If you’re a nurse or aspiring to be one, it’s crucial to have a solid understanding of nursing considerations for pneumonia. This article will provide you with the essential knowledge and nursing management strategies you need to effectively care for patients with pneumonia. From understanding the pathophysiology of the disease to implementing appropriate interventions, we’ve got you covered. So, put on your nursing cap and get ready to enhance your skills in providing optimal care for individuals with pneumonia.

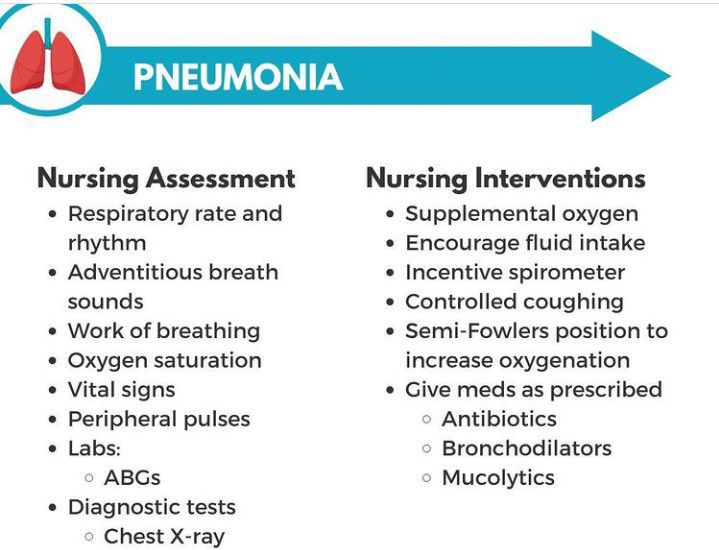
Assessment
Collecting patient history
When assessing a patient with pneumonia, it is crucial to collect a comprehensive patient history. This includes information about the patient’s medical history, current symptoms, and any relevant risk factors. It is important to ask about the onset of symptoms, the severity of symptoms, and any factors that may have triggered the illness such as recent travel or exposure to someone with a respiratory infection. Additionally, it is essential to gather information about the patient’s past medical history, including any underlying conditions that may increase their risk for pneumonia, such as chronic obstructive pulmonary disease (COPD) or immunosuppression. By collecting a detailed patient history, nurses can better understand the individual needs of the patient and provide appropriate care.
Performing physical examination
A thorough physical examination is necessary to assess the patient’s respiratory status and identify any abnormalities or signs of complications associated with pneumonia. During the examination, it is important to assess the patient’s breathing pattern, respiratory effort, and the presence of any accessory muscle use or retractions. Listening to lung sounds is essential in evaluating the presence and distribution of breath sounds, as well as the presence of crackles, wheezes, or decreased breath sounds. The nurse should also assess the patient’s vital signs, including temperature, heart rate, respiratory rate, and blood pressure. By performing a comprehensive physical examination, nurses can gather information that will aid in the diagnosis and management of pneumonia.
Assessing vital signs
Assessing vital signs is a crucial component of monitoring patients with pneumonia. Fever is a common symptom of pneumonia, and assessing the patient’s temperature is important for evaluating disease severity and response to treatment. Additionally, monitoring heart rate, respiratory rate, and blood pressure can provide insights into the patient’s overall condition. Tachypnea or rapid breathing is a common respiratory finding in pneumonia and can be indicative of respiratory distress or increased work of breathing. By regularly assessing vital signs, nurses can detect early changes in the patient’s condition and intervene accordingly.
Monitoring oxygen saturation levels
Oxygen saturation levels should be closely monitored in patients with pneumonia to assess the adequacy of oxygenation and respiratory function. Pulse oximetry is a non-invasive method used to measure oxygen saturation levels in arterial blood. A normal oxygen saturation level is typically above 95%. In the case of pneumonia, decreased oxygen saturation levels may indicate respiratory compromise and the need for supplemental oxygen. By monitoring oxygen saturation levels, nurses can identify early signs of hypoxemia and ensure appropriate oxygen therapy is provided to maintain optimal oxygenation.
Diagnostic Tests
Chest X-ray
A chest X-ray is a commonly ordered diagnostic test for evaluating patients with suspected pneumonia. It is used to identify the presence of infiltrates or consolidation in the lungs, which are indicative of pneumonia. By obtaining a chest X-ray, healthcare providers can confirm the diagnosis of pneumonia and assess the extent and location of the infection. This information is crucial for determining the appropriate treatment plan and monitoring the patient’s progress.
Complete blood count (CBC)
A complete blood count (CBC) is a blood test that provides information about the patient’s overall health and can aid in the diagnosis and management of pneumonia. An elevated white blood cell count is often seen in patients with bacterial pneumonia, indicating the presence of an infection. Additionally, a CBC can provide information about the patient’s hemoglobin and hematocrit levels, which can help identify anemia or blood loss associated with pneumonia. By reviewing the results of a CBC, nurses can gain valuable insights into the patient’s immune response and overall health status.
Arterial blood gas (ABG) analysis
Arterial blood gas (ABG) analysis is a test used to assess the patient’s acid-base balance and oxygenation status. In patients with pneumonia, ABG analysis can reveal abnormalities in oxygen and carbon dioxide levels, providing valuable information about the severity and progression of the disease. ABG results can guide the need for respiratory support and the adjustment of oxygen therapy. By closely monitoring ABG values, nurses can ensure that the patient’s respiratory status is adequately managed.
Sputum culture and sensitivity
A sputum culture and sensitivity test is performed to identify the specific bacteria or pathogens causing the pneumonia infection and determine the most appropriate antibiotic treatment. Collecting a sputum sample from the patient is necessary for this test. Nurses play a critical role in obtaining a high-quality sputum sample and ensuring that it is properly labeled and sent to the laboratory. By facilitating the sputum culture and sensitivity test, nurses contribute to the accurate diagnosis and effective treatment of pneumonia.

Nursing Diagnoses
Ineffective airway clearance
Ineffective airway clearance is a common nursing diagnosis for patients with pneumonia. The infection and inflammation in the lungs can lead to the production of excessive mucus, which can obstruct the airways and impair the patient’s ability to breathe effectively. Nurses can intervene by assisting the patient with coughing and deep breathing exercises to promote airway clearance. They may also administer medications, such as bronchodilators or mucolytics, to help loosen and remove secretions.
Impaired gas exchange
Impaired gas exchange is another critical nursing diagnosis for patients with pneumonia. The infection and inflammation in the lungs can impair the exchange of oxygen and carbon dioxide, leading to hypoxemia and respiratory distress. Nurses can monitor the patient’s oxygen saturation levels, provide supplemental oxygen as needed, and encourage deep breathing exercises to optimize gas exchange. It is important to closely monitor the patient’s respiratory status and intervene promptly if any signs of worsening gas exchange occur.
Risk for infection
Patients with pneumonia are at an increased risk for developing secondary infections due to their weakened immune system and compromised respiratory function. Nurses can implement infection prevention strategies, such as proper hand hygiene, isolation precautions, and monitoring for signs of infection, to reduce the risk of further complications. Educating patients and their families about the importance of infection prevention measures can also help minimize the risk of additional infections.
Activity intolerance
Pneumonia can cause significant fatigue and weakness, leading to activity intolerance in patients. Nurses can assess the patient’s tolerance for physical activity and assist with energy conservation techniques. It is important to promote rest and gradually increase activity levels as the patient’s condition improves. By addressing activity intolerance, nurses can help patients regain their strength and minimize the impact of pneumonia on their daily activities.
Nursing Interventions
Positioning the patient
Positioning the patient is an essential nursing intervention for promoting optimal respiratory function in patients with pneumonia. Positioning the patient in an upright or semi-upright position, such as sitting in a chair or using pillows to prop them up in bed, can help improve lung expansion and reduce the risk of complications, such as aspiration. By maintaining proper positioning, nurses can facilitate effective breathing and improve oxygenation.
Administering prescribed medications
Nurses play a critical role in administering prescribed medications to patients with pneumonia. This may include antibiotics to treat the underlying infection, as well as medications to manage symptoms such as pain, fever, and cough. It is important for nurses to ensure that medications are administered on time and according to the prescribed dosage. Additionally, nurses should closely monitor for any adverse reactions or interactions with other medications the patient may be taking.
Encouraging adequate fluid intake
Staying well-hydrated is crucial for patients with pneumonia as it helps thin mucus secretions, facilitates expectoration, and prevents dehydration. Nurses should encourage patients to drink an adequate amount of fluids, and monitor their intake and output. It is important to educate patients about the importance of hydration and provide options such as water, broth, or warm liquids to facilitate fluid intake.
Implementing chest physiotherapy techniques
Chest physiotherapy techniques, such as chest percussion, vibration, and postural drainage, can help mobilize and remove mucus from the lungs in patients with pneumonia. Nurses can collaborate with respiratory therapists to implement these techniques and provide the necessary education and support to patients and their families. By incorporating chest physiotherapy into the patient’s care plan, nurses can promote effective airway clearance and improve respiratory function.

Patient Education
Explaining the importance of completing a full course of antibiotics
One crucial aspect of patient education for those with pneumonia is explaining the importance of completing a full course of antibiotics. It is essential for patients to understand that stopping antibiotics prematurely can lead to incomplete eradication of the infection and increase the risk of antibiotic resistance. Nurses should provide clear instructions on the prescribed duration and schedule for antibiotic therapy, emphasizing the importance of adherence and addressing any concerns or questions the patient may have.
Teaching deep breathing and coughing exercises
Deep breathing and coughing exercises are vital techniques that can aid in airway clearance and improve lung function in patients with pneumonia. Nurses should teach patients the proper technique for deep breathing exercises, emphasizing the need to take slow, deep breaths and exhale fully. Additionally, nurses should educate patients on effective coughing techniques, such as “huff” coughs or controlled coughing, which help to mobilize mucus and prevent the buildup of secretions in the airways.
Encouraging smoking cessation
Smoking is a significant risk factor for developing pneumonia and can worsen the respiratory symptoms associated with the infection. Nurses can play a crucial role in encouraging smoking cessation by providing information about the health risks of smoking, discussing available resources and support programs, and offering behavioral interventions. By promoting smoking cessation, nurses can help patients improve their respiratory health and reduce the risk of recurrent pneumonia and other respiratory illnesses.
Promoting hand hygiene
Hand hygiene is a fundamental aspect of infection prevention and control, especially for patients with pneumonia. Nurses should emphasize the importance of frequent handwashing or using hand sanitizers to patients and their families. Educating patients about proper hand hygiene techniques, such as washing hands with soap and water for at least 20 seconds, can help prevent the spread of infections and reduce the risk of complications.
Prevention and Control
Immunizations
Immunizations are a crucial preventive measure for reducing the risk of developing pneumonia. Vaccines such as the pneumococcal and influenza vaccines can help protect against the most common pathogens that cause pneumonia. Nurses play a vital role in educating patients about the benefits of immunizations, providing information on vaccine schedules, and administering vaccines based on the patient’s age, medical history, and immunization status.
Pneumococcal and influenza vaccines
The pneumococcal and influenza vaccines are specifically recommended for individuals at a higher risk of developing pneumonia, such as older adults and those with chronic medical conditions. Nurses should ensure that eligible patients receive these vaccines according to the recommended guidelines. By promoting immunization, nurses can help prevent the occurrence of pneumonia and its associated complications.
Isolation precautions
Isolation precautions are essential for preventing the transmission of infectious agents and protecting vulnerable individuals from contracting pneumonia. Nurses should be familiar with the specific isolation protocols and provide education to patients and their families about infection control measures, such as wearing personal protective equipment (PPE) and practicing respiratory hygiene and cough etiquette. By implementing proper isolation precautions, nurses can help minimize the spread of pneumonia in healthcare settings and the community.
Proper hand hygiene
Hand hygiene is a critical component of infection prevention and control. Nurses should lead by example and practice proper hand hygiene techniques, such as washing hands with soap and water or using hand sanitizers before and after patient contact. It is important to promote a culture of hand hygiene among healthcare providers and reinforce its importance in preventing the transmission of infectious agents. Nurses can also educate patients and their families about proper hand hygiene techniques to encourage adherence outside of the healthcare setting.
Monitoring and Evaluation
Regular assessment of respiratory status
Monitoring the respiratory status of patients with pneumonia is essential for evaluating their progress and identifying any changes that may require intervention. Nurses should regularly assess the patient’s breathing pattern, respiratory effort, and oxygen saturation levels. Additionally, monitoring the patient’s lung sounds and respiratory rate can provide valuable information about the effectiveness of the prescribed treatments and the patient’s overall respiratory status.
Monitoring oxygen saturation levels
Oxygen saturation levels should be continuously monitored in patients with pneumonia to ensure adequate oxygenation. Nurses can use pulse oximetry to assess and document the patient’s oxygen saturation levels. Regular monitoring allows for early detection of hypoxemia and ensures prompt intervention with supplemental oxygen or other necessary treatments.
Tracking response to treatment
Tracking the patient’s response to treatment is an essential part of nursing care for pneumonia. Nurses should monitor the patient’s symptoms, vital signs, and laboratory values to evaluate the effectiveness of the prescribed treatment plan. By closely tracking the patient’s response, nurses can identify any improvements or deteriorations and collaborate with the healthcare team to adjust the treatment approach as needed.
Evaluating patient’s overall condition
Evaluating the patient’s overall condition involves considering multiple factors, including respiratory status, vital signs, symptoms, and response to treatment. Nurses should regularly assess the patient’s general well-being, physical comfort, and emotional state. By evaluating the patient’s overall condition, nurses can recognize any changes or complications that may require further intervention or interdisciplinary collaboration.
Collaborative Care
Consulting with respiratory therapist
Respiratory therapists are vital members of the healthcare team when it comes to managing patients with pneumonia. Nurses should collaborate with respiratory therapists to optimize the patient’s respiratory care plan. Respiratory therapists can provide expertise in areas such as oxygen therapy, airway management, and pulmonary function testing. By consulting with respiratory therapists, nurses can ensure that the patient receives comprehensive respiratory care and treatment.
Coordinating with other healthcare providers
Collaboration and coordination with other healthcare providers, such as physicians, pharmacists, and physical therapists, are essential for holistic patient care. Nurses should actively communicate and share information with the healthcare team to facilitate a comprehensive and coordinated approach to managing pneumonia. This may involve providing updates on the patient’s condition, relaying medication orders, or coordinating necessary interventions. By working collaboratively, healthcare providers can provide effective and individualized care for patients with pneumonia.
Referring patients for pulmonary rehabilitation
Pulmonary rehabilitation programs can significantly benefit patients with pneumonia, especially those with persistent symptoms or functional limitations. Nurses should identify eligible patients and refer them to appropriate pulmonary rehabilitation services. These programs typically include exercise training, education, and psychosocial support to improve the patient’s respiratory function, quality of life, and overall well-being. By referring patients for pulmonary rehabilitation, nurses can support their long-term recovery and enhance their ability to manage pneumonia.
Facilitating a multidisciplinary approach to care
Pneumonia management often requires a multidisciplinary approach involving various healthcare professionals. Nurses should facilitate interdisciplinary collaboration and ensure effective communication among team members. This may involve coordinating care conferences, conducting regular team meetings, or sharing relevant patient information. By promoting a multidisciplinary approach, nurses can optimize patient outcomes and provide comprehensive care that addresses all aspects of the patient’s well-being.

Complications
Respiratory failure
Respiratory failure is a severe complication of pneumonia and can occur when the lungs are unable to maintain adequate oxygenation or eliminate carbon dioxide. Nurses should closely monitor patients for signs of respiratory distress, such as increasing respiratory rate, use of accessory muscles, and changes in mental status. Prompt recognition and intervention, such as supplemental oxygen and respiratory support, are vital in managing respiratory failure and preventing further deterioration.
Sepsis
Pneumonia can lead to sepsis, a life-threatening systemic infection that occurs when the body’s response to an infection becomes dysregulated. Nurses should be vigilant for the signs and symptoms of sepsis, which may include fever, increased heart rate, altered mental status, and signs of organ dysfunction. Early recognition and prompt initiation of appropriate treatment, such as intravenous antibiotics and fluid resuscitation, are essential in managing sepsis and improving patient outcomes.
Pleural effusion
Pleural effusion is a buildup of fluid in the space between the layers of tissue that line the lungs and chest cavity. It can occur as a complication of pneumonia and may cause symptoms such as chest pain, shortness of breath, and decreased breath sounds. Nurses should monitor patients for signs of pleural effusion and collaborate with the healthcare team to arrange diagnostic imaging and interventions, such as thoracentesis or chest tube placement, if necessary.
Lung abscess
A lung abscess is a localized collection of pus within the lung tissue and can occur as a complication of pneumonia. It often presents with persistent fever, productive cough with foul-smelling sputum, and chest pain. Nurses should closely monitor patients for signs of lung abscess and work closely with the healthcare team to initiate appropriate diagnostic testing, antibiotic therapy, and, in some cases, surgical intervention.
Ethical Considerations
Informed consent for medical interventions
Obtaining informed consent is an ethical obligation when performing medical interventions for pneumonia. Nurses should ensure that patients or their legally authorized representatives fully understand the risks, benefits, and alternatives of proposed treatments. This includes explaining the potential side effects of medications, the rationale for specific interventions, and the importance of monitoring for potential complications. By promoting informed consent, nurses respect the autonomy and decision-making capacity of the patients.
Respecting patient autonomy
Respecting patient autonomy is a fundamental principle in nursing care. Nurses should involve patients in the decision-making process by providing information, answering questions, and considering their preferences and values. It is important to empower patients to actively participate in their care and make choices that align with their goals and beliefs. By respecting patient autonomy, nurses foster trust and promote patient-centered care.
Protecting patient confidentiality
Maintaining patient confidentiality is essential for maintaining trust and upholding ethical standards in healthcare. Nurses should ensure that patient information is kept confidential and only shared with authorized individuals involved in the patient’s care. This includes following established protocols for the handling of patient records, using secure communication methods, and being mindful of conversations regarding patient information in public areas. By protecting patient confidentiality, nurses demonstrate respect for patient privacy and promote a culture of trust and confidentiality.
Promoting cultural sensitivity
Promoting cultural sensitivity is vital in nursing care for pneumonia. Nurses should recognize and respect the diverse cultural backgrounds, beliefs, and values of patients and their families. Culturally sensitive care involves adapting communication styles, tailoring education materials, and being aware of cultural practices related to health and illness. By promoting cultural sensitivity, nurses ensure that care is delivered in a respectful and inclusive manner that considers the unique needs of each patient.
In conclusion, nursing considerations and management for pneumonia encompass a wide range of assessments, interventions, and education to ensure optimal patient outcomes. By collecting a comprehensive patient history, performing a thorough physical examination, and monitoring vital signs and oxygen saturation levels, nurses can assess the severity and progression of pneumonia. Diagnostic tests such as chest X-rays, complete blood counts, arterial blood gas analysis, and sputum culture and sensitivity tests aid in the diagnosis and management of pneumonia. Nursing diagnoses such as ineffective airway clearance, impaired gas exchange, risk for infection, and activity intolerance guide the nursing interventions, including patient positioning, the administration of prescribed medications, encouraging adequate fluid intake, and implementing chest physiotherapy techniques. Patient education plays a crucial role in promoting adherence to treatment, deep breathing and coughing exercises, smoking cessation, and hand hygiene. Prevention and control strategies focus on immunizations, isolation precautions, and promoting proper hand hygiene. Monitoring and evaluation involve the regular assessment of respiratory status, monitoring oxygen saturation levels, tracking response to treatment, and evaluating the patient’s overall condition. Collaborative care includes consulting with respiratory therapists, coordinating with other healthcare providers, referring patients for pulmonary rehabilitation, and facilitating a multidisciplinary approach to care. Complications such as respiratory failure, sepsis, pleural effusion, and lung abscess should be closely monitored and managed. Ethical considerations, such as obtaining informed consent, respecting patient autonomy, protecting patient confidentiality, and promoting cultural sensitivity, should guide nursing practice in the care of patients with pneumonia. Ultimately, by implementing comprehensive nursing care, nurses can contribute to better patient outcomes, improved quality of life, and the prevention of complications associated with pneumonia.