Living with chronic obstructive pulmonary disease (COPD) can present various challenges, but with the help of nursing considerations and proper management, individuals can find relief and improve their quality of life. This article aims to explore key strategies and approaches employed by nurses in the care of COPD patients, including the importance of patient education, medication adherence, and lifestyle modifications. By understanding the unique needs of COPD patients and implementing tailored nursing interventions, healthcare professionals can play a crucial role in supporting individuals with this chronic condition.
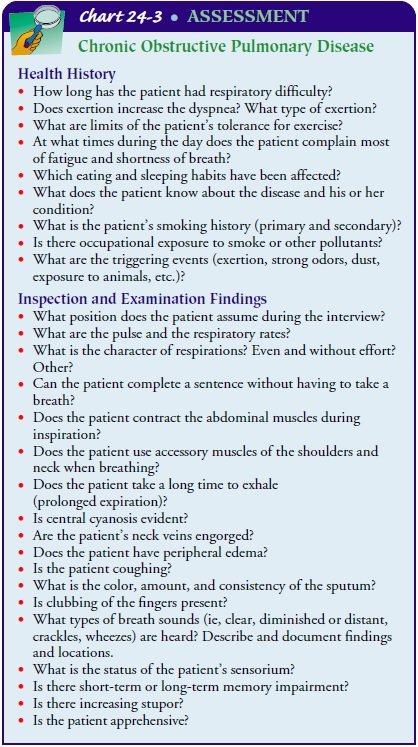
Assessment
Medical history
When assessing a patient with COPD, it is essential to gather a comprehensive medical history. This includes information about any previous diagnoses, hospitalizations, surgeries, or chronic conditions they may have. Additionally, it is vital to inquire about their smoking history, including the number of years they smoked and the average number of cigarettes smoked per day. Family history should also be considered, as genetics can play a role in the development of COPD.
Physical examination
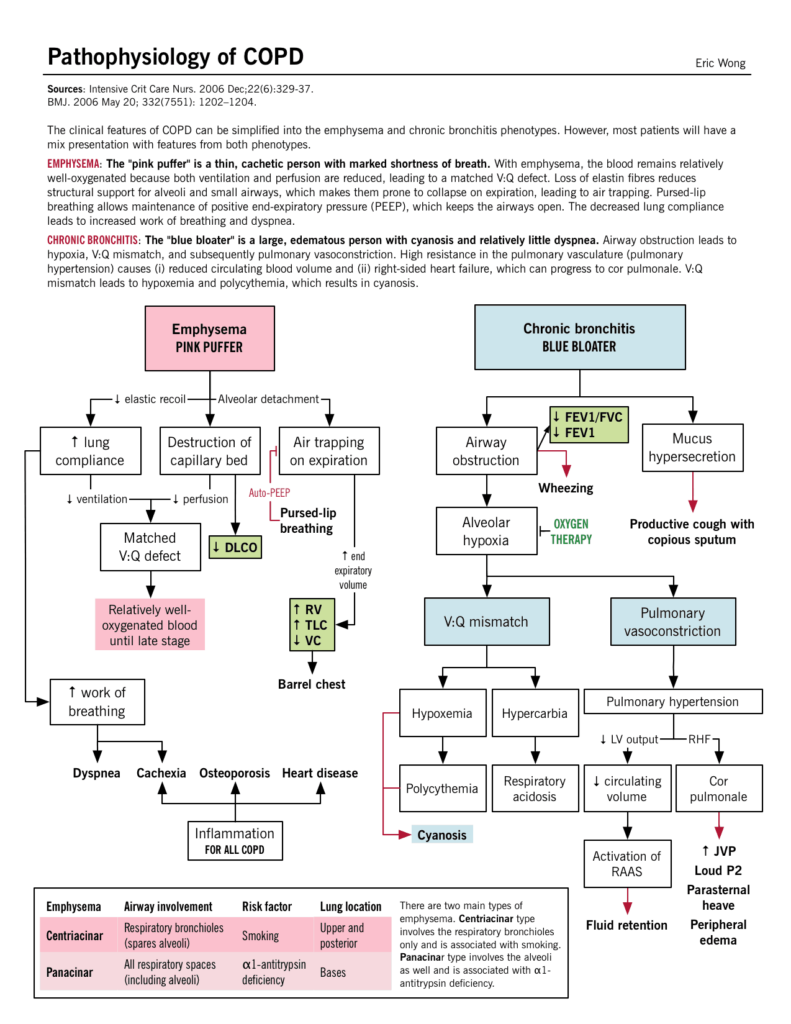
A thorough physical examination is crucial in assessing a patient with COPD. This includes assessing the patient’s general appearance, respiratory effort, and lung sounds upon auscultation. The nurse should observe for signs of respiratory distress, such as increased work of breathing or the use of accessory muscles. Examining the patient’s chest for any abnormalities, such as barrel chest or increased anteroposterior diameter, is also important. Additionally, the nurse should assess the patient’s vital signs, including heart rate, respiratory rate, and oxygen saturation levels.
Diagnostic tests
Various diagnostic tests can aid in the assessment and diagnosis of COPD. Pulmonary function tests, such as spirometry, are commonly used to measure lung function and airflow limitations. These tests can help determine the severity of the patient’s COPD and guide treatment decisions. Chest X-rays may also be performed to assess the presence of any abnormal lung findings or to rule out other pulmonary conditions. In some cases, blood tests may be ordered to evaluate the patient’s oxygen and carbon dioxide levels.
Monitoring and Evaluation
Oxygen saturation levels
Monitoring the patient’s oxygen saturation levels is essential to assess their respiratory status. This is typically done using a pulse oximeter, which measures the percentage of oxygen saturation in the blood. In COPD patients, oxygen saturation levels below 88-92% may indicate hypoxemia and the need for supplemental oxygen therapy.
Arterial blood gas analysis
Arterial blood gas (ABG) analysis provides valuable information regarding the patient’s acid-base balance and oxygenation status. It measures the levels of oxygen, carbon dioxide, and acidity in the arterial blood. ABG analysis is especially useful in determining the severity of respiratory failure in COPD patients.
Respiratory rate
Monitoring the patient’s respiratory rate on a regular basis is essential to identify any changes or worsening of their respiratory status. An increased respiratory rate may indicate respiratory distress or worsening airflow limitations.
Heart rate
Heart rate monitoring is crucial in COPD patients to identify any signs of cardiovascular compromise or abnormalities. Changes in heart rate may indicate increased stress on the heart or inadequate oxygenation.
Peak expiratory flow rate
Peak expiratory flow rate (PEFR) measures the maximum speed at which a patient can exhale after a deep inspiration. It can provide valuable information about a patient’s airflow limitations and the effectiveness of bronchodilator therapy. Regular PEFR monitoring can help assess the severity of COPD and guide treatment adjustments.
Cough frequency and sputum production
Assessing a patient’s cough frequency and sputum production is important in evaluating the effectiveness of treatment and identifying any exacerbations. Increased cough and sputum production may indicate worsening of the patient’s condition or the presence of an infection.
Dyspnea severity
Dyspnea, or shortness of breath, is a common symptom in COPD patients. Assessing the severity and impact of dyspnea on the patient’s daily activities can guide treatment decisions and help evaluate the effectiveness of interventions.
Exercise tolerance
Monitoring a patient’s exercise tolerance is crucial in evaluating their functional capacity and overall respiratory status. It can help determine the appropriateness of exercise interventions or the need for referral to pulmonary rehabilitation programs.
Medication Management
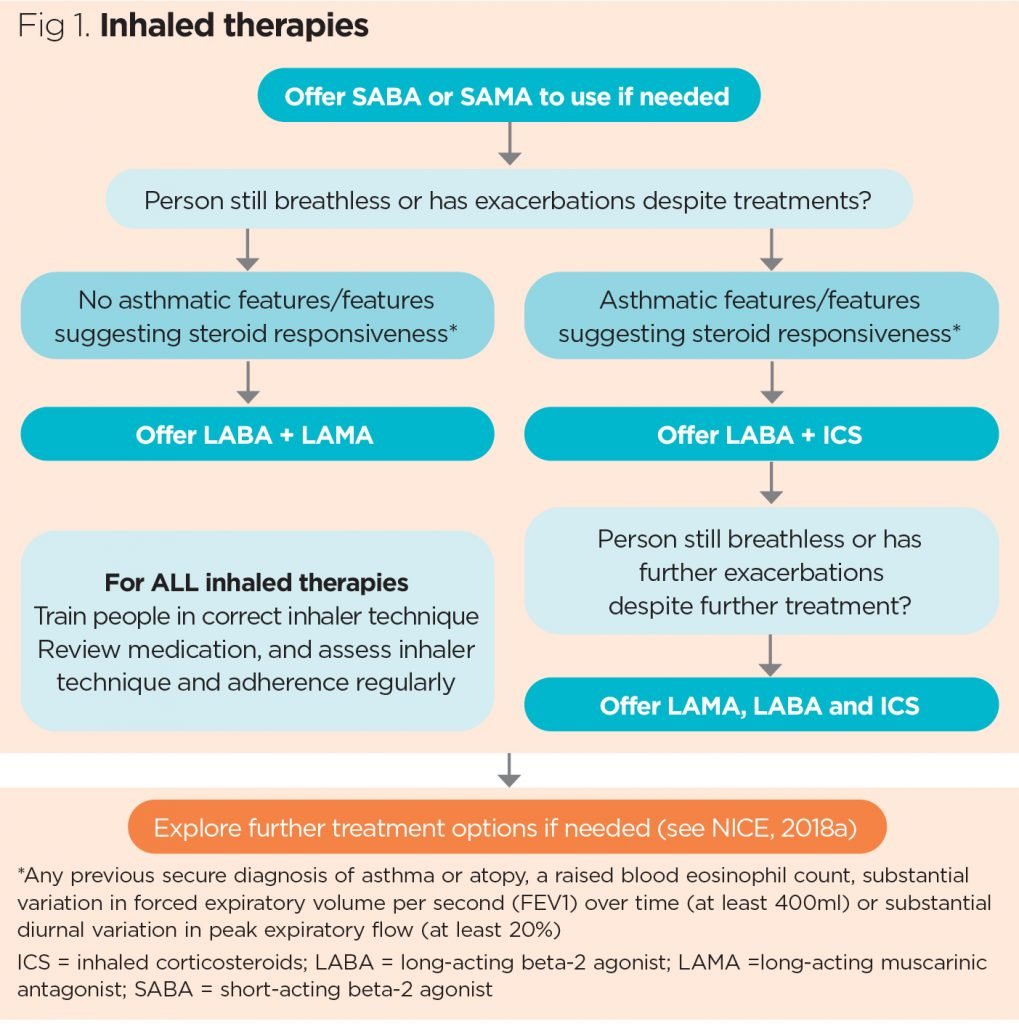
Bronchodilators
Bronchodilators, such as short-acting beta-agonists and long-acting anticholinergics, are commonly prescribed medications for COPD patients. These medications work by relaxing the airway smooth muscles, improving airflow, and relieving bronchospasms. Nurses play a vital role in educating patients on proper inhaler technique and adherence to medication schedules.
Corticosteroids
Corticosteroids, such as inhaled or systemic glucocorticoids, may be prescribed to reduce airway inflammation and manage COPD exacerbations. Nurses should provide education on the potential side effects of corticosteroids and monitor patients for any adverse reactions.
Mucolytics
Mucolytics, such as acetylcysteine, help thin and mobilize mucus, making it easier for patients to clear their airways. Nurses should educate patients on proper administration techniques and encourage the use of mucolytics as prescribed.
Antibiotics
In cases of COPD exacerbations or suspected respiratory infections, antibiotics may be prescribed to treat bacterial infections. Nurses should monitor the patient’s response to antibiotic therapy and educate them on the importance of completing the full course of treatment.
Vaccinations
COPD patients are at increased risk of respiratory infections, so preventive vaccinations play a crucial role in their management. Nurses should ensure that patients receive yearly influenza vaccinations and appropriate pneumococcal vaccines to reduce the risk of complications.
Oxygen Therapy
Assessing oxygen requirements
Assessing a patient’s oxygen requirements is essential in determining the need for supplemental oxygen therapy. This is typically done using arterial blood gas analysis and monitoring oxygen saturation levels. Nurses should collaborate with the healthcare team to establish target oxygen saturation levels and adjust therapy as necessary.
Administering supplemental oxygen
Nurses are responsible for administering supplemental oxygen to COPD patients as prescribed. They should ensure that oxygen delivery devices, such as nasal cannulas or oxygen masks, are properly fitted and used correctly to maximize oxygen delivery while ensuring patient comfort.
Monitoring oxygen therapy effectiveness
Regular monitoring of oxygen saturation levels and ABG analysis is essential to evaluate the effectiveness of oxygen therapy in COPD patients. Nurses should closely monitor the patient’s respiratory status and adjust oxygen flow rates or fractions as needed.
Education on oxygen therapy
Nurses play a crucial role in educating COPD patients and their families about oxygen therapy. They should explain the purpose of oxygen therapy, demonstrate proper device use, and provide instructions on safety precautions and maintenance.

Airway Clearance Techniques
Chest physiotherapy
Chest physiotherapy techniques, such as percussion and vibration, help mobilize and remove mucus from the airways. Nurses should perform and teach these techniques to COPD patients to facilitate airway clearance.
Postural drainage
Postural drainage involves positioning the patient to help facilitate the drainage of mucus from specific lung segments. Nurses should assist patients in assuming the appropriate positions and educate them on the benefits and proper techniques of postural drainage.
Positive expiratory pressure
Positive expiratory pressure (PEP) devices are used to maintain positive pressure in the airways during expiration, helping to recruit collapsed lung units and improve airway clearance. Nurses should instruct patients on how to use PEP devices effectively and monitor their response to therapy.
Mechanical insufflation-exsufflation
Mechanical insufflation-exsufflation (MI-E) devices provide assisted coughing by delivering a positive pressure during inspiration and switching to negative pressure during exhalation. Nurses should train patients on the use of MI-E devices for effective airway clearance.
High-frequency chest wall oscillation
High-frequency chest wall oscillation devices use mechanical vibrations to help loosen and mobilize mucus from the airway walls. Nurses should educate patients on the use of these devices and monitor their response to treatment.
Smoking Cessation
Assessing smoking habits
Assessing a patient’s smoking habits is crucial in developing a personalized smoking cessation plan. Nurses should inquire about the patient’s smoking history, the number of cigarettes smoked per day, and any previous quit attempts.
Providing smoking cessation counseling
Nurses play a vital role in providing smoking cessation counseling to COPD patients. They should educate patients about the harmful effects of smoking on respiratory health, discuss the benefits of quitting, and provide strategies and resources to help patients quit smoking.
Referring to smoking cessation programs
Nurses should refer COPD patients to smoking cessation programs and support groups to enhance their chances of quitting successfully. These programs often provide additional counseling, medications, and peer support.
Educating on the benefits of quitting smoking
Nurses should educate COPD patients about the significant benefits of quitting smoking, including improved lung function, reduced risk of exacerbations, and enhanced quality of life. Reinforcing these benefits can motivate patients to make positive changes.

Nutritional Support
Assessing nutritional status
Assessing a patient’s nutritional status is essential to identify any deficiencies or malnutrition. Nurses should conduct a thorough nutritional assessment, including collecting information on dietary habits, weight changes, and symptoms of malnutrition.
Providing dietary counseling
Nurses play a crucial role in providing dietary counseling to COPD patients. They should educate patients about the importance of a balanced diet, including adequate protein and calorie intake, to support respiratory muscle function and maintain health.
Monitoring weight changes
Regular monitoring of weight changes is crucial in evaluating the effectiveness of nutritional interventions and identifying any signs of malnutrition or fluid retention. Nurses should document and track the patient’s weight on an ongoing basis.
Referring to nutritionists or dietitians
For more complex nutritional needs, nurses should consider referring COPD patients to nutritionists or dietitians who can provide specialized guidance and support.
Psychosocial Support
Assessing anxiety and depression
Psychosocial support is essential in managing COPD patients’ emotional well-being. Nurses should assess for symptoms of anxiety or depression, which are common in individuals with chronic respiratory conditions.
Providing emotional support
Nurses can provide emotional support by actively listening to patients, acknowledging their fears and concerns, and providing reassurance. They should create a supportive environment where patients feel comfortable expressing their emotions and seeking help.
Referring to mental health professionals
In cases where COPD patients require specialized mental health support, nurses should refer them to mental health professionals, such as psychologists or psychiatrists, who can provide appropriate assessment and intervention.
Promoting patient education and self-care
Nurses should empower COPD patients with education and self-care strategies to enhance their understanding of the condition and improve their ability to manage symptoms. They can provide resources, educational materials, and teach coping mechanisms to promote self-care and self-management.

Exercise and Physical Activity
Assessing exercise tolerance
Assessing a patient’s exercise tolerance is crucial in tailoring personalized exercise plans. Nurses should evaluate each patient’s current abilities, limitations, and any symptoms experienced during physical activity.
Developing personalized exercise plans
Nurses should collaborate with patients and other healthcare professionals to develop personalized exercise plans that suit their specific needs and abilities. These plans may include aerobic exercises, such as walking or cycling, as well as strength training exercises.
Providing education on breathing techniques during exercise
Nurses should teach COPD patients proper breathing techniques, such as pursed-lip breathing or diaphragmatic breathing, to optimize lung function during exercise. These techniques can help reduce dyspnea and improve exercise tolerance.
Monitoring exercise progress
Regular monitoring of exercise progress is essential to evaluate the patient’s response to therapy and make necessary adjustments. Nurses should track changes in exercise tolerance, symptom severity, and overall well-being.
Referring to pulmonary rehabilitation programs
Nurses should refer COPD patients to specialized pulmonary rehabilitation programs, where they can receive multidisciplinary care, exercise training, and education on self-management strategies. These programs can significantly improve COPD patients’ overall quality of life and functional capacity.
Education and Self-Management
Explaining COPD and its management
Nurses should provide comprehensive education to COPD patients regarding the nature of the disease, its progression, and the importance of ongoing management. They should explain the causes of COPD, risk factors, and the benefits of adhering to treatment plans.
Teaching proper inhaler use
Proper inhaler technique is crucial for effective medication delivery. Nurses should teach COPD patients how to use their inhalers correctly to ensure optimal drug absorption and maximize therapeutic benefits.
Providing strategies for symptom management
Nurses should educate COPD patients about various strategies for managing symptoms, such as utilizing pursed-lip breathing during dyspnea episodes, staying hydrated, and using relaxation techniques. These self-management strategies can help patients cope with daily challenges related to COPD.
Creating action plans for exacerbations
Nurses should help COPD patients develop personalized action plans for exacerbations, outlining steps to take when symptoms worsen. These plans may include adjusting medication doses, increasing rescue inhaler use, or seeking medical attention.
Promoting adherence to treatment plans
Nurses should emphasize the importance of medication adherence, regular follow-up appointments, and lifestyle modifications to improve disease management. They should provide ongoing support and reinforcement to encourage patients to stay committed to their treatment plans.
By following these nursing considerations and incorporating a holistic approach to care, healthcare professionals can optimize the management of COPD patients, improve their quality of life, and reduce the frequency and severity of exacerbations.