Do you ever experience that annoying, involuntary twitching of your eyelid? It’s not uncommon and can happen to anyone. But what exactly causes this irritating phenomenon? In this article, we will explore the nursing considerations and management for eye twitching, shedding light on the potential causes and discussing the effective nursing strategies to provide relief and alleviate this pesky problem. So, let’s delve into the world of eye twitching and discover the solutions that can help you bid farewell to those bothersome twitches.

Definition and Causes
Definition of eye twitching
Eye twitching, also known as eyelid myokymia, is a repetitive, involuntary spasm or twitching of the eyelid muscles. It is usually brief and can occur in one or both eyes. Eye twitching can range from a mild annoyance to a more persistent and bothersome problem.
Common causes of eye twitching
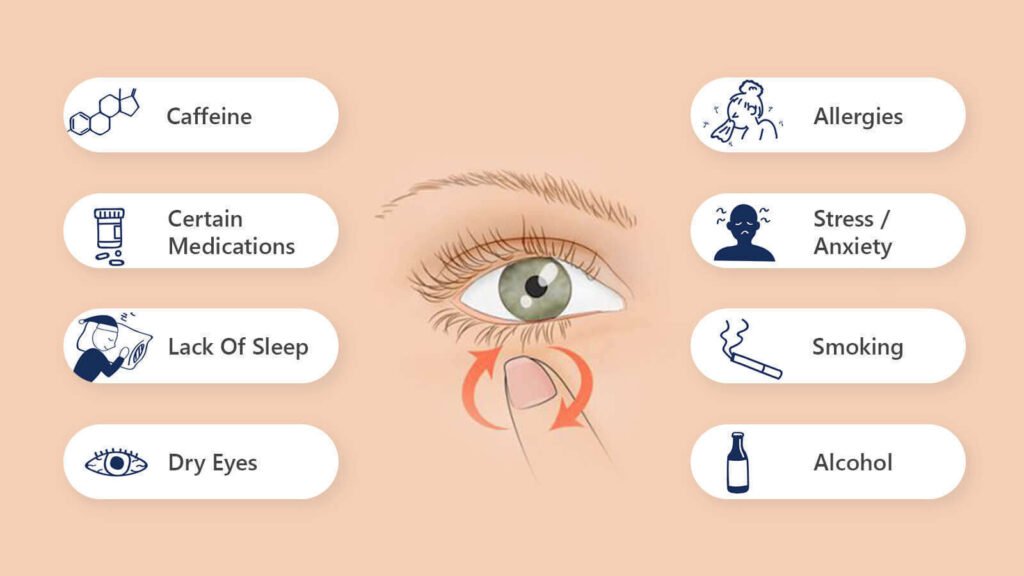
Eye twitching is often harmless and self-limiting, and its exact cause is often unknown. However, there are several common factors that can contribute to eye twitching. These include stress and anxiety, fatigue, excessive caffeine intake, eyestrain, dry eyes, and irritation from dust or foreign bodies.
Less common causes of eye twitching
In some cases, eye twitching may be caused by underlying medical conditions or medications. Less common causes of eye twitching may include neurological disorders, such as blepharospasm or hemifacial spasm, as well as certain medications, such as antihistamines, antidepressants, or stimulants. If eye twitching is persistent or accompanied by other concerning symptoms, it is important to seek medical evaluation to rule out any underlying conditions.
Assessment
Observing frequency and duration of eye twitching
As a nurse, it is important to assess the frequency and duration of eye twitching in order to gather important information about the condition. Ask the patient how often the eye twitching occurs and how long each episode lasts. This information can help determine the severity and impact of the twitching on the patient’s daily life.
Determining triggers and aggravating factors
Identifying triggers and aggravating factors can help in managing eye twitching effectively. Encourage the patient to keep a diary or log of their activities, stress levels, and any other factors that may be associated with the onset or worsening of eye twitching. This can include factors such as caffeine consumption, exposure to irritants, or specific situations that may cause stress or anxiety.
Evaluating associated symptoms
In addition to eye twitching, it is important to assess whether the patient is experiencing any other symptoms that may be related. These can include eye irritation, redness, excessive tearing, or blurred vision. Understanding the full range of symptoms can help guide the nursing management and treatment approach.
Assessing patient’s medical history
Taking a thorough medical history is crucial in assessing and managing eye twitching. Nursing staff should inquire about any past or current eye conditions, previous episodes of eye twitching, and any medical conditions or medications that may be relevant. Certain medical conditions, such as dry eyes, allergies, or neurological disorders, may increase the risk of eye twitching and require further evaluation or management.
Diagnostic Tests
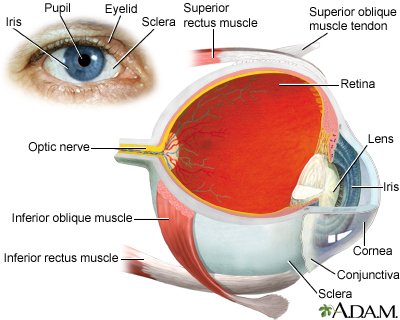
Electromyography (EMG)
Electromyography (EMG) is a diagnostic test that measures the electrical activity of the muscles. It can be used to assess the muscles involved in eye twitching and determine if there are any abnormal patterns or underlying muscle disorders. This test can help rule out more serious causes of eye twitching and provide valuable information for treatment planning.
Blood tests
In some cases, blood tests may be ordered to evaluate for any underlying medical conditions that may be contributing to eye twitching. These tests can help identify factors such as hormonal imbalances, vitamin deficiencies, or autoimmune disorders that may be causing or exacerbating the twitching.
MRI or CT scan
In rare cases where an underlying neurological disorder or structural abnormality is suspected, an MRI or CT scan may be ordered. These imaging tests can help visualize the structures of the brain, nerves, and muscles and provide more detailed information about any potential causes of eye twitching.
Patient Education and Counseling
Explaining eye twitching and its causes
It is important to educate patients about eye twitching and reassure them that it is often a benign condition. Explain that eye twitching is typically a result of muscle spasms in the eyelids and is commonly triggered by stress, fatigue, or other factors. Help patients understand that while the exact cause may not always be known, there are strategies and treatments available to help manage and alleviate the symptoms.
Providing reassurance and support
Eye twitching can be frustrating and may cause anxiety for some patients. As a nurse, providing reassurance and emotional support is essential. Encourage patients to share their concerns and address any misconceptions or worries they may have. Offer guidance on coping mechanisms and stress reduction techniques to help them feel more at ease.
Educating on self-care measures
Empower patients by educating them on self-care measures that can help alleviate eye twitching. This can include recommendations such as getting enough rest and sleep, reducing caffeine intake, practicing stress management techniques, and using warm compresses to soothe the eyes. Emphasize the importance of good eye hygiene, such as avoiding rubbing the eyes and practicing proper contact lens care.
Discussing treatment options
Depending on the severity and impact of the eye twitching, various treatment options may be considered. Discuss potential treatment options with the patient, such as lifestyle modifications, medications, or alternative therapies. Help patients understand the potential benefits and risks associated with each option and involve them in the decision-making process.
Eye Twitching Management
Identifying and addressing underlying causes
When managing eye twitching, it is important to identify and address any underlying causes. Encourage patients to modify behaviors or habits that may contribute to eye twitching, such as reducing caffeine consumption, practicing stress reduction techniques, or taking regular breaks to rest the eyes during prolonged periods of screen time. Addressing these underlying causes can effectively reduce the frequency and intensity of eye twitching.
Recommendations for stress reduction
Stress and anxiety are common triggers for eye twitching. Provide patients with personalized stress reduction strategies, such as deep breathing exercises, mindfulness techniques, or engaging in hobbies and activities that promote relaxation. Encourage the incorporation of regular exercise and healthy lifestyle habits, as these can help reduce overall stress levels and contribute to improved eye health.
Lifestyle modifications to prevent eye strain
Eyestrain can contribute to eye twitching. Encourage patients to practice good eye ergonomics, such as maintaining proper distance from screens, adjusting lighting conditions to reduce glare, and ensuring a comfortable working environment. Advise regular eye breaks and encourage blinking exercises to prevent dryness and strain.
Suggestions for proper eye hygiene
Proper eye hygiene is essential for maintaining optimal eye health and preventing eye twitching. Advise patients to avoid rubbing their eyes, as this can further irritate the eyelid muscles and exacerbate twitching. Encourage them to practice good hand hygiene and to ensure that any contact lenses or eye makeup are properly cleaned and disposed of to reduce the risk of irritation or infection.
Medication Considerations
Anticholinergic medications
In certain cases, anticholinergic medications may be prescribed to help manage eye twitching. These medications work by blocking the transmission of certain nerve signals that can trigger muscle spasms. However, it is important to carefully weigh the potential benefits and risks of these medications, as they can have side effects and may not be suitable for everyone.
Muscle relaxants
Muscle relaxant medications may be considered for individuals with severe or persistent eye twitching that significantly affects their quality of life. These medications help to reduce muscle spasms and can provide relief from twitching. However, it is important to closely monitor the patient and assess for any potential side effects or interactions with other medications.
Botulinum toxin injections
Botulinum toxin injections, such as Botox, may be recommended for individuals with severe or chronic eye twitching that does not respond to other treatment approaches. These injections work by temporarily paralyzing the muscles responsible for the twitching. However, this intervention requires careful assessment and monitoring, as it carries potential risks and side effects.

Alternative and Complementary Interventions
Acupuncture
Acupuncture is a traditional Chinese medicine technique that involves the insertion of thin needles into specific points on the body. Some individuals find acupuncture to be helpful in reducing eye twitching, as it can help balance the body’s energy and promote relaxation. However, the scientific evidence for its effectiveness in managing eye twitching is limited, and it may not be suitable for everyone.
Relaxation techniques
Various relaxation techniques, such as meditation, guided imagery, or progressive muscle relaxation, may help individuals manage and reduce eye twitching. These techniques can help lower stress levels and promote overall relaxation, which may alleviate the frequency and intensity of eye twitching episodes.
Herbal remedies
Certain herbal remedies, such as chamomile or lavender, are thought to have calming properties that may help reduce eye twitching. However, it is important to exercise caution when using herbal remedies, as their safety and efficacy may vary, and potential interactions with other medications should be considered. It is recommended to consult with a healthcare professional before starting any herbal remedies.
Monitoring and Follow-up
Tracking frequency and intensity of eye twitching
Effective monitoring of eye twitching involves tracking the frequency and intensity of episodes. Encourage patients to keep a record or diary of their eye twitching episodes, noting the date, time, duration, and any associated symptoms. This information can help evaluate the effectiveness of treatment interventions and guide further management decisions.
Assessing treatment effectiveness
Regular follow-up assessments are essential in evaluating the effectiveness of the chosen treatment options. Monitor patient responses to interventions, such as lifestyle modifications or prescribed medications, and assess whether there has been a reduction in the frequency and intensity of eye twitching episodes. Adjustments to the treatment plan may be required based on the patient’s progress or changing needs.
Addressing any new concerns or side effects
During follow-up appointments, encourage patients to share any new concerns or side effects they may be experiencing. Address these concerns promptly, as they may require further evaluation or adjustment of the treatment plan. Open and ongoing communication with patients is crucial in providing optimal care and support.

Interdisciplinary Collaboration
Collaborating with ophthalmologists
Collaboration with ophthalmologists is important for accurate diagnosis and comprehensive management of eye twitching. Ophthalmologists can provide expertise in eye health and help rule out any underlying eye conditions or complications. Regular communication and collaboration with ophthalmologists ensure a holistic approach to patient care.
Referring to neurologists or other specialists
In cases where eye twitching is persistent or severe, referral to a neurologist or other specialists may be necessary. These professionals can further evaluate the underlying causes of eye twitching, particularly if a neurological disorder or structural abnormality is suspected. Collaboration with specialists ensures that patients receive appropriate, specialized care.
Coordinating care with primary healthcare providers
Coordinating care with primary healthcare providers, such as family physicians or nurse practitioners, is essential in ensuring continuity and comprehensive management of eye twitching. Sharing relevant assessment findings, treatment plans, and follow-up progress with primary healthcare providers helps facilitate holistic patient care and promotes optimal outcomes.
Documentation and Reporting
Accurate documentation of assessments and interventions
Accurate and detailed documentation of the assessments conducted and interventions implemented is crucial in providing quality care. Document the patient’s medical history, assessment findings, treatment plans, and patient education provided. This documentation serves as a reference for future healthcare providers and helps ensure continuity of care.
Reporting any significant changes or concerns
If any significant changes or concerns arise during the nursing management of eye twitching, it is important to report them promptly to the appropriate healthcare professionals. This may include reporting any worsening symptoms, complications, or unexpected reactions to treatments. Timely reporting ensures that patients receive appropriate and timely interventions.
