If you’re looking for valuable insights on nursing considerations for the prevention and treatment of blood clots, you’ve come to the right place! This article will provide you with essential information on the critical role nurses play in managing and preventing blood clots. From understanding risk factors to implementing preventive measures and administering appropriate treatments, nurses are key players in ensuring patient safety. So, let’s dive into the world of nursing considerations for the prevention and treatment of blood clots!
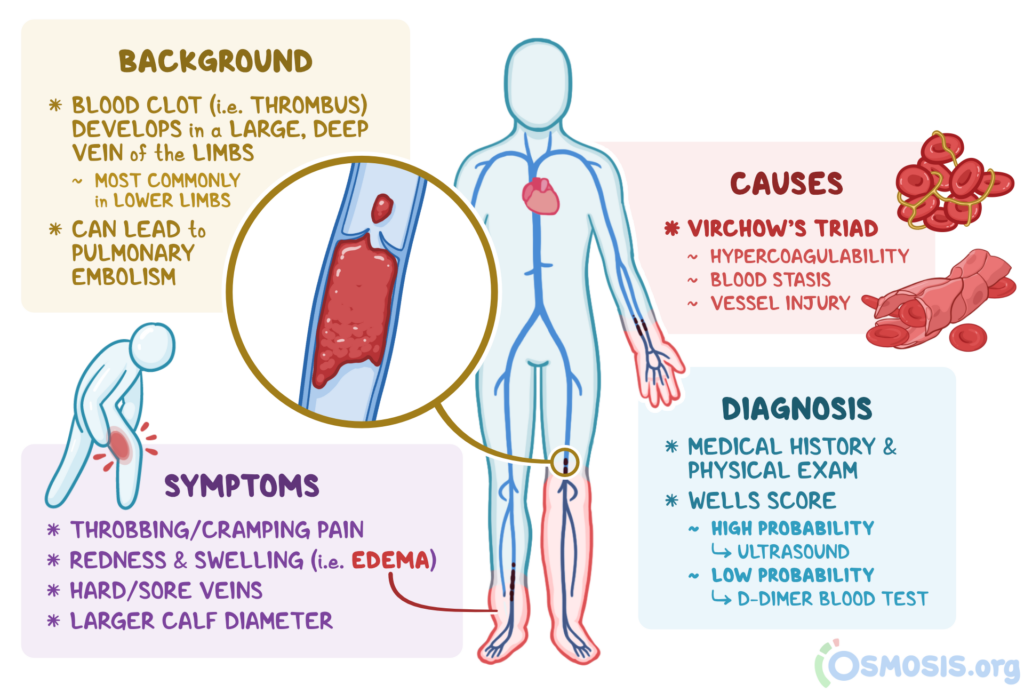
Assessment and Diagnosis of Blood Clots
Assessment of risk factors
When it comes to assessing the risk factors for blood clots, it is essential to consider both the patient’s medical history and their current condition. Some common risk factors include being overweight or obese, having a sedentary lifestyle, smoking, and a family history of blood clots. Other conditions such as cancer, heart disease, and inflammatory disorders can also increase the risk. Assessing these risk factors is crucial in determining the appropriate preventive measures and interventions.
Physical assessment for signs and symptoms
One of the key aspects of diagnosing blood clots is conducting a thorough physical assessment to identify any signs and symptoms. Patients with blood clots may experience pain, swelling, redness, or warmth in the affected area. They may also complain of shortness of breath, chest pain, and a rapid heart rate if the blood clot has traveled to the lungs. The nurse should carefully examine the patient’s skin, checking for areas of discoloration or tenderness. Additionally, vital signs such as blood pressure and oxygen saturation should be monitored to detect any abnormalities that may indicate the presence of blood clots.
Diagnostic tests for blood clot detection
To confirm the presence of blood clots, various diagnostic tests can be performed. These tests include ultrasound, venography, and D-dimer blood tests. Ultrasound imaging is often the initial method used to assess for blood clots, as it is non-invasive and highly accurate. Venography involves injecting a contrast dye into the veins and taking X-ray images to visualize blood flow and detect any blockages. D-dimer blood tests measure the levels of a specific blood protein that is elevated when there is clot formation. These diagnostic tests play a crucial role in accurately diagnosing blood clots and determining the appropriate course of treatment.
Prevention of Blood Clots
Identification and management of modifiable risk factors
Identifying and managing modifiable risk factors is a fundamental aspect of preventing blood clots. Nurses can educate patients about the importance of maintaining a healthy lifestyle, including regular exercise, a balanced diet, and smoking cessation. Encouraging weight management and stress management techniques can also help reduce the risk of blood clots. Additionally, addressing underlying medical conditions and optimizing their management can further decrease the chances of clot formation.
Patient education on prevention strategies
Educating patients about prevention strategies is vital in empowering them to take an active role in their own healthcare. Informing patients about the importance of maintaining good hydration, avoiding prolonged immobility, and taking regular breaks during long-distance travel can significantly reduce the risk of blood clots. It is also essential to provide guidance on recognizing the signs and symptoms of blood clots, such as swelling and pain, so that patients can seek prompt medical attention.
Prophylactic measures in high-risk patients
For patients at high risk of developing blood clots, prophylactic measures can be implemented to prevent their occurrence. These measures may include the use of compression stockings or pneumatic compression devices to promote blood flow and prevent stasis. Additionally, pharmacological interventions such as low molecular weight heparin or anticoagulant medications may be prescribed to reduce the risk of blood clot formation. Nurses play a crucial role in educating patients about these prophylactic measures and ensuring their adherence to prevent complications.

Pharmacological Interventions
Anticoagulant therapy options
Anticoagulant therapy is a common pharmacological intervention used in the management of blood clots. These medications work by inhibiting the clotting factors in the blood, preventing the formation of new clots and allowing existing clots to dissolve. Common anticoagulant medications include heparin, warfarin, and direct oral anticoagulants (DOACs) such as apixaban and rivaroxaban. The choice of anticoagulant therapy depends on various factors, including the severity of the clot, patient characteristics, and the potential for drug interactions or side effects. Nurses should closely monitor patients on anticoagulants, ensuring proper dosing and frequent laboratory monitoring to maintain therapeutic levels.
Monitoring and dosage adjustments for anticoagulants
Monitoring patients on anticoagulant therapy is crucial for ensuring the efficacy and safety of the medication. Nurses must monitor laboratory values such as the international normalized ratio (INR) for patients on warfarin and anti-factor Xa levels for patients on DOACs. Regular monitoring allows for dosage adjustments to maintain the therapeutic range and prevent complications such as bleeding or recurrent clot formation. Nurses should provide education on the importance of adhering to laboratory monitoring schedules and promptly reporting any signs of abnormal bleeding or other adverse effects.
Administration and patient education for anticoagulant medications
Proper administration of anticoagulant medications is essential for their effectiveness. Nurses should provide thorough education on the correct administration techniques, including the importance of taking the medication as prescribed and at the right time. Patients should also be educated on potential drug interactions, dietary considerations, and the importance of regular medication refills to ensure uninterrupted therapy. Furthermore, it is crucial for nurses to emphasize the significance of proper medication storage, such as keeping medications out of reach of children and avoiding exposure to extreme temperatures.
Non-Pharmacological Interventions
Early mobilization and ambulation
Encouraging early mobilization and ambulation is essential in preventing blood clot formation. Nurses should educate patients on the importance of moving their limbs and engaging in gentle exercises, especially after periods of prolonged immobility. Simple activities such as walking, leg exercises, and stretching can promote blood flow, reduce stasis, and decrease the risk of blood clot formation. Nurses can work collaboratively with physical therapists to develop personalized mobility plans for patients, taking into account their individual needs and capabilities.
Compression therapy for prevention and treatment
Compression therapy is another non-pharmacological intervention used in both the prevention and treatment of blood clots. Compression stockings or bandages can be applied to the lower extremities to promote venous blood flow and reduce the risk of stasis. These stockings exert pressure on the legs, helping to prevent the formation of blood clots. Nurses should educate patients on the proper use of compression stockings, including the correct size, wearing duration, and how to monitor for any skin reactions or discomfort. It is important to assess for contraindications, such as peripheral arterial disease, before initiating compression therapy.
Nutritional interventions and hydration
Proper nutrition and hydration are crucial in preventing blood clots. Nurses should educate patients on the importance of consuming a well-balanced diet rich in fruits, vegetables, and whole grains. Adequate hydration is essential as it helps maintain optimal blood viscosity and prevents dehydration, which can increase the risk of blood clot formation. Nurses should assess patients’ dietary habits and provide guidance on healthy eating choices. Additionally, ensuring access to clean drinking water and encouraging patients to consume an appropriate amount of fluids throughout the day can contribute to their overall well-being and blood clot prevention.

Surgical Interventions
Thrombectomy procedures
Thrombectomy procedures may be required in certain cases where blood clots are large or causing severe symptoms. This surgical intervention involves the removal of the clot using various techniques, such as open surgery or minimally invasive procedures like catheter-directed thrombolysis or mechanical thrombectomy. Nurses play a crucial role in preparing patients for these procedures, ensuring informed consent, and providing pre-operative and post-operative care. Close monitoring and assessment of patients’ vital signs, pain levels, and potential complications are essential for successful outcomes.
Insertion and management of vena cava filters
In some high-risk cases or when anticoagulant therapy is contraindicated, the insertion of a vena cava filter may be considered. A vena cava filter is a small device inserted into the inferior vena cava, a large vein that returns blood to the heart. It functions by trapping and preventing blood clots from traveling to vital organs, such as the lungs. Nurses should educate patients about the purpose of the vena cava filter, potential complications, and the need for follow-up care. Close monitoring and regular imaging are necessary to assess the filter’s position and ensure its continued effectiveness.
Special Considerations for Pregnant Patients
Risks and management of blood clots during pregnancy
Pregnancy increases the risk of blood clots due to hormonal changes and the increased pressure on blood vessels in the pelvis. Nurses should be aware of this heightened risk and provide appropriate education to pregnant patients. The management of blood clots during pregnancy often involves a delicate balance between the safety of the mother and the developing fetus. Anticoagulant therapy may be prescribed, and close monitoring is essential. Nurses must ensure proper coordination and communication between the patient’s obstetrician, hematologist, and other healthcare providers to ensure the best possible outcomes for both the mother and the baby.
Antenatal and postnatal care for at-risk pregnant patients
During antenatal care, nurses should identify pregnant patients at higher risk for blood clots and provide appropriate education and support. This may include encouraging regular physical activity, optimizing nutrition, and implementing prophylactic measures such as compression stockings. Postnatally, nurses should continue to monitor and assess these patients for any signs or symptoms of blood clots, as the risk remains elevated even after delivery. Providing ongoing support, education, and follow-up care are vital components of the nursing management of at-risk pregnant patients.

Management of Complications
Bleeding management in patients receiving anticoagulants
One potential complication of anticoagulant therapy is bleeding. Nurses must closely monitor patients on these medications and promptly address any signs of bleeding or abnormal laboratory values. In cases of minor bleeding, wound care and local hemostatic measures may be sufficient. However, more significant bleeding may require the administration of specific reversal agents or blood products. Nurses should be knowledgeable about the reversal agents available for different anticoagulant medications and implement appropriate interventions to manage bleeding effectively.
Management of pulmonary embolism
Pulmonary embolism (PE) is a serious complication of blood clots that requires immediate medical attention. Nurses play a vital role in recognizing the signs and symptoms of PE, such as sudden onset of shortness of breath, chest pain, and rapid breathing. Rapid response and coordination with the healthcare team are crucial in initiating diagnostic tests, such as computed tomography (CT) scans, to confirm the diagnosis. Nurses must provide ongoing monitoring, administer prescribed interventions (such as oxygen therapy and anticoagulant medications), and ensure adequate support and education for patients and their families throughout the treatment and recovery process.
Post-thrombotic syndrome prevention and treatment
Post-thrombotic syndrome (PTS) is a chronic condition that can occur after a blood clot has formed. It is characterized by pain, swelling, and chronic skin changes in the affected area. Nurses can play a crucial role in preventing and managing PTS through early identification and intervention. Implementing measures such as compression therapy, regular exercise, and elevation of the affected limb can help reduce symptoms and prevent further complications. Additionally, providing ongoing education, emotional support, and appropriate referrals to other healthcare providers, such as physical therapists, can contribute to the holistic management of PTS.
Patient Education and Counseling
Explanation of blood clot risk factors and signs
One of the key responsibilities of nurses is providing patient education and counseling regarding blood clot risk factors and signs. By explaining the various risk factors, such as obesity, immobility, and underlying medical conditions, nurses can empower patients to make lifestyle modifications and take preventive measures. Additionally, educating patients about the signs and symptoms of blood clots, such as pain, swelling, and shortness of breath, enables them to recognize potential problems and seek timely medical attention.
Teaching self-care measures and early recognition of complications
Nurses should provide comprehensive education on self-care measures to prevent blood clots and recognize any early signs of complications. This may include teaching patients about the importance of regular exercise, hydration, and medication adherence. Patients should also be educated on the need for prompt reporting of any concerning symptoms, such as sudden pain, difficulty breathing, or unexplained swelling. By equipping patients with this knowledge, nurses empower them to actively participate in their own healthcare and take appropriate action when needed.
Promotion of medication adherence and lifestyle modifications
Nurses play a vital role in promoting medication adherence and facilitating successful lifestyle modifications. Through regular communication and education, nurses can emphasize the importance of taking prescribed medications as directed and the potential consequences of non-adherence. They can also provide guidance and support in implementing lifestyle changes such as healthy eating, regular exercise, and smoking cessation. By promoting medication adherence and lifestyle modifications, nurses contribute to the long-term management and prevention of blood clots.

Collaborative Care and Interdisciplinary Approach
Communication and coordination with healthcare team members
Collaboration and communication among healthcare team members are essential in providing comprehensive care to patients with blood clots. Nurses should actively participate in interdisciplinary team meetings and discussions to ensure a holistic approach to patient management. Effective communication with physicians, pharmacists, physical therapists, and other healthcare providers promotes seamless care coordination, facilitates timely interventions, and enhances patient outcomes. Nurses should be proactive in sharing patient assessments, observations, and concerns to facilitate a comprehensive and cohesive plan of care.
Utilization of evidence-based practice guidelines
Nurses should base their practice on evidence-based guidelines to ensure the delivery of high-quality care to patients with blood clots. Staying up to date with the latest research and guidelines enables nurses to provide the most effective and appropriate interventions. By utilizing evidence-based practice, nurses can enhance patient safety, optimize outcomes, and promote best practices within their healthcare settings.
Integration of social and psychological support
The management of blood clots can have a significant impact on patients’ social and psychological well-being. Nurses should assess patients’ psychosocial needs and provide appropriate support and referrals as needed. This may include connecting patients with support groups, counseling services, or other community resources that can provide emotional support. By addressing patients’ social and psychological concerns, nurses contribute to the overall well-being and recovery of individuals affected by blood clots.
Long-term Management and Follow-up
Monitoring and adjusting anticoagulant therapy
Long-term management of blood clots often involves monitoring and adjusting anticoagulant therapy to maintain therapeutic levels and prevent recurrent clot formation. Nurses play a vital role in monitoring laboratory values, such as INR or anti-factor Xa levels, to ensure appropriate dosage adjustments. Moreover, nurses should educate patients on the importance of regular laboratory monitoring, medication compliance, and follow-up appointments to ensure ongoing management and prevent complications.
Prevention and surveillance of recurrent blood clots
Patients who have experienced blood clots are at risk of developing recurrent clots. Nurses should educate patients on the importance of continued preventive measures, such as regular exercise, compression therapy, and adequate hydration. Encouraging patients to promptly report any concerning symptoms and ensuring regular follow-up appointments are essential for ongoing surveillance and early detection of potential recurrence. By promoting vigilant monitoring and proactive management, nurses contribute to long-term prevention and wellness.
Continued patient education and support
Patient education and support should be an ongoing process throughout the management of blood clots. Nurses should provide patients with educational materials, resources, and support groups to facilitate self-management and adaptation to lifestyle changes. By ensuring ongoing education, answering questions, and addressing concerns, nurses empower patients to actively participate in their long-term management and maintain optimal health outcomes.
In conclusion, the comprehensive management of blood clots requires a multi-faceted approach that encompasses assessment, prevention, intervention, patient education, collaborative care, and long-term follow-up. Nurses, as key members of the healthcare team, play a vital role in each stage of this process. By employing evidence-based practice, advocating for patient-centered care, and fostering effective communication, nurses can contribute to the prevention, treatment, and long-term management of blood clots, ultimately improving patient outcomes and quality of life.