In this article, “The Devastating Effects of Sepsis,” we explore the grim consequences of blood poisoning, also known as sepsis. With lives claimed and bodies ravaged, sepsis poses a severe threat to individuals worldwide. Uncover the haunting reality of this condition as we delve into its destructive impact on the human body. Brace yourself for a sobering journey that sheds light on the devastating effects of sepsis.

Definition of Sepsis
Globally Accepted Definition
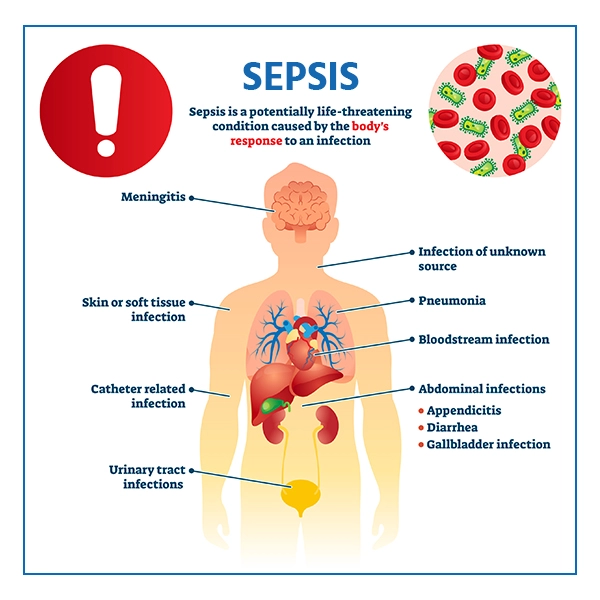
Sepsis is a potentially life-threatening condition that arises when the body’s response to an infection injures its own tissues and organs. The Global Sepsis Alliance defines sepsis as “life-threatening organ dysfunction caused by a dysregulated host response to infection.”
Symptoms of Sepsis
Sepsis can present with a wide range of symptoms, some of which may be subtle at first. Common signs include fever, increased heart rate, rapid breathing, confusion, extreme fatigue, dizziness, and decreased urine output. In severe cases, it can progress rapidly to septic shock, characterized by low blood pressure, decreased oxygen delivery to organs, and compromised organ function.
Causes and Risk Factors
Bacterial Infections
Bacterial infections are a leading cause of sepsis. Common examples include urinary tract infections, pneumonia, cellulitis, and abdominal infections. If left untreated, these infections can spread throughout the body and trigger a systemic inflammatory response, leading to sepsis.
Other Types of Infections
While bacterial infections are the primary culprits, sepsis can also arise from other types of infections, such as viral or fungal infections. In rare cases, parasites can also cause sepsis.
Weakened Immune System
Individuals with weakened immune systems, such as those with HIV/AIDS, cancer, or under immunosuppressive medications, are at a higher risk of developing sepsis. Their bodies may struggle to mount an effective immune response to combat the infection.
Hospitalization
Hospital-acquired infections pose a significant risk for sepsis. Patients with invasive medical devices, such as central venous catheters or urinary catheters, are more prone to infections that can progress to sepsis.
Chronic Illnesses
Chronic illnesses, such as diabetes, kidney disease, liver disease, and lung disease, can weaken the body’s defenses and make individuals more susceptible to infections that can lead to sepsis.
Age
Extreme age groups, particularly the elderly and infants, are more vulnerable to sepsis due to their developing or weakened immune systems, respectively. It is crucial to closely monitor these populations for signs of infection and initiate prompt treatment to prevent sepsis.
Pathophysiology of Sepsis
Infection and Immune Response
Sepsis begins with an infection, which triggers the body’s immune response. Normally, immune cells release various signaling molecules to fight off the infection. However, in sepsis, an uncontrolled release of these molecules occurs, resulting in widespread inflammation that can damage organs and impair their function.
Systemic Inflammatory Response Syndrome (SIRS)
SIRS is a condition closely related to sepsis and can be seen as an early warning sign. The criteria for SIRS include abnormal body temperature (fever or hypothermia), increased heart rate, increased respiratory rate, and abnormal white blood cell count. Sepsis occurs when SIRS is present in the setting of an infection.
Complications of Sepsis
Sepsis can have severe consequences if not promptly recognized and treated. It can progress to septic shock, where the body’s organs are unable to receive adequate blood flow and oxygen. This can lead to organ dysfunction or failure, potentially affecting the lungs, kidneys, liver, heart, and brain. Additionally, sepsis survivors may experience long-term effects, such as post-sepsis syndrome and mental health issues.
Diagnosis and Clinical Presentation
Physical Examination
Diagnosing sepsis requires a thorough physical examination. The healthcare provider will evaluate vital signs, check for signs of infection (such as localized redness or swelling), and assess organ function. They will look for specific signs that suggest sepsis, such as altered mental status, low blood pressure, and abnormal heart or lung sounds.
Laboratory Tests
Laboratory tests play a crucial role in confirming a suspected diagnosis of sepsis. Blood cultures can identify the pathogens causing the infection, while complete blood count and inflammatory markers (such as C-reactive protein and procalcitonin) can help assess the body’s response to infection.
Diagnostic Criteria
To diagnose sepsis, healthcare professionals rely on specific criteria. The Sequential Organ Failure Assessment (SOFA) score assesses organ function, while the quick Sepsis-related Organ Failure Assessment (qSOFA) score aids in the quick identification of patients at high risk for sepsis. Other criteria, such as the Systemic Inflammatory Response Syndrome (SIRS) criteria, can also be used.

Long-Term Effects of Sepsis
Organ Dysfunction and Failure
Sepsis can have long-lasting impacts on organ function. Depending on the severity and duration of the infection, organs such as the lungs, kidneys, liver, heart, and brain may experience varying degrees of damage. This can lead to chronic organ dysfunction or even organ failure, requiring ongoing medical management.
Post-Sepsis Syndrome
Post-sepsis syndrome refers to a collection of physical, cognitive, and emotional symptoms that may persist following sepsis. Fatigue, muscle weakness, and difficulty concentrating are common physical symptoms, while anxiety, depression, and post-traumatic stress disorder (PTSD) can affect a person’s mental health. Rehabilitation and support are vital for individuals recovering from post-sepsis syndrome.
Mental Health Issues
Sepsis survivors may develop mental health issues, including anxiety and depression, as a result of the traumatic experience. The critical illness, the prolonged hospitalization, and the potential loss of loved ones during the sepsis episode can take a toll on a person’s mental well-being. Access to mental health support is essential for holistic recovery.
Risk of Recurrence
While the majority of sepsis cases resolve with appropriate treatment, there is a risk of recurrence. Individuals with underlying chronic illnesses, weakened immune systems, or a history of previous sepsis episodes are especially susceptible. It is crucial for healthcare providers to closely monitor and manage these high-risk patients to prevent future episodes.
Treatment and Management
Early Recognition and Antibiotics
Early recognition and prompt treatment are of utmost importance in managing sepsis. Healthcare providers must identify the signs and symptoms of sepsis and initiate appropriate antibiotics as soon as possible. Timing is crucial to halt the progression of the infection and prevent organ damage.
Supportive Care
In addition to antibiotics, supportive care is crucial for sepsis management. This includes ensuring adequate oxygenation, fluid resuscitation to maintain blood pressure, and close monitoring of vital signs and organ function. Supportive care may also involve providing pain relief, nutrition, and addressing any underlying medical conditions.
Intensive Care Unit (ICU) Management
Severe cases of sepsis often necessitate management in an intensive care unit. In the ICU, patients receive specialized monitoring, close observation, and interventions such as vasopressor medications to maintain blood pressure and mechanical ventilation for respiratory support.
Sepsis Bundles
Sepsis bundles are evidence-based protocols that outline specific steps for healthcare providers to follow in the diagnosis and treatment of sepsis. They aim to standardize care, promote timely interventions, and improve patient outcomes. Examples include the Surviving Sepsis Campaign bundles, which provide guidelines for delivering optimal care to septic patients.
Rehabilitation and Recovery
For sepsis survivors, comprehensive rehabilitation and recovery programs are essential. These programs may involve physical therapy to regain strength and function, occupational therapy to improve daily living skills, and psychological support to address any mental health issues. The goal is to enhance overall well-being and aid in the return to pre-sepsis levels of function.

Prevention and Awareness
Proper Hand Hygiene
Hand hygiene is one of the most effective ways to prevent infections and reduce the risk of sepsis. Regularly washing hands with soap and water for at least 20 seconds, or using alcohol-based hand sanitizers, helps eliminate harmful bacteria and viruses.
Vaccinations
Vaccinations play a vital role in preventing infections that can lead to sepsis. Vaccines for influenza, pneumococcus, meningococcus, and other infections are recommended for individuals of all ages, especially those at high risk, such as the elderly and those with chronic illnesses.
Infection Control Measures
Implementing robust infection control measures in healthcare settings is crucial in preventing hospital-acquired infections. This includes proper disinfection of equipment, adherence to aseptic techniques during procedures, and strict adherence to infection prevention and control guidelines.
Educating Healthcare Professionals
Continuing education and training programs for healthcare professionals are essential to increase awareness and knowledge of sepsis. Training should focus on early recognition, proper diagnosis, and evidence-based management strategies. This ensures that healthcare providers are equipped to deliver optimal care to septic patients.
Public Awareness Campaigns
Raising public awareness about sepsis is paramount to improving outcomes. Public awareness campaigns can educate individuals about the signs and symptoms of sepsis, the importance of seeking timely medical attention, and the role of preventive measures such as vaccinations and hand hygiene.
Public Health Impact
Global Burden of Sepsis
Sepsis is a major global health concern, affecting millions of people each year. It is estimated that there are over 30 million cases of sepsis worldwide annually, with a significant number of deaths attributed to the condition. The burden of sepsis is substantial, both in terms of human suffering and healthcare resources.
Economic Costs
The economic costs associated with sepsis are immense. Sepsis treatment often requires intensive care, prolonged hospital stays, and a range of medical interventions. These expenses, coupled with the long-term effects and disability caused by sepsis, can have a significant impact on healthcare systems, families, and economies.
Healthcare Resource Utilization
Sepsis places a considerable strain on healthcare resources and infrastructure. It necessitates specialized monitoring, laboratory investigations, and often requires management in intensive care units. The demand for resources, including medications, equipment, and healthcare personnel, increases significantly when dealing with sepsis cases.
Impact on Patients and Families
Sepsis has a profound impact on affected individuals and their families. Not only does it cause physical and psychological distress, but it can also lead to long-term disability, loss of income, and increased healthcare expenses. The support and understanding of healthcare providers, family members, and the community are crucial in helping patients and their families navigate the challenges of sepsis.

Research and Advances
Improved Diagnostic Tools
Ongoing research aims to develop improved diagnostic tools for sepsis. These tools might include biomarkers, genomic testing, and imaging techniques to aid in earlier detection and accurate diagnosis. Early diagnosis allows for timely intervention and treatment, potentially improving outcomes for septic patients.
New Treatment Approaches
Researchers are continuously exploring new treatment approaches for sepsis. This includes developing targeted therapies, such as immunomodulatory medications, to prevent the excessive inflammatory response associated with sepsis. There is also ongoing investigation into the potential benefits of adjunctive therapies, such as probiotics and stem cell therapy.
Sepsis Surveillance Systems
Sepsis surveillance systems are being developed and implemented to monitor the incidence and outcomes of sepsis. These systems enable healthcare providers to track trends, identify high-risk populations, and implement targeted interventions. By improving data collection and analysis, healthcare systems can optimize sepsis prevention and management strategies.
Education and Training Programs
Education and training programs for healthcare professionals are continuously evolving to incorporate the latest evidence and guidelines pertaining to sepsis management. These programs promote knowledge, skill development, and adherence to best practices. Continued education ensures that healthcare providers are equipped to deliver high-quality care to sepsis patients.
Conclusion
Recognizing the Devastating Impact
Sepsis is a devastating condition that affects millions of people worldwide, with significant morbidity and mortality rates. It is crucial for both healthcare professionals and the general public to recognize the signs and symptoms of sepsis to ensure early detection and timely treatment.
Call to Action for Healthcare Systems
Given the global burden and impact of sepsis, there is a pressing need for healthcare systems to prioritize sepsis prevention, recognition, and management. This includes comprehensive sepsis protocols, ongoing education, and the development of effective surveillance systems. By working together, we can reduce the burden of sepsis and improve outcomes for patients worldwide.