In the ever-evolving field of medical research, advancements are constantly being made to enhance our understanding and treatment of various diseases. Among these breakthroughs, new progress has emerged in the realm of liver cancer research. By uncovering novel findings and exploring innovative treatment approaches, scientists worldwide are now shaping a brighter future for those affected by this formidable disease. In this article, you will be introduced to some of the latest advancements in liver cancer research, offering a glimpse into the remarkable strides being made in combatting this complex condition.

Diagnosis of Liver Cancer
Imaging techniques
Imaging techniques play a crucial role in the diagnosis of liver cancer. In this context, doctors often rely on several imaging tests to accurately identify and assess the extent of the disease. One commonly used method is ultrasound, a non-invasive and relatively cost-effective imaging technique that uses sound waves to create images of the liver. Ultrasound can help detect the presence of tumors and determine their size and location.
Additionally, computed tomography (CT) scans are frequently employed to provide detailed cross-sectional images of the liver. These scans can help differentiate between cancerous and non-cancerous masses, as well as assess the involvement of nearby blood vessels. Magnetic resonance imaging (MRI) is another valuable tool in liver cancer diagnosis, utilizing powerful magnets and radio waves to generate detailed images of the liver’s structures and any potentially cancerous lesions.
Blood tests
Blood tests serve as an important diagnostic aid in liver cancer detection by measuring various markers and substances that can indicate the presence of the disease. For instance, alpha-fetoprotein (AFP) is a protein that can be elevated in individuals with liver cancer. Regular monitoring of AFP levels, along with other liver function tests, can provide useful information about the progression of the disease and the effectiveness of treatment.
In addition to AFP, other blood markers such as des-gamma-carboxy prothrombin (DCP) and glypican-3 (GPC3) have shown promise in contributing to the diagnosis of liver cancer. Although blood tests alone are not definitive for diagnosing liver cancer, they can serve as an initial screening tool and warrant further investigation through imaging techniques or a biopsy.
Biopsy
A biopsy is often performed to confirm the presence of liver cancer and determine its type and stage. During a biopsy, a small sample of liver tissue is obtained and examined under a microscope by a pathologist. This enables the identification of cancer cells or other abnormalities in the liver, allowing for an accurate diagnosis.
Various methods can be employed to obtain a liver tissue sample, including percutaneous needle biopsy, laparoscopic biopsy, and surgical biopsy. Percutaneous needle biopsy, the most common approach, involves using a thin needle to extract a sample of liver tissue with the guidance of imaging techniques such as ultrasound or CT scans.
Treatment Options for Liver Cancer
Surgical interventions
Surgical interventions are a crucial component of liver cancer treatment, especially in cases where the tumor is localized and has not spread extensively. The primary aim of surgery is to remove the tumor and any surrounding healthy tissue. One common surgical approach for liver cancer is liver resection, where a portion of the liver containing the tumor is surgically removed.
Liver transplantation is another surgical option for certain cases of liver cancer. This procedure involves replacing the patient’s diseased liver with a healthy liver received from a deceased or living donor. Liver transplantation is generally reserved for patients with small tumors or those with advanced disease who are not candidates for resection.
Radiofrequency ablation (RFA) is a minimally invasive procedure that uses heat to destroy liver tumors. It involves inserting a thin needle into the tumor and delivering a high-frequency electrical current that generates heat, resulting in tumor cell death.
Chemotherapy
Chemotherapy, which refers to the use of drugs to kill cancer cells, can be a valuable treatment option for liver cancer. Systemic chemotherapy involves administering medications intravenously or orally to reach cancer cells throughout the body. This approach is particularly useful when the cancer has spread beyond the liver or is inoperable.
In some cases, regional chemotherapy may be employed, focusing the delivery of chemotherapy directly to the liver. This can be achieved through techniques such as transarterial chemoembolization (TACE), which combines the administration of chemotherapy drugs with the injection of substances that block the blood supply to the tumor.
Targeted therapy
Targeted therapy is a relatively new and promising treatment approach for liver cancer. It involves using drugs that specifically target certain molecules or proteins involved in the growth and spread of cancer cells. By interfering with these specific targets, targeted therapy can inhibit the growth and survival of liver cancer cells while causing minimal damage to healthy cells.
Tyrosine kinase inhibitors (TKIs) are a type of targeted therapy commonly used in liver cancer treatment. TKIs work by blocking the action of certain proteins that promote cell growth and division in cancer cells. Monoclonal antibodies, another class of targeted therapy, can identify and bind to specific proteins on cancer cells, signaling the immune system to attack and destroy them.
Advancements in Surgical Interventions
Liver resection
Liver resection is a surgical procedure that has seen significant advancements in recent years, allowing for safer and more effective removal of liver tumors. With the advent of sophisticated imaging techniques, surgeons can better visualize the tumor and surrounding structures, aiding in accurate planning and execution of the resection.
In addition, advancements in surgical techniques, such as laparoscopic liver resection, have reduced the invasiveness of the procedure, resulting in shorter recovery times and reduced complications. These advancements have made liver resection a viable option for more patients, expanding the pool of individuals who can benefit from this potentially curative treatment.
Liver transplantation
Liver transplantation remains a complex but life-saving surgical intervention for selected patients with liver cancer. Advances in organ preservation techniques and immunosuppressive medication regimens have significantly improved the success rates and long-term outcomes of liver transplantation.
Moreover, innovations in surgical techniques, including split liver transplantation and living donor liver transplantation, have expanded the donor pool, providing more opportunities for patients in need. These advancements, coupled with stringent selection criteria for transplantation candidates, have contributed to improved patient survival rates and enhanced quality of life following transplantation.
Radiofrequency ablation
Radiofrequency ablation (RFA) has emerged as an effective minimally invasive treatment modality for liver cancer. This technique involves using radiofrequency energy to heat and destroy liver tumors. Recent advancements in RFA technology, such as the development of multiple electrode devices and real-time monitoring through imaging guidance, have enhanced treatment precision and overall effectiveness.
Furthermore, the application of RFA in combination with other treatment modalities, such as targeted therapy or chemotherapy, has shown promise in improving treatment outcomes. By combining different approaches, clinicians can optimize therapeutic efficacy and potentially achieve better long-term control of liver cancer.
Immunotherapies for Liver Cancer
Immune checkpoint inhibitors
Immune checkpoint inhibitors have revolutionized the treatment landscape for liver cancer, particularly for patients with advanced disease. These medications work by blocking specific checkpoint proteins, such as PD-1 or CTLA-4, which are responsible for suppressing the immune system’s response against cancer cells.
By inhibiting these checkpoint proteins, immune checkpoint inhibitors unleash the body’s immune response, enabling it to recognize and attack cancer cells more effectively. This approach has demonstrated remarkable results in improving overall survival rates and achieving durable responses in some patients with advanced liver cancer.
Adoptive cell transfer therapy
Adoptive cell transfer therapy, also known as CAR-T cell therapy, is an innovative and promising immunotherapy approach for liver cancer. This technique involves genetically modifying a patient’s own immune cells to express chimeric antigen receptors (CARs) that target specific proteins on cancer cells.
Once infused back into the patient’s body, these modified CAR-T cells recognize and eliminate cancer cells, leading to tumor regression. Adoptive cell transfer therapy has shown significant potential in clinical trials and offers hope for patients with advanced liver cancer who do not respond to conventional treatments.

Progress in Targeted Therapy
Tyrosine kinase inhibitors
Tyrosine kinase inhibitors (TKIs) have emerged as a key component of targeted therapy for liver cancer. These drugs work by blocking the action of certain enzymes known as tyrosine kinases, which play a crucial role in cancer cell growth and survival.
Several TKIs, such as sorafenib and lenvatinib, have been approved for the treatment of advanced liver cancer. These medications have demonstrated the ability to slow down tumor progression, improve overall survival, and delay the need for more invasive interventions. Ongoing research aims to further refine the use of TKIs and identify optimal treatment combinations to maximize their effectiveness.
Monoclonal antibodies
Monoclonal antibodies are an important class of targeted therapy for liver cancer. These antibodies are designed to bind specifically to certain proteins on cancer cells, triggering an immune response or directly interfering with cancer cell growth and survival.
Bevacizumab, a monoclonal antibody that targets vascular endothelial growth factor (VEGF), has shown efficacy in combination with chemotherapy for advanced liver cancer. Similarly, ramucirumab, another monoclonal antibody, has demonstrated significant benefits when combined with TKIs. Ongoing research into novel monoclonal antibodies holds promise for further advancements in targeted therapy for liver cancer.
Role of Nanotechnology in Liver Cancer Research
Nanoformulations for drug delivery
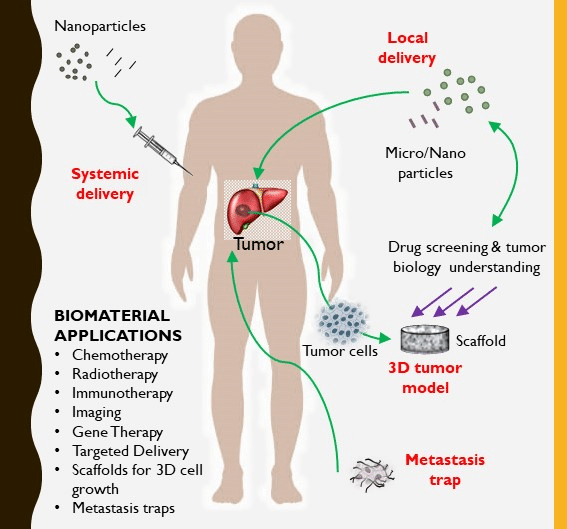
Nanotechnology has emerged as a promising field in liver cancer research, with potential applications in drug delivery systems. Nanoformulations allow for the precise encapsulation and targeted delivery of anticancer drugs to liver tumors while minimizing their systemic toxicity.
By leveraging nanoscale drug carriers, such as liposomes or nanoparticles, researchers can enhance drug stability, improve drug accumulation in tumor cells, and overcome multidrug resistance. This targeted drug delivery approach has the potential to enhance treatment outcomes and reduce adverse effects.
Nanoparticle-based imaging agents
Nanotechnology also offers innovative solutions in the field of imaging for liver cancer. Nanoparticles can be engineered to carry contrast agents, enabling enhanced imaging of liver tumors. These nanoparticle-based imaging agents can provide higher resolution and sensitivity than conventional imaging techniques, facilitating early detection and accurate staging of liver cancer.
Furthermore, nanoparticles can be designed for molecular imaging, allowing visualization of specific molecular features associated with liver cancer. This enables clinicians to assess treatment response and monitor disease progression more effectively, ultimately contributing to improved patient management.
Emerging Biomarkers for Liver Cancer
Liquid biopsies
Liquid biopsies have emerged as a promising non-invasive approach for diagnosing and monitoring liver cancer. These tests involve the analysis of various biological components, such as circulating tumor DNA (ctDNA) or microRNAs, in a patient’s blood sample.
Liquid biopsies offer several advantages over traditional tissue biopsies, including minimal invasiveness, ease of sample collection, and the ability to detect tumor heterogeneity. By identifying specific genetic alterations or molecular signatures associated with liver cancer, liquid biopsies can aid in early detection, treatment selection, and monitoring of treatment response.
Circulating tumor cells
Circulating tumor cells (CTCs) are cancer cells that detach from the primary tumor and enter the bloodstream. The analysis of CTCs holds promise as a valuable biomarker in liver cancer diagnosis and prognosis. By capturing and analyzing these cells, researchers can gain insights into the biological characteristics of the tumor and predict treatment response.
CTC enumeration and characterization can provide information about tumor aggressiveness, metastatic potential, and potential resistance to therapy. Consequently, CTC analysis may prove instrumental in guiding treatment decisions and monitoring disease progression in liver cancer patients.
Genetic Studies and Precision Medicine
Molecular profiling
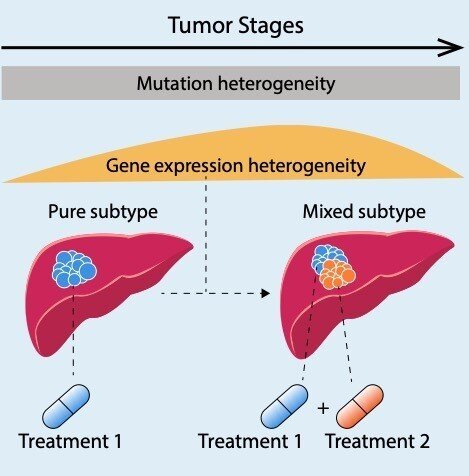
Advancements in genetic studies and molecular profiling have paved the way for precision medicine in liver cancer. The comprehensive analysis of a patient’s tumor using various molecular techniques, such as next-generation sequencing or gene expression profiling, enables the identification of specific genetic alterations driving tumor growth.
By understanding the unique molecular features of an individual’s liver cancer, clinicians can tailor treatment strategies to target specific pathways or mutations. Precision medicine holds the potential to improve treatment outcomes, minimize unnecessary side effects, and optimize therapeutic efficacy in liver cancer patients.
Personalized treatment approaches
Based on the genetic characteristics of a patient’s liver cancer, personalized treatment approaches can be developed to address their specific needs. By combining molecular profiling with knowledge of targeted therapies or immunotherapies, clinicians can select the most appropriate treatment options for each individual.
Personalized treatment approaches may involve the use of targeted therapies based on the presence of specific mutations or the availability of immunotherapies that can augment the patient’s immune response against the tumor. These tailored strategies aim to optimize treatment outcomes and improve the overall prognosis of liver cancer patients.
Combination Therapies for Liver Cancer
Sequential therapy
Sequential therapy involves the administration of different treatment modalities in a specific order, aiming to maximize their effectiveness. For example, a common approach involves using targeted therapy as an initial treatment to shrink the tumor, followed by surgical resection or transplantation to remove the remaining cancerous tissue.
Sequential therapy allows for the potential synergy of different treatment modalities, leading to improved outcomes for liver cancer patients. By combining therapies and utilizing each one’s strengths, clinicians can optimize the chances of achieving tumor control or remission.
Simultaneous therapy
Simultaneous therapy refers to the concurrent administration of multiple treatment modalities to target liver cancer from different angles. For instance, a patient may receive a combination of chemotherapy, targeted therapy, and radiation therapy to achieve a more comprehensive attack on the tumor.
The rationale behind simultaneous therapy is to enhance treatment efficacy and overcome the potential limitations of individual modalities. By utilizing each treatment’s distinct mechanisms of action and potential side effects, clinicians can optimize treatment outcomes and potentially improve patient survival rates.
Advances in Palliative Care for Liver Cancer
Symptom management
Palliative care plays a crucial role in supporting liver cancer patients by focusing on symptom management and enhancing their quality of life. Patients with advanced liver cancer often experience symptoms such as pain, fatigue, nausea, and loss of appetite. Palliative care teams work closely with patients to address these symptoms and provide personalized treatment plans.
Through the use of medications, pain management techniques, complementary therapies, and psychological support, palliative care specialists aim to alleviate distressing symptoms and improve the overall well-being of patients. This holistic approach ensures that patients receive the necessary support to navigate the challenges associated with liver cancer.
Psychosocial support
Living with liver cancer can have a significant emotional and psychological impact on patients and their families. Psychosocial support in palliative care focuses on addressing the emotional, social, and spiritual needs of patients.
Counseling, support groups, and therapy sessions can help patients and their families cope with the emotional upheaval that often accompanies a liver cancer diagnosis. By providing a safe and nurturing environment, psychosocial support enables patients to express their concerns, fears, and hopes and receive guidance and reassurance throughout their cancer journey.
End-of-life care
End-of-life care encompasses the provision of compassionate and dignified care to patients with advanced liver cancer who are approaching the end of their lives. This aspect of palliative care focuses on ensuring comfort, minimizing suffering, and promoting a peaceful transition.
End-of-life care includes symptom management, emotional support for patients and their families, spiritual guidance, and assistance with advance care planning and decision-making. By providing comprehensive and compassionate end-of-life care, palliative care teams aim to honor the wishes of patients and support their loved ones during this difficult time.
In conclusion, the field of liver cancer research has witnessed significant advancements in various areas, including diagnosis, treatment options, immunotherapy, targeted therapy, nanotechnology, biomarker identification, genetic studies, combination therapies, and palliative care. These advancements offer hope for improving the diagnosis, treatment outcomes, and overall quality of life for individuals affected by liver cancer. With continued research and innovation, the collective efforts of healthcare professionals, researchers, and patients hold the potential to further transform the landscape of liver cancer management in the future.
