In the world of healthcare, it is crucial for nurses to be well-prepared and knowledgeable about a wide range of conditions. One such condition that demands attention is the presence of brain-eating amoeba. When encountering patients affected by this rare but serious infection, nurses play a vital role in providing thoughtful care and management. From understanding the symptoms and potential complications to implementing effective treatment plans, this article will explore the important nursing considerations for brain-eating amoeba and how nurses can make a significant impact in patient outcomes.

Understanding Brain-Eating Amoeba
What is Brain-Eating Amoeba?
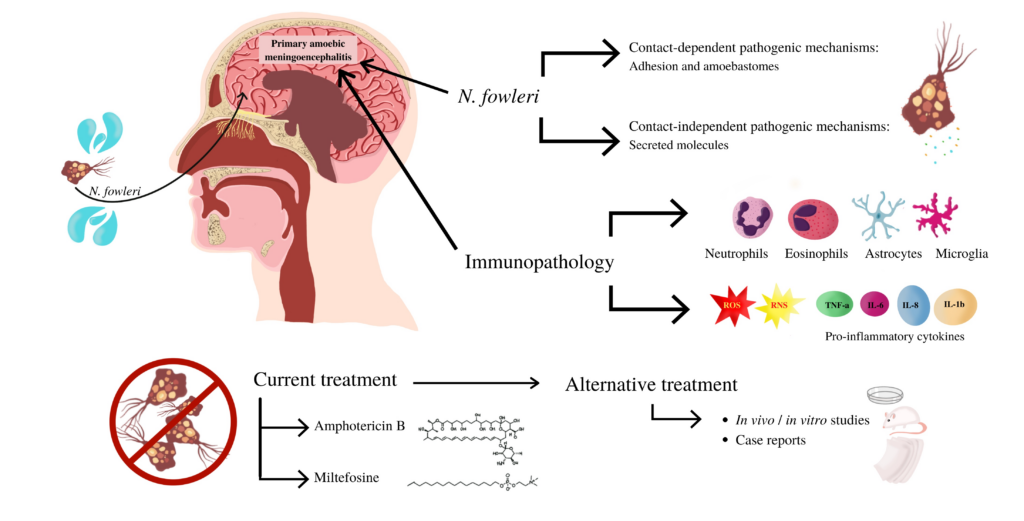
Brain-Eating Amoeba, scientifically known as Naegleria fowleri, is a rare and highly dangerous microorganism that can cause severe infection in the brain. It is commonly found in warm freshwater environments such as lakes, hot springs, and poorly maintained swimming pools. While the amoeba is harmless when swallowed, it can cause devastating infection if it enters the body through the nose.
How does Brain-Eating Amoeba cause infection?
Infection with Brain-Eating Amoeba occurs when contaminated water enters the nasal passages. The amoeba then migrates to the brain, causing inflammation and destruction of brain tissue. This infection, known as primary amoebic meningoencephalitis (PAM), is extremely rare but has a high fatality rate.
Symptoms of Brain-Eating Amoeba infection
The symptoms of Brain-Eating Amoeba infection usually develop within one to nine days after exposure. Early symptoms may mimic those of bacterial meningitis, including fever, headache, and neck stiffness. As the infection progresses, more severe symptoms may appear, such as hallucinations, seizures, changes in taste and smell, and coma. It is essential to seek immediate medical attention if these symptoms arise, especially after water exposure.
Diagnosis and Treatment
Diagnostic methods for Brain-Eating Amoeba infection
Diagnosing Brain-Eating Amoeba infection can be challenging due to its rarity and the rapid progression of symptoms. A lumbar puncture, commonly known as a spinal tap, is often performed to collect cerebrospinal fluid for analysis. Laboratory tests, including polymerase chain reaction (PCR) and microscopic examination, can help identify the presence of Naegleria fowleri. These diagnostic methods play a crucial role in confirming the infection and guiding appropriate treatment.
Medical interventions for Brain-Eating Amoeba infection
Treating Brain-Eating Amoeba infection requires a multidisciplinary approach involving infectious disease specialists, neurologists, and critical care teams. Antimicrobial medications such as amphotericin B are typically administered intravenously to combat the infection. These medications work by targeting the amoeba and inhibiting its growth. In severe cases, additional therapies, such as intrathecal drug administration, may be necessary. Prompt initiation of treatment is crucial for improving the chances of survival.
Preventive Measures
Educating patients and communities about Brain-Eating Amoeba
Raising awareness about Brain-Eating Amoeba is crucial in preventing infection. Healthcare providers play a vital role in educating patients and communities about the risks associated with freshwater exposure. Providing accurate information about the causes, symptoms, and preventive measures can empower individuals to take necessary precautions and seek medical attention promptly.
Preventing exposure to Brain-Eating Amoeba in water sources
Preventing exposure to Brain-Eating Amoeba requires implementing various strategies. Avoiding water-related activities in warm freshwater environments where the amoeba is commonly found is vital. If water exposure is unavoidable, using nose clips or keeping the head above water can prevent the entry of contaminated water through the nose. Regular maintenance and proper disinfection of swimming pools and hot tubs can also help minimize the risk of infection.
Safe swimming practices to prevent Brain-Eating Amoeba infection
Promoting safe swimming practices is essential for reducing the risk of Brain-Eating Amoeba infection. Encouraging individuals to swim only in properly maintained pools with adequate chlorine levels and appropriate filtration systems can significantly lower the chances of exposure. Additionally, advising individuals to avoid stirring up sediment or stirring water forcefully in warm freshwater environments can help minimize the risk of encountering the amoeba.
Patient Assessment
Recognizing high-risk individuals
Identifying high-risk individuals is essential for early intervention and prevention of Brain-Eating Amoeba infection. Individuals with a history of recent freshwater exposure, especially in warm water bodies, should be considered at higher risk. Additionally, those who engage in activities like diving, water skiing, or using water toys that increase the likelihood of water entering the nasal passages should also be recognized as high-risk individuals.
Performing a thorough health history
When assessing patients for potential Brain-Eating Amoeba infection, obtaining a detailed health history is critical. Inquiring about any recent water-related activities and potential exposure to freshwater environments is essential. Additionally, it is important to ask about the presence of any symptoms consistent with the infection, such as fever, headache, or changes in taste or smell. This information helps healthcare providers in making accurate diagnoses and timely treatment decisions.
Assessing presenting symptoms of potential infection
Recognizing the presenting symptoms of potential Brain-Eating Amoeba infection is crucial for timely intervention. Symptoms such as fever, severe headache, stiff neck, vomiting, and changes in mental status should raise concern for possible infection. Close monitoring of vital signs, neurological status, and any changes in symptomatology is necessary to ensure prompt medical attention and appropriate treatment.
Infection Control
Implementing strict isolation precautions
Due to the rarity and potentially fatal nature of Brain-Eating Amoeba infection, implementing strict isolation precautions is crucial. Isolating infected individuals in negative-pressure rooms equipped with high-efficiency particulate air (HEPA) filters can minimize the spread of the amoeba. Wearing appropriate personal protective equipment (PPE) and adhering to strict hand hygiene practices by healthcare providers are essential infection control measures that must be maintained at all times.
Proper handling and disposal of contaminated equipment
Proper handling and disposal of contaminated equipment are critical to prevent the transmission of Brain-Eating Amoeba. Proper sterilization or disposal of instruments and equipment used during procedures, such as lumbar punctures, should be followed meticulously. Adhering to strict disinfection protocols and utilizing single-use disposable items whenever possible can significantly reduce the chances of cross-contamination or subsequent infections.
Ensuring healthcare worker safety
Ensuring the safety of healthcare workers is paramount when managing patients with Brain-Eating Amoeba infection. Providing comprehensive training on infection control practices and the proper use of PPE is essential. Regular communication, updates, and education on emerging research and new treatment modalities help healthcare workers stay informed and effectively manage infected patients while minimizing their own risk of exposure.
Supportive Care
Maintaining adequate hydration
Supportive care plays a crucial role in managing patients with Brain-Eating Amoeba infection. Maintaining adequate hydration is vital to prevent complications such as dehydration and electrolyte imbalances. Intravenous fluids may be administered if oral fluid intake is inadequate. Monitoring daily fluid balance and addressing any fluctuations promptly are essential for optimizing patient outcomes.
Providing comfort measures for symptoms
Patients with Brain-Eating Amoeba infection may experience a range of distressing symptoms. Providing comfort measures to alleviate symptoms can improve the overall patient experience. Controlling fever and pain with appropriate medications and implementing non-pharmacological interventions such as cool compresses and relaxation techniques can offer relief. Collaboration with other healthcare providers, such as pain management specialists or palliative care teams, can enhance the delivery of comprehensive comfort care.
Addressing psychosocial needs of the patient and family
The diagnosis and treatment of Brain-Eating Amoeba infection can have a significant impact on the emotional well-being of patients and their families. Providing emotional support and counseling services to address anxiety, fear, and grief is crucial. Involving social workers, psychologists, or chaplains who specialize in supporting patients and families facing severe illnesses can help alleviate psychosocial distress and improve overall coping mechanisms.
Administration of Antimicrobial Agents
Prescribing and administering appropriate medications
Antimicrobial agents are a cornerstone of treatment for Brain-Eating Amoeba infection. Prescribing and administering appropriate medications, such as amphotericin B, require careful consideration of the patient’s age, weight, renal function, and potential drug interactions. Collaboration between healthcare providers, infectious disease specialists, and pharmacists is crucial in selecting the most effective and safe antimicrobial agents for optimal treatment outcomes.
Monitoring for side effects and therapeutic effectiveness
Monitoring patients for potential side effects and therapeutic effectiveness of antimicrobial agents is essential during the treatment of Brain-Eating Amoeba infection. Regular assessment of renal function, electrolyte levels, and hematological parameters can help detect any adverse effects. Additionally, monitoring the clinical response, such as improvement in symptoms and resolution of cerebrospinal fluid abnormalities, is necessary to ensure treatment efficacy.
Nursing Interventions
Promoting adherence to treatment and follow-up care
As key members of the healthcare team, nurses play a critical role in promoting adherence to treatment and follow-up care. Providing clear instructions regarding medication administration, potential side effects, and the importance of completing the entire treatment course is essential. Regular communication, patient education, and addressing any concerns or barriers to treatment adherence can help improve patient outcomes.
Monitoring vital signs and neurological status
Continuous monitoring of vital signs and neurological status is vital for detecting any changes or complications in patients with Brain-Eating Amoeba infection. Frequent assessment of temperature, blood pressure, heart rate, respiratory rate, and level of consciousness helps identify any early signs of deterioration. Nurses should be vigilant in documenting and reporting any changes promptly to the healthcare team for further evaluation and intervention.
Documenting accurate and timely records
Accurate and timely documentation of all assessments, interventions, and patient responses is of utmost importance in the care of patients with Brain-Eating Amoeba infection. Complete documentation provides a comprehensive picture of the patient’s condition, helps track progress or setbacks, and ensures continuity of care among healthcare team members. Thorough documentation also aids in research, analysis, and quality improvement initiatives related to the management of Brain-Eating Amoeba infection.

Collaborative Care
Ensuring collaboration between healthcare teams
Collaboration among healthcare teams is critical when managing patients with Brain-Eating Amoeba infection. Promoting effective communication, interdisciplinary rounds, and regular team meetings facilitate shared decision-making, treatment planning, and coordination of care. Ensuring that all team members have access to timely and accurate information optimizes patient outcomes and reduces the risk of errors or gaps in care.
Coordination with public health agencies for reporting and surveillance
Coordination with public health agencies is necessary for reporting and surveillance of Brain-Eating Amoeba infections. Healthcare providers should promptly report any suspected or confirmed cases to the appropriate authorities to facilitate epidemiological investigations and prevent further spread. By following established reporting protocols and collaborating with public health agencies, healthcare providers contribute to the ongoing surveillance and prevention efforts against Brain-Eating Amoeba.
Facilitating communication with other healthcare providers
Effective communication with other healthcare providers, including primary care physicians, specialist consultants, and home healthcare agencies, is crucial in optimizing continuity of care for patients with Brain-Eating Amoeba infection. Sharing relevant patient information, treatment plans, and updates ensures a seamless transition between different healthcare settings and promotes holistic patient-centered care. Utilizing secure electronic communication channels and standardized protocols enhances efficient and timely communication among healthcare providers.
Education and Discharge Planning
Providing patient and caregiver education on post-discharge care
Patient and caregiver education plays a vital role in ensuring optimal post-discharge care for individuals recovering from Brain-Eating Amoeba infection. Providing comprehensive information about medication regimens, follow-up appointments, potential signs of recurrence or complications, and strategies to prevent future exposure is essential. Empowering patients and caregivers with knowledge and resources equips them to make informed decisions and actively participate in their own recovery process.
Establishing a comprehensive discharge plan
A comprehensive discharge plan must be established before patients with Brain-Eating Amoeba infection leave the healthcare facility. Collaboration among healthcare providers, including case managers, social workers, and home healthcare agencies, is crucial in arranging necessary medical equipment, medications, and any additional support services required at home. Ensuring a smooth transition to the home environment with appropriate follow-up care helps facilitate the ongoing recovery and well-being of patients.
Referring patients for necessary follow-up and support services
Referral to appropriate follow-up and support services is essential for individuals recovering from Brain-Eating Amoeba infection. This may include referrals to neurologists, infectious disease specialists, rehabilitation services, and mental health professionals. Coordinating referrals, ensuring timely appointments, and providing clear instructions on how to access these services supports the long-term recovery and quality of life for patients affected by Brain-Eating Amoeba infection.