Bronchiectasis, a condition that affects the health of your lungs, can often be overlooked or misunderstood. In this article, we will shed light on the impact that bronchiectasis can have on your lung health, and provide you with the essential information you need to understand this condition. Whether you or a loved one are dealing with bronchiectasis or simply want to be well-informed, we’ve got you covered. Get ready to gain a deeper understanding of bronchiectasis and its effects on your overall well-being.
What is Bronchiectasis
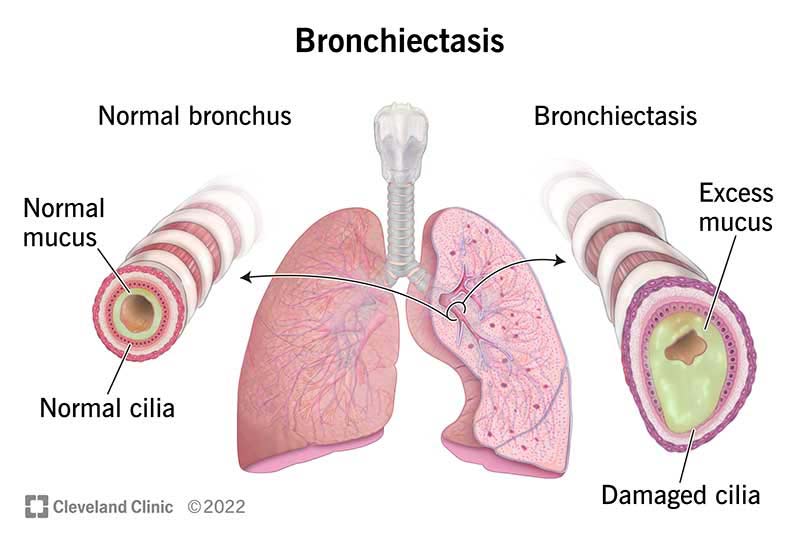
Bronchiectasis is a chronic lung condition characterized by the permanent enlargement and damage of the bronchial tubes, which are the airways that carry air in and out of the lungs. This condition is the result of repeated infections and inflammation that cause the walls of the bronchial tubes to become thickened and weakened, leading to a loss of elasticity. As a result, the airways become dilated and are unable to clear mucus effectively, thus leading to a buildup of mucus and increased susceptibility to infections. Bronchiectasis can have a significant impact on lung function and overall respiratory health.
Definition
Bronchiectasis is a respiratory condition that is marked by the abnormal and irreversible widening of the bronchial tubes. This permanent dilation of the airways is caused by damage to the bronchial walls, which leads to the accumulation of mucus and an increased risk of lung infections. The condition can affect both children and adults and can be either congenital (present from birth) or acquired (developed later in life). It is important to note that bronchiectasis is a chronic condition that requires ongoing management and treatment to prevent further damage and complications.
Causes
Bronchiectasis can be caused by a variety of factors. In some cases, it is the result of an underlying medical condition or genetic predisposition, while in others, it may be caused by repeated respiratory infections. Common causes of bronchiectasis include:
- Chronic infections, such as recurrent pneumonia or tuberculosis
- Respiratory conditions, such as chronic obstructive pulmonary disease (COPD) or asthma
- Immunodeficiency disorders, such as common variable immunodeficiency (CVID)
- Genetic factors, such as cystic fibrosis or alpha-1 antitrypsin deficiency
It is essential to identify and address the underlying cause of bronchiectasis to ensure appropriate management and treatment.
Symptoms
The symptoms of bronchiectasis can vary depending on the severity of the condition and the extent of lung damage. Common symptoms include:
- Chronic cough, often accompanied by large amounts of mucus production
- Recurrent respiratory infections, such as bronchitis or pneumonia
- Shortness of breath, particularly during physical activity
- Fatigue and general weakness
- Wheezing or a whistling sound when breathing
- Chest pain
- Clubbing of the fingers or toes (enlarged fingertips or toenails)
It is important to note that bronchiectasis symptoms can worsen over time if left untreated, leading to more frequent and severe lung infections and a decline in overall respiratory health.
Diagnosis
The diagnosis of bronchiectasis involves a combination of medical history evaluation, physical examination, and specialized tests. Your healthcare provider will start by asking about your symptoms, medical history, and any risk factors you may have. They will then perform a physical examination, which may involve listening to your lungs with a stethoscope to identify abnormal breath sounds.
To confirm the diagnosis, your healthcare provider may order one or more of the following tests:
- Chest X-ray: This imaging test can help visualize the structure of the lungs and may reveal signs of bronchiectasis, such as thickened bronchial walls or areas of dilation.
- High-resolution computed tomography (HRCT) scan: This advanced imaging technique provides detailed images of the lungs and can accurately detect bronchiectasis even in its early stages.
- Pulmonary function tests (PFTs): These tests measure lung capacity and the ability to inhale and exhale effectively. Abnormal results may indicate underlying bronchiectasis.
- Sputum cultures: These tests involve analyzing a sample of mucus coughed up from the lungs to identify the type of bacteria causing recurrent infections.
Once a diagnosis is confirmed, further tests may be required to determine the underlying cause of bronchiectasis and guide treatment decisions.
Treatment
The management and treatment of bronchiectasis aim to control symptoms, reduce the frequency and severity of respiratory infections, and slow down the progression of lung damage. The specific treatment plan will depend on the underlying cause of bronchiectasis, the severity of symptoms, and the individual’s overall health.
Airway Clearance Techniques
One of the primary components of bronchiectasis treatment is airway clearance techniques. These techniques help to mobilize and remove mucus from the lungs, preventing it from becoming trapped in the airways and causing further infections. Some common airway clearance techniques include:
- Chest physiotherapy: This technique involves gentle percussion or clapping on the chest and back to help loosen and mobilize mucus.
- Postural drainage: This technique uses specific body positioning to promote the drainage of mucus from specific areas of the lungs.
- Breathing exercises: These exercises can help improve lung function and promote effective coughing to clear mucus.
Airway clearance techniques should be performed regularly, as instructed by a healthcare professional, to maintain optimal lung health.
Medications
Bronchiectasis treatment may also involve the use of medications to manage symptoms and prevent complications. Some common medications used in the treatment of bronchiectasis include:
- Bronchodilators: These medications help to relax and open the airways, making breathing easier.
- Mucolytics: These medications help thin and loosen mucus, making it easier to cough up and clear from the lungs.
- Inhaled corticosteroids: These medications help to reduce inflammation in the airways, preventing them from becoming further damaged.
- Antibiotics: Antibiotics may be prescribed to treat bacterial infections or prevent them from recurring.
It is important to take medications as prescribed and to adhere to the recommended treatment plan to effectively manage bronchiectasis.
Lung Transplantation
In severe cases of bronchiectasis where there is significant lung damage and impaired lung function, lung transplantation may be considered as a treatment option. Lung transplantation involves replacing the diseased lungs with healthy donor lungs to improve overall respiratory function and quality of life. However, lung transplantation is a complex procedure with potential risks and should be carefully discussed with a healthcare provider.
Types of Bronchiectasis
Bronchiectasis can present in different forms, depending on the specific pattern of airway dilation and damage. The four main types of bronchiectasis include:
Cylindrical Bronchiectasis
Cylindrical bronchiectasis is characterized by a consistent and uniform dilation of the airways. The bronchial walls are cylindrical in shape and maintain their circular structure. This type of bronchiectasis usually affects larger airways and is often associated with chronic obstructive pulmonary disease (COPD).
Varicose Bronchiectasis
Varicose bronchiectasis is characterized by irregular and bulbous dilation of the airways. The bronchial walls have a varicose-like appearance, with areas of constriction alternating with areas of dilation. This type of bronchiectasis can affect both larger and smaller airways.
Cystic Bronchiectasis
Cystic bronchiectasis is characterized by the formation of cysts or sac-like structures within the airway walls. These cysts can become filled with mucus and contribute to the obstruction of the airways. Cystic bronchiectasis is often associated with underlying genetic conditions, such as cystic fibrosis.
Saccular Bronchiectasis
Saccular bronchiectasis is characterized by the presence of large, pouch-like dilations of the airways. These dilations are generally located at the ends of the bronchial tubes and are more prone to recurrent infections. Saccular bronchiectasis is often associated with congenital abnormalities or previous lung damage.
It is important to note that the different types of bronchiectasis can coexist in an individual, and the specific pattern of airway dilation can vary from person to person.

Risk Factors for Bronchiectasis
While bronchiectasis can affect individuals of all ages and backgrounds, certain risk factors may increase the likelihood of developing the condition. These risk factors include:
Chronic Infections
Chronic respiratory infections, such as recurrent pneumonia or tuberculosis, can cause inflammation and damage to the airways, increasing the risk of bronchiectasis. Individuals with a history of repeated respiratory infections should be vigilant for any persistent or worsening respiratory symptoms and seek medical attention if necessary.
Respiratory Conditions
Pre-existing respiratory conditions, such as asthma or chronic obstructive pulmonary disease (COPD), can contribute to the development of bronchiectasis. These conditions can lead to chronic inflammation in the airways, which can eventually result in permanent damage and dilation.
Immunodeficiency Disorders
Immunodeficiency disorders, such as common variable immunodeficiency (CVID) or HIV/AIDS, can weaken the immune system’s ability to fight off infections. This can result in recurrent respiratory infections, which increase the risk of bronchiectasis.
Genetic Factors
Certain genetic conditions, such as cystic fibrosis or alpha-1 antitrypsin deficiency, can predispose individuals to the development of bronchiectasis. These conditions often result in abnormal mucus production or impaired lung defenses, making individuals more susceptible to respiratory infections and subsequent damage to the airways.
It is important for individuals with these risk factors to be aware of the potential signs and symptoms of bronchiectasis and seek prompt medical attention if they suspect they may have the condition.
Impact of Bronchiectasis on Lung Function
Bronchiectasis can have a significant impact on lung function and overall respiratory health. Some of the ways in which bronchiectasis can affect lung function include:
Obstruction of Airways
The permanent dilation and damage of the bronchial tubes in bronchiectasis can lead to the obstruction of the airways. This obstruction can make it difficult for air to flow freely in and out of the lungs, resulting in reduced lung function and impaired breathing.
Impaired Airflow
Due to the enlargement of the airways and the accumulation of mucus, bronchiectasis can lead to impaired airflow within the lungs. This can result in decreased oxygen exchange and reduced lung capacity, leading to feelings of breathlessness, fatigue, and decreased exercise tolerance.
Mucus Accumulation
One of the hallmark features of bronchiectasis is the excessive production and buildup of mucus in the airways. The inability to effectively clear this mucus can lead to further blockage of the airways and increased susceptibility to respiratory infections. The presence of excess mucus can also contribute to persistent coughing and discomfort.
Decreased Lung Capacity
As the damage to the airways progresses, bronchiectasis can lead to a decrease in lung capacity. This means that the lungs are unable to expand and take in as much air as they should, resulting in reduced overall respiratory function. This decreased lung capacity can lead to increased fatigue, shortness of breath, and limitations in daily activities.
It is important for individuals with bronchiectasis to work closely with their healthcare providers to monitor and manage these effects and take steps to optimize lung function and quality of life.
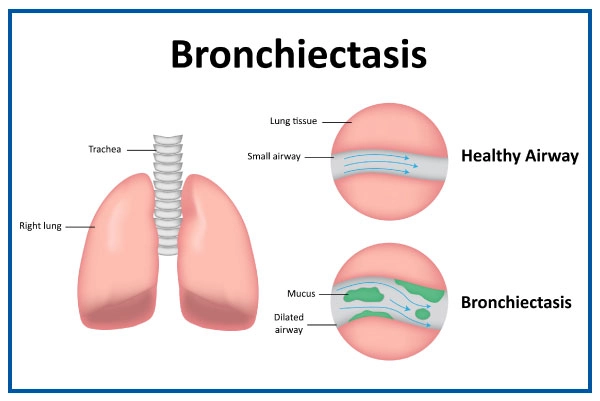
Complications Associated with Bronchiectasis
Bronchiectasis can give rise to several complications, which can further impact respiratory health and overall well-being. Some of the common complications associated with bronchiectasis include:
Recurrent Infections
Due to the impaired ability to clear mucus from the airways, individuals with bronchiectasis are more prone to recurrent respiratory infections. These infections can cause further damage to the airways and lead to worsening symptoms, increased mucus production, and greater lung impairment.
Respiratory Failure
In severe cases of bronchiectasis, where there is extensive lung damage and significant impairment of lung function, respiratory failure can occur. Respiratory failure means that the lungs are no longer able to provide sufficient oxygen to the body or remove carbon dioxide effectively. This is a life-threatening condition and requires immediate medical intervention.
Hemoptysis
Hemoptysis refers to the coughing up of blood from the respiratory tract. In bronchiectasis, hemoptysis often occurs as a result of damaged blood vessels within the dilated airways. The presence of blood in mucus can be alarming and may indicate a need for further medical evaluation.
Pneumonia
Recurrent respiratory infections in individuals with bronchiectasis can increase the risk of developing pneumonia. Pneumonia is a serious infection of the lungs that can further compromise respiratory function and overall health. Prompt treatment with appropriate antibiotics is necessary to prevent the spread of infection and complications.
It is important for individuals with bronchiectasis to be aware of these potential complications and work closely with their healthcare providers to prevent and manage them effectively.
Management and Treatment of Bronchiectasis
The management and treatment of bronchiectasis involve a comprehensive approach aimed at controlling symptoms, reducing the frequency of infections, and optimizing lung function. Some of the key components of bronchiectasis management include:
Airway Clearance Techniques
Airway clearance techniques play a crucial role in the management of bronchiectasis. These techniques aim to mobilize and remove mucus from the airways, preventing its accumulation and the subsequent risk of infection. Chest physiotherapy, postural drainage, and breathing exercises are common airway clearance techniques used in bronchiectasis management. These techniques should be performed regularly as part of a daily routine under the guidance of a healthcare professional.
Medications
Medications may be prescribed to manage bronchiectasis symptoms and prevent complications. Bronchodilators can help relax and open up the airways, making breathing easier. Mucolytics can help thin and loosen mucus, making it easier to cough up and clear from the lungs. Inhaled corticosteroids may be used to reduce airway inflammation. Antibiotics are often prescribed to treat acute respiratory infections or prevent recurrent infections.
It is important to take medications as prescribed and to adhere to the recommended treatment plan to effectively manage bronchiectasis.
Antibiotics
Given the increased susceptibility to respiratory infections, individuals with bronchiectasis may require antibiotic treatment. Antibiotics can help treat bacterial infections and prevent them from recurring. The choice of antibiotics will depend on the type of bacteria causing the infection and may be tailored to the individual’s specific needs. It is essential to take antibiotics as prescribed and to complete the full course of treatment to ensure effective eradication of the infection.
Lung Transplantation
In severe cases of bronchiectasis with advanced lung damage, lung transplantation may be considered as a treatment option. Lung transplantation involves replacing the diseased lungs with healthy donor lungs to improve overall respiratory function and quality of life. However, lung transplantation is a complex procedure with potential risks and should be carefully discussed with a healthcare provider.
It is important for individuals with bronchiectasis to work closely with a healthcare provider to develop an individualized management plan that addresses their specific needs and goals.

Prevention and Lifestyle Modifications
While bronchiectasis is a chronic condition, there are steps that individuals can take to prevent its progression and improve overall respiratory health. Some preventive measures and lifestyle modifications may include:
Vaccinations
Ensuring up-to-date vaccinations can help protect against respiratory infections, reducing the risk of exacerbations and complications. Vaccinations such as the influenza vaccine and the pneumococcal vaccine are recommended for individuals with bronchiectasis.
Regular Exercise
Engaging in regular exercise and physical activity can help improve lung function and strengthen the respiratory muscles. Exercise can also enhance overall fitness and stamina, making daily activities easier to manage. It is important to work with a healthcare provider or exercise specialist to develop a safe and appropriate exercise program for individuals with bronchiectasis.
Smoking Cessation
Smoking is a significant risk factor for the development and progression of bronchiectasis. Quitting smoking is essential for both preventing bronchiectasis and slowing down its progression in individuals already diagnosed with the condition. Smoking cessation can improve lung function, reduce symptoms, and decrease the risk of respiratory infections.
Avoidance of Air Pollution
Exposure to environmental pollutants, such as air pollution or occupational hazards, can worsen respiratory symptoms in individuals with bronchiectasis. It is important to minimize exposure to these pollutants by avoiding heavily polluted areas, using air filters in the home, and following recommended safety precautions in the workplace.
Implementing these preventive measures and lifestyle modifications can significantly improve the quality of life for individuals with bronchiectasis and help prevent complications.
Support and Resources for Bronchiectasis Patients
Living with bronchiectasis can be challenging, but there are numerous support and resources available to help individuals manage the condition effectively. Some of the key support options include:
Patient Support Groups
Joining a patient support group can provide a valuable source of emotional support, practical advice, and shared experiences. Connecting with others who understand the challenges of living with bronchiectasis can help individuals feel less alone and more empowered in managing their condition.
Educational Materials
Educational materials, such as brochures, pamphlets, and online resources, can provide valuable information about bronchiectasis, treatment options, self-care strategies, and lifestyle modifications. These resources can help individuals better understand their condition and actively participate in their own care.
Online Forums
Online forums and discussion boards provide a platform for individuals with bronchiectasis to ask questions, share experiences, and seek advice from others in similar situations. These forums can be accessed from the comfort of home and allow for ongoing communication and support.
Counseling Services
Living with a chronic condition like bronchiectasis can take a toll on mental health and well-being. Counseling services, such as individual therapy or support groups, can provide a safe and confidential space to address the emotional challenges and psychological impact of living with bronchiectasis.
It is important for individuals with bronchiectasis to explore these support options and connect with their healthcare providers for further guidance and resources specific to their needs.

Promising Research and Future Directions
Advancements in medical research continue to uncover new possibilities for the diagnosis and treatment of bronchiectasis. Some of the promising areas of research and future directions include:
Novel Therapies
Researchers are exploring the development of novel therapies that target the underlying mechanisms of bronchiectasis. These therapies aim to reduce inflammation, prevent infection, and promote lung repair. Clinical trials are underway to investigate the safety and efficacy of these new treatment options.
Gene Therapy
Gene therapy holds promise for individuals with bronchiectasis caused by specific genetic mutations. By delivering functional genes to targeted cells, gene therapy aims to correct the underlying genetic defect and potentially reverse or slow down the progression of the condition. Research in this field is ongoing, with the goal of developing safe and effective gene-based treatments.
Stem Cell Research
Stem cell research is exploring the potential of using stem cells to repair damaged lung tissue and restore lung function in individuals with bronchiectasis. This emerging field of regenerative medicine seeks to harness the regenerative properties of stem cells to regenerate healthy lung tissue and improve respiratory function.
Advancements in Diagnosis
Advancements in imaging techniques, such as high-resolution computed tomography (HRCT), continue to improve the diagnosis and monitoring of bronchiectasis. These advanced imaging methods provide detailed and precise images of the lungs, allowing for earlier and more accurate detection of bronchiectasis, even in its early stages.
The ongoing research efforts in bronchiectasis hold promise for improved diagnosis, treatment, and quality of life for individuals living with this condition. It is important for individuals with bronchiectasis to stay informed about these advancements and discuss potential opportunities with their healthcare providers.
Conclusion
Bronchiectasis is a chronic respiratory condition characterized by permanent dilation and damage of the bronchial tubes. It can have a significant impact on lung function and overall respiratory health. Understanding the causes, symptoms, diagnosis, and treatment options for bronchiectasis is essential for effective management and improved quality of life. By following a comprehensive treatment plan, engaging in preventive measures, and accessing appropriate support and resources, individuals with bronchiectasis can effectively manage their condition and minimize complications. Ongoing research and advancements in medical knowledge offer hope for continued progress in the diagnosis, treatment, and future outcomes for individuals with bronchiectasis.