If you’re one of the many individuals dealing with the challenges of Benign Prostatic Hyperplasia (BPH), then understanding the essential role that medication plays in treating this condition is crucial. BPH, a condition characterized by an enlarged prostate gland, can lead to troublesome urinary symptoms and impact your quality of life. In this article, we will explore the importance of medication in managing BPH and how it can provide relief from the discomfort it brings. So, let’s explore the world of BPH medication and discover how it can make a positive difference in your life.
Understanding Benign Prostatic Hyperplasia (BPH)
Benign Prostatic Hyperplasia (BPH) refers to the non-cancerous enlargement of the prostate gland. As men get older, the prostate gland naturally grows in size, leading to BPH. This condition is fairly common among aging men and can cause various urinary symptoms.
Definition of BPH
BPH is characterized by the enlargement of the prostate gland, which surrounds the urethra – the tube responsible for carrying urine from the bladder out of the body. As the prostate gland enlarges, it can put pressure on the urethra, leading to symptoms such as frequent urination, weak urine stream, difficulty starting and stopping urination, and incomplete bladder emptying.
Causes and risk factors
While the exact cause of BPH is not fully understood, hormonal imbalances and age-related changes in the levels of certain hormones, such as dihydrotestosterone (DHT), are believed to contribute to prostate enlargement. Additional risk factors for developing BPH include being over the age of 40, having a family history of the condition, and obesity.
Symptoms of BPH
BPH can lead to a range of urinary symptoms that can significantly impact a man’s quality of life. Common symptoms of BPH include increased frequency of urination, especially at night (nocturia), weak urine flow, difficulty starting and stopping urine flow, dribbling at the end of urination, the sensation of incomplete bladder emptying, and the need to strain or push to urinate. These symptoms can manifest gradually and worsen over time if left untreated.
Diagnosing BPH
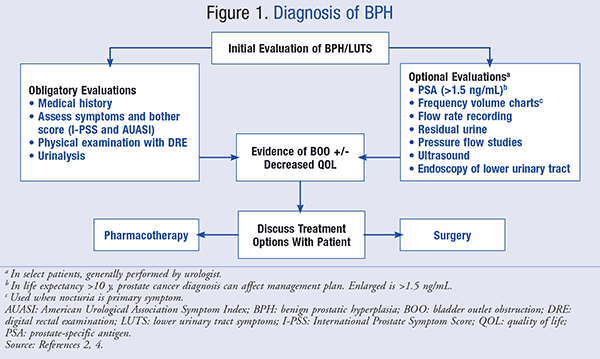
An accurate diagnosis of BPH involves a comprehensive evaluation of a patient’s medical history, physical examination, and various diagnostic tests. This helps to rule out other potential conditions with similar symptoms and determine the most appropriate treatment approach.
Physical examination
During a physical examination, the healthcare provider will perform a general evaluation and focus on the abdominal and genital regions. The examination may involve palpation of the lower abdomen and a digital rectal exam (DRE) to assess the size, shape, and texture of the prostate gland.
Medical history
A detailed medical history is crucial to identify any underlying conditions or medications that could contribute to urinary symptoms. The healthcare provider will inquire about symptoms, their duration and severity, and any previous treatments or surgeries related to urinary issues.
Digital rectal exam
A digital rectal exam allows the healthcare provider to assess the size, shape, and texture of the prostate gland by inserting a gloved, lubricated finger into the rectum. This examination helps to evaluate the prostate for enlargement or irregularities.
Prostate-specific antigen (PSA) test
The PSA test measures the blood levels of prostate-specific antigen, a protein produced by the prostate gland. While elevated PSA levels can be an indication of prostate conditions, including BPH, it is not a definitive test for diagnosing BPH alone. Additional tests and evaluations are necessary to confirm a BPH diagnosis.
Urinary flow test
A urinary flow test measures the speed and volume of urine during urination by asking the patient to urinate into a special device. This test provides an objective assessment of urinary flow and helps screen for potential obstructions caused by BPH.
Ultrasound
An ultrasound of the prostate allows for a visual examination of the prostate gland using sound waves. This imaging technique helps determine the size of the prostate and can assist in diagnosing other conditions that may contribute to urinary symptoms.
Cystoscopy
In certain cases, a cystoscopy may be recommended to further evaluate the urethra and bladder. During this procedure, a thin, flexible tube with a camera on the end (cystoscope) is inserted through the urethra to visualize the urinary tract for any abnormalities or obstructions.
Goals of BPH Treatment
The primary goals of BPH treatment are to alleviate bothersome symptoms, prevent complications, and improve a patient’s overall quality of life. Treatment options for BPH can include lifestyle modifications, non-medication approaches, and various medications.
Alleviating symptoms
The main objective of BPH treatment is to relieve the bothersome urinary symptoms associated with the condition. By reducing urinary symptoms, treatment can improve the patient’s quality of life and overall well-being.
Preventing complications
In some cases, BPH can lead to complications such as urinary tract infections, acute urinary retention (inability to urinate), bladder stones, and kidney damage. Treating BPH aims to prevent these complications and mitigate the potential risks they pose to a patient’s health.
Improving quality of life
BPH can significantly impact a man’s daily life, causing discomfort, disruption of sleep, and limitations in activities. Treatment is aimed at improving the overall quality of life for individuals with BPH by reducing symptoms and enabling them to resume their daily routines without interference.
Non-Medication Treatment Options for BPH
Before considering medication, non-medication treatment options can be explored. These approaches range from watchful waiting to lifestyle modifications and minimally invasive procedures.
Watchful waiting
Watchful waiting, also known as active surveillance, involves monitoring BPH symptoms without immediate intervention. This option is often suitable for individuals with mild symptoms that do not significantly affect their quality of life.
Lifestyle modifications
Certain lifestyle modifications can help manage BPH symptoms. These may include avoiding caffeine and alcohol, limiting fluid intake before bedtime, regular exercise, and practicing techniques to strengthen the pelvic floor muscles.
Minimally invasive procedures
Minimally invasive procedures are non-surgical techniques that aim to relieve urinary symptoms associated with BPH. These procedures can include transurethral microwave therapy (TUMT), transurethral needle ablation (TUNA), and water-induced thermotherapy.
Surgical interventions
In cases where symptoms are severe or other treatments have been ineffective, surgical interventions may be considered. These can include transurethral resection of the prostate (TURP), laser ablation, prostate artery embolization, and open prostatectomy.
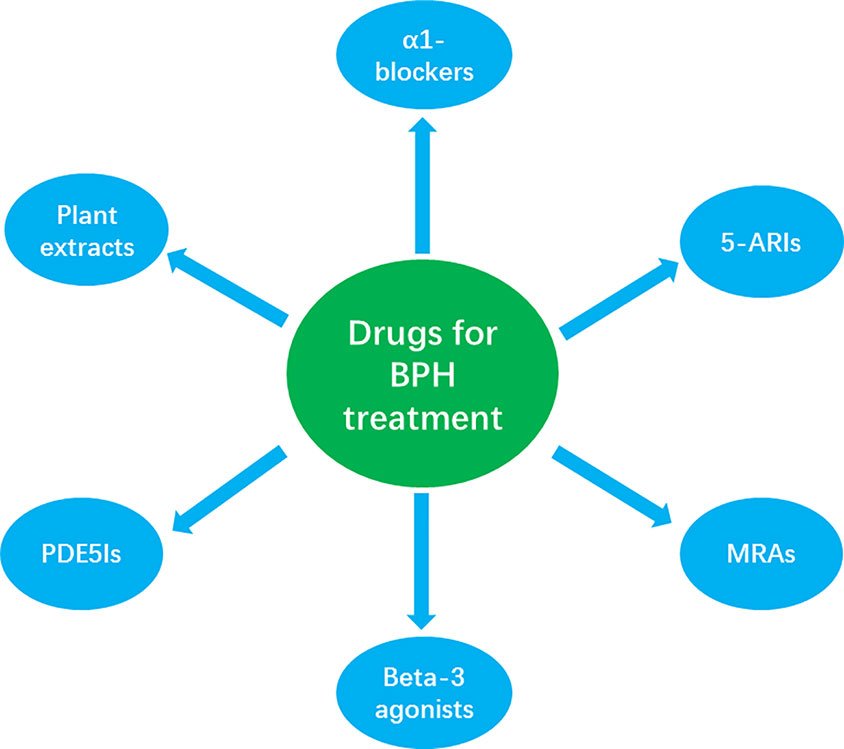
Types of Medications for BPH
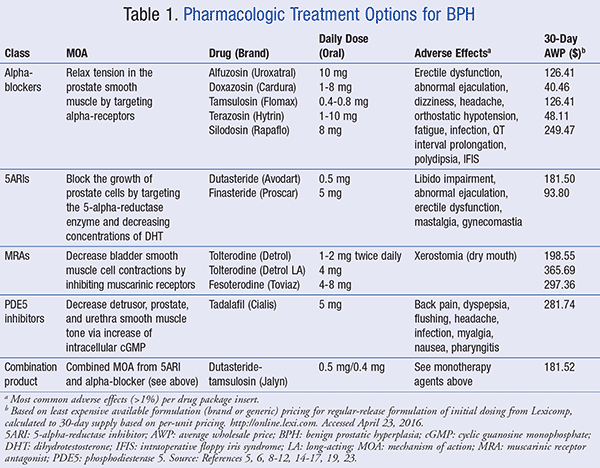
Medications play a crucial role in the management of BPH symptoms and can be effective in alleviating urinary symptoms and reducing the size of the prostate gland. Different types of medications are available, each targeting specific mechanisms within the body.
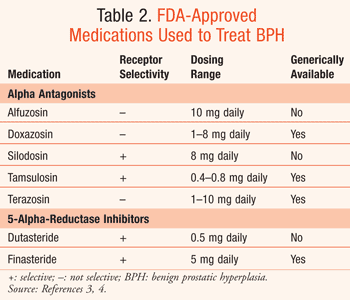
Alpha blockers
Alpha blockers work by relaxing the smooth muscles of the prostate and bladder neck, thereby relieving the symptoms of BPH. These medications help improve urine flow and reduce the obstruction caused by an enlarged prostate.
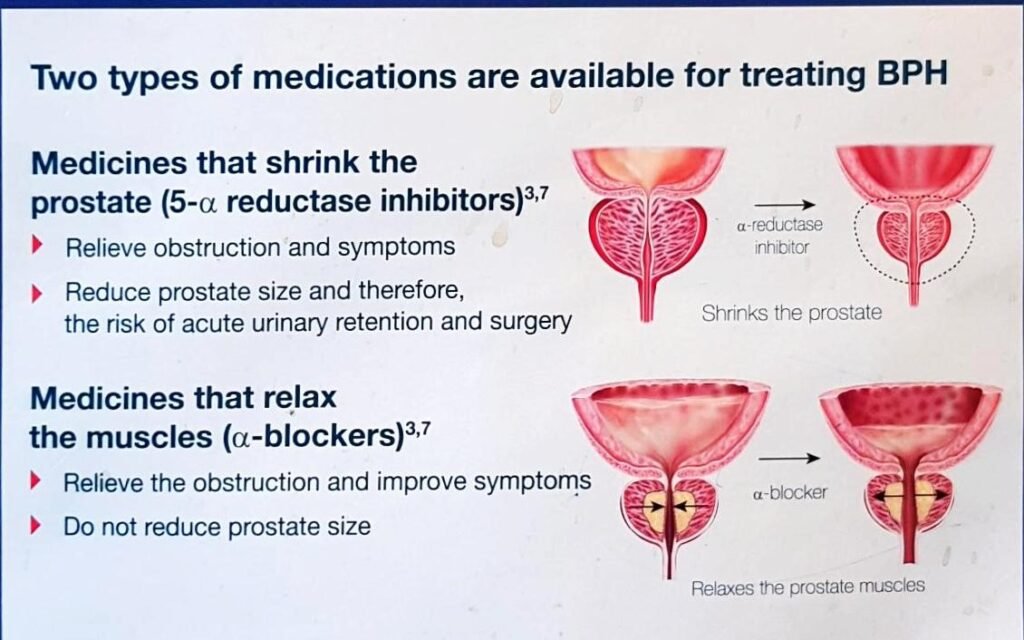
5-alpha reductase inhibitors (5-ARIs)
5-ARIs target the hormone-related component of BPH by inhibiting the conversion of testosterone to dihydrotestosterone (DHT). This action can reduce the size of the prostate gland, relieve urinary symptoms, and slow down the progression of BPH.
Combination therapy
Combination therapy involves the simultaneous use of both alpha blockers and 5-ARIs. This approach aims to address different aspects of BPH by reducing symptoms and preventing disease progression.
Phosphodiesterase-5 inhibitors (PDE5Is)
PDE5Is, commonly used for erectile dysfunction, can also be beneficial for individuals with BPH. These medications relax the smooth muscles of the prostate and bladder, improving urinary symptoms.
Anticholinergic medications
Anticholinergic medications may be prescribed to individuals with BPH who also experience overactive bladder symptoms. These medications help relax the bladder muscles, reducing frequency and urgency.
Phytotherapy
Phytotherapy involves the use of herbal and plant-based supplements to manage BPH symptoms. Commonly used phytotherapeutic agents for BPH include saw palmetto, pygeum, and stinging nettle.
Alpha Blockers
Among the medications commonly prescribed for BPH, alpha blockers are widely used due to their effectiveness in improving urinary symptoms.
Mechanism of action
Alpha blockers work by selectively relaxing the smooth muscles in the prostate and bladder neck. By blocking the alpha-adrenergic receptors, these medications reduce the tension in the muscles, allowing for improved urine flow and relieving symptoms.
Commonly prescribed alpha blockers
Some commonly prescribed alpha blockers for BPH include tamsulosin, terazosin, and doxazosin. These medications are available in oral form and are typically taken once daily.
Effectiveness and side effects
Alpha blockers have been shown to be effective in improving urinary symptoms and increasing peak urine flow rates. However, they may cause side effects such as dizziness, low blood pressure, nasal congestion, and retrograde ejaculation.
Considerations for use
Alpha blockers are generally well-tolerated, but caution should be exercised in individuals with certain medical conditions, such as low blood pressure or liver problems. It is important to discuss any existing medical conditions or medications with a healthcare provider before starting alpha blocker therapy.
5-alpha Reductase Inhibitors (5-ARIs)
Another class of medications commonly used for BPH is 5-alpha reductase inhibitors, which primarily target the hormone-related aspects of the condition.
Mechanism of action
5-ARIs work by inhibiting the enzyme responsible for converting testosterone to dihydrotestosterone (DHT). By reducing the levels of DHT, these medications can shrink the prostate gland, alleviate urinary symptoms, and slow down the progression of BPH.
Commonly prescribed 5-ARIs
Finasteride and dutasteride are the two main 5-ARIs prescribed for BPH. These medications are taken orally and are usually administered on a daily basis.
Effectiveness and side effects
Clinical studies have shown that 5-ARIs can significantly reduce the size of the prostate gland, improve urinary symptoms, and increase peak urine flow rates. However, they may cause side effects such as decreased libido, erectile dysfunction, breast tenderness, and ejaculation disorders.
Considerations for use
Before starting 5-ARI therapy, healthcare providers may evaluate the patient’s prostate-specific antigen (PSA) levels and conduct other clinical assessments to determine the appropriateness of this medication. It’s important to be aware that 5-ARIs may not provide immediate relief of symptoms and may take several months to achieve noticeable improvements.
Combination Therapy
Combination therapy involves the use of both alpha blockers and 5-ARIs concurrently to achieve greater therapeutic effects and address different aspects of BPH.
Use of alpha blockers and 5-ARIs together
Combination therapy is often considered when a patient experiences moderate to severe symptoms and has an enlarged prostate gland. By combining the mechanisms of action of both medications, improved relief of symptoms and a reduction in the rate of disease progression can be achieved.
Rationale and benefits
Alpha blockers work quickly to alleviate symptoms, while 5-ARIs target the underlying hormonal component of BPH and help shrink the prostate gland. By combining these medications, patients may experience faster symptom relief, a reduction in prostate size, and a decreased risk of disease progression.
Potential side effects
As with any medication, combination therapy may carry a risk of side effects. These can include low blood pressure, orthostatic hypotension, dizziness, and sexual dysfunction. It is important to discuss the potential risks and benefits of combination therapy with a healthcare provider.
Considerations for use
Combination therapy may not be suitable for all individuals and should be tailored to each patient’s specific needs. Healthcare providers will consider factors such as the severity of symptoms, prostate size, and overall health to determine the appropriateness of combination therapy.
Phosphodiesterase-5 Inhibitors (PDE5Is)
Although primarily used for erectile dysfunction, phosphodiesterase-5 inhibitors can also provide benefits for individuals with BPH.
Mechanism of action
PDE5Is work by preventing the breakdown of cyclic guanosine monophosphate (cGMP), resulting in the relaxation of smooth muscles and increased blood flow. In the context of BPH, this relaxation helps to alleviate urinary symptoms by reducing tension in the prostate and bladder.
Commonly prescribed PDE5Is
Tadalafil is the primary PDE5I used for BPH. It is available in an oral form and is typically taken once a day.
Effectiveness and side effects
Clinical studies have shown that PDE5Is can improve urinary symptoms, increase urine flow rate, and reduce prostate size in individuals with BPH. Common side effects of PDE5Is include headache, indigestion, back pain, muscle aches, and flushing.
Considerations for use
When considering the use of PDE5Is for BPH, it is important to assess the patient’s overall health and determine their suitability for this class of medication. PDE5Is should be used with caution in individuals taking nitrate medications due to the potential for a sudden decrease in blood pressure.
Phytotherapy
Phytotherapy involves the use of herbal and plant-based supplements to manage BPH symptoms. While research on the effectiveness of phytotherapeutic agents in treating BPH is ongoing, some agents have shown promising results.
Use of herbal and plant-based supplements
Numerous herbal and plant-based supplements are commonly used in the management of BPH. Examples include saw palmetto, pygeum, stinging nettle, and rye grass pollen extract. These supplements are available in various forms, such as capsules, extracts, or teas.
Commonly used phytotherapeutic agents
Saw palmetto is one of the most widely studied and commonly used herbal supplements for BPH. Pygeum, stinging nettle, and rye grass pollen extract are also popular choices. These agents are believed to have anti-inflammatory and anti-androgenic properties, helping to reduce prostate size and relieve urinary symptoms.
Effectiveness and potential side effects
While studies have provided mixed results regarding the effectiveness of phytotherapeutic agents, some individuals may experience symptom improvement with their use. However, it is important to note that the quality and purity of these supplements can vary, and potential side effects should be considered. These can include stomach upset, nausea, headaches, and allergic reactions.
Considerations for use
Before using any phytotherapeutic agents, individuals should consult with a healthcare provider to ensure the safety and appropriateness of these supplements. It is important to disclose any existing medical conditions and medications to avoid potential interactions or adverse effects.
In conclusion, understanding BPH is crucial for individuals experiencing urinary symptoms associated with the condition. Proper diagnosis, evaluation, and consideration of treatment options can significantly improve quality of life. Whether through non-medication approaches, such as lifestyle modifications and minimally invasive procedures, or the use of medications like alpha blockers, 5-ARIs, combination therapy, PDE5Is, and phytotherapeutic agents, there are various treatment options available to help manage BPH and alleviate its bothersome symptoms. Consulting with a healthcare provider is essential to determine the most appropriate course of treatment based on individual needs and preferences. With the right approach, individuals with BPH can find relief and regain control of their urinary health.