In the world of medical management, understanding and effectively preventing complications of acute pancreatitis is crucial to the well-being of patients. This comprehensive article explores various strategies and recommendations for preventing and managing the complications that can arise from this condition. From identifying potential risk factors to implementing appropriate treatment plans, this informative piece aims to equip healthcare professionals with the knowledge and guidance needed to provide optimal care for individuals suffering from acute pancreatitis.
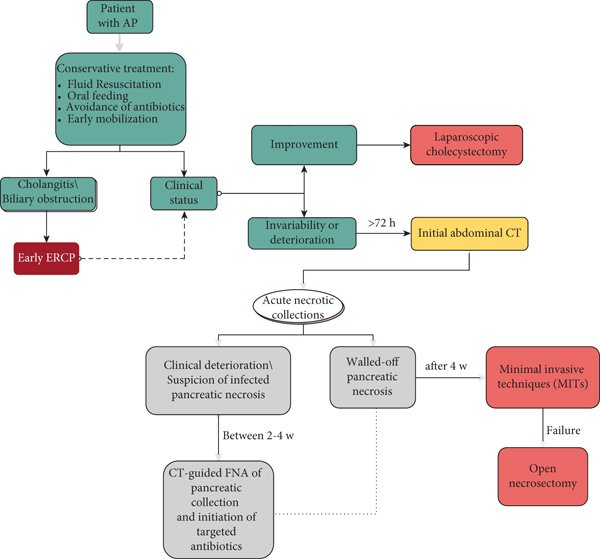
Prevention of Acute Pancreatitis Complications
Acute pancreatitis is a serious condition that can lead to complications if not properly managed. However, there are several strategies and recommendations that can help prevent these complications and ensure a better outcome for patients. In this article, we will discuss different approaches to preventing acute pancreatitis complications, including implementing lifestyle changes, identifying and treating underlying causes, and following immunization and vaccination recommendations.
Implementing Lifestyle Changes
One of the key ways to prevent complications of acute pancreatitis is by implementing certain lifestyle changes. These changes can include adopting a healthy diet that is low in fat and high in fruits and vegetables. Avoiding alcohol consumption is also crucial, as it is a leading cause of acute pancreatitis. Additionally, maintaining a healthy weight and engaging in regular exercise can reduce the risk of developing complications.
Identifying and Treating Underlying Causes
Another important aspect of preventing complications is identifying and treating the underlying causes of acute pancreatitis. This may involve investigating the patient’s medical history, conducting imaging tests, and performing blood tests to determine any potential triggers or contributing factors. Once identified, treating the underlying causes can help reduce the risk of complications and promote better healing.
Immunization and Vaccination Recommendations
Immunization and vaccination play a vital role in preventing complications of acute pancreatitis. It is recommended that individuals with acute pancreatitis receive vaccinations against diseases such as influenza, hepatitis A and B, and pneumococcal pneumonia. These vaccinations help protect the weakened immune system of individuals with acute pancreatitis and reduce the risk of acquiring additional infections that could lead to complications.
Early Recognition of Acute Pancreatitis Complications
Early recognition of complications is crucial for timely intervention and better patient outcomes in cases of acute pancreatitis. Regular monitoring and assessment of patients can help identify any signs of complications early on, allowing for prompt treatment and management.
Performing Regular Monitoring and Assessment
Healthcare providers should regularly monitor and assess patients with acute pancreatitis to identify any potential complications. This may involve conducting physical examinations, reviewing laboratory results, and performing imaging studies. By closely monitoring changes in the patient’s condition, healthcare providers can quickly identify complications and initiate appropriate interventions.
Recognizing Warning Signs and Symptoms
Recognizing the warning signs and symptoms of acute pancreatitis complications is essential for early intervention. Some common warning signs include severe abdominal pain that radiates to the back, fever, rapid heartbeat, nausea, and vomiting. Patients should be educated about these warning signs and instructed to seek immediate medical attention if they experience them. Timely recognition and intervention can significantly improve outcomes and prevent the progression of complications.

Therapeutic Management of Acute Pancreatitis Complications
Once complications of acute pancreatitis are recognized, therapeutic management becomes crucial in preventing further complications and promoting recovery. There are several specific areas of therapeutic management that should be addressed, including fluid resuscitation and electrolyte balance, pain management, antibiotics and prophylaxis, nutrition support, and surgical intervention.
Fluid Resuscitation and Electrolyte Balance
Maintaining fluid resuscitation and electrolyte balance is essential in the management of acute pancreatitis complications. Patients with acute pancreatitis often experience severe fluid loss due to vomiting and decreased oral intake. Intravenous fluids, electrolyte replacements, and close monitoring of fluid status are necessary to prevent dehydration and maintain optimal organ function.
Pain Management
Pain management is a critical aspect of therapeutic management in acute pancreatitis. Severe abdominal pain is one of the hallmark symptoms of this condition. Analgesics such as nonsteroidal anti-inflammatory drugs (NSAIDs) and opioids are commonly used to alleviate pain. However, caution must be exercised when prescribing opioids due to the risk of addiction and respiratory depression. Close monitoring and adjustment of pain medications are necessary to ensure effective pain relief while minimizing side effects.
Antibiotics and Prophylaxis
In some cases, antibiotics may be necessary to prevent or manage infections associated with acute pancreatitis complications. Prophylactic antibiotic therapy is typically recommended for patients at high risk of infected pancreatic necrosis or other related infections. The choice of antibiotics should be guided by the specific pathogens commonly associated with pancreatic infections and tailored to the patient’s individual risk factors.
Nutrition Support
Nutrition support plays a vital role in the recovery and prevention of complications in acute pancreatitis. Patients with acute pancreatitis often have impaired nutritional status due to decreased appetite, malabsorption, and increased metabolic demands. Enteral nutrition, preferably through a nasogastric or nasojejunal tube, is generally preferred over parenteral nutrition. Enteral feeding helps maintain gut integrity, reduces the risk of infection, and improves overall nutritional status.
Surgical Intervention
In severe cases or when complications do not respond to conservative management, surgical intervention may be necessary. Surgical procedures may be performed to drain pseudocysts or abscesses, remove necrotic pancreatic tissue, relieve biliary obstruction, or address other specific complications. Surgical intervention is typically performed by a specialized team and requires careful evaluation of the patient’s overall condition and risks.
Preventing Infection-related Complications
Infections are common complications of acute pancreatitis and can significantly worsen patient outcomes. Preventing infection-related complications involves implementing infection control measures and prompt antibiotic administration when necessary.
Infection Control Measures
Implementing infection control measures is essential to prevent the transmission and development of infections in patients with acute pancreatitis. These measures include proper hand hygiene, proper use of personal protective equipment, and adherence to sterile techniques during invasive procedures or dressing changes. By maintaining a clean and infection-free environment, the risk of infection-related complications can be minimized.
Prompt Antibiotic Administration
When there is a suspected or confirmed infection in acute pancreatitis, prompt administration of appropriate antibiotics is crucial. The choice of antibiotics should be guided by the likely pathogens involved and the patient’s individual risk factors. Early initiation of antibiotics can prevent the progression of infections and reduce the risk of complications such as sepsis or infected necrotizing pancreatitis.
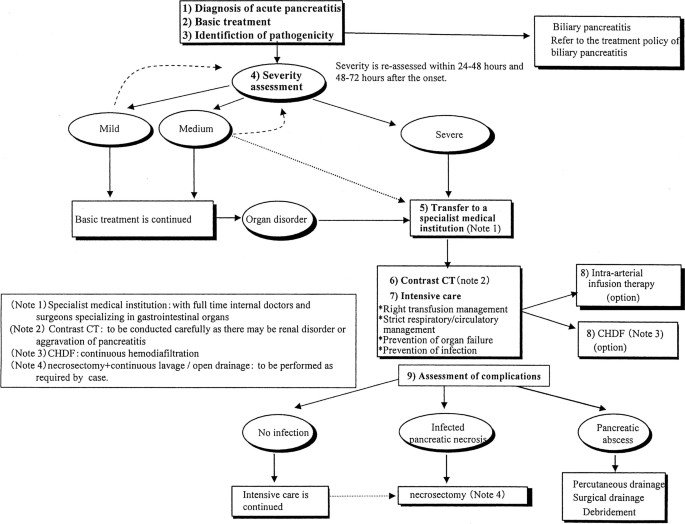
Preventing Acute Pancreatitis Recurrence
Preventing the recurrence of acute pancreatitis is essential for long-term management and the prevention of complications. This involves treating underlying causes and ensuring regular follow-up care and monitoring.
Treating Underlying Causes
Identifying and treating the underlying causes of acute pancreatitis is vital in preventing its recurrence. Common causes include gallstone disease, alcohol abuse, medication-related pancreatitis, and genetic conditions. Once the underlying cause is identified, appropriate interventions can be implemented, such as gallbladder removal for gallstone pancreatitis or alcohol cessation for alcohol-related pancreatitis.
Follow-up Care and Monitoring
Regular follow-up care and monitoring are essential to detect any signs of recurrent or ongoing pancreatitis. Patients should be advised to attend scheduled appointments and undergo any necessary tests or imaging studies. Monitoring may involve assessing pancreatic enzyme levels, conducting imaging studies to evaluate pancreatic morphology, and assessing the patient’s overall clinical status. Early detection and intervention can help prevent complications and manage any recurrent episodes effectively.
Dealing with Complications of Acute Pancreatitis
Despite prevention efforts, complications of acute pancreatitis can still occur. Effectively dealing with these complications is crucial to ensure the best possible outcomes. Here, we will discuss some common complications and their management.
Pseudocysts and Abscesses
Pseudocysts and abscesses are two common complications of acute pancreatitis. Pseudocysts are collections of fluid, tissue, and pancreatic enzymes, while abscesses are infected collections of pus. Treatment options for pseudocysts and abscesses range from conservative management to surgical drainage, depending on the size, location, and overall condition of the patient. Conservative management may involve observation, nutritional support, and medical therapy, while larger or symptomatic pseudocysts and abscesses may require surgical drainage or endoscopic intervention.
Necrotizing Pancreatitis
Necrotizing pancreatitis refers to the death of pancreatic tissue due to inflammation and subsequent infection. It is a severe complication that requires prompt intervention. Treatment options for necrotizing pancreatitis may include the use of antibiotics, surgical debridement to remove necrotic tissue, and the placement of feeding tubes to provide nutrition support. In some cases, minimally invasive procedures such as percutaneous drainage or endoscopic necrosectomy may be utilized. The management of necrotizing pancreatitis requires a multidisciplinary approach involving various specialists.
Hemorrhage
Hemorrhage is a rare but potentially life-threatening complication of acute pancreatitis. It can occur due to erosion of blood vessels by pancreatic enzymes or as a result of the rupture of an infected pseudocyst. Prompt diagnosis and intervention are crucial in managing hemorrhage. Treatment options may include blood transfusions, fluid resuscitation, surgical intervention to control bleeding, and embolization of bleeding vessels.
Pancreatic Fistula
Pancreatic fistula refers to an abnormal connection between the pancreas and another organ, typically the gastrointestinal tract. It can occur as a complication of acute pancreatitis and may lead to persistent drainage and leakage of pancreatic enzymes. Management of pancreatic fistulas may involve close observation, drainage of fluid collections, and, in some cases, surgical intervention to close the abnormal connection. Nutritional support to maintain gut rest and optimize pancreatic healing is also important in managing pancreatic fistulas.
Organ Failure
Acute pancreatitis can lead to organ failure, including respiratory failure, renal failure, and cardiovascular instability. Prompt recognition and treatment of organ failure are vital in preventing further complications and improving patient outcomes. Management may involve supportive care, such as mechanical ventilation for respiratory failure, hemodialysis for renal failure, and hemodynamic support for cardiovascular instability. Multidisciplinary collaboration and close monitoring are crucial in managing organ failure associated with acute pancreatitis.
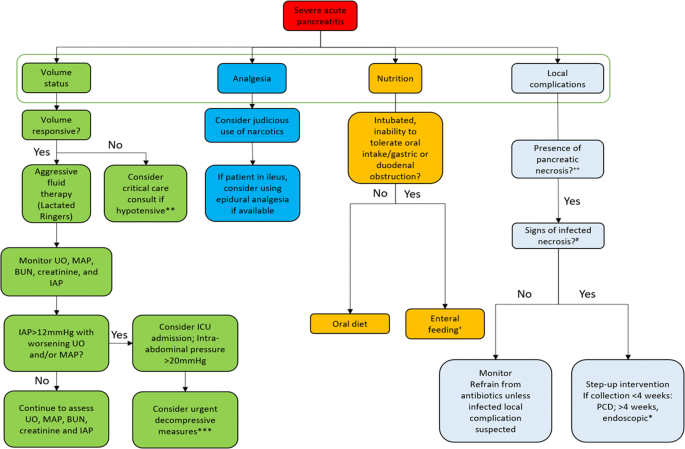
Special Considerations for High-risk Individuals
Certain population groups may be at a higher risk of complications from acute pancreatitis and require special considerations in their management.
Chronic Pancreatitis Patients
Individuals with chronic pancreatitis are at a higher risk of developing complications and require tailored management strategies. Treatment focuses on pain control, addressing nutritional deficiencies, managing exocrine and endocrine insufficiency, and preventing disease progression. Regular follow-up care, close monitoring, and multidisciplinary collaboration are necessary to provide comprehensive care to patients with chronic pancreatitis.
Pregnant Women with Acute Pancreatitis
Acute pancreatitis in pregnant women poses additional challenges due to the need to balance the care of the mother and the unborn baby. Treatment should prioritize the well-being of both individuals and may involve conservative management, careful monitoring of the woman and the fetus, and, in severe cases, surgical intervention. Obstetricians, gastroenterologists, and other specialists should collaborate closely to ensure the best outcomes for both the mother and the baby.
Pediatric Patients
Acute pancreatitis in pediatric patients requires specialized care and management tailored to their unique needs. Treatment strategies may include supportive care, nutritional support, pain management, and addressing underlying causes. Close monitoring and collaboration between pediatricians, dieticians, and other specialists are necessary to optimize outcomes and minimize complications in pediatric patients.
Role of Multidisciplinary Care Teams
The management of acute pancreatitis complications often requires the expertise of multiple healthcare professionals. A multidisciplinary care team approach ensures comprehensive and coordinated care for patients. Collaboration and communication between team members, including gastroenterologists, surgeons, radiologists, nurses, dieticians, and other specialists, is crucial to effectively manage complications, make informed decisions, and provide individualized treatment plans.
Collaboration and Communication
Effective collaboration and communication between members of the care team are key to the successful management of acute pancreatitis and its complications. Regular team meetings, case conferences, and shared decision-making ensure that all team members are up to date on the patient’s condition, treatment goals, and progress. Collaboration allows for a holistic approach to patient care and promotes the best possible outcomes.
Individualized Treatment Plans
Every patient with acute pancreatitis and its complications is unique, requiring individualized treatment plans. The multidisciplinary care team works together to develop and implement the most appropriate management strategies for each patient. These plans may include medical therapy, surgical interventions, nutrition support, pain management, and rehabilitation. By tailoring treatment to the specific needs of each patient, the care team can optimize outcomes and improve the patient’s quality of life.

Supportive Care and Patient Education
In addition to medical interventions, supportive care, and patient education play a critical role in managing acute pancreatitis complications.
Providing Psychological Support
Diagnosing and managing acute pancreatitis complications can be stressful and overwhelming for patients and their families. Providing psychological support is essential to help individuals cope with the emotional and psychological impact of the condition. This may involve access to mental health professionals, support groups, and counseling services. Addressing the psychological well-being of patients can improve their adherence to treatment plans and enhance their overall quality of life.
Dietary Modifications
Dietary modifications are often necessary to manage acute pancreatitis and prevent complications. Patients should be educated about the importance of following a low-fat, nutritious diet to avoid triggering episodes of acute pancreatitis. Avoidance of alcohol and other known triggers is essential. Dieticians can play a crucial role in providing personalized dietary recommendations and helping patients make appropriate food choices to support their recovery and prevent complications.
Educating Patients about Warning Signs
Patient education is vital in preventing complications of acute pancreatitis by empowering individuals to recognize and respond to warning signs. Patients should be educated about the common symptoms of complications, such as severe abdominal pain, fever, and rapid heartbeat. They should also be instructed on when and how to seek immediate medical attention if these symptoms arise. Timely recognition and intervention can significantly improve outcomes and prevent the progression of complications.
Importance of Timely Intervention
Timely intervention is paramount in the management of acute pancreatitis and its complications. Early diagnosis and treatment significantly impact patient outcomes and reduce the risk of severe complications.
Early Diagnosis and Treatment
Prompt diagnosis is essential in acute pancreatitis to initiate appropriate interventions and prevent complications. Early diagnosis involves a comprehensive evaluation of clinical symptoms, medical history, physical examinations, and laboratory and imaging studies. Accurate and timely diagnosis allows for the implementation of appropriate treatment strategies and close monitoring to prevent the development or progression of complications.
Prompt Referral to Specialists
Timely referral to appropriate specialists is crucial in managing acute pancreatitis complications effectively. Gastroenterologists, surgeons, interventional radiologists, and other specialists play integral roles in the diagnosis, treatment, and ongoing management of complications. Early referral ensures that patients receive the expertise and specialized care needed to optimize their outcomes.
Preventing and managing complications of acute pancreatitis requires a comprehensive approach that includes implementing lifestyle changes, identifying underlying causes, following immunization recommendations, and early recognition of complications. Therapeutic management, preventing infection-related complications, and dealing with the complications themselves require prompt and multidisciplinary care. Special considerations for high-risk individuals, supportive care, and timely interventions are vital to ensuring the best possible outcomes for patients. By prioritizing prevention, early recognition, and effective management, healthcare providers can minimize the impact of acute pancreatitis complications and improve the lives of those affected.
Watch This Video Below
Related Terms About Preventing and Managing Complications of Acute Pancreatitis
Does Acute Pancreatitis Cause Permanent Damage, Local Complications Of Acute Pancreatitis, Management Of Complications Of Acute Pancreatitis, What Complications Can Occur With Acute Pancreatitis, What Is The Most Common Complication Of Acute Pancreatitis