthalmologist. If the symptoms are severe, persistent, or associated with other eye conditions, a referral to an ophthalmologist may be necessary. Ophthalmologists specialize in the diagnosis and treatment of eye disorders, including floaters and flashes. They can provide a higher level of care and offer advanced treatment options, such as laser therapy or surgical interventions, to address the patient’s specific needs.
Collaborative Care and Referrals
Interprofessional Collaboration
Interprofessional collaboration is essential in the management of eye floaters and flashes. As a nurse, you will work closely with other healthcare professionals, such as ophthalmologists, optometrists, and ophthalmic technicians, to ensure comprehensive and coordinated care for your patients. Effective communication, mutual respect, and sharing of expertise are vital for the optimal management of eye conditions, including assessment, diagnosis, treatment, and follow-up care.
Referral to Ophthalmologist
As mentioned earlier, a referral to an ophthalmologist may be necessary in certain cases of eye floaters or flashes. Ophthalmologists are medical doctors specializing in eye care, and they have extensive knowledge and experience in diagnosing and managing complex eye conditions. They can perform advanced diagnostic tests, provide surgical interventions when needed, and offer specialized treatment options. Collaborating with ophthalmologists helps ensure the best possible outcomes for patients with more severe or complicated cases of floaters or flashes.
Consultation with Optometrist
Working collaboratively with optometrists is also crucial in the management of eye floaters and flashes. Optometrists are eye care professionals who specialize in the diagnosis, treatment, and management of common eye conditions. They can provide comprehensive eye examinations, prescribe corrective lenses, and offer valuable advice on maintaining optimal eye health. Consulting with optometrists ensures that patients receive appropriate care and management for their eye health needs, enhancing their overall visual well-being.
Coordinating Follow-up Care
Coordinating follow-up care is an essential aspect of nursing management for eye floaters and flashes. After the initial assessment and treatment, patients may require regular monitoring and follow-up appointments to assess the progression of their condition, the effectiveness of treatment, and any potential complications. Coordinating these appointments, providing clear instructions, and addressing any concerns or questions the patient may have helps ensure continuity of care and promotes positive outcomes.
Complications and Risk Factors
Potential Complications
While eye floaters and flashes are usually benign, there are certain potential complications associated with these conditions. One complication is the development of retinal tears or detachments, particularly if the floaters or flashes are caused by vitreous traction on the retina. Retinal tears or detachments can lead to vision loss if not promptly diagnosed and treated. Another complication is the psychological impact of persistent or severe floaters or flashes, which can cause anxiety, depression, or reduced quality of life. It is essential to educate patients about these potential complications and to encourage regular eye examinations to detect any significant changes in their condition.
Factors Increasing Risk
Several factors can increase the risk of developing eye floaters or flashes. Age is a significant risk factor, as the vitreous humor naturally undergoes changes with age, making floaters more common. Individuals who are nearsighted or have undergone cataract surgery are also at increased risk. Other risk factors include a history of eye trauma or injury, ocular inflammation or infection, and certain medical conditions such as diabetes or hypertension. Understanding these risk factors can help identify patients who may be more susceptible to developing eye floaters or flashes and allow for appropriate monitoring and management.
Preventive Measures
While it may not be possible to prevent the development of eye floaters or flashes completely, there are certain preventive measures that individuals can take to promote eye health. Protecting the eyes from injury by wearing appropriate safety glasses or goggles when engaging in activities that pose a risk is essential. Managing systemic health conditions, such as diabetes and hypertension, through regular medical care and lifestyle modifications can also help reduce the risk of eye complications. Additionally, maintaining a healthy lifestyle, including a balanced diet, regular exercise, and avoiding smoking, can contribute to overall eye health and potentially minimize the occurrence of floaters or flashes.
Pharmacological Interventions
Medications for Symptom Relief
Pharmacological interventions for eye floaters and flashes primarily focus on managing symptoms and providing relief to patients. While there are no specific medications designed to eliminate floaters or flashes, certain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs) or corticosteroids, may be prescribed to reduce inflammation and improve symptomatology. It is important to note that medication alone may not completely eliminate floaters or flashes, and the potential benefits and risks should be thoroughly discussed with a healthcare provider.
Risks and Benefits of Medications
As with any medication, there are risks and benefits associated with the use of pharmacological interventions for eye floaters or flashes. It is essential for healthcare providers to educate patients about the potential risks, such as side effects, drug interactions, or allergic reactions, and discuss the benefits that medications may provide in managing symptoms. A thorough assessment of the patient’s medical history, current medications, and any contraindications or precautions is necessary to determine the appropriate course of pharmacological intervention.
Educating Patients on Medications
Patient education is critical when prescribing medications for eye floaters or flashes. It is essential to provide patients with clear and concise instructions on how to take the medication, including dosage, frequency, and duration. Educating patients about potential side effects, how to recognize them, and when to seek further medical advice is crucial for their safety and well-being. Patients should also be encouraged to ask questions and voice any concerns or uncertainties they may have regarding their medication regimen.
Surgical Interventions
Indications for Surgery
Surgical interventions for eye floaters or flashes are typically reserved for cases where the symptoms significantly impact a patient’s quality of life or when there is a risk of vision loss due to a retinal tear or detachment. Indications for surgery depend on a thorough evaluation of the patient’s condition, including the severity and persistence of the symptoms, the presence of retinal abnormalities, and the overall impact on vision and daily activities. It is important to carefully weigh the potential benefits against the risks of surgery and discuss these factors with the patient to determine the most appropriate course of action.
Different Surgical Options
There are several surgical options available for the treatment of eye floaters or flashes. One common procedure is vitrectomy, which involves removing the vitreous humor and replacing it with a saline solution. This procedure can help alleviate floaters by removing the clumps or particles casting shadows on the retina. Laser therapy or cryotherapy may also be used to target and break up larger floaters, making them less noticeable. The specific surgical option recommended depends on the individual patient’s needs, and a detailed discussion with an ophthalmologist is essential to determine the most suitable approach.
Pre- and Postoperative Care
Pre- and postoperative care for surgical interventions related to eye floaters or flashes is crucial for patient outcomes. This care involves educating the patient about the surgical procedure, its potential benefits and risks, and addressing any questions or concerns they may have. Preoperative care may include various preparations, such as fasting prior to surgery or discontinuing certain medications that may interfere with the surgical process. Postoperative care may involve monitoring for any signs of complications, providing appropriate eye care instructions, and scheduling follow-up appointments to assess the healing process and address any postoperative concerns.
Managing Surgical Expectations
Managing surgical expectations is a vital aspect of nursing care for patients undergoing surgical interventions for eye floaters or flashes. It is important to provide realistic information about the potential outcomes, as well as the limitations and risks associated with the procedure. Patients should understand that while surgery can provide symptom relief and improve vision in some cases, complete elimination of floaters or flashes may not always be achievable. Setting realistic expectations and ensuring open communication with patients can help foster trust and provide them with a more positive surgical experience.
Supporting Patients with Visual Changes
Assisting with Adaptation
When patients experience visual changes due to eye floaters or flashes, they may require assistance in adapting to these changes and optimizing their quality of life. As a nurse, you can provide support by educating patients about strategies to improve visual function, such as enhancing lighting conditions, using magnification devices or large-print materials, and organizing their environment to minimize potential hazards. Encouraging patients to explore adaptive techniques and technologies can help them maintain independence and engage in their daily activities confidently.
Referral to Low Vision Rehabilitation
For patients who continue to experience visual difficulties despite standard management options, referral to low vision rehabilitation may be beneficial. Low vision rehabilitation focuses on maximizing visual performance and promoting independence for individuals with vision impairment. Services offered through low vision rehabilitation can include specialized assessments, customized visual aids, mobility training, and counseling to address emotional and psychological aspects of vision loss. Collaborating with low vision specialists ensures that patients receive comprehensive and tailored support to enhance their visual functioning and overall well-being.
Promoting Independence
Maintaining independence is a crucial goal for patients experiencing visual changes. Nurses can play a key role in promoting independence by providing guidance on self-care techniques, organizing their environment to optimize safety and accessibility, and offering education on strategies to compensate for visual impairments. Encouraging patients to seek training in skills such as orientation and mobility, adaptive technology use, and daily living tasks can empower them to navigate their environment confidently and maintain a fulfilling lifestyle despite visual challenges.
Providing Assistive Devices
Assistive devices can significantly enhance visual function for patients with eye floaters or flashes. As a nurse, you can provide information and assistance in accessing suitable assistive devices. These devices can range from simple magnifiers or glare control filters to more advanced technologies, such as closed-circuit television systems or screen-reading software. Collaborating with low vision specialists, optometrists, or occupational therapists can help identify appropriate assistive devices tailored to the individual patient’s needs and facilitate their acquisition and training in their use.
In conclusion, understanding the anatomy and physiology of the eye is essential in comprehending the development, management, and nursing considerations for eye floaters and eye flashes. Recognizing the symptoms, diagnosing the causes, and effectively managing these conditions require a collaborative approach involving various healthcare professionals, such as ophthalmologists, optometrists, and nurses. Patient education and support play a crucial role in addressing concerns, providing information on self-care, and promoting emotional well-being. Collaborative care, referral to specialists, and appropriate assessment and observation techniques are essential for optimal patient outcomes. By addressing the complications, risk factors, and preventive measures associated with eye floaters and flashes, nurses can support patients in managing their condition and maintaining visual well-being.