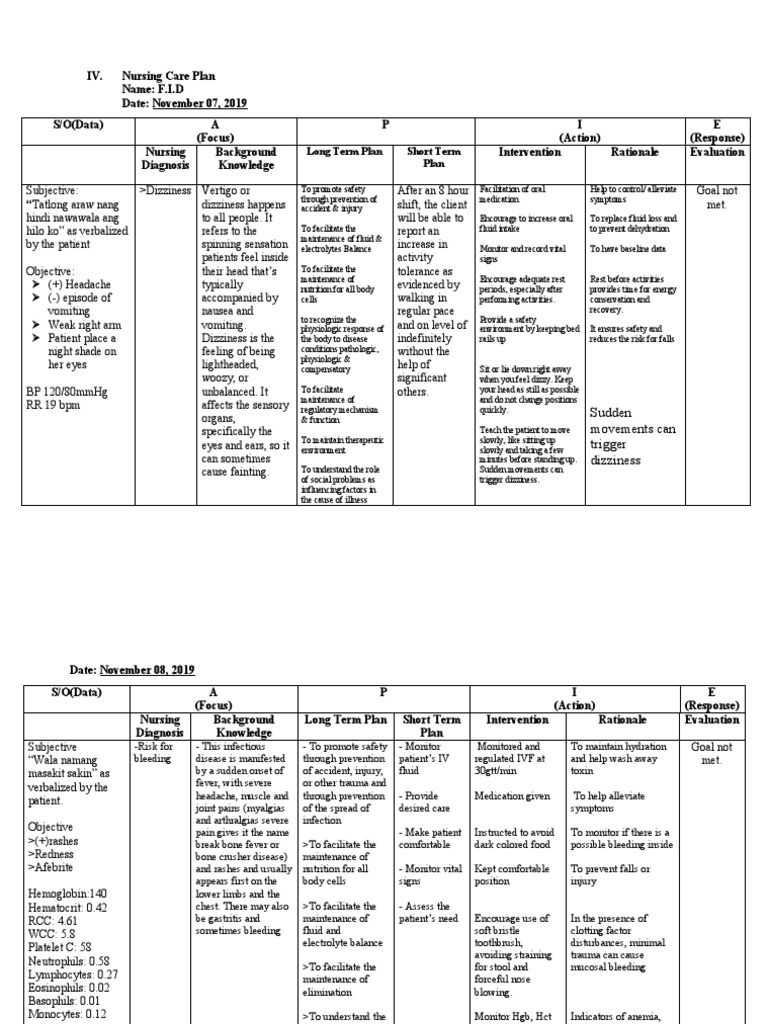
Imagine yourself as a nurse, entrusted with the care of patients experiencing the disorienting symptoms of vertigo. In this article, we will explore the crucial nursing considerations and management strategies for effectively addressing vertigo. By understanding the underlying causes, implementing appropriate interventions, and providing compassionate support, you can play a pivotal role in helping patients regain their balance and find relief from this challenging condition. So, let’s jump right in and discover the valuable insights that will empower you in your nursing practice.
Assessment
Assessing a patient with vertigo is crucial in order to develop an accurate diagnosis and provide appropriate treatment. The assessment begins with obtaining the patient’s medical history, which includes information about previous episodes of vertigo, any existing medical conditions, and medications being taken. This information helps to identify any underlying causes or risk factors for vertigo.
Patient’s Medical History
When gathering the patient’s medical history, it is important to ask about any preexisting conditions that may contribute to the development of vertigo. This includes cardiovascular diseases, diabetes, and neurological conditions. Additionally, the nurse should inquire about any recent head trauma or ear infections that could be associated with vertigo.
Symptoms
During the assessment, it is vital to obtain a detailed description of the patient’s symptoms. Vertigo is characterized by a sensation of spinning or imbalance, and it can be associated with symptoms such as nausea, vomiting, and changes in hearing. The nurse should ask about the frequency, duration, and intensity of the symptoms, as well as any triggers or factors that may worsen or alleviate the vertigo.
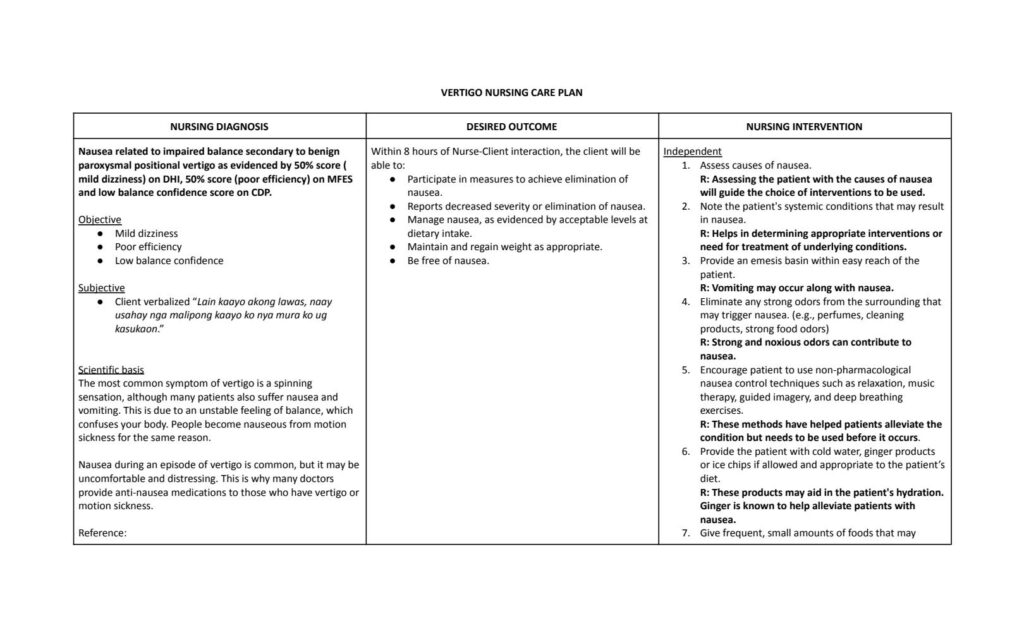
Physical Examination
A thorough physical examination should be performed to assess the patient’s balance, coordination, and gait. The nurse should observe the patient for any signs of unsteadiness or abnormal movements. Tests, such as the Romberg test, may be conducted to evaluate the patient’s balance. Additionally, a neurological examination should be conducted to rule out any neurological causes of vertigo.
Diagnosis
After completing the assessment, the nurse can work collaboratively with the healthcare team to establish a diagnosis for the patient’s vertigo. This often involves considering a range of possible causes and conducting further diagnostic tests to confirm the diagnosis.
Differential Diagnosis
Determining the cause of vertigo can be challenging due to the variety of conditions that can result in similar symptoms. Differential diagnosis involves considering various possibilities and ruling out other potential causes. Common differential diagnoses for vertigo include benign paroxysmal positional vertigo (BPPV), Meniere’s disease, vestibular neuritis, and labyrinthitis.

Diagnostic Tests
To confirm the diagnosis, specific diagnostic tests may be ordered. These tests can include audiological evaluations, such as audiometry and auditory brainstem response testing, to assess the patient’s hearing function. Imaging studies, such as magnetic resonance imaging (MRI) or computed tomography (CT) scans, may also be conducted to evaluate the structures of the inner ear and identify any abnormalities.
Treatment
The treatment plan for vertigo will depend on the underlying cause and severity of the condition. It may involve a combination of medications, physical maneuvers, vestibular rehabilitation, or in some cases, surgical interventions.
Medications
Medications can be prescribed to alleviate vertigo symptoms and manage any associated symptoms such as nausea and vomiting. Commonly used medications for vertigo include antiemetics, antihistamines, anticholinergics, and benzodiazepines. These medications work by targeting the underlying mechanisms that contribute to vertigo, such as reducing inflammation, suppressing the vestibular system, or alleviating nausea.
Physical Maneuvers
Physical maneuvers are non-invasive techniques that can be performed to reposition or dislodge displaced calcium crystals in the inner ear, which can cause vertigo. The most commonly used physical maneuvers for vertigo include the Epley maneuver, Semont maneuver, and Brandt-Daroff exercise. These maneuvers aim to move the calcium crystals from the semicircular canals to a different part of the inner ear where they won’t cause symptoms.
Vestibular Rehabilitation
Vestibular rehabilitation is an exercise-based therapy that helps to improve balance and reduce symptoms of vertigo. This type of therapy may be recommended for patients who continue to experience dizziness and imbalance despite other treatments. Vestibular rehabilitation typically includes balance exercises, visual tracking exercises, and gaze stability exercises. These exercises aim to retrain the brain and central nervous system to compensate for the patient’s vestibular dysfunction.
Surgery
Surgery is typically only considered as a last resort for patients with severe and debilitating vertigo that does not respond to other treatments. Different surgical procedures can be performed depending on the underlying cause of the vertigo. These procedures may include endolymphatic sac decompression, vestibular nerve section, or labyrinthectomy. Surgical interventions can be effective in alleviating symptoms and improving the patient’s quality of life.

Patient Education
Educating patients about their condition is crucial for managing vertigo effectively. Providing detailed explanations about the nature of vertigo and its causes can help patients gain a better understanding of their symptoms. Additionally, patients should be informed about lifestyle modifications that can minimize vertigo episodes, such as avoiding triggers like alcohol or caffeine, maintaining a regular sleep schedule, and practicing stress reduction techniques.
Lifestyle Modifications
Encouraging patients to make lifestyle modifications can significantly impact the frequency and severity of vertigo episodes. This can include advising patients to avoid sudden head movements, changing positions slowly, and using assistive devices for stability. Patients should also be encouraged to stay well-hydrated, eat a balanced diet, and engage in regular physical activity to promote overall health and well-being.
Safety Measures
To prevent accidents and injuries, patients with vertigo should be educated about safety measures. This includes advising patients to use handrails when going up or down stairs, installing grab bars in bathrooms, and removing potential hazards from their immediate environment. Patients should also be cautious when driving or operating heavy machinery, as vertigo can significantly impair their ability to maintain balance and focus.
Fall Prevention
Assessing the risk of falls is critical in managing patients with vertigo, as dizziness and imbalance place them at a higher risk of falls. Nurses should conduct a comprehensive assessment of the patient’s fall risk, including factors such as muscle weakness, visual impairments, and environmental hazards. Implementing appropriate fall prevention strategies can help minimize the risk of injury.
Environmental Modifications
Making environmental modifications can greatly reduce the risk of falls for patients with vertigo. This may involve removing clutter or trip hazards in the home, ensuring proper lighting throughout the living space, and installing assistive devices such as handrails or grab bars in areas prone to falls. By creating a safe and accessible environment, patients can minimize the possibility of accidents.
Mobility Aids
For patients with severe vertigo or a high risk of falls, the use of mobility aids can provide added support and stability. Devices such as canes or walkers can help patients maintain their balance and reduce the risk of falls. The selection and fitting of the appropriate mobility aid should be done in collaboration with a healthcare professional to ensure proper usage and effectiveness.
Psychosocial Support
Living with vertigo can have a significant impact on a patient’s emotional well-being. The unpredictable nature of vertigo episodes, coupled with the physical limitations they impose, can lead to stress, anxiety, and depression. Providing psychosocial support is essential for patients to cope with the emotional challenges associated with vertigo.
Coping Strategies
Teaching patients coping strategies can empower them to manage the emotional and psychological impact of vertigo. Encouraging patients to practice relaxation techniques, such as deep breathing or meditation, can help reduce anxiety and stress levels. Cognitive behavioral therapy (CBT) techniques, such as reframing negative thoughts or engaging in pleasant activities, can also be beneficial in managing the psychological effects of vertigo.
Support Groups
Connecting patients with support groups or online communities can offer invaluable emotional support and a sense of belonging. These groups provide a platform for individuals to share their experiences, learn from others, and receive encouragement and empathy. By participating in support groups, patients can gain insight, positivity, and a network of people who understand and can relate to their journey with vertigo.
Referral to Mental Health Professionals
In some cases, patients with vertigo may require professional mental health support to alleviate symptoms of anxiety or depression. Referring patients to mental health professionals, such as psychologists or psychiatrists, can provide them with specialized care and interventions. These professionals can assess the patient’s mental health status and offer therapies, medications, or other treatments to improve their overall well-being.
In conclusion, nursing considerations and management for vertigo involve a comprehensive assessment of the patient, establishing a diagnosis, and implementing appropriate treatments and support. By addressing the physical, emotional, and psychological impact of vertigo, nurses play a crucial role in improving the quality of life for patients with this challenging condition.
Herbal Treatment Of Vertigo, Home Remedy For Vertigo Treatment, Home Treatment For Dizziness And Nausea, Home Treatment Of Vertigo, Is There A Natural Treatment For Vertigo, Natural Cure For Tinnitus And Vertigo, Natural Cure For Vertigo Attacks