Clostridium Difficile, commonly known as C. Difficile, poses an alarming and increasing threat to public health. This bacterial infection primarily targets the colon and causes severe diarrhea, often leading to complications and even death. With its prevalence soaring in hospitals, nursing homes, and other healthcare facilities, it is essential to understand the risks, symptoms, and preventative measures against C. Difficile. In this article, we will explore the growing concern surrounding this formidable pathogen and the efforts being made to combat its spread.

Overview of Clostridium Difficile
What is Clostridium Difficile?
Clostridium difficile, commonly referred to as C. difficile or C. diff, is a bacterium that can cause a range of symptoms from mild diarrhea to severe life-threatening conditions. It is a spore-forming bacterium that is known to be resistant to many commonly used disinfectants and can survive for extended periods on surfaces.
Prevalence of Clostridium Difficile
Clostridium difficile infections have been on the rise in recent years, making it a growing public health concern. It is estimated that there are approximately half a million cases of C. difficile infections in the United States each year, resulting in thousands of deaths. The prevalence of C. difficile varies across different healthcare settings, with hospitals and long-term care facilities being high-risk environments.
Transmission of Clostridium Difficile
The primary mode of transmission for C. difficile is the fecal-oral route. The bacterium is present in the stool of infected individuals and can be spread through direct contact with contaminated surfaces or objects. Healthcare settings provide ample opportunities for transmission due to the close proximity of patients, frequent use of antibiotics, and inadequate adherence to infection control measures.
Risk Factors for Clostridium Difficile Infection
Advanced Age
One significant risk factor for developing a Clostridium difficile infection is advanced age. Older adults, particularly those over the age of 65, are more susceptible to C. difficile due to weakened immune systems and higher prevalence of underlying health conditions. The likelihood of severe complications and poor outcomes is also increased in this age group.
Hospitalization
Hospitalization is another risk factor for acquiring a Clostridium difficile infection. The prolonged exposure to healthcare settings, where C. difficile is often present, increases the chances of colonization and infection. The use of invasive procedures, indwelling devices, and broad-spectrum antibiotics in a hospital setting further contribute to the risk.
Antibiotic Use
Antibiotic use is a significant risk factor for the development of C. difficile infection. Antibiotics can disrupt the balance of the gut microbiota, allowing C. difficile to flourish and cause infection. Certain antibiotics, such as clindamycin, fluoroquinolones, and broad-spectrum cephalosporins, have been associated with an increased risk of C. difficile infection.
Gastrointestinal Surgery
Individuals who have undergone gastrointestinal surgery are at an increased risk of developing a C. difficile infection. The disruption of the normal gastrointestinal flora during surgery, combined with the use of antibiotics and prolonged hospital stays, creates an environment favorable for C. difficile colonization and infection.
Immunosuppression
Immunosuppression, whether due to underlying medical conditions or medication use, increases the risk of C. difficile infection. A weakened immune system is less able to fight off the bacterium, leading to a higher likelihood of infection and severe disease. Conditions such as HIV/AIDS, organ transplantation, and cancer treatment can significantly increase the risk of C. difficile infection.

Symptoms and Complications of Clostridium Difficile Infection
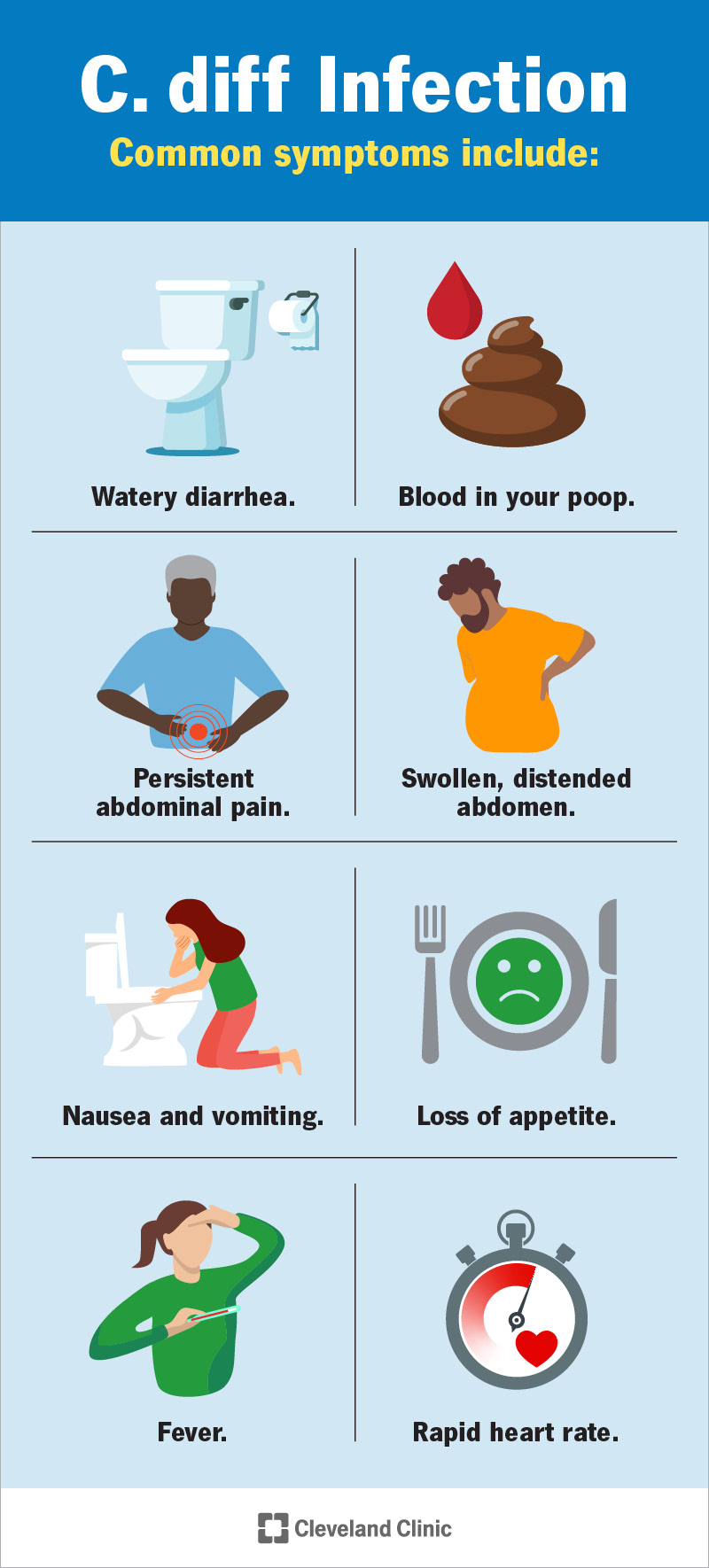
Mild Symptoms
Clostridium difficile infection can present with a range of symptoms, from mild to severe. Mild cases often manifest as diarrhea, which may be watery or have a loose consistency. Other symptoms may include abdominal cramping, bloating, and a mild fever. The severity and duration of symptoms can vary from person to person.
Severe Symptoms
In severe cases, Clostridium difficile infection can lead to more severe symptoms and complications. Severe diarrhea, often accompanied by blood or pus, is a hallmark of severe disease. Abdominal pain, fever, dehydration, and weight loss may also be present. In some cases, C. difficile infection can progress to a life-threatening condition known as pseudomembranous colitis.
Complications
Complications of Clostridium difficile infection can be severe and potentially life-threatening. These may include toxic megacolon, a condition characterized by severe inflammation and dilation of the colon, as well as bowel perforation. In some cases, C. difficile infection can lead to sepsis, a widespread infection that can be fatal if not promptly treated.
Diagnosis of Clostridium Difficile Infection
Physical Examination
The diagnosis of Clostridium difficile infection begins with a thorough physical examination. The healthcare provider will evaluate the patient’s symptoms, medical history, and potential risk factors. Abdominal tenderness or distention may be present, along with signs of dehydration or systemic illness.
Laboratory Tests
Laboratory tests play a critical role in the diagnosis of Clostridium difficile infection. The most commonly used test is the detection of the C. difficile toxin in the stool sample. This can be done through various methods, including enzyme immunoassays or polymerase chain reaction (PCR) tests. In some cases, a stool culture may be performed to isolate and identify the bacterium.
Other Diagnostic Methods
In certain situations, additional diagnostic methods may be necessary for confirming a Clostridium difficile infection. These may include endoscopic evaluation of the colon, such as colonoscopy or sigmoidoscopy, to assess the extent of inflammation and pseudomembranes. Imaging studies, such as abdominal CT scans, can help identify complications like toxic megacolon.
Treatment of Clostridium Difficile Infection
Antibiotic Therapy
The primary treatment for Clostridium difficile infection involves the use of specific antibiotics. Oral vancomycin and fidaxomicin are commonly prescribed antibiotics that target C. difficile. Metronidazole may also be used for mild to moderate cases. The duration and choice of antibiotics may vary depending on the severity of the infection, previous treatment response, and other individual factors.
Supportive Care
In addition to antibiotic therapy, supportive care is essential for the management of Clostridium difficile infection. This includes maintaining hydration with oral rehydration solutions or intravenous fluids if necessary. In severe cases, hospitalization may be required to provide close monitoring and supportive interventions.
Fecal Microbiota Transplantation
Fecal microbiota transplantation (FMT) is an emerging treatment option for recurrent or refractory Clostridium difficile infection. It involves the transfer of fecal material from a healthy donor into the gastrointestinal tract of the infected individual. By restoring a healthy microbiota balance, FMT can help eliminate C. difficile and prevent recurrent infections.
Surgical Intervention
In rare cases where medical treatment fails or complications arise, surgical intervention may be necessary. This can include surgical removal of the affected portion of the colon or creation of an ostomy. Surgery is typically reserved for severe cases with complications that do not respond to medical management.
Prevention and Control Measures
Hand Hygiene
Hand hygiene is crucial in preventing the transmission of Clostridium difficile. Healthcare workers should adhere to proper hand hygiene practices, including the use of soap and water or alcohol-based hand sanitizers when soap is not available. Hand hygiene should be performed before and after patient contact, after using the restroom, and before handling food.
Appropriate Antibiotic Use
Appropriate antibiotic use is essential in preventing the development of Clostridium difficile infection. Healthcare providers should follow guidelines for prescribing antibiotics, including proper dosage, duration, and selection based on the specific infection being treated. Overuse or misuse of antibiotics can disrupt the normal gut flora and increase the risk of C. difficile infection.
Isolation Precautions
Isolation precautions are necessary to prevent the spread of Clostridium difficile in healthcare settings. Infected individuals should be placed in a single-patient room whenever possible, with dedicated equipment that is not shared with others. Healthcare workers should wear appropriate personal protective equipment, including gloves and gowns, when caring for patients with C. difficile infection.
Environmental Cleaning
Thorough and frequent environmental cleaning is essential in preventing the spread of Clostridium difficile. Surfaces should be cleaned using a bleach-based disinfectant or other sporicidal agents that are effective against C. difficile spores. High-touch surfaces, such as bedrails, doorknobs, and bedside tables, should receive extra attention.
Vaccination
Currently, there is no specific vaccine available for the prevention of Clostridium difficile infection. However, research is underway to develop vaccine candidates that could potentially reduce the risk of infection or decrease the severity of illness in those who develop the infection.
Emerging Strains and Antibiotic Resistance
NAP1/BI/027 Strain
The NAP1/BI/027 strain of Clostridium difficile, also known as the “hypervirulent” strain, has gained attention due to its increased virulence and ability to cause severe disease. This strain is associated with higher mortality rates and an increased likelihood of recurrence. It is also more resistant to certain antibiotics, making treatment more challenging.
Hypervirulent Strains
Apart from the NAP1/BI/027 strain, other hypervirulent strains of Clostridium difficile have also been identified. These strains possess additional toxins that contribute to increased virulence and severity of disease. Monitoring and surveillance for these emerging strains are essential for early detection and appropriate management of C. difficile infections.
Antibiotic Resistance
Clostridium difficile has been increasingly associated with antibiotic resistance. The overuse and misuse of antibiotics have contributed to the development of multidrug-resistant strains. This poses a significant challenge in providing effective treatment for C. difficile infections, highlighting the importance of judicious antibiotic use and development of alternative therapies.
Impact of Clostridium Difficile Infection
Healthcare Burden
Clostridium difficile infection imposes a significant healthcare burden, particularly in hospital settings. It leads to increased hospital stays, utilization of healthcare resources, and healthcare costs. The management of C. difficile infection requires dedicated infection control measures, interventions, and monitoring, which contribute to the workload of healthcare providers.
Economic Costs
The economic costs associated with Clostridium difficile infection are substantial. Hospitalizations, treatment, and complications of C. difficile infection result in increased healthcare expenditures. Moreover, the indirect costs due to lost productivity and economic burden on individuals affected by the infection further contribute to the economic impact.
Patient Morbidity and Mortality
Clostridium difficile infection can have significant morbidity and mortality. Severe cases, especially those with complications and recurrence, can lead to prolonged hospital stays, worsening health outcomes, and increased risk of death. Older adults and those with underlying health conditions are particularly vulnerable and at higher risk for adverse outcomes.
Research and Future Directions
Development of New Therapies
Ongoing research aims to develop new therapies for the prevention and treatment of Clostridium difficile infection. This includes the exploration of novel antibiotics, alternative antimicrobial agents, and immunotherapeutic approaches. The development of targeted therapies that specifically inhibit C. difficile without disrupting the normal gut microbiota is a promising area of investigation.
Improved Diagnostic Methods
Efforts are underway to improve diagnostic methods for Clostridium difficile infection. This includes the development of rapid and accurate tests that can quickly detect C. difficile toxins or genetic markers. The utilization of advanced technologies, such as next-generation sequencing, may provide valuable insights into the epidemiology and transmission dynamics of C. difficile infections.
Enhanced Infection Control Strategies
Enhanced infection control strategies are essential to prevent the spread of Clostridium difficile. Ongoing research aims to identify effective measures to reduce the transmission of C. difficile spores, improve hand hygiene practices, and optimize environmental cleaning procedures. The implementation of bundled interventions and strict adherence to infection control guidelines can help mitigate the risk of C. difficile infection.
Conclusion
Clostridium difficile infection is a significant and growing threat to public health. It poses a substantial burden on healthcare systems, with the potential for severe complications and adverse outcomes. Understanding the risk factors, symptoms, diagnostic methods, and treatment options is crucial for the prevention and management of C. difficile infections. Ongoing research and implementation of effective infection control measures are necessary to address this growing problem and reduce the impact of C. difficile in healthcare settings and the community as a whole.