Imagine a world where there is a disease that can strike suddenly and cause devastating effects. This disease can be especially dangerous for children, teens, and young adults. But fear not, because there are steps you can take to protect yourself and your loved ones. In this article, we will explore the important information you need to know about preventing meningococcal disease. We will cover the symptoms, transmission methods, and most importantly, the strategies for prevention. So let’s get started on this journey to safeguard our health and well-being!

What is Meningococcal Disease?
Definition and Overview
Meningococcal disease is a severe and potentially life-threatening illness caused by the bacterium Neisseria meningitidis, also known as meningococcus. This bacterium is responsible for causing meningitis, which is the inflammation of the membranes surrounding the brain and spinal cord. Meningococcal disease can also lead to septicemia, a bloodstream infection that can cause organ damage and even death if left untreated.
Types of Meningococcal Disease
There are several different types of meningococcal disease, categorized by the specific strain of Neisseria meningitidis bacteria. Serogroups A, B, C, W, X, and Y are the most common serogroups responsible for causing disease worldwide. Each serogroup has its own unique characteristics and geographic distribution. Serogroup B, in particular, is the most prevalent cause of meningococcal disease in many countries, including the United States.
Symptoms and Signs of Meningococcal Disease
The symptoms and signs of meningococcal disease can vary depending on the age of the affected individual and the severity of the infection. Common symptoms include high fever, severe headache, stiff neck, sensitivity to light, and a purplish rash that does not fade when pressed. Other symptoms may include nausea, vomiting, confusion, and joint pain. It is essential to recognize these symptoms early and seek immediate medical attention, as meningococcal disease can progress rapidly and become life-threatening if not treated promptly.
Understanding the Causes and Transmission
The Meningococcus Bacteria
The primary bacterium responsible for meningococcal disease, Neisseria meningitidis, is typically found in the throat and nose of healthy individuals without causing any harm. However, under certain circumstances, the bacteria can invade the bloodstream and travel to the meninges, leading to the development of meningitis. The reason why certain individuals develop invasive disease while others do not is still not fully understood and is an area of ongoing research.
Modes of Transmission
Meningococcal disease is primarily transmitted through direct contact with respiratory droplets from an infected individual. This can occur through activities such as coughing, sneezing, or kissing. The bacteria are incredibly contagious, especially in crowded settings such as dormitories, military barracks, or daycare centers. Close and prolonged contact with an infected individual increases the risk of transmission.
Risk Factors for Meningococcal Disease
Although anyone can contract meningococcal disease, certain factors can increase an individual’s susceptibility to infection. These risk factors include living in close quarters with others, such as college students or military personnel, having a weakened immune system, and certain genetic factors. Additionally, individuals traveling to areas with high rates of meningococcal disease, such as the “meningitis belt” in sub-Saharan Africa, are at an increased risk.
Vaccination: The Best Defense
Vaccine Types
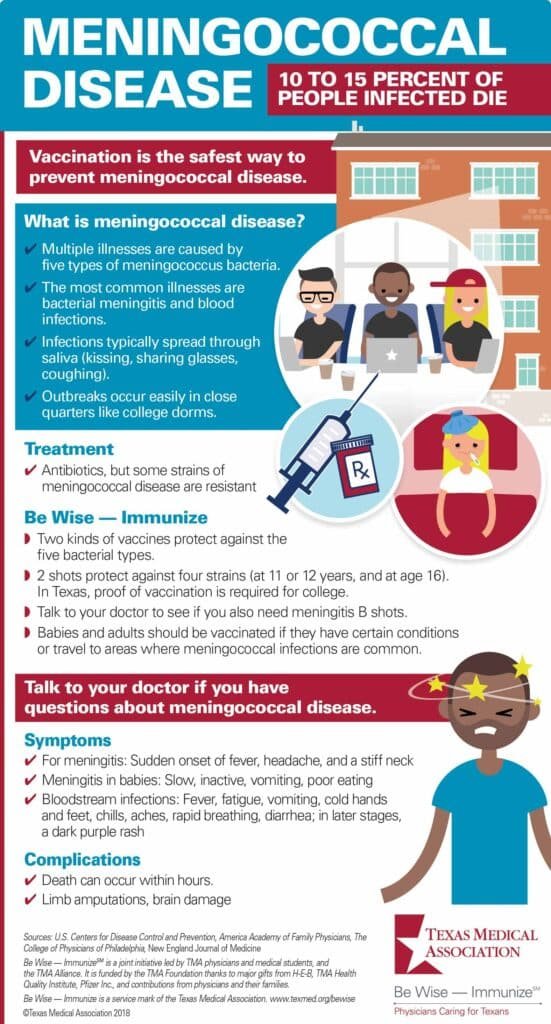
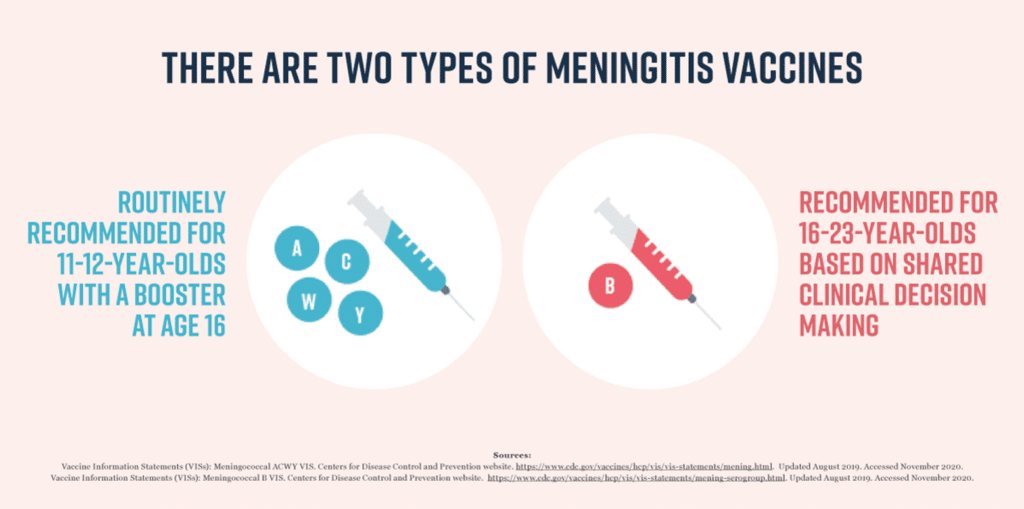
Vaccination is the most effective way to prevent meningococcal disease. There are different types of vaccines available, targeting specific serogroups of Neisseria meningitidis. The most commonly used vaccines are meningococcal conjugate vaccines, which protect against serogroups A, C, W, Y, and, in some cases, serogroup B. These vaccines stimulate the immune system to produce an immune response, providing protection against the targeted serogroups.
Recommended Schedule
The recommended vaccination schedule for meningococcal disease varies depending on the age of the individual and their risk factors. In general, infants and children should receive the routine meningococcal vaccinations as part of their childhood immunization schedule. Adolescents are also recommended to receive the meningococcal conjugate vaccine, with a booster dose in late adolescence. Additionally, individuals with weakened immune systems or certain medical conditions may require additional doses or different vaccine formulations.
Effectiveness and Duration of Protection
Meningococcal vaccines have been shown to be highly effective in preventing invasive meningococcal disease caused by the targeted serogroups. However, it is important to note that no vaccine provides 100% protection, and breakthrough cases can still occur. The duration of protection provided by the vaccines varies, with some vaccines requiring booster doses to maintain immunity over time. It is crucial to follow the recommended vaccination schedule and discuss any concerns with a healthcare provider.
Preventive Measures for Meningococcal Disease
Personal Hygiene Practices
Practicing good personal hygiene can help reduce the risk of meningococcal disease. This includes proper handwashing with soap and water, especially after coughing, sneezing, or using the restroom. Avoiding close contact with individuals who are sick or have symptoms of respiratory infections is also important. Covering your mouth and nose when coughing or sneezing with a tissue or your elbow can help prevent the spread of respiratory droplets.
Avoiding High-Risk Environments
Certain environments, such as crowded living spaces or areas with a high prevalence of meningococcal disease, carry an increased risk of transmission. Individuals should take precautions when in these settings, such as maintaining good ventilation, avoiding overcrowding, and practicing respiratory hygiene. It is also advisable to avoid sharing personal items, such as drinking cups or utensils, with individuals who may be infected.
Protective Measures during Outbreaks
During outbreaks of meningococcal disease, additional protective measures may be recommended to reduce the risk of transmission. These measures can include mass vaccination campaigns targeting high-risk populations, enhanced surveillance and testing to detect cases early, and the administration of antibiotics to close contacts of individuals with the disease. Public health authorities play a crucial role in implementing these measures to control outbreaks swiftly and effectively.
Meningococcal Disease in Different Age Groups
Infants and Young Children
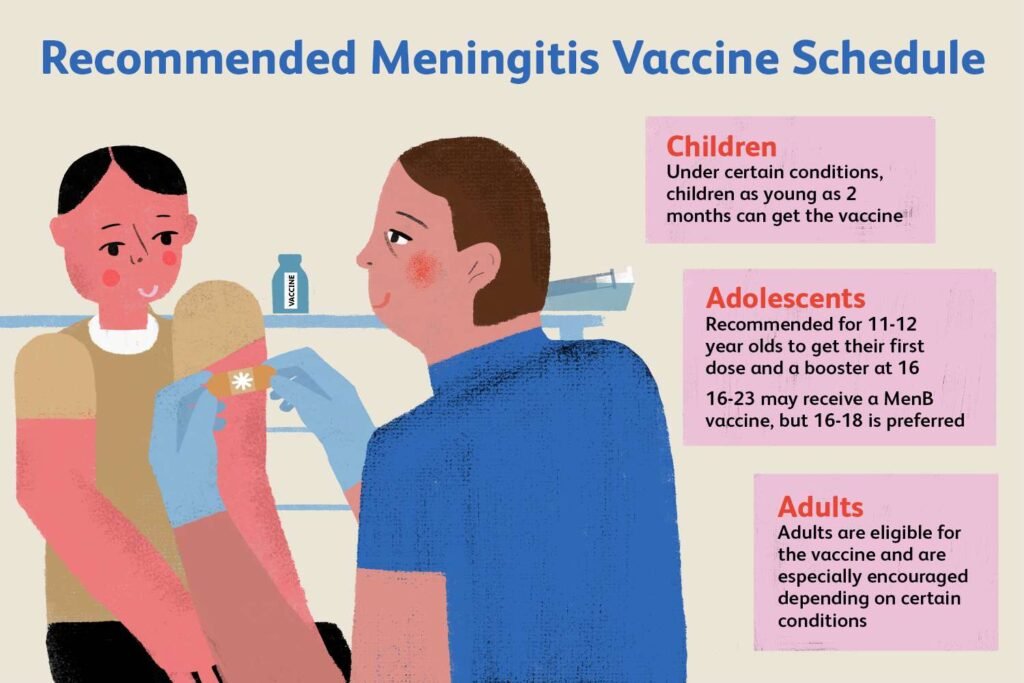
Infants and young children are particularly vulnerable to meningococcal disease due to their immature immune system. Routine immunization during early childhood is essential for protecting this age group from infection. Vaccination against meningococcal serogroups included in routine childhood immunization schedules helps provide immunity and reduce the risk of disease. It is essential for parents and caregivers to follow the recommended vaccination schedule and consult with healthcare providers regarding any concerns.
Adolescents and College Students
Adolescents and college students are at an increased risk of contracting meningococcal disease, primarily due to their close living arrangements and social activities. Vaccination against meningococcal serogroups, especially serogroups A, C, W, and Y, is recommended for this age group. Many colleges and universities require proof of meningococcal vaccination as a condition of enrollment. Additionally, promoting awareness and educating adolescents and college students about the importance of vaccination and preventive measures is crucial in reducing the incidence of meningococcal disease.
Adults
Although the risk of meningococcal disease declines in adulthood, certain individuals may still be at increased risk due to specific medical conditions or lifestyle factors. Individuals with compromised immune systems, such as those living with HIV or undergoing certain medical treatments, may have a higher susceptibility to meningococcal disease. Additionally, individuals traveling to areas with a high prevalence of meningococcal disease should consider vaccination before their trip. Consulting with a healthcare provider is essential to determine the need for vaccination based on individual risk factors.
Preventing Meningococcal Disease in Community Settings
Educational and Awareness Campaigns
Educational campaigns play a crucial role in raising awareness about meningococcal disease, its symptoms, and the importance of vaccination. Public health organizations, schools, and community groups can collaborate to disseminate accurate and up-to-date information through various channels, such as social media, educational materials, and community events. Promoting awareness helps empower individuals to take preventive measures, seek timely medical attention, and adhere to recommended vaccination schedules.
Routine Vaccination Programs
Implementing routine vaccination programs is an effective strategy to prevent meningococcal disease at the community level. Many countries have incorporated meningococcal vaccines into their national immunization schedules, targeting young children, adolescents, and other high-risk groups. These programs aim to ensure widespread vaccine coverage, reduce the incidence of disease, and protect vulnerable populations. Regular monitoring and evaluation of vaccination coverage and disease surveillance are essential to assess the effectiveness of these programs and identify areas for improvement.
Contact Tracing and Monitoring
When meningococcal disease cases occur in a community setting, contact tracing and monitoring become crucial to prevent further transmission. Identifying and notifying close contacts of infected individuals allows for targeted vaccination or antibiotic prophylaxis to interrupt disease transmission. Close monitoring of affected individuals and the community can help identify potential outbreaks and guide public health interventions. Collaboration between healthcare providers, public health authorities, and affected communities is essential for effective contact tracing and monitoring efforts.
Meningococcal Disease and Travel
Traveling to High-risk Areas
Certain regions of the world, such as the “meningitis belt” in sub-Saharan Africa, have a higher prevalence of meningococcal disease. Travelers planning to visit these areas should be aware of the risk and take appropriate precautions. It is advisable to consult healthcare providers or travel medicine specialists well in advance of travel to discuss the need for meningococcal vaccination and other preventive measures. Additionally, following standard hygiene practices and avoiding crowded areas can help reduce the risk of exposure.
Vaccination Requirements
Some countries may require proof of meningococcal vaccination as a condition of entry, especially for travelers coming from areas with high rates of meningococcal disease. It is important to check the vaccination requirements of the destination country before travel and ensure compliance with any necessary immunizations. Keeping an updated vaccination record and carrying necessary documents while traveling can help ensure a smoother entry process and protect against potential health risks.
Precautions for Travelers
Travelers can take several precautions to reduce the risk of meningococcal disease while abroad. In addition to receiving the recommended vaccinations, practicing good personal hygiene, such as regular handwashing and proper respiratory etiquette, is crucial. Avoiding close contact with individuals who are visibly ill or have respiratory symptoms is advisable. Travelers should also be aware of the signs and symptoms of meningococcal disease to seek prompt medical attention if necessary.
Diagnosis and Treatment of Meningococcal Disease
Recognizing the Symptoms
Prompt recognition of the symptoms of meningococcal disease is essential for early diagnosis and treatment. Symptoms such as high fever, severe headache, stiff neck, and a purplish rash that does not fade under pressure should raise concerns. If these symptoms are present, it is crucial to seek immediate medical attention in an emergency setting. Early treatment can significantly improve outcomes and reduce the risk of complications.
Diagnostic Tests
Once a suspected case of meningococcal disease is identified, healthcare providers may order various diagnostic tests to confirm the infection and determine the specific serogroup involved. These tests can include blood cultures, cerebrospinal fluid (CSF) analysis, polymerase chain reaction (PCR) testing, and serological assays. Prompt and accurate diagnosis allows for appropriate treatment and the initiation of public health interventions to prevent further transmission.
Antibiotic Treatment
Meningococcal disease is a medical emergency that requires immediate treatment with antibiotics. The specific choice of antibiotics will depend on the local antimicrobial resistance patterns and the suspected serogroup involved. Early initiation of antibiotics can help control the infection, prevent complications, and reduce the risk of death. Close monitoring of the patient’s clinical progress is necessary to ensure the effectiveness of treatment and manage any potential complications.
Preventing Meningococcal Disease Complications
Prompt Medical Attention
Seeking prompt medical attention for suspected meningococcal disease is crucial to minimize the risk of complications. Delayed diagnosis and treatment can lead to a more severe illness and increase the likelihood of long-term complications or death. If you or someone you know experiences symptoms suggestive of meningococcal disease, do not hesitate to visit the nearest emergency department or call your local emergency number.
Supportive Care
In addition to antibiotic treatment, supportive care plays an important role in managing meningococcal disease. This can include measures such as adequate fluid and electrolyte management, pain relief, and close monitoring of vital signs and organ function. Depending on the severity of the infection, hospitalization may be necessary to provide the necessary medical care and ensure a favorable outcome.
Potential Long-term Effects
While prompt diagnosis and treatment can minimize the risk of complications, some individuals may experience long-term effects following meningococcal disease. These can include neurological deficits, such as hearing loss, cognitive impairment, or seizures. Rehabilitation and follow-up care may be necessary to address and manage these complications. It is essential for individuals who have recovered from meningococcal disease to discuss any ongoing concerns with their healthcare provider.
Case Studies and Outbreak Management
Notable Meningococcal Disease Outbreaks
Throughout history, there have been several notable outbreaks of meningococcal disease. One such example is the meningitis belt in sub-Saharan Africa, where large-scale epidemics occur periodically. These outbreaks are often associated with overcrowded living conditions, limited healthcare access, and other socioeconomic factors. Other notable outbreaks have occurred in college campuses, military barracks, and other community settings. These outbreaks highlight the importance of vaccination, early detection, and swift public health response.
Emergency Response and Public Health Measures
When a meningococcal disease outbreak or cluster occurs, a coordinated emergency response is crucial to limit the spread of the disease and protect the affected population. Public health authorities work closely with healthcare providers, laboratories, and other stakeholders to implement rapid response measures. These measures may include contact tracing, mass vaccination campaigns, enhanced surveillance, and public education campaigns. Timely communication and collaboration between all involved parties are vital for effective outbreak management.
Lessons Learned
Each meningococcal disease outbreak presents an opportunity to learn valuable lessons and improve future response efforts. Outbreak investigations help identify gaps in surveillance, diagnostic capabilities, and public health response strategies. Collaboration between local, national, and international health agencies can help identify emerging trends, explore innovative prevention strategies, and share best practices. These lessons learned contribute to ongoing research and policy development, ultimately improving the global response to meningococcal disease.
In conclusion, meningococcal disease is a serious and potentially life-threatening infection caused by an intransigent bacterium called Neisseria meningitidis. Understanding the causes, modes of transmission, and symptoms of meningococcal disease is crucial in preventing its spread and minimizing its impact on individuals and communities. Vaccination remains the most effective strategy to protect against the disease, with different vaccines available for different age groups and risk factors. Emphasizing personal hygiene practices, avoiding high-risk environments, and implementing preventive measures during outbreaks are other important steps in reducing the incidence of meningococcal disease. By implementing comprehensive public health strategies, including routine vaccination programs, educational campaigns, and emergency response measures, we can strive towards a future where meningococcal disease is no longer a global health threat.