If you or a loved one has been diagnosed with Crohn’s Disease, you’ll be pleased to know that there have been significant breakthroughs in treatment options. In this article, we’ll explore the latest research and advancements that are offering hope for those living with Crohn’s Disease. From new medications to innovative therapies, the medical community is making great strides in improving the quality of life for individuals affected by this chronic inflammatory condition. Whether you’re seeking alternative treatments or simply curious about the latest discoveries, this article will provide you with valuable insights into the ever-evolving world of Crohn’s Disease treatment.

1. Overview of Crohn’s Disease
Crohn’s Disease is a chronic inflammatory bowel disease that affects the digestive tract. It is characterized by inflammation and ulceration in various parts of the gastrointestinal tract, most commonly the small intestine and the colon. This condition can cause a range of symptoms, including diarrhea, abdominal pain and cramping, fatigue, weight loss, and reduced appetite. Crohn’s Disease can also lead to complications such as strictures (narrowing of the intestines), fistulas (abnormal tunnels between organs), and abscesses.
1.1 Definition and prevalence
Crohn’s Disease is an autoimmune disorder, which means that the body’s immune system mistakenly attacks its own healthy cells in the digestive tract, leading to inflammation. While the exact cause of Crohn’s Disease is still unclear, researchers believe that factors such as genetics, environmental triggers, and an overactive immune response play a role in its development.
The prevalence of Crohn’s Disease varies across different regions of the world, with higher rates reported in Western countries. It is estimated that approximately 1.3 million people in the United States are living with this condition. Crohn’s Disease can affect individuals of any age, but it commonly first appears in adolescents and young adults.
1.2 Symptoms and complications
The symptoms of Crohn’s Disease can vary from person to person and may change over time. Common symptoms include persistent diarrhea, abdominal pain and cramping, fatigue, unintended weight loss, reduced appetite, and rectal bleeding. Additionally, some individuals may experience extraintestinal symptoms such as joint pain, skin problems, and eye inflammation.
Crohn’s Disease can lead to various complications that can significantly impact a person’s quality of life. Strictures can develop as a result of long-term inflammation, causing the intestines to become narrowed and leading to bowel obstruction. Fistulas, which are abnormal connections between different parts of the intestine or between the intestine and other organs, can also occur. These can cause pain, infection, and the passage of stool or mucus through unusual routes. Abscesses, or pus-filled pockets, may develop due to inflammation, leading to further complications if left untreated.
2. Diagnosis of Crohn’s Disease
Early and accurate diagnosis of Crohn’s Disease is crucial in order to initiate appropriate treatment and prevent complications. Diagnosis typically involves a combination of medical history evaluation, physical examination, and diagnostic tests.
2.1 Initial evaluation
During the initial evaluation, your healthcare provider will review your medical history and symptoms, as well as perform a physical examination. They may ask questions about your diet, bowel habits, and family history of inflammatory bowel disease. It is important to provide thorough and honest information, as this will help guide the diagnostic process.
2.2 Diagnostic tests
Various diagnostic tests may be ordered to confirm the presence of Crohn’s Disease and to assess the extent and severity of the condition. These include:
-
Blood tests: Blood tests can help evaluate your overall health, check for signs of inflammation, and assess nutritional deficiencies. They may include a complete blood count (CBC), C-reactive protein (CRP), and erythrocyte sedimentation rate (ESR).
-
Stool sample analysis: Analyzing a stool sample can help identify potential infections or signs of inflammation in the digestive tract.
-
Imaging tests: Imaging techniques such as X-rays, computed tomography (CT) scans, magnetic resonance imaging (MRI), and ultrasound may be used to visualize the gastrointestinal tract and detect structural abnormalities, inflammation, or complications.
-
Endoscopy and biopsy: Endoscopic procedures, such as colonoscopy or upper endoscopy, involve the insertion of a flexible tube with a camera into the gastrointestinal tract. This allows your doctor to directly visualize the lining of the intestines and collect tissue samples (biopsies) for further examination under a microscope.

3. Traditional Treatment Approaches
The treatment of Crohn’s Disease typically involves a combination of medications, surgery, and lifestyle modifications. The main goals of treatment are to reduce inflammation, relieve symptoms, promote healing, and prevent complications.
3.1 Medications
Medications play a key role in managing Crohn’s Disease and controlling inflammation. The choice of medication depends on the severity of the disease and the specific symptoms and complications experienced by the individual. Common medications used for Crohn’s Disease include:
-
Aminosalicylates: These medications help reduce inflammation in the intestine and are often used to treat mild to moderate cases of Crohn’s Disease.
-
Corticosteroids: Corticosteroids are potent anti-inflammatory drugs that can provide short-term relief from symptoms. They are typically used for short periods due to their potential side effects.
-
Immune modifiers: These medications work by suppressing the immune system to reduce inflammation. They are often used for individuals who do not respond to other treatments or who require long-term maintenance therapy.
3.2 Surgery
Surgery may be recommended for individuals with severe symptoms, complications, or when medication and lifestyle modifications do not provide adequate relief. The specific surgical approach depends on the location and extent of the disease. Surgery aims to remove affected segments of the intestine, repair fistulas or strictures, or drain abscesses. In some cases, a temporary or permanent ostomy (an opening on the abdomen to divert waste) may be created.
3.3 Lifestyle modifications
In addition to medication and surgery, certain lifestyle modifications can help manage Crohn’s Disease and improve overall well-being. These include:
-
Dietary changes: Some individuals find that certain foods can trigger or worsen their symptoms. Keeping a food diary can help identify potential triggers, and working with a registered dietitian can help develop a personalized diet plan.
-
Stress management: Stress and anxiety can exacerbate symptoms of Crohn’s Disease. Engaging in stress-reducing activities such as mindfulness, meditation, yoga, or regular exercise can help manage stress levels.
-
Smoking cessation: Smoking has been shown to worsen symptoms and increase the risk of complications in individuals with Crohn’s Disease. Quitting smoking can have significant benefits for overall health and disease management.
4. Advances in Crohn’s Disease Treatment
Research and medical advancements have led to the development of new treatment approaches for Crohn’s Disease. These advances aim to provide more targeted and effective therapies, improve outcomes, and enhance the quality of life for individuals living with this condition.
4.1 Biologic therapies
Biologic therapies are a type of medication that targets specific proteins involved in the immune response. These medications help reduce inflammation and are used for individuals with moderate to severe Crohn’s Disease who do not respond well to other treatments. Biologics are typically administered through injection or intravenous infusion and work by blocking the action of proteins such as tumor necrosis factor-alpha (TNF-alpha) or integrins.
4.2 Targeted therapies
Targeted therapies are a newer class of medications that focus on specific molecules or pathways involved in the development and progression of Crohn’s Disease. They aim to modify the immune response and reduce inflammation. Examples of targeted therapies include Janus kinase (JAK) inhibitors and sphingosine-1-phosphate receptor modulators.
4.3 Stem cell therapies
Stem cell therapies are an exciting area of research that holds promise for the treatment of Crohn’s Disease. These therapies involve the use of stem cells to repair damaged tissues and modulate the immune response. Clinical trials are currently underway to evaluate the safety and efficacy of stem cell therapies in Crohn’s Disease.
4.4 Fecal microbiota transplantation
Fecal microbiota transplantation (FMT) is a procedure that involves transferring the fecal matter from a healthy donor into the gastrointestinal tract of a person with Crohn’s Disease. This procedure aims to restore the balance of gut bacteria and improve symptoms. While FMT has shown promise in certain cases, further research is needed to better understand its benefits and risks.

5. Nutritional Approaches for Crohn’s Disease
Dietary interventions can play a significant role in managing Crohn’s Disease and reducing symptoms. While there is no one-size-fits-all approach, several nutritional approaches have shown promise in the management of this condition.
5.1 Exclusive enteral nutrition
Exclusive enteral nutrition (EEN) involves consuming a liquid diet that provides all the necessary nutrients while giving the intestines a rest. This approach has been shown to induce remission and promote healing in children and adolescents with Crohn’s Disease. EEN may also be used in combination with other treatments for adults.
5.2 Specific carbohydrate diet
The specific carbohydrate diet (SCD) is a restrictive diet that eliminates complex carbohydrates and focuses on easily digestible foods. The goal is to reduce bacterial overgrowth and inflammation in the gut. While there is limited scientific evidence supporting the effectiveness of SCD in Crohn’s Disease, some individuals report symptom improvement with this dietary approach.
5.3 Elemental diet
Elemental diet involves consuming liquid formulas that contain predigested nutrients. This approach aims to provide complete nutrition while minimizing the workload on the digestive system. Elemental diets are typically used for short periods to induce remission in individuals with severe Crohn’s Disease.
6. Complementary and Alternative Therapies
In addition to conventional treatments, many individuals with Crohn’s Disease explore complementary and alternative therapies to manage symptoms and improve their quality of life. While these therapies may not replace traditional medical treatments, they can be used as adjunctive approaches to support overall well-being.
6.1 Probiotics and prebiotics
Probiotics are live bacteria that can promote a healthy balance of gut bacteria, while prebiotics are fibers that nourish the beneficial bacteria in the gut. Some studies suggest that certain strains of probiotics may help reduce inflammation and improve symptoms in individuals with Crohn’s Disease. However, more research is needed to determine the specific strains and dosages that are most effective.
6.2 Acupuncture
Acupuncture is an ancient Chinese practice that involves the insertion of thin needles into specific points on the body. It is believed to help promote the flow of energy and restore balance. While acupuncture has been studied for its potential benefits in inflammatory bowel disease, including Crohn’s Disease, the evidence is limited and conflicting. Some individuals may find acupuncture helpful for symptom management, but it should be used in conjunction with conventional treatments.
6.3 Herbal supplements
Certain herbal supplements, such as aloe vera, Boswellia serrata, and turmeric, have been studied for their potential anti-inflammatory properties and may be considered as adjunctive therapies for individuals with Crohn’s Disease. However, it is important to consult with a healthcare provider before starting any herbal supplements, as they can interact with medications and may not be suitable for everyone.
7. Personalized Medicine for Crohn’s Disease
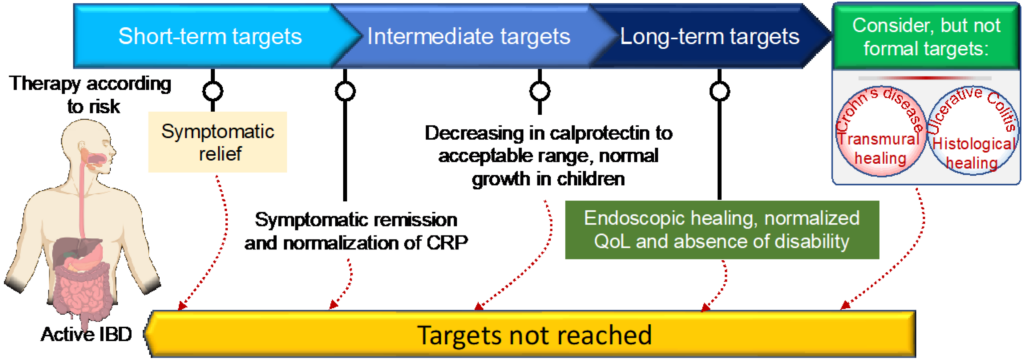
Advancements in genetics and biomarker research have paved the way for personalized medicine in the management of Crohn’s Disease. Personalized medicine aims to tailor treatments based on an individual’s unique genetic and biomarker profiles, allowing for more targeted and effective therapies.
7.1 Genetics and biomarkers
Genetic factors play a role in the development and progression of Crohn’s Disease. Certain genetic variations have been associated with an increased risk of developing this condition and can influence the response to different treatments. Biomarkers, such as blood markers of inflammation or genetic markers, can help predict disease activity and guide treatment decisions.
7.2 Pharmacogenomics
Pharmacogenomics is the study of how an individual’s genetics influence their response to medications. By analyzing genetic variations, healthcare providers can identify the most suitable medication and dosage for a particular individual. This personalized approach can help optimize treatment outcomes and minimize side effects.
7.3 Individualized treatment plans
Personalized medicine allows for the development of individualized treatment plans that take into account a person’s unique characteristics, such as their genetics, biomarkers, and disease phenotype. By tailoring treatments to each individual, healthcare providers can optimize therapeutic outcomes and improve long-term disease management.
8. Surgery Advancements in Crohn’s Disease
Surgery has long been a part of the treatment approach for Crohn’s Disease, and advancements in surgical techniques have improved outcomes and reduced the need for extensive resection of the intestines.
8.1 Minimally invasive techniques
Minimally invasive surgical techniques, such as laparoscopic or robotic-assisted surgery, have revolutionized the field of Crohn’s Disease surgery. These approaches involve making small incisions and using specialized instruments to perform the surgery, resulting in less scarring, reduced pain, and faster recovery times compared to traditional open surgery.
8.2 Enhanced recovery after surgery (ERAS)
Enhanced recovery after surgery (ERAS) protocols are multimodal approaches designed to optimize a patient’s preoperative, intraoperative, and postoperative experience. ERAS focuses on minimizing surgical stress, providing optimal pain management, early nutritional support, and early mobilization. These protocols have shown promising results in improving outcomes and reducing hospital stays in individuals undergoing surgery for Crohn’s Disease.
8.3 Intestinal transplantation
Intestinal transplantation may be considered as a last resort for individuals with severe Crohn’s Disease who have exhausted all other treatment options and have significant intestinal failure. This complex procedure involves replacing the diseased intestine with a healthy donor intestine. Intestinal transplantation is a highly specialized treatment approach and is only considered in rare cases.
9. New Drug Development for Crohn’s Disease
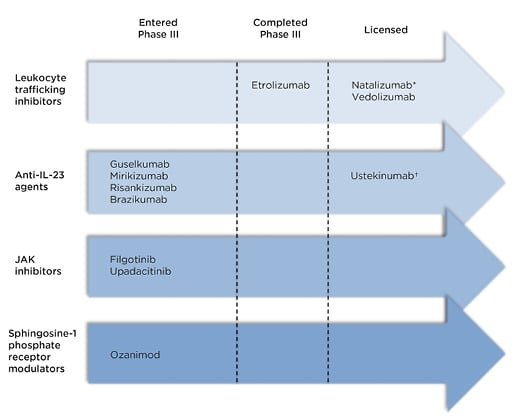
Ongoing research and clinical trials are focused on developing new drugs and treatment modalities for Crohn’s Disease. These innovations aim to provide additional options for individuals who do not respond to conventional therapies or who experience significant side effects.
9.1 Novel therapeutic targets
Researchers are actively investigating new therapeutic targets for Crohn’s Disease, aiming to identify molecules or pathways that can be targeted to reduce inflammation and promote healing. These targets may include specific immune cells, cytokines, or signaling pathways.
9.2 Drug delivery systems
Improving drug delivery systems is another area of research in Crohn’s Disease treatment. Novel approaches, such as nanoparticles and targeted drug delivery systems, are being developed to enhance the efficacy and safety of medications in the gastrointestinal tract.
9.3 Clinical trials and research
Clinical trials play a crucial role in advancing the understanding and treatment of Crohn’s Disease. These trials evaluate the safety and efficacy of new drugs, treatment approaches, and surgical techniques. Participating in a clinical trial may provide access to cutting-edge treatments and contribute to the development of future therapies for Crohn’s Disease.
10. Integrative Approaches to Crohn’s Disease Management
Integrative approaches to Crohn’s Disease management emphasize a comprehensive and holistic approach to care. These approaches recognize the importance of addressing physical, emotional, and psychosocial aspects of the disease.
10.1 Comprehensive care teams
Comprehensive care teams consist of healthcare providers from different disciplines, including gastroenterologists, surgeons, dietitians, mental health professionals, and nurses. This multidisciplinary approach ensures that individuals with Crohn’s Disease receive comprehensive care and have access to a range of expertise and support.
10.2 Psychological support
Living with a chronic condition like Crohn’s Disease can take a toll on a person’s emotional well-being. Psychological support, such as counseling or therapy, can help individuals cope with the challenges of the disease, manage stress, and improve overall mental health and quality of life.
10.3 Patient education and self-management
Patient education is a critical component of Crohn’s Disease management. Empowering individuals with knowledge about their condition, treatment options, and self-management strategies can help them take an active role in their own care. Tools such as educational materials, support groups, and self-management apps can facilitate patient education and promote self-efficacy.
In conclusion, Crohn’s Disease is a complex condition that requires a multifaceted approach to management. With advancements in research and treatment, individuals living with Crohn’s Disease have access to a wider range of options to effectively control inflammation, relieve symptoms, and improve their quality of life. It is important for individuals with Crohn’s Disease to work closely with their healthcare providers to develop a personalized treatment plan that addresses their specific needs and goals. By staying informed about the latest research and advancements in Crohn’s Disease treatment, individuals can be proactive in managing their condition and optimizing their overall well-being.