Hey there! If you’re a nurse or aspiring to be one, we’ve got some valuable insights for you. In this article, we’ll be discussing the important nursing considerations when it comes to treating anal abscesses. From understanding the symptoms and causes to implementing effective nursing management strategies, we’ll provide you with a comprehensive guide that will help you navigate this condition with confidence. So, grab a cup of coffee, get comfortable, and let’s dive into the world of anal abscesses!

Assessment
Monitoring vital signs
In the assessment phase of treating an anal abscess, it is important to closely monitor the patient’s vital signs. This includes checking their temperature, heart rate, blood pressure, and respiratory rate. Monitoring vital signs is crucial in detecting any changes that may indicate infection or other complications. By regularly assessing the patient’s vital signs, healthcare providers can identify any abnormalities early on and provide appropriate interventions.
Assessing pain level
Another essential aspect of the assessment process is evaluating the patient’s pain level. Pain associated with an anal abscess can be quite intense and significantly impact a person’s quality of life. Healthcare professionals should use a pain assessment scale to quantify the severity of the pain and determine the most appropriate pain management strategies. Regularly assessing the patient’s pain level allows for the adjustment of pain medications or the exploration of alternative pain relief options if necessary.
Inspecting the affected area
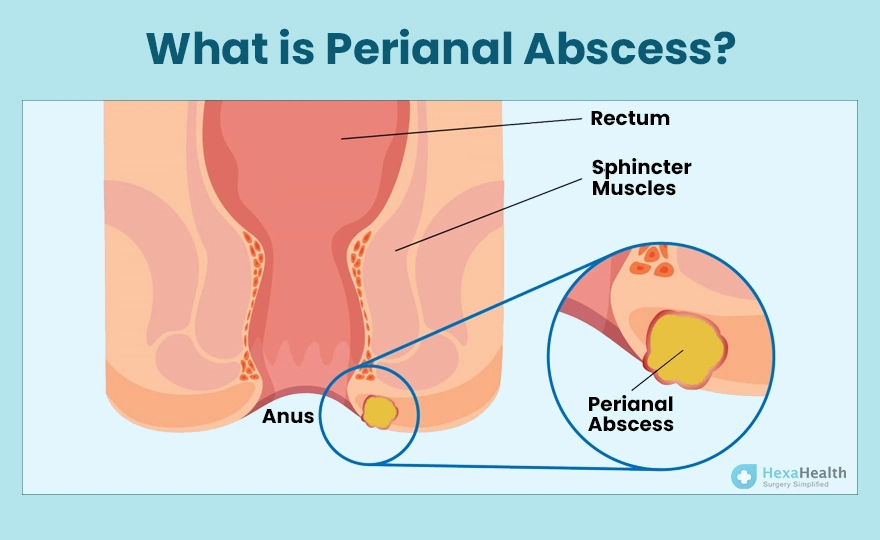
Inspecting the affected area is a critical step in assessing an anal abscess. By visually examining the area, healthcare providers can determine the location, size, and appearance of the abscess. This inspection also allows for the identification of any secondary complications, such as swelling, redness, or discharge. Careful inspection of the affected area provides vital information for developing an effective treatment plan and monitoring the healing progress.
Assessing signs of infection
Assessing signs of infection is crucial in the evaluation of an anal abscess. Infections can quickly worsen if not promptly identified and treated. Healthcare providers should carefully assess the area for signs such as increased redness, warmth, swelling, or the presence of pus. Monitoring for systemic signs of infection, such as fever or elevated white blood cell count, is also essential. By actively assessing for signs of infection, healthcare professionals can initiate appropriate interventions to prevent further complications.
Medical History
Gathering the patient’s medical history
When treating an anal abscess, it is vital to gather the patient’s complete medical history. This includes information about any pre-existing medical conditions, previous surgeries or treatments, and any current medications the patient may be taking. Understanding the patient’s medical history helps healthcare providers identify potential risk factors and tailor the treatment plan accordingly. Obtaining a thorough medical history also allows for a comprehensive evaluation of the patient’s overall health, aiding in the development of an appropriate care plan.
Identifying risk factors
Identifying risk factors is essential in effectively managing an anal abscess. Certain factors may increase a person’s susceptibility to developing an abscess or experiencing complications. Risk factors can include conditions such as diabetes, immunosuppression, or a history of prior abscesses. By identifying these risk factors, healthcare providers can implement preventive measures and consider additional interventions to minimize the likelihood of recurrence or complications.
Assessing previous treatments or surgeries
Knowing the patient’s previous treatments or surgeries is essential for managing an anal abscess. Previous interventions may impact the current treatment plan, as certain procedures, such as an incision and drainage, may have been performed in the past. Understanding the outcome of these previous treatments helps healthcare providers determine the best course of action and avoid unnecessary repetition. By assessing the patient’s previous treatments or surgeries, healthcare professionals can make informed decisions and ensure the most effective management of the anal abscess.
Diagnostic Tests
Ordering laboratory tests
Ordering laboratory tests is a crucial step in diagnosing and managing an anal abscess. These tests can provide valuable information about the patient’s overall health, determine the presence of infection, and assess the adequacy of immune function. Laboratory tests may include a complete blood count (CBC) to check for signs of infection, blood glucose levels to evaluate diabetes control, and cultures to identify specific pathogens. By ordering appropriate laboratory tests, healthcare providers can make accurate diagnoses and tailor treatment plans accordingly.
Performing a physical examination
Performing a thorough physical examination is an important aspect of diagnosing and monitoring an anal abscess. This examination involves a comprehensive assessment of the affected area, including palpation, inspection, and assessment of any related symptoms or complications. By conducting a physical examination, healthcare providers can gather essential information about the abscess’s characteristics, assess its size, and identify any potential complications. These findings contribute to a precise diagnosis and guide the development of an effective treatment plan.
Scheduling imaging studies
In some cases, scheduling imaging studies may be necessary to further evaluate an anal abscess. Imaging modalities such as ultrasound, computed tomography (CT) scans, or magnetic resonance imaging (MRI) can provide detailed information about the abscess’s location, extent, and relationship to nearby structures. These imaging studies can help healthcare providers determine the most appropriate treatment approach, especially in complex cases or abscesses that involve deeper tissues. By scheduling and interpreting imaging studies, healthcare professionals can optimize the management of an anal abscess.
Patient Education
Explaining the nature of the condition
Patient education plays a vital role in the treatment of an anal abscess. It is essential to explain the nature of the condition to the patient in a clear and comprehensive manner. This includes providing information about the cause of the abscess, its symptoms, and the potential complications that may arise if left untreated. By explaining the nature of the condition, healthcare providers empower patients to participate actively in their care and make informed decisions regarding their treatment options.
Describing potential treatment options
Describing the potential treatment options is crucial in helping patients understand the available choices for managing an anal abscess. This includes discussing both conservative and surgical interventions, such as antibiotics, incision and drainage, or surgical excision. Healthcare providers should explain the benefits, risks, and expected outcomes of each treatment option to ensure the patient’s understanding and involvement in the decision-making process. Describing potential treatment options allows patients to actively participate in their care and choose the approach that best suits their preferences and needs.
Educating about wound care and hygiene practices
Proper wound care and hygiene practices are essential for the successful management of an anal abscess. Healthcare providers should educate patients about the importance of keeping the affected area clean and dry, using appropriate wound dressings, and following recommended hygiene practices. This includes gentle cleansing, avoiding harsh soaps and strong perfumes, and ensuring regular hand hygiene. By providing comprehensive education on wound care and hygiene practices, healthcare professionals empower patients to take an active role in their recovery and prevent complications.

Pain Management
Administering appropriate analgesics
Pain management is a crucial aspect of treating an anal abscess. Healthcare providers should administer appropriate analgesics to relieve the patient’s pain and improve their comfort. This may include the use of non-opioid pain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs), or opioids for severe pain. The choice of analgesics should consider the patient’s pain level, medical history, and any contraindications or side effects. Administering appropriate analgesics allows patients to experience comfort while receiving treatment for their anal abscess.
Exploring non-pharmacological pain relief options
In addition to pharmacological interventions, healthcare providers should explore non-pharmacological pain relief options for managing pain associated with an anal abscess. These can include complementary therapies such as relaxation techniques, heat or cold therapy, or distraction techniques. Non-pharmacological pain relief options provide additional support and can be used in conjunction with analgesic medications to enhance pain management strategies. By exploring non-pharmacological alternatives, healthcare professionals can individualize pain management for each patient and optimize their overall comfort.
Monitoring effectiveness of pain management
The effectiveness of pain management interventions should be regularly monitored to ensure optimal relief for patients with an anal abscess. Healthcare providers should assess the patient’s pain level before and after administering analgesics or implementing pain relief strategies. By evaluating the effectiveness of pain management techniques, healthcare professionals can make adjustments as needed and ensure that the patient’s pain is adequately controlled. Monitoring the effectiveness of pain management interventions helps promote patient comfort and satisfaction throughout the treatment process.
Treatment Plan
Collaborating with the healthcare team
Collaboration among healthcare providers is vital in developing and implementing an effective treatment plan for an anal abscess. Depending on the severity and complexity of the abscess, the healthcare team may include nurses, physicians, surgeons, and other specialists such as infectious disease specialists or wound care nurses. By working together, healthcare professionals can pool their expertise, share information, and collectively decide on the most appropriate treatment approach for the patient. Collaborating with the healthcare team ensures comprehensive and coordinated care for individuals with an anal abscess.
Developing an individualized treatment plan
Each patient with an anal abscess requires an individualized treatment plan that addresses their specific needs and circumstances. The treatment plan should be tailored to factors such as the abscess’s location, size, and severity, as well as the patient’s overall health and preferences. Collaborating with the healthcare team, healthcare providers should develop a comprehensive plan that includes appropriate wound care, pain management, and follow-up care. An individualized treatment plan optimizes the chances of successful management and facilitates a smooth recovery for patients with an anal abscess.
Coordinating surgical interventions if required
In some cases, surgical interventions may be necessary for the management of an anal abscess. This can include procedures such as incision and drainage or surgical excision. Healthcare providers should coordinate with surgeons or other specialists to schedule and perform these interventions safely and efficiently. Coordinating surgical interventions involves ensuring proper preparation, informed consent, and appropriate post-operative care. By coordinating surgical interventions effectively, healthcare professionals can facilitate adequate abscess drainage, promote healing, and reduce the risk of complications.
Infection Control
Implementing standard precautions
Proper infection control practices are essential in the management of an anal abscess to prevent the spread of infection. Healthcare providers should implement standard precautions, including hand hygiene, appropriate use of personal protective equipment (PPE), and proper disinfection of equipment and surfaces. By adhering to these practices, healthcare professionals minimize the risk of healthcare-associated infections and protect both themselves and the patient. Implementing standard precautions is crucial in maintaining a safe and hygienic environment throughout the treatment of an anal abscess.
Administering antibiotics as prescribed
Antibiotics may be prescribed to manage or prevent infection in individuals with an anal abscess. Healthcare providers should ensure proper administration of antibiotics according to the prescribed dosage, frequency, and duration. They should also educate patients about the importance of completing the full course of antibiotics as advised. Administering antibiotics as prescribed helps eradicate or control the infection, reduce the risk of complications, and promote successful healing. Monitoring for any adverse reactions or interactions is also essential during antibiotic therapy.
Monitoring for signs of systemic infection
While treating an anal abscess, healthcare providers must closely monitor patients for signs of systemic infection. Systemic infection can occur if bacteria from the abscess enter the bloodstream and spread throughout the body, leading to a potentially life-threatening condition known as sepsis. Signs of systemic infection may include high fever, increased heart rate, rapid breathing, confusion, or decreased urine output. By vigilantly monitoring for these signs, healthcare professionals can promptly intervene and initiate appropriate treatment to prevent the progression of a systemic infection.
Wound Care
Cleaning and dressing the wound
Proper wound care is crucial in the management of an anal abscess. Healthcare providers should clean the wound thoroughly using sterile techniques and appropriate wound cleansers. They should also apply appropriate dressings to protect the wound and promote healing. The choice of wound dressings will depend on factors such as the amount of drainage, presence of infection, and clinician preference. Regular cleaning and dressing changes help prevent infection, maintain a moist environment for healing, and promote the formation of healthy granulation tissue.
Managing drainage and exudate
Managing drainage and exudate is an important aspect of wound care for individuals with an anal abscess. Excessive drainage and exudate can hinder the healing process and increase the risk of infection. Healthcare providers should assess the amount and characteristics of drainage regularly and adjust dressings as needed. This may involve providing adequate absorbent dressings, implementing negative pressure wound therapy, or ensuring proper positioning. By effectively managing drainage and exudate, healthcare professionals optimize wound healing and reduce the risk of complications.
Monitoring for signs of wound complications
Monitoring for signs of wound complications is crucial in the management of an anal abscess. These complications can include wound dehiscence (partial or complete separation of wound edges), delayed wound healing, or the development of a chronic wound. Healthcare providers should monitor the wound regularly for signs such as increasing pain, redness, swelling, foul odor, or non-healing. Timely identification of wound complications allows for prompt intervention and the implementation of appropriate care strategies. By diligently monitoring for signs of wound complications, healthcare professionals ensure optimal wound healing outcomes.

Nutritional Support
Assessing the patient’s nutritional status
Assessing the patient’s nutritional status is essential in providing comprehensive care for an individual with an anal abscess. Malnutrition or inadequate nutrient intake can compromise the immune system and delay the healing process. Healthcare providers should assess factors such as the patient’s weight, dietary intake, and any pre-existing nutritional deficiencies. This assessment may involve working with a registered dietitian to evaluate the patient’s caloric and nutrient needs. Identifying and addressing nutritional deficits allows healthcare professionals to develop appropriate dietary interventions and optimize the patient’s nutritional status.
Providing a balanced diet
Providing a balanced diet is crucial for individuals with an anal abscess to support healing and overall health. Healthcare providers should collaborate with registered dietitians to develop a nutritionally balanced meal plan tailored to the patient’s specific needs and preferences. This may involve ensuring an adequate intake of protein, vitamins, minerals, and other essential nutrients. A balanced diet enhances the body’s healing capabilities, supports the immune system, and reduces the risk of complications. By providing a balanced diet, healthcare professionals contribute to the successful recovery of individuals with an anal abscess.
Encouraging adequate fluid intake
Encouraging adequate fluid intake is vital for individuals with an anal abscess. Proper hydration supports the body’s overall function and aids in the healing process. Healthcare providers should emphasize the importance of consuming an adequate amount of water and other fluids throughout the day. This may include advising patients to avoid excessive caffeine or alcohol consumption, which can promote dehydration. Encouraging adequate fluid intake helps maintain hydration, supports wound healing, and prevents complications associated with dehydration.
Follow-Up and Continuity of Care
Scheduling regular follow-up appointments
Scheduling regular follow-up appointments is essential to ensure ongoing monitoring and appropriate management of an anal abscess. These appointments allow healthcare providers to assess the patient’s progress, evaluate treatment outcomes, and promptly intervene if necessary. Regular follow-up appointments may involve wound reassessment, laboratory tests, and discussions about ongoing care and potential complications. Scheduling follow-up appointments promotes continuity of care, ensures timely adjustments to the treatment plan, and provides patients with an opportunity to address any questions or concerns.
Coordinating with other healthcare providers
Coordinating with other healthcare providers is crucial in providing comprehensive care for individuals with an anal abscess. This often involves liaising with specialists such as surgeons, infectious disease experts, or wound care nurses. Healthcare providers should communicate information about the patient’s condition, treatment plan, and progress to ensure a coordinated and integrated approach to care. Coordinating with other healthcare providers allows for a cohesive management strategy, minimizes potential gaps in care, and optimizes patient outcomes.
Ensuring seamless transition of care
Ensuring a seamless transition of care is fundamental in the management of an anal abscess. As patients progress through different healthcare settings or transfer to home care, it is essential to promote continuity and ensure essential information is shared. Healthcare providers should collaborate with patients, their families, and other healthcare professionals to ensure a smooth transition from hospital to home or from one care setting to another. By facilitating a seamless transition of care, healthcare professionals promote patient safety, facilitate ongoing support, and enable effective management of an anal abscess beyond the acute care setting.
In summary, effectively managing an anal abscess requires a comprehensive approach that entails thorough assessment, individualized treatment plans, and proper wound care. Monitoring vital signs, assessing pain levels, and inspecting the affected area are essential for accurate diagnosis and ongoing evaluation. Gathering the patient’s medical history, identifying risk factors, and assessing previous treatments or surgeries inform the development of a tailored treatment plan. Diagnostic tests such as laboratory tests and imaging studies aid in diagnosis and treatment decision-making. Patient education, pain management, infection control, and nutritional support contribute to successful recovery. Coordinating with the healthcare team, providing wound care, and ensuring follow-up and continuity of care are vital for long-term management and prevention of complications. By following these important nursing considerations, healthcare professionals can provide optimal care for individuals with an anal abscess.