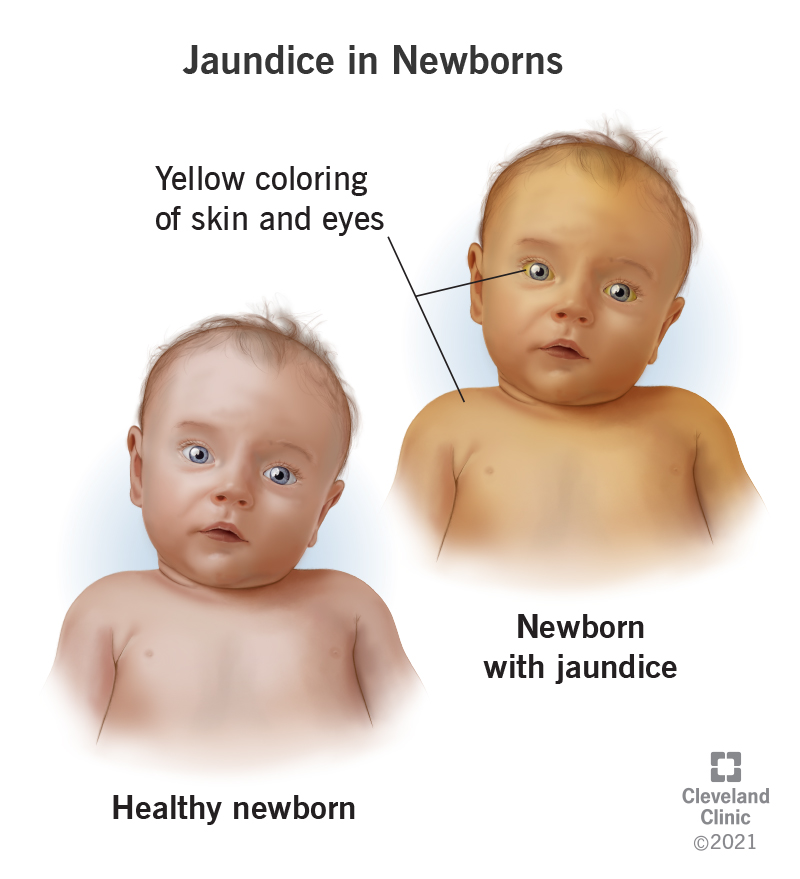
Jaundice, a common condition in newborns, occurs when there is a high level of bilirubin in their blood, causing a yellow discoloration in the skin and eyes. Although it is often harmless, it is important to identify and treat jaundice early on to prevent any potential complications. In this article, we will explore the signs and symptoms of jaundice in newborns, discuss the factors that contribute to its occurrence, and provide insights on how to effectively identify and treat this condition to ensure your little one’s health and well-being.

Understanding Jaundice in Newborns
Jaundice is a common condition that affects newborns, causing their skin and eyes to turn yellow. It is important for parents and caregivers to understand the causes, symptoms, complications, and treatment options for jaundice in newborns. By gaining a better understanding of this condition, you can ensure the well-being and proper care of your newborn.
Causes of Jaundice in Newborns
There are several factors that can contribute to the development of jaundice in newborns. The most common causes include:
Physiological Jaundice
Physiological jaundice is the most common type of jaundice in newborns. It occurs when there is an increased breakdown of red blood cells, leading to a build-up of bilirubin in the blood. This type of jaundice typically appears within the first few days of life and resolves on its own within a week or two.
Breastfeeding Jaundice
Breastfeeding jaundice can occur when the baby is not getting enough breast milk. Inadequate intake can contribute to a higher level of bilirubin in the blood. This type of jaundice usually appears within the first week of life and can be resolved by ensuring proper breastfeeding techniques and increasing milk supply.
Breast Milk Jaundice
Breast milk jaundice is a less common form of jaundice that occurs when substances in the breast milk disrupt the baby’s liver’s ability to process bilirubin. This type of jaundice may persist for several weeks and typically does not require treatment. However, it is important to monitor bilirubin levels closely.
Blood Incompatibility
In some cases, jaundice can occur due to a blood type incompatibility between the mother and the baby. This can happen if the mother has Rh-negative blood and the baby is Rh-positive. Incompatibility can lead to the destruction of red blood cells in the baby, causing an increase in bilirubin levels.
Infections
Certain infections, such as urinary tract infections or sepsis, can contribute to the development of jaundice in newborns. These infections can disrupt the liver’s function and lead to an accumulation of bilirubin in the blood.
Liver and Gallbladder Disorders
Jaundice can also be caused by liver or gallbladder disorders in newborns. These disorders can impair the liver’s ability to process bilirubin, resulting in its accumulation in the blood.
Metabolic Disorders
In rare cases, metabolic disorders such as Gilbert syndrome or Crigler-Najjar syndrome can contribute to the development of jaundice in newborns. These disorders affect the liver’s ability to process bilirubin properly.
Genetic Factors
Certain genetic factors can increase the risk of jaundice in newborns. These factors can affect the baby’s liver function or the breakdown of red blood cells, leading to a higher concentration of bilirubin in the blood.
Prematurity
Premature babies are more susceptible to developing jaundice due to their underdeveloped liver function. Their immature liver may not be able to process bilirubin efficiently, leading to a build-up in the blood.

Symptoms of Jaundice in Newborns
It is important for parents and caregivers to be aware of the common symptoms of jaundice in newborns. Prompt recognition of these symptoms can help ensure timely medical intervention. The symptoms of jaundice in newborns can include:
Yellowing of the Skin and Eyes
The most noticeable symptom of jaundice is the yellowing of the baby’s skin and eyes. This yellowing, called icterus, occurs due to the accumulation of bilirubin in the blood.
Dark Urine
Jaundice can cause the baby’s urine to become darker in color. This is due to the presence of bilirubin in the urine.
Pale Stools
Stools of newborns with jaundice may appear pale or clay-colored. This is a result of reduced bilirubin excretion through the stool.
Irritability and Poor Feeding
Some babies with jaundice may become irritable and have difficulty feeding. This can be caused by the overall discomfort and fatigue associated with the condition.
Sleepiness or Lethargy
Jaundice can also cause newborns to become excessively sleepy or lethargic. This can interfere with their feeding schedule and overall well-being.
High-Pitched Crying
In some cases, newborns with jaundice may exhibit a high-pitched cry. This can be a sign of distress and should be brought to the attention of a healthcare provider.
Fever
While jaundice itself does not usually cause a fever, the underlying causes of jaundice, such as infections, can lead to an elevated body temperature.
Enlarged Liver or Spleen
In severe cases of jaundice, the baby’s liver or spleen may become enlarged. This can be detected during a physical examination by a healthcare professional.
Unusual Bleeding or Bruising
In rare cases, jaundice may be accompanied by unusual bleeding or bruising. This can be a sign of a more serious underlying condition and should be evaluated by a healthcare provider.
Difficulty Gaining Weight
Infants with jaundice may have difficulty gaining weight. This can be attributed to the fatigue and irritability caused by the condition, which can impact their feeding habits.
Complications of Jaundice in Newborns
While most cases of jaundice in newborns are mild and resolve on their own, there are potential complications that can arise in more severe cases. It is important to be aware of these complications and seek medical attention if necessary. Complications of jaundice in newborns can include:
Kernicterus
Kernicterus is a rare but serious complication of severe jaundice. It occurs when the build-up of bilirubin in the brain causes neurological damage. Kernicterus can result in long-term cognitive and movement disabilities.
Acute Bilirubin Encephalopathy
Acute bilirubin encephalopathy is a condition characterized by bilirubin toxicity in the brain. This can lead to significant neurological damage and can be life-threatening if left untreated.
Long-Term Neurological Damage
Severe or prolonged jaundice can cause long-term neurological damage in newborns. This can manifest as developmental delays, cognitive impairments, or movement disorders.
Hearing Loss
In some cases, severe jaundice can lead to permanent hearing loss. Early detection and treatment are crucial in preventing this complication.
Developmental Delays
If jaundice is not properly managed, it can contribute to developmental delays in newborns. Prompt treatment and follow-up care are essential in minimizing the risk of such delays.
Death
In rare cases, severe untreated jaundice can lead to death. This underscores the importance of early detection and timely medical intervention.

Prevalence of Jaundice in Newborns
Jaundice is a relatively common condition among newborns around the world. The prevalence of jaundice can vary depending on various factors.
Global Prevalence
Globally, it is estimated that approximately 60% of full-term newborns and 80% of premature infants develop jaundice within the first week of life. The prevalence of jaundice may be influenced by factors such as genetics, ethnic background, and healthcare access.
Prevalence in the United States
In the United States, jaundice is one of the most common conditions observed among newborns. It is estimated that around 60% of term infants and 80% of preterm infants develop jaundice.
Ethnic and Racial Differences
Certain ethnic groups may have a higher prevalence of jaundice. For example, babies of East Asian or Mediterranean descent have been found to have a higher risk of developing jaundice.
Gender Differences
Although jaundice can affect both male and female newborns, studies have shown that male infants may have a slightly higher risk of developing significant jaundice. The reasons for this gender difference are not entirely understood and require further research.
Risk Factors for Jaundice in Newborns
While jaundice can occur in any newborn, certain risk factors increase the likelihood of its development. It is important for parents and caregivers to be aware of these risk factors and take appropriate steps to monitor and manage their baby’s health. Common risk factors for jaundice in newborns include:
Prematurity
Premature infants are at a higher risk of developing jaundice due to their underdeveloped liver function. Immature livers may not be able to adequately process bilirubin, leading to its accumulation in the blood.
Blood Type Incompatibility
If the mother has a different blood type than the baby, such as Rh or ABO incompatibility, there is an increased risk of jaundice. Incompatibility can lead to the destruction of red blood cells, resulting in a higher concentration of bilirubin.
Previous Sibling with Jaundice
If a previous sibling had jaundice, there is a higher chance of subsequent babies developing the condition. This suggests a potential genetic predisposition.
East Asian or Mediterranean Descent
Babies of East Asian or Mediterranean descent have a higher risk of developing jaundice. This may be due to genetic factors or variations in the breakdown of red blood cells.
Breastfeeding Issues
Breastfeeding-related factors, such as insufficient milk supply or poor latch, can contribute to the development of jaundice in newborns. These issues can impact the baby’s feeding and overall bilirubin elimination.
Bruising or Trauma at Birth
Babies who experience significant bruising or trauma during birth may be at an increased risk of developing jaundice. This is due to the breakdown of red blood cells as a result of the trauma.
Infection During Pregnancy
Certain infections during pregnancy can increase the risk of jaundice in newborns. Infections can disrupt the baby’s liver function and overall health.
Rh or ABO Incompatibility
Incompatibility between the mother’s blood type and the baby’s blood type can lead to an increased risk of jaundice. This is because the mother’s immune system may produce antibodies that destroy the baby’s red blood cells.
Cephalohematoma
Cephalohematoma, a collection of blood beneath the scalp, can increase the risk of jaundice in newborns. The breakdown of blood cells within the cephalohematoma can lead to elevated levels of bilirubin.
Maternal Factors
Certain maternal factors, such as diabetes or gestational hypertension, can increase the risk of jaundice in newborns. These conditions can impact the baby’s overall health and liver function.
When to Seek Medical Help
It is important to know when to seek medical help if you suspect your newborn may have jaundice. While mild jaundice can be a normal part of a newborn’s adjustment, certain signs and symptoms warrant prompt medical attention. You should seek medical help if you notice:
Yellowing of Skin or Eyes
If your baby’s skin or eyes appear yellow, it is important to contact your healthcare provider. This yellowing, known as jaundice, can be an indication of elevated bilirubin levels.
Changes in Feeding Habits
If your baby is not feeding well or is displaying feeding difficulties, it is important to consult with a healthcare provider. Feeding issues can be a sign of an underlying problem, such as jaundice.
Lack of Weight Gain
If your baby is not gaining weight or is losing weight, it is essential to seek medical attention. Poor weight gain can be a sign of inadequate feeding or an underlying health issue, including jaundice.
Frequent Sleepiness
Excessive sleepiness or lethargy in newborns can be a cause for concern. If your baby is overly sleepy, it can be a sign of jaundice or other health issues that require medical evaluation.
High-Pitched Crying
If your newborn has a high-pitched cry that is unusual or persistent, it is important to consult with a healthcare provider. This can be a sign of distress or discomfort, including jaundice.
Fever
While jaundice itself does not typically cause a fever, certain underlying causes, such as infections, can lead to an elevated body temperature. If your baby has a fever, it is important to seek medical attention.
Unusual Bleeding or Bruising
Unusual bleeding or bruising in a newborn should not be ignored. These symptoms can indicate an underlying health condition, including jaundice or a bleeding disorder, and require medical evaluation.
Navel or Penis with Yellow Discharge
If you notice any yellow discharge from your baby’s navel or penis, it is crucial to contact your healthcare provider. This can be a sign of infection or jaundice-related complications.
Pale Stools or Dark Urine
Stools that appear pale or clay-colored, along with dark urine, can be signs of jaundice. It is important to discuss these symptoms with your healthcare provider.
Enlarged Liver or Spleen
If you notice that your baby’s abdomen appears enlarged or feel any lumps in the area of the liver or spleen, it is important to consult with a healthcare provider. Enlarged organs can be a sign of underlying health issues, including jaundice.
Diagnosing Jaundice in Newborns
If jaundice is suspected in a newborn, a healthcare provider will conduct a series of tests and evaluations to confirm the diagnosis and determine the underlying causes. The diagnostic process may include:
Physical Examination
During a physical examination, the healthcare provider will assess the baby’s skin color, eyes, abdomen, and overall well-being. They may also check for signs of liver or spleen enlargement.
Blood Tests
Blood tests are commonly performed to measure the levels of bilirubin in the baby’s blood. These tests can help determine the severity of jaundice and guide the appropriate treatment.
Measuring Bilirubin Levels
Bilirubin levels will be measured using blood tests. The results will help determine if the bilirubin levels are within the normal range or if they indicate jaundice.
Assessing Liver Function
Liver function tests may be conducted to evaluate the baby’s liver function. These tests can help identify any underlying liver disorders that may contribute to jaundice.
Other Diagnostic Techniques
In some cases, additional diagnostic techniques may be used to further evaluate the baby’s condition. These techniques may include imaging studies, such as ultrasound or MRI, to assess the liver and gallbladder.

Treatment Options for Jaundice in Newborns
The treatment options for jaundice in newborns depend on the underlying causes and the severity of the condition. In most cases, simple interventions and close monitoring are sufficient. Treatment options for jaundice in newborns may include:
Phototherapy
Phototherapy is a common treatment for jaundice in newborns. It involves exposing the baby’s skin to specific wavelengths of light that help break down bilirubin. Phototherapy can be administered through special lights or light-emitting pads.
Exchange Transfusion
In severe cases of jaundice, where the bilirubin levels are dangerously high, an exchange transfusion may be necessary. This involves replacing the baby’s blood with fresh blood from a donor to remove excess bilirubin.
Medication Treatment
In certain cases, medication may be prescribed to help lower bilirubin levels or treat underlying conditions that contribute to jaundice. These medications should be administered under the guidance of a healthcare professional.
Fluid Therapy
In some cases, intravenous fluids may be administered to newborns with jaundice to ensure adequate hydration and support liver function.
Nutritional Support
Proper nutrition is essential for newborns with jaundice. In cases of breastfeeding jaundice, ensuring proper breastfeeding techniques and increasing milk supply can help resolve the condition.
Surgery (in severe cases)
In rare cases, surgical intervention may be required to treat underlying liver or gallbladder disorders that contribute to jaundice. These surgeries are typically performed by specialists in pediatric surgery.
Follow-Up Care
Follow-up care is crucial for newborns with jaundice to monitor their progress and ensure proper management. Regular check-ups and ongoing monitoring of bilirubin levels are important to track the baby’s response to treatment.
Preventing Jaundice in Newborns
While jaundice is a common condition among newborns, there are steps that can be taken to reduce the risk and severity of jaundice. Preventive measures for jaundice in newborns may include:
Ensuring Adequate Feeding
Promoting proper feeding techniques and ensuring that newborns receive sufficient breast milk or formula can help prevent jaundice caused by breastfeeding issues.
Managing Risk Factors
If you are aware of certain risk factors that can contribute to jaundice, such as blood type incompatibility or previous siblings with jaundice, it is important to discuss these factors with your healthcare provider. Monitoring and early intervention can help prevent or minimize the severity of jaundice.
Early Detection and Intervention
Regular check-ups and newborn screenings can help detect jaundice at an early stage. Early detection allows for timely intervention, preventing complications and ensuring proper treatment.
Providing Skin-to-Skin Contact
Skin-to-skin contact between the mother and baby can help promote breastfeeding and overall bonding. This can aid in establishing proper feeding habits and reducing the risk of breastfeeding-related jaundice.
Managing Infections
Taking steps to prevent infections during pregnancy, such as practicing good hygiene and seeking timely medical care, can help reduce the risk of jaundice caused by infections.
Monitoring Bilirubin Levels
In some cases, monitoring bilirubin levels at home may be recommended. This can help detect any changes or indications of jaundice that require medical attention.
Long-Term Outlook and Follow-Up Care
Most cases of jaundice in newborns are mild and resolve within a few weeks without any long-term complications. However, some newborns may require long-term follow-up care to monitor their progress and ensure their healthy development. Long-term outlook and follow-up care for jaundice may include:
Monitoring Bilirubin Levels
Regular monitoring of bilirubin levels may be necessary to ensure that they return to normal and to detect any recurring or persistent jaundice.
Developmental Assessment
Developmental assessments help evaluate the baby’s cognitive and physical development. This can help identify any delays or impairments associated with severe jaundice.
Hearing Screening
Hearing screenings are recommended for newborns to detect any hearing loss associated with jaundice. Early intervention can help minimize the impact of hearing loss on the baby’s development.
Neurological Evaluation
In severe cases of jaundice, a neurological evaluation may be conducted to assess the baby’s brain function and identify any long-term damage.
Early Intervention Services
If developmental delays or impairments are identified, early intervention services may be recommended. These services provide specialized support and therapy to help the baby reach their developmental milestones.
Support for Parents and Caregivers
Caring for a newborn with jaundice can be challenging, both emotionally and physically. It is important to seek support from healthcare providers, support groups, and loved ones to ensure proper care and address any concerns or questions.
In conclusion, understanding jaundice in newborns is crucial for parents and caregivers. By familiarizing themselves with the causes, symptoms, complications, treatment options, preventive measures, and long-term outlook of jaundice, they can provide the necessary care and support to their newborns. Prompt medical attention, regular check-ups, and ongoing monitoring play a vital role in ensuring the well-being of newborns with jaundice.