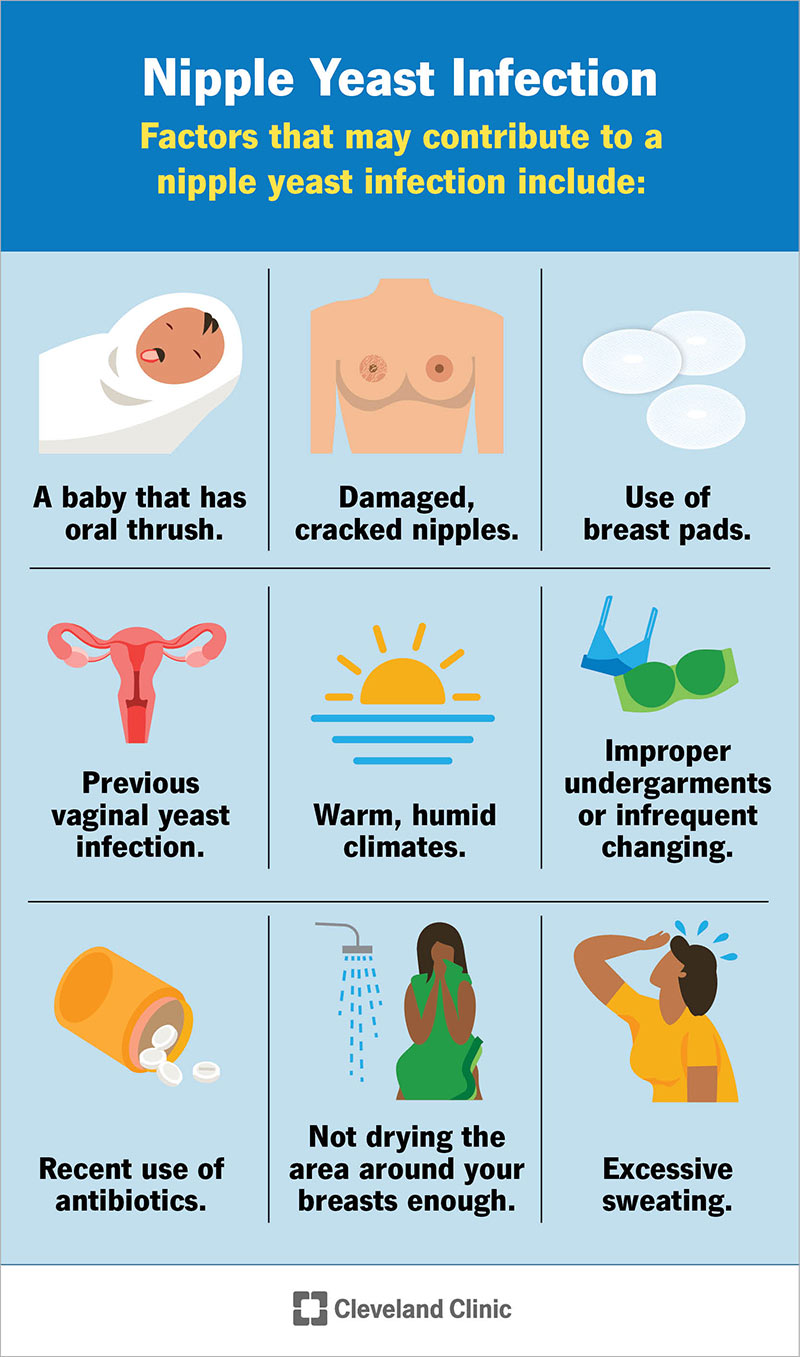
Yeast infections can be uncomfortable and frustrating, but with the right nursing management, you can effectively treat and prevent them. From identifying the symptoms to implementing preventive measures, this article provides comprehensive nursing considerations to help you support patients in managing yeast infections. By approaching this topic with empathy and providing friendly guidance, you can play a crucial role in ensuring your patients’ comfort and well-being.

Assessment of Yeast Infection
Patient history
When assessing a patient with a yeast infection, it is crucial to gather information about their medical history and any previous occurrences or treatments for the infection. Asking questions about the duration and severity of symptoms, any contributing factors such as recent antibiotic use or diabetes, and any previous history of sexually transmitted infections can help in understanding the patient’s condition better.
Physical examination
A thorough physical examination is essential to assess the extent and severity of the yeast infection. The nurse should examine the affected areas, such as the genitals, oral cavity, or skin folds, for any signs of redness, swelling, discharge, or characteristic white patches that are indicative of a yeast infection. Additionally, evaluating other areas of the body, such as the nails or scalp, can help identify any secondary infections or related conditions.
Diagnostic tests
While yeast infections are often diagnosed based on clinical symptoms and examination findings, diagnostic tests may be performed to confirm the presence of Candida, the fungus responsible for the infection. These tests can include microscopic examination of a sample collected from the affected area, such as a vaginal swab or skin scraping. Additionally, cultures or laboratory tests may be done to identify the specific species of Candida involved and to guide appropriate treatment decisions.
Education and Patient Counseling
Overview of yeast infection
Providing patients with a comprehensive overview of yeast infections is crucial in helping them understand their condition better. Nurses should explain that yeast infections are caused by an overgrowth of Candida, which is a normal part of the body’s microbiota. They can occur in various parts of the body, including the genitals, mouth, and skin folds, and are more common in women, individuals with compromised immune systems, and those with diabetes.
Causes and risk factors
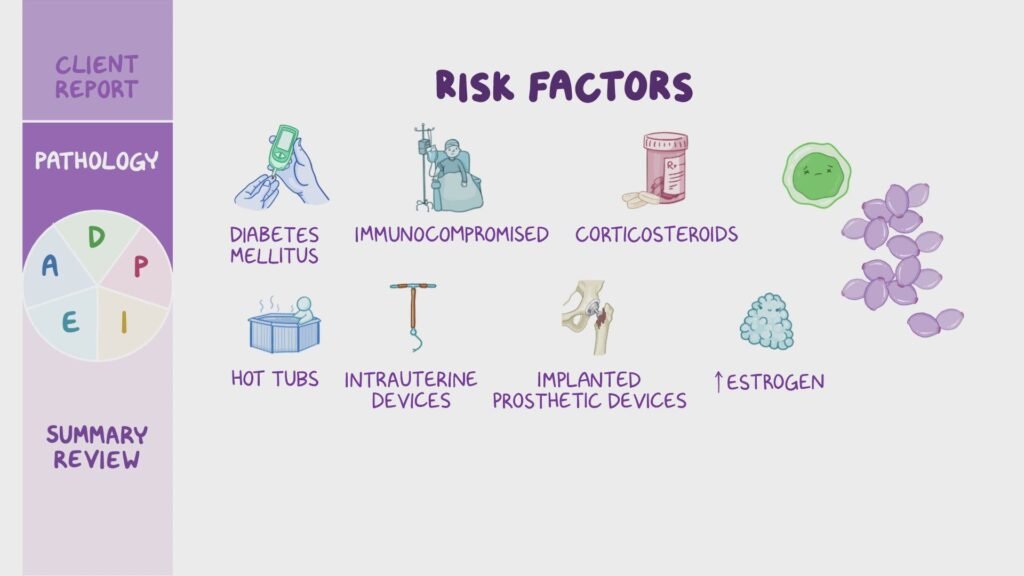
It is important to educate patients about the causes and risk factors associated with yeast infections. Nurses should explain that factors such as antibiotic use, hormonal changes, wearing tight or non-breathable clothing, excessive moisture in the affected areas, and a weakened immune system can contribute to the development of yeast infections. Additionally, engaging in unprotected sexual intercourse or having multiple sexual partners can increase the risk of acquiring a yeast infection.
Prevention strategies
To prevent yeast infections, nurses should educate patients about adopting certain preventive strategies. These include maintaining good hygiene practices, such as keeping the affected areas clean and dry, avoiding the use of harsh soaps or douches, and changing out of wet clothing promptly. Patients should also be advised to wear breathable cotton underwear, avoid tight-fitting pants or pantyhose, and opt for loose-fitting clothes to allow air circulation. Encouraging patients to make lifestyle modifications, such as maintaining a healthy diet, managing stress levels, and avoiding excessive consumption of sugary foods, can also contribute to prevention.
Proper hygiene practices
Patients should be educated on proper hygiene practices to prevent yeast infections and manage their symptoms. Nurses can advise patients to gently cleanse the affected areas with mild soap and water and avoid using scented or irritating products. It is essential to emphasize that excessive cleansing or harsh scrubbing can disrupt the natural balance of the skin or mucous membranes, potentially worsening the infection. Teaching patients to pat the area dry rather than rubbing it and to wear loose-fitting clothing that allows proper air circulation can also help maintain good hygiene.
Safe sexual practices
For patients with vaginal yeast infections, discussing safe sexual practices is essential. Nurses should emphasize that yeast infections are not considered sexually transmitted infections but can be transmitted through sexual activity. Encouraging the use of barrier methods, such as condoms or dental dams, during sexual intercourse can reduce the risk of transmission. It is also important to advise patients to avoid sharing sex toys and to clean them thoroughly after each use.
Management of recurring infections
Patients who experience recurring yeast infections may benefit from additional counseling and management strategies. Nurses should offer support and reassurance while exploring potential triggers or underlying causes for the recurrent infections. This could include revisiting any possible contributing factors, such as medications, chronic medical conditions, or immune system disorders, and working collaboratively with the healthcare team to address them. Nurses should also educate patients about appropriate self-care measures and when to seek medical attention if the infections persist or worsen despite treatment.
Pharmacological Management
Topical antifungal medications
Topical antifungal medications are often the first-line treatment for yeast infections. These medications, available as creams, ointments, or sprays, work by directly targeting the Candida fungus on the affected areas. Nurses should educate patients on proper application techniques, emphasizing the importance of covering the entire affected area and following the prescribed frequency and duration of treatment. It is vital to advise patients to continue the treatment as prescribed, even if symptoms improve, to ensure complete eradication of the infection.
Oral antifungal medications
In cases of more severe or recurrent yeast infections, oral antifungal medications may be prescribed. These medications work systemically to eliminate the Candida fungus throughout the body. Nurses should provide thorough education regarding the proper administration of oral antifungals, emphasizing the importance of completing the full course of treatment, possible side effects, and drug interactions. Patients should be encouraged to discuss any concerns or questions with their healthcare provider.
Antifungal suppositories and creams
In specific instances, such as vaginal yeast infections, antifungal suppositories or creams may be recommended for localized treatment. Nurses should demonstrate the proper technique for insertion and application, ensuring patients understand the frequency and duration of treatment. It is crucial to promote adherence to the prescribed regimen, even if symptoms improve, to prevent recurrent infections. Patients should be reminded to wash their hands before and after administration to maintain proper hygiene.
Probiotics
Probiotics, especially those containing Lactobacillus strains, have gained attention as a potential management strategy for yeast infections. Nurses can educate patients about the role of probiotics in promoting healthy microbial balance and inhibiting the overgrowth of Candida. Discussing the different available forms, such as oral supplements and vaginal suppositories, can help patients make informed decisions about their use. It is important to remind patients that while probiotics may offer potential benefits, they should not replace prescribed antifungal medications and should be used as an adjunctive therapy after consulting with their healthcare provider.
Non-Pharmacological Management
Dietary modifications
Dietary modifications can play a supportive role in managing yeast infections. Nurses should educate patients about the potential impact of certain foods on yeast overgrowth, such as high-sugar and high-carbohydrate diets. Encouraging patients to adopt a balanced diet rich in fruits, vegetables, whole grains, and lean proteins can help support overall immune function and reduce the risk of yeast infections. Additionally, discussing the benefits of consuming probiotic-rich foods, such as yogurt or kefir, can provide patients with additional tools for maintaining microbial balance.
Natural remedies and alternative therapies
When discussing natural remedies and alternative therapies for yeast infections, nurses should approach the topic with caution. It is important to emphasize that while some natural remedies, such as tea tree oil or garlic, may have antimicrobial properties, evidence regarding their efficacy and safety is limited. Patients should be encouraged to consult with their healthcare provider before using any natural remedies or alternative therapies to ensure they do not interfere with prescribed treatments or exacerbate their condition.
Avoidance of irritants
For patients experiencing yeast infections in areas other than the genitals, such as skin folds, it is essential to educate them about avoiding irritants. Nurses should advise patients to avoid using harsh soaps or detergents in the affected areas and to opt for gentle, hypoallergenic products instead. Additionally, patients should be encouraged to avoid prolonged exposure to moisture or friction by keeping the area clean and dry, using absorbent powders or moisture-wicking fabrics, and ensuring proper ventilation in those areas.
Wearing breathable clothing
Wearing breathable clothing is another important non-pharmacological management strategy for yeast infections. Nurses should educate patients about the benefits of wearing loose-fitting, cotton underwear or breathable fabrics that allow proper air circulation. Encouraging patients to avoid tight-fitting pants, pantyhose, and synthetic materials can help reduce moisture buildup and create an unfavorable environment for yeast overgrowth. Patients should also be reminded to change out of wet clothing, such as bathing suits or sweaty workout gear, promptly to prevent prolonged skin contact with moisture.
Maintaining proper genital hygiene
Proper genital hygiene is crucial in managing and preventing yeast infections. Nurses should educate patients on the importance of washing the genital area daily using gentle cleansing techniques and mild soap. Emphasize the significance of thoroughly drying the area after washing to prevent excess moisture buildup. Patients should also be advised to avoid using scented products, harsh cleansers, or douches in the genital area, as these can disrupt the natural balance of the microbiota and potentially worsen the infection.
Management of Complications
Treatment of secondary infections
In some cases, yeast infections can lead to secondary bacterial or fungal infections, especially when left untreated or when the immune system is compromised. Nurses should closely monitor patients for any signs of secondary infections, such as increased redness, swelling, pain, or discharge. If a secondary infection is suspected, prompt intervention, such as appropriate antibiotic or antifungal therapy, should be initiated in collaboration with the healthcare team.
Prevention and management of skin breakdown and irritation
Yeast infections in skin folds or areas of increased moisture can contribute to skin breakdown and irritations. Nurses should educate patients on proper skin care to prevent or manage these complications. Recommending gentle cleansing and drying techniques, regular inspection of the affected areas, and the use of barrier creams or ointments can help protect the skin and promote healing. It is important to remind patients to report any signs of worsening skin breakdown, such as open sores or non-healing wounds, to their healthcare provider for further evaluation and management.
Addressing emotional and psychological concerns
Yeast infections can have a significant impact on a patient’s emotional and psychological well-being. Nurses should provide a supportive and empathetic environment for patients to express their concerns, fears, or anxieties related to their condition. Offering education on the common nature of yeast infections, reassurance, and coping strategies can help alleviate emotional distress. If necessary, nurses should collaborate with the healthcare team to provide appropriate referrals to mental health professionals for additional support.
Collaborative Care
Interdisciplinary communication
Collaboration among healthcare providers is essential for comprehensive care of patients with yeast infections. Nurses play a critical role in facilitating effective communication among the interdisciplinary team, including physicians, pharmacists, and other healthcare professionals. Sharing accurate and timely information regarding the patient’s condition, treatment plan, and response to therapy ensures coordinated and holistic care.
Referral to specialists
In some cases, patients with complex or recurring yeast infections may require referral to specialists for further evaluation and management. Nurses should be familiar with the appropriate referral processes and criteria for infectious disease specialists, gynecologists, dermatologists, or other healthcare professionals who can provide specialized care. Prompt referral to specialists can help ensure the best outcomes for patients who require additional expertise.
Collaboration with pharmacists and other healthcare providers
Pharmacists play a vital role in medication management for patients with yeast infections. Nurses should collaborate with pharmacists to ensure appropriate selection, dosing, and administration of antifungal medications. Pharmacists can provide valuable information regarding drug interactions, contraindications, and potential side effects. Engaging in effective communication with pharmacists and other healthcare providers helps to optimize patient care and promote positive treatment outcomes.
Nursing Interventions
Medication administration and monitoring
Nurses are responsible for administering prescribed antifungal medications accurately and monitoring the patient’s response to therapy. This includes assessing for medication allergies or contraindications, educating patients about medication administration techniques, and monitoring for potential side effects. Regular follow-up assessments are essential to evaluate treatment effectiveness, ensure adherence to the prescribed regimen, and modify the plan of care if needed.
Assistance with hygiene and comfort measures
Assisting patients with hygiene and comfort measures is an essential nursing intervention in the management of yeast infections. Nurses should ensure that patients have the necessary supplies, such as mild soap, clean towels, and appropriate clothing options, to practice good hygiene. Providing guidance on proper cleansing techniques, assisting with dressing changes or application of topical medications, and addressing any discomfort or pain associated with the infection are vital aspects of nursing care.
Emotional support and counseling
Yeast infections can cause emotional distress and embarrassment for patients. Nurses should provide emotional support and counseling to help patients cope with the psychosocial aspects of their condition. Active listening, empathy, and reassurance can go a long way in alleviating anxiety or stress related to the infection. Encouraging patients to ask questions, express their concerns, and actively involving them in their care can empower them to take an active role in managing their condition.
Education and promotion of self-care practices
Patient education is a fundamental aspect of nursing care for yeast infections. Nurses should provide comprehensive education about the infection, its causes, prevention strategies, and appropriate self-care practices. This includes discussing proper hygiene techniques, appropriate clothing choices, and lifestyle modifications that can reduce the risk of recurrent infections. Patients should be encouraged to actively participate in their care by asking questions, seeking clarification, and maintaining open communication with their healthcare provider.
Documentation and Reporting
Accurate assessment documentation
Accurate and thorough documentation is essential in the nursing management of yeast infections. Nurses should document the patient’s medical history, including any previous occurrences or treatments for yeast infections. Detailed assessments, including the description of symptoms, examination findings, and diagnostic test results, should be documented accurately and objectively. This documentation provides a baseline for evaluating treatment outcomes and assists in effective communication among the healthcare team.
Recording of interventions and outcomes
Recording all nursing interventions and their outcomes is crucial for continuity of care. Nurses should document the administration of antifungal medications, any assistance provided with hygiene or comfort measures, and the patient’s response to interventions. This documentation assists in evaluating the efficacy of interventions, identifying potential areas for improvement, and facilitating interdisciplinary communication.
Communication with the healthcare team
Effective communication with the healthcare team is vital for providing optimal care to patients with yeast infections. Nurses should communicate important findings, changes in the patient’s condition or response to therapy, and any concerns or questions to the healthcare team. This includes reporting abnormal laboratory results, discussing the need for additional consultations or referrals, and collaborating on the development of an individualized plan of care for the patient.

Evaluation and Follow-up
Assessing treatment outcomes
Nurses should regularly assess and evaluate the patient’s response to treatment for yeast infections. This includes monitoring for resolution of symptoms, reduction in redness or discharge, and improvement in overall well-being. Evaluating treatment outcomes helps determine the effectiveness of the prescribed interventions and guides the need for further interventions or modifications to the plan of care.
Monitoring for recurrence
Patients who have had yeast infections are at risk for recurrence. Nurses should educate patients on the signs and symptoms of recurrent infections, such as itching, redness, or discharge, and the importance of seeking prompt medical attention if these occur. Regular follow-up assessments can help identify early signs of recurrence and facilitate immediate intervention to prevent further complications.
Continued patient education and support
Continued patient education and support are crucial in the long-term management of yeast infections. Nurses should provide ongoing education about preventive strategies, lifestyle modifications, and proper self-care practices. Patients should be encouraged to maintain open communication with their healthcare provider, seek clarification on any concerns or questions, and report any changes in their condition. Providing continuous support and encouragement throughout the patient’s journey can help them effectively manage their recurrent infections and maintain overall wellness.
Legal and Ethical Considerations
Privacy and confidentiality
Respecting patient privacy and maintaining confidentiality are essential legal and ethical considerations in the nursing management of yeast infections. Nurses should ensure that patient information and records are securely protected and only shared with authorized healthcare providers. Obtaining informed consent for any procedures, examinations, or treatments is necessary, and patients should be informed about their rights regarding privacy and confidentiality.
Informed consent for treatment
Obtaining informed consent is a legal and ethical responsibility of nurses when providing treatment for yeast infections. Nurses should explain the nature of the infection, available treatment options, potential risks and benefits, and any alternative therapies or remedies. Patients should be given ample opportunity to ask questions, seek clarification, and make informed decisions about their care. Documentation of informed consent is essential as evidence of the patient’s understanding and agreement to proceed with the recommended treatment.
Advocacy for patient rights
Nurses have a responsibility to advocate for the rights of patients with yeast infections. This includes ensuring that patients receive respectful and non-discriminatory care, have access to appropriate treatments, and are actively involved in decision-making about their care. Advocacy also involves advocating for the availability of resources and support services that can help patients manage their condition effectively, such as mental health counseling or peer support groups. Nurses should stay informed about current guidelines, best practices, and legal requirements to effectively advocate for their patients.