In this article, we will explore key considerations for nursing management of croup, a common respiratory infection in children. We will delve into the important nursing considerations and management techniques that can help provide optimal care for children with croup. From recognizing early signs and symptoms to implementing proper interventions, this article aims to equip nurses with valuable knowledge to effectively manage this condition and ensure the well-being of their young patients. So, let’s explore the essential guidelines for nursing management of croup and discover the ways in which nurses can play a crucial role in providing quality care.

Assessment and Diagnosis of Croup
Clinical Presentation
When assessing a child with croup, you will typically observe common clinical features. These may include a barking cough, stridor, and hoarseness. The child may also exhibit signs of respiratory distress, such as increased work of breathing, retractions, and nasal flaring. Assessing the child’s overall appearance, including their color, level of consciousness, and ability to speak or cry, is crucial in determining the severity of their condition.
Diagnostic Criteria
Diagnosing croup is primarily based on clinical presentation and a thorough history. However, certain diagnostic criteria can aid in confirming the diagnosis. For instance, a radiograph of the neck may reveal the characteristic “steeple sign,” which indicates narrowing of the airway due to subglottic swelling. Lab tests, such as a complete blood count (CBC), are generally not necessary but may be performed if the child’s condition is severe or if there is a concern for bacterial infection.
Differential Diagnosis
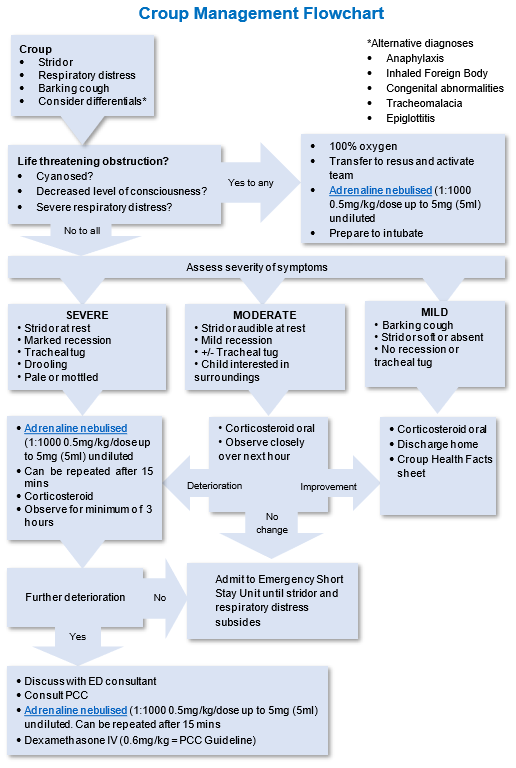
It is essential to differentiate croup from other conditions with similar symptoms. Some possible differentials to consider include epiglottitis, foreign body aspiration, acute asthma exacerbation, and bacterial tracheitis. Evaluating the child’s clinical presentation, past medical history, and any potential triggers can help identify the underlying cause and guide appropriate management.
Monitoring and Observation
Respiratory Assessment
Continuous respiratory monitoring is crucial in managing a child with croup. Assess the child’s respiratory rate, depth, and effort. Observe for any signs of worsening respiratory distress, such as increased retractions, decreased air entry, or cyanosis. Regular auscultation of lung sounds can provide further insight into the status of the child’s airway and lung function.
Signs of Respiratory Distress
Recognizing signs of respiratory distress is vital in promptly addressing any worsening of the child’s condition. These signs may include increased work of breathing, such as nasal flaring, use of accessory muscles, and intercostal retractions. Stridor at rest or with minimal exertion is also indicative of significant airway narrowing and should be closely monitored.
Vital Signs Monitoring
Regularly monitoring the child’s vital signs, including heart rate, blood pressure, and oxygen saturation, is essential for evaluating their overall clinical status. Changes in vital signs, such as tachycardia, hypertension, and hypoxemia, may suggest worsening respiratory distress or the need for further interventions.

Medical Interventions
Nebulized Epinephrine
Nebulized epinephrine is often used as a first-line treatment for croup due to its vasoconstrictive properties. It helps reduce airway swelling and improve symptoms. As a nurse, you will administer nebulized epinephrine according to the healthcare provider’s orders, ensuring proper dosing and monitoring the child’s response. It is important to educate the parents or caregivers on the potential side effects, such as increased heart rate and anxiety, and provide reassurance that these effects are typically transient.
Systemic Steroids
Systemic steroids, such as dexamethasone, play a crucial role in managing croup. These medications help reduce inflammation and swelling in the airway, thereby improving symptoms. As a nurse, you will administer systemic steroids as ordered and monitor for potential side effects, such as hyperglycemia or gastrointestinal upset. Educate the parents or caregivers about the importance of completing the full course of steroids and the expected timeline for improvement.
Cool Mist Humidification
Cool mist humidification is a non-invasive intervention that can help alleviate croup symptoms. It works by providing moisture to the air, which can help soothe the child’s inflamed airway and decrease coughing. Ensure that the cool mist humidifier is properly cleaned and set up in the child’s room. Educate parents or caregivers on the appropriate use of humidification and the importance of regular cleaning to prevent the growth of mold or bacteria.
Maintaining Airway Patency
Positioning
Proper positioning is essential in maintaining optimal airway patency in a child with croup. Elevating the head of the bed or using pillows to elevate the child’s upper body can help alleviate symptoms by promoting drainage of secretions and reducing airway obstruction. Encourage the child to remain in a comfortable position that allows for easy breathing, and educate the parents or caregivers on the importance of maintaining appropriate positioning throughout the day and during sleep.
Suctioning
Suctioning may be necessary in cases where there is excessive secretions or mucus obstructing the airway. As a nurse, you may perform suctioning using appropriate equipment and techniques, following infection control guidelines. Ensure that you maintain a calm and reassuring approach to minimize the child’s distress during the suctioning procedure. Educate parents or caregivers on signs that may indicate the need for suctioning and provide clear instructions on how to perform basic suctioning at home, if appropriate.
Administration of Oxygen
In severe cases of croup, oxygen supplementation may be required to maintain adequate oxygenation. As a nurse, you will monitor the child’s oxygen saturation levels closely and administer supplemental oxygen as ordered. Ensure proper placement and functioning of the oxygen delivery system, and provide education to parents or caregivers on the signs that may indicate the need for supplemental oxygen at home.
Promoting Comfort and Rest
Frequent Rest
Rest is essential for a child with croup to allow for recovery and conserve energy. Encourage parents or caregivers to provide a calm and quiet environment conducive to rest and sleep. Help establish a consistent sleep schedule, and educate them on the importance of allowing the child to rest as needed, even during the day.
Provide Comfort Measures
Providing comfort measures can help relieve the child’s discomfort associated with croup. Encourage the child to stay hydrated by offering small, frequent sips of fluids. Cold fluids, such as ice chips or popsicles, may help soothe the child’s sore throat. Additionally, offering comforting activities, such as reading a favorite book or engaging in quiet play, can help distract the child from their symptoms and promote a sense of well-being.
Importance of Fluids
Maintaining proper hydration is crucial for a child with croup, especially if they have a fever or increased respiratory effort. Educate parents or caregivers on the importance of offering fluids regularly, even if the child does not feel like drinking. Promote the use of clear liquids, such as water, diluted fruit juices, or electrolyte solutions, to replenish fluids lost through increased respiratory efforts and fever.
Supporting Parental Education
Explanation of Croup
As a nurse, it is essential to provide parents or caregivers with a clear explanation of croup, its causes, and expected course of the illness. Explain that croup is typically caused by a viral infection and that the symptoms are due to inflammation and swelling of the upper airway. Provide reassurance that croup is usually a self-limiting condition and that most children recover fully within a few days to a week.
Home Management Strategies
Educate parents or caregivers on home management strategies to support their child’s recovery and prevent complications. Emphasize the importance of maintaining a calm and supportive environment, implementing appropriate positioning techniques, and utilizing comfort measures, such as humidification. Instruct them on the proper administration of medications, including timing and dosing, and highlight the significance of completing the full course of prescribed medications.
Recognition of Signs
It is crucial for parents or caregivers to recognize signs that may indicate a worsening condition or the development of complications. Educate them on the signs of increased respiratory distress, such as increased work of breathing, persistent stridor, or decreased responsiveness. Instruct them to seek immediate medical attention if these signs occur or if the child’s condition deteriorates despite home management strategies.

Preventing Complications
Identification of High-risk Cases
Identifying high-risk cases of croup is key in preventing complications. Some children, such as those with underlying respiratory conditions or those who are immunocompromised, may be at a higher risk of developing severe croup or complications. As a nurse, ensure a thorough assessment of the child’s medical history and clinical presentation to identify any risk factors that may require additional interventions or close monitoring.
Prompt Referral for Advanced Care
In cases where the child’s condition worsens or fails to improve with conservative management, it is crucial to promptly refer them for advanced care. This may involve consulting with a pediatrician or seeking care in an emergency department. Timely referral ensures that the child receives appropriate interventions, such as nebulized epinephrine, systemic steroids, or more intensive respiratory support, if needed.
Preventing Secondary Infections
Children with croup are at an increased risk of developing secondary respiratory infections, such as pneumonia. Promote good hand hygiene practices, both for the child and the caregivers, to minimize the risk of spreading or acquiring additional infections. Educate parents or caregivers on the importance of appropriate cough etiquette and respiratory hygiene to prevent the spread of respiratory droplets.
Collaboration with Healthcare Team
Interdisciplinary Communication
Collaboration with the healthcare team is crucial in managing a child with croup effectively. Maintain open and clear communication with other healthcare professionals involved in the child’s care, such as pediatricians, respiratory therapists, and other nurses. Share relevant information, such as changes in the child’s clinical status, response to interventions, or concerns regarding their overall well-being.
Involvement of Respiratory Therapists
Respiratory therapists play a vital role in managing the airway and providing specific interventions for children with croup. Collaborate with respiratory therapists to ensure appropriate administration of nebulized medications, including epinephrine, and to monitor the child’s response. Seek their expertise in managing acute respiratory distress and addressing any complications that may arise.
Consultation with Pediatrician
Consultation with a pediatrician is essential in managing croup, particularly in cases where the child’s condition is severe or fails to improve with initial interventions. Collaborate with a pediatrician to discuss the child’s clinical course, review diagnostic findings, and determine the appropriate medical management. Seek guidance regarding the need for additional interventions, such as hospitalization or specialist referral, based on the child’s individual needs.
Documentation and Reporting
Accurate and Timely Documentation
Accurate and timely documentation is necessary to ensure continuity of care and effective communication among healthcare providers. Document the child’s clinical presentation, vital signs, assessment findings, and interventions implemented. Include details regarding the child’s response to interventions and any changes in their condition that may require further interventions or consultations.
Reporting to Healthcare Providers
Regularly report the child’s progress and any concerns to the healthcare providers involved in their care. Provide them with concise and relevant information, such as changes in the child’s clinical status or the need for additional interventions. Keep them informed about the child’s response to treatments and any challenges encountered during the course of care.
Communication Handoffs
During shift changes or handoffs, ensure effective communication of essential information to the incoming nurse or healthcare provider. Provide a comprehensive report that includes the child’s history, current interventions, response to treatments, and any pending actions or follow-up required. Promote clear and concise communication to facilitate safe and efficient care continuity.
Evaluation and Follow-up
Assessing Response to Interventions
Continuous evaluation of the child’s response to interventions is crucial in determining the effectiveness of the management plan. Monitor the child’s respiratory status, vital signs, and overall clinical progress regularly. Assess for improvements in symptoms, such as decreased stridor, resolution of cough, and improved work of breathing. If the child’s condition fails to improve or worsens, reassess the management plan and involve the healthcare team for further guidance.
Evaluation of Airway Patency
Evaluate the child’s airway patency regularly by assessing for the presence of stridor at rest or with minimal exertion. Auscultate lung sounds to ensure adequate air entry. Monitor for signs of respiratory distress or increased work of breathing. If there are concerns regarding the child’s airway patency, promptly intervene and involve the healthcare team for further evaluation and intervention.
Post-hospital Discharge Instructions
When preparing a child for discharge, ensure proper education on home management strategies, including medication administration, comfort measures, and follow-up care. Provide clear instructions regarding when to seek medical attention, such as persistent or worsening symptoms, high fever, or severe respiratory distress. Emphasize the importance of completing the full course of prescribed medications and attending any scheduled follow-up appointments with the pediatrician.