Are you a nurse looking to enhance your knowledge and skills in managing headaches? Look no further! In this article, we will provide you with valuable insights and nursing considerations for effectively managing headaches. From identifying different types of headaches to implementing appropriate interventions, we’ve got you covered. So let’s dive right in and equip you with the necessary tools to alleviate your patients’ headache symptoms and improve their overall quality of life.
Assessment
Gathering patient history
When assessing a patient with headaches, gathering a thorough patient history is essential. This includes obtaining information about the onset, duration, frequency, and intensity of the headaches. It is important to ask about any triggers or exacerbating factors, as well as any associated symptoms such as nausea, vomiting, or visual disturbances. Additionally, it is crucial to inquire about the patient’s medical history, including any previous head injuries, chronic illnesses, or medication use. By gathering a comprehensive patient history, nurses can gather clues and valuable information that will assist in the diagnosis and management of the headaches.
Performing a physical examination
Once the patient history has been obtained, conducting a physical examination is the next step in the assessment process. The physical examination for headache patients typically includes a detailed neurological examination to assess for any abnormalities. This may involve testing vision, cranial nerve function, motor coordination, and sensation. The nurse should also assess vital signs, as changes in blood pressure or heart rate may be indicative of certain types of headaches. By performing a thorough physical examination, nurses can identify any physical findings that may aid in the diagnosis and management of headaches.
Assessing headache characteristics
Assessing headache characteristics is a critical aspect of the assessment process. Nurses should carefully document the location, quality, and radiation of the headache pain. Additionally, it is important to inquire about the presence of any associated symptoms such as photophobia, phonophobia, or aura. Nurses should also assess the impact of the headache on the patient’s daily activities and overall quality of life. By gathering information about the specific characteristics of the headache, nurses can better understand the type and potential cause of the headache, which will guide the subsequent steps in diagnosis and management.
Diagnosis
Using diagnostic tools
Once the assessment is complete, nurses may utilize various diagnostic tools to aid in the diagnosis of headaches. These tools may include imaging studies such as CT scans or MRIs to rule out any structural abnormalities or tumors. Additionally, laboratory tests may be ordered to assess for any underlying medical conditions or abnormalities such as electrolyte imbalances or hormonal disorders. By utilizing these diagnostic tools, nurses can gather objective data that will help confirm or exclude potential causes of the headaches.
Identifying potential causes
Identifying potential causes of headaches is an important step in the nursing diagnosis process. Nurses should consider both primary and secondary causes of headaches. Primary headaches, such as tension headaches or migraines, are typically not associated with an underlying medical condition. Secondary headaches, on the other hand, are caused by an underlying condition such as a sinus infection or head trauma. Nurses should carefully review the patient’s history, physical examination findings, and diagnostic test results to identify any potential causes of the headaches. This will guide the subsequent management plan and interventions.
Collaborating with healthcare team
Collaboration with the healthcare team is essential in the diagnosis of headaches. Nurses should work closely with physicians, neurologists, and other healthcare professionals to ensure a comprehensive assessment and accurate diagnosis. This may involve discussing the patient’s history, physical examination findings, and diagnostic test results to gather different perspectives and insights. By collaborating with the healthcare team, nurses can ensure a holistic and multidisciplinary approach to headache diagnosis and management.
Medical Interventions
Prescribing analgesics
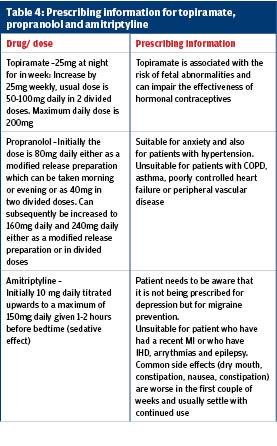
One of the key medical interventions in managing headaches is the prescription of analgesics. Nurses may assist the healthcare team in prescribing appropriate pain medications to alleviate headache symptoms. Commonly used analgesics for headaches include nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or acetaminophen. These medications help to reduce inflammation and relieve pain. It is important for nurses to educate patients about the proper use and potential side effects of analgesics, as well as monitor for any adverse reactions or interactions with other medications.
Administering triptans
Triptans are another class of medications that may be used in the management of headaches. These medications work by constricting blood vessels in the brain and reducing inflammation. They are typically used for migraine headaches. Nurses may be responsible for administering triptans or providing education to patients about their use. It is important to carefully assess the patient’s health history and ensure there are no contraindications or potential drug interactions before administering triptans.
Using ergotamine derivatives
Ergotamine derivatives are a class of medications that may be used in the management of severe or refractory headaches. These medications work by constricting blood vessels in the brain and reducing inflammation. They are typically used for cluster headaches or migraines. Nurses should closely monitor patients receiving ergotamine derivatives for any adverse reactions or side effects, such as nausea, vomiting, or muscle pain. Education should be provided to patients about the proper use, potential side effects, and precautions associated with these medications.
Non-pharmacological Interventions
Applying cold or hot compresses
Non-pharmacological interventions are an important component of headache management. Applying cold or hot compresses to the affected area can provide relief for tension headaches or migraines. Cold compresses help to reduce inflammation, while hot compresses help to relax tense muscles. Nurses can teach patients proper techniques for using cold or hot compresses and educate them about potential precautions, such as avoiding excessive heat or cold exposure.
Using relaxation techniques
Relaxation techniques, such as deep breathing exercises or progressive muscle relaxation, can also help manage headache symptoms. These techniques promote relaxation and reduce stress, which may be contributing factors to headaches. Nurses can teach patients these relaxation techniques and encourage their practice as part of a comprehensive headache management plan. It is important to provide ongoing support and reinforcement for patients as they incorporate these techniques into their daily routines.
Implementing lifestyle changes
Implementing lifestyle changes is another important non-pharmacological intervention in headache management. Nurses should assess the patient’s lifestyle habits and identify any potential triggers or exacerbating factors for headaches. This may include assessing factors such as sleep patterns, stress levels, dietary habits, and physical activity. Nurses can work with patients to develop strategies for making positive lifestyle changes, such as practicing regular exercise, maintaining a consistent sleep schedule, or adopting healthy eating habits. By implementing these lifestyle changes, patients may experience a reduction in the frequency or intensity of their headaches.

Patient Education
Explaining headache triggers
Patient education is a crucial component of headache management. Nurses should provide information to patients about common headache triggers and how to avoid or minimize them. Common triggers include stress, lack of sleep, certain foods or beverages, environmental factors such as loud noises or strong odors, and hormonal fluctuations. By explaining these triggers, patients can make informed decisions and lifestyle modifications to prevent or minimize their headaches.
Discussing medication adherence
Medication adherence is essential in headache management. Nurses should educate patients about the importance of adhering to prescribed medication regimens and provide information about the potential benefits and risks of the medications. It is important to emphasize the importance of taking medications as directed and not skipping doses, even if symptoms improve. Nurses can also provide strategies for improving medication adherence, such as using pill organizers or setting reminders. By discussing medication adherence, nurses can help patients achieve optimal treatment outcomes.
Teaching stress management techniques
Stress management techniques are important for patients with headaches, as stress can often trigger or exacerbate symptoms. Nurses should teach patients various stress management techniques, such as deep breathing exercises, meditation, or engaging in activities that bring joy and relaxation. These techniques can help patients cope with stress and reduce its impact on headache frequency and intensity. Nurses should also encourage patients to seek additional support if needed, such as counseling or support groups, to further enhance their stress management skills.
Monitoring and Evaluation
Assessing treatment effectiveness
Monitoring and evaluating the effectiveness of headache treatments is crucial for optimizing patient outcomes. Nurses should closely monitor patients’ response to medications and other interventions, assessing for any improvement in headache frequency, intensity, and duration. Regular follow-up assessments should be scheduled to assess treatment effectiveness and make any necessary adjustments to the management plan. By assessing treatment effectiveness, nurses can ensure that patients are receiving the most appropriate and effective interventions for their headaches.
Monitoring for adverse effects
In addition to assessing treatment effectiveness, nurses should also closely monitor patients for any potential adverse effects or complications related to headache medications or other interventions. This may involve monitoring vital signs, assessing for signs of medication toxicity, or conducting laboratory tests as indicated. Nurses should educate patients about potential side effects and instruct them to report any concerning symptoms. By monitoring for adverse effects, nurses can promptly identify and address any potential complications, ensuring patient safety.
Tracking headache patterns
Tracking headache patterns is an important aspect of monitoring and evaluation. Nurses should encourage patients to keep a headache diary or use a mobile application to record details about their headaches, such as onset, duration, frequency, intensity, and associated symptoms. This information can provide valuable insights into headache triggers or patterns and guide the management plan. Nurses should review and analyze the data collected in the headache diary during follow-up assessments to further tailor the management plan to the individual patient’s needs.

Safety Precautions
Identifying contraindications
Identifying contraindications to certain headache medications is essential to ensure patient safety. Nurses should carefully review the patient’s health history, including allergies and previous adverse reactions to medications, to identify any contraindications or precautions. For example, certain medications may be contraindicated in patients with liver or kidney dysfunction or in pregnant or breastfeeding women. By identifying contraindications, nurses can prevent potential harm or adverse reactions in patients.
Monitoring for potential complications
Monitoring for potential complications is another important safety precaution in headache management. Nurses should be vigilant for any signs or symptoms of medication toxicity, such as severe drowsiness, confusion, or difficulty breathing, and take appropriate action if needed. Additionally, nurses should assess for any worsening of headache symptoms or the development of new symptoms that may require further evaluation. By monitoring for potential complications, nurses can ensure early detection and intervention to promote patient safety.
Ensuring proper medication storage
Proper medication storage is crucial to maintain medication efficacy and prevent potential harm. Nurses should educate patients about the importance of storing medications in a cool, dry place away from direct sunlight and out of reach of children or pets. Additionally, patients should be instructed on how to properly dispose of expired or unused medications to prevent accidental ingestion or environmental contamination. By ensuring proper medication storage, nurses can help prevent medication errors and promote patient safety.
Collaboration and Referrals
Consulting with neurologists
Collaboration with neurologists is often necessary in the management of complex or refractory headaches. Nurses should consult with neurologists for their expertise and guidance in diagnosing and managing challenging headache cases. This may involve discussing the patient’s assessment findings, treatment plan, and progress to gather additional insights and recommendations. By collaborating with neurologists, nurses can ensure that patients with complex headaches receive specialized care and interventions.
Referring to headache specialists
In some cases, referral to headache specialists may be necessary for further evaluation and management. Headache specialists, such as neurologists or pain management physicians, have extensive knowledge and experience in the diagnosis and treatment of various headache disorders. Nurses should work with the healthcare team to identify appropriate headache specialists and facilitate referrals for patients who may benefit from specialized care. By referring to headache specialists, nurses can ensure that patients receive comprehensive and expert management of their headaches.
Collaborating with psychologists
Psychological factors, such as stress, anxiety, or depression, can often play a significant role in the experience and management of headaches. Nurses should collaborate with psychologists or other mental health professionals to address and manage these psychological factors. This may involve referring patients to psychologists for counseling or therapy, incorporating behavioral interventions into the management plan, or providing education and support to patients and their families. By collaborating with psychologists, nurses can ensure a holistic and patient-centered approach to headache management.

Documentation
Maintaining accurate records
Accurate and comprehensive documentation is critical in headache management. Nurses should maintain detailed records of the patient’s history, physical examination findings, diagnostic test results, treatment plans, and interventions. Accurate documentation ensures continuity of care and enables healthcare professionals to provide appropriate and effective treatment. Nurses should adhere to institutional policies and guidelines for documentation and ensure that all entries are legible, dated, and signed.
Recording medication administration
Recording medication administration is another important aspect of documentation in headache management. Nurses should accurately record the administration of medications, including the name, dose, route, time, and any adverse reactions or effects observed. This documentation provides a record of the patient’s medication history and assists in monitoring treatment effectiveness. Nurses should follow institutional protocols for medication administration documentation, ensuring compliance with legal and regulatory requirements.
Documenting patient education
Documenting patient education is essential to ensure that patients receive consistent and accurate information. Nurses should document the topics discussed during patient education sessions, such as headache triggers, medication adherence, and stress management techniques. This documentation serves as a reference for both the patient and the healthcare team, ensuring that important information is not forgotten or misunderstood. Nurses should encourage patients to ask questions and seek clarification during education sessions, and document any concerns or additional information provided.
Ethical Considerations
Respecting patient autonomy
Respecting patient autonomy is a fundamental ethical consideration in headache management. Nurses should involve patients in the decision-making process, providing them with information about their condition, treatment options, and potential risks and benefits. Patients should be given the opportunity to ask questions, express their preferences, and make informed decisions about their care. Nurses should also respect patients’ rights to refuse or discontinue certain treatments and ensure that their choices are honored.
Maintaining confidentiality
Maintaining confidentiality is another important ethical consideration in headache management. Nurses should ensure that all patient information is kept private and confidential, in compliance with legal and ethical standards. This includes protecting patient information during discussions, documentation, and electronic record-keeping. Nurses should also obtain patient consent before sharing any relevant information with other healthcare professionals involved in the patient’s care. By maintaining confidentiality, nurses uphold patient privacy and trust.
Promoting cultural sensitivity
Promoting cultural sensitivity is crucial in providing patient-centered care for individuals with headaches. Nurses should be aware of and respect cultural beliefs, values, and practices that may influence the patient’s experience and management of headaches. This may involve asking open-ended questions to understand the patient’s cultural perspectives on health and illness, adapting communication and education strategies to be culturally appropriate, and involving interpreters or cultural liaisons as needed. By promoting cultural sensitivity, nurses can provide individualized and culturally competent care to diverse patient populations.
