You’ve probably experienced the discomfort and pain that comes with an ear infection at some point in your life. Whether it’s the throbbing ache or the muffled sounds, ear infections can be quite bothersome. But fear not, as there are effective treatments available to soothe your discomfort and aid in your recovery. In this article, we will explore some common causes of ear infections and discuss various treatment options that can help you find relief. So, sit back, relax, and let’s explore the world of treating ear infections together!
Overview of Ear Infections
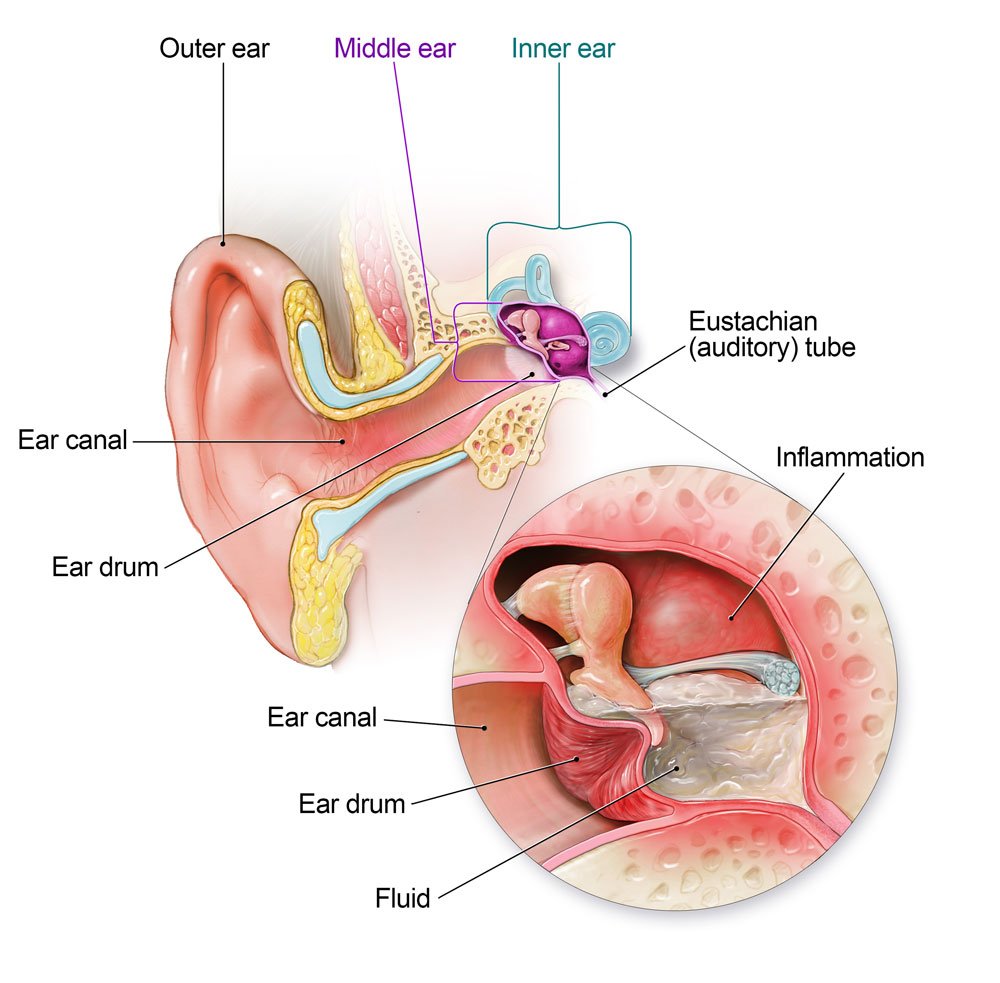
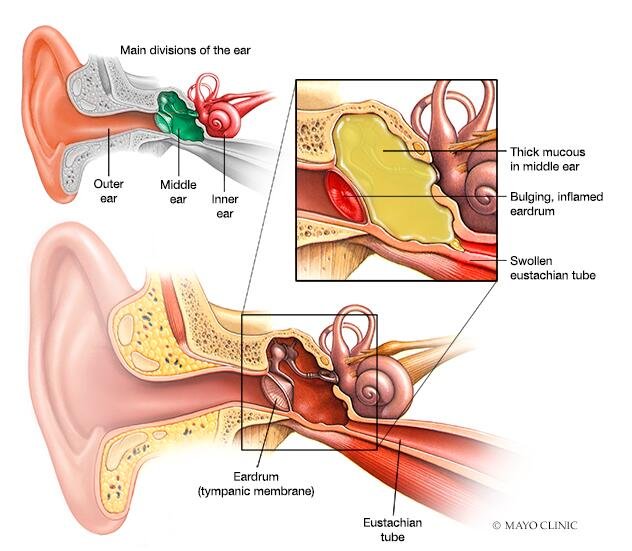
Ear infections, also known as otitis media, are a common condition affecting people of all ages. They occur when there is an infection or inflammation in the middle ear, the space behind the eardrum. Ear infections can be painful and uncomfortable, and if left untreated, they can lead to complications such as hearing loss or recurrent infections. Understanding the causes, symptoms, diagnostic methods, treatment options, and prevention strategies for ear infections is essential for maintaining ear health and preventing further complications.
Definition and Types of Ear Infections
Ear infections can be classified into two main types: acute otitis media (AOM) and otitis media with effusion (OME). Acute otitis media refers to a sudden and severe infection of the middle ear, while otitis media with effusion is the presence of fluid in the middle ear without any signs of infection. Both types can be experienced by people of all ages, but they are more common in children.
Causes of Ear Infections
Ear infections are commonly caused by bacteria or viruses that enter the middle ear through the Eustachian tube. The Eustachian tube is a narrow passage that connects the middle ear to the back of the throat. When the Eustachian tube becomes blocked or fails to function properly, it can create a favorable environment for the growth of bacteria or viruses, leading to an ear infection. Other factors that can contribute to the development of ear infections include allergies, respiratory infections, changes in altitude, and exposure to cigarette smoke.
Symptoms of Ear Infections
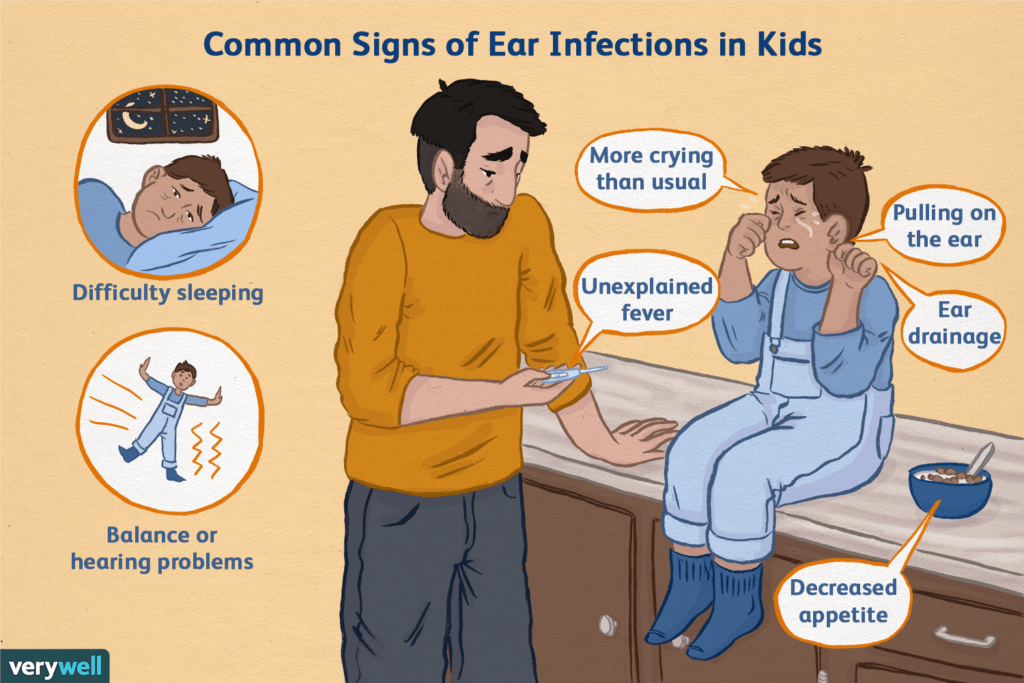
The symptoms of ear infections can vary depending on the age of the person and the severity of the infection. In children, common symptoms include ear pain or pulling at the ears, irritability, difficulty sleeping, fever, reduced appetite, and fluid drainage from the ear. In adults, symptoms may include earache, headache, temporary hearing loss, ringing in the ears, and a feeling of ear fullness or pressure. It is important to note that not all ear infections present with obvious symptoms, especially in cases of otitis media with effusion.
Diagnosing Ear Infections
Diagnosing an ear infection involves a combination of physical examination, medical history assessment, and diagnostic tests.
Physical Examination
During a physical examination, a healthcare professional will inspect the outer ear, the eardrum, and the surrounding area for signs of infection or inflammation. They may use an otoscope, a handheld instrument with a light, to examine the eardrum and check for redness, bulging, or fluid accumulation. The examination may also involve gentle pressure to assess the pain response and determine the severity of the infection.
Medical History
Taking a detailed medical history is important to identify any risk factors or underlying conditions that may contribute to the development of ear infections. The healthcare professional will ask about previous ear infections, the frequency and duration of symptoms, any hearing difficulties, recent respiratory infections, allergies, and exposure to cigarette smoke or other environmental factors.
Diagnostic Tests
In some cases, additional diagnostic tests may be required to confirm the presence of an ear infection or to determine the severity of the condition. These tests may include a tympanometry, which measures the movement of the eardrum in response to changes in air pressure, or a middle ear fluid culture, which involves collecting a sample of the fluid from the middle ear for laboratory analysis.
Treatment Options for Ear Infections
The treatment options for ear infections depend on various factors, including the severity of the infection, the age of the person, and the presence of any complicating factors.
1. Antibiotics
Antibiotics are commonly prescribed for bacterial ear infections to help eliminate the infection and reduce symptoms. The choice of antibiotic will depend on the specific bacteria causing the infection and any known antibiotic allergies. It is important to complete the full course of antibiotics as prescribed, even if symptoms improve, to prevent the development of antibiotic resistance.
2. Pain Relief Medications
Over-the-counter pain relief medications, such as acetaminophen or ibuprofen, can help alleviate the pain and discomfort associated with ear infections. These medications also help reduce fever, if present. It is important to follow the recommended dosage guidelines and consult a healthcare professional before giving medications to children.
3. Ear Drops
In some cases, ear drops may be recommended to relieve pain and inflammation associated with ear infections. These drops may contain analgesics to provide temporary pain relief or anti-inflammatory agents to reduce swelling. It is important to follow the instructions provided by the healthcare professional when using ear drops, and avoid using them if the eardrum is perforated.
4. Surgery
Surgery is typically reserved for severe or recurrent cases of ear infections that do not respond to other treatment options. The most common surgical procedure for ear infections is the placement of tympanostomy tubes, also known as ear tubes. These tubes help equalize the pressure in the middle ear, prevent fluid buildup, and reduce the frequency and severity of ear infections. Surgery may also be necessary to treat complications of ear infections, such as the removal of an abscess or repair of a perforated eardrum.
Prevention and Home Remedies
Taking proactive steps to prevent ear infections can help reduce the risk of developing the condition. Additionally, certain home remedies can provide relief for mild symptoms or support the healing process.
1. Frequent Handwashing
Practicing good hand hygiene is essential in reducing the spread of bacteria and viruses that can lead to ear infections. Encourage regular handwashing with soap and water for at least 20 seconds, especially before and after meals, after using the restroom, and after being in public places.
2. Vaccination
Ensuring that you and your family are up to date with vaccinations can help prevent some types of ear infections. Vaccines, such as the pneumococcal conjugate vaccine and the influenza vaccine, can protect against bacteria and viruses commonly associated with ear infections.
3. Avoiding Smoking
Exposure to cigarette smoke can increase the risk of developing ear infections, especially in children. If you smoke, it is important to avoid smoking indoors and around children. If you are a non-smoker, it is advisable to limit exposure to secondhand smoke as much as possible.
4. Breastfeeding
Breastfeeding has been associated with a reduced risk of ear infections in infants. Breast milk contains antibodies and other beneficial components that can help boost the immune system and protect against infections. If possible, try to exclusively breastfeed your baby for the first six months of life.
5. Stay Updated with Immunizations
Staying updated with immunizations is crucial in preventing various infectious diseases, including those that can lead to ear infections. Consult with a healthcare professional to ensure you are receiving all recommended immunizations for your age and condition.
Natural Remedies for Ear Infections
In addition to medical treatment, there are some natural remedies that may provide relief from the symptoms of ear infections. However, it is important to consult with a healthcare professional before using any natural remedies, particularly for children or individuals with underlying health conditions.
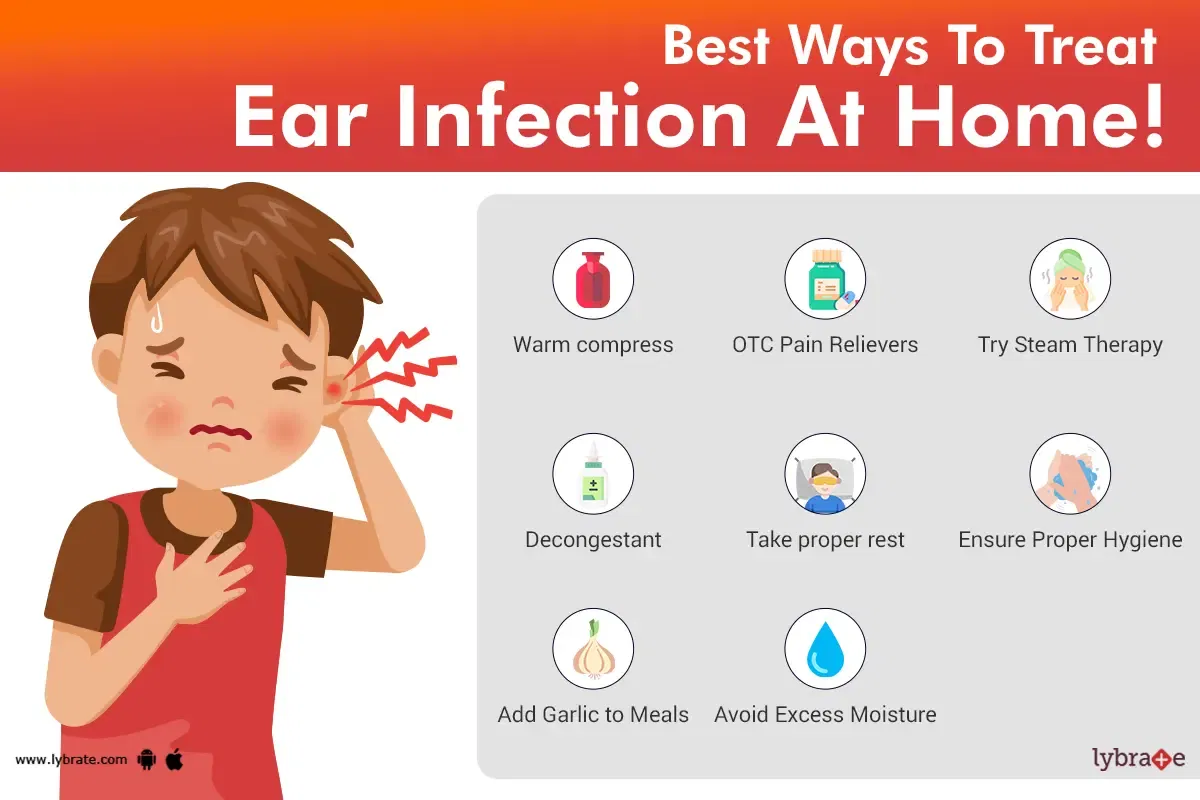
1. Warm Compress
Applying a warm compress to the affected ear can help alleviate pain and reduce inflammation. Soak a clean cloth in warm water, wring out the excess moisture, and place it over the ear for 10-15 minutes at a time. Make sure the compress is warm, not hot, to avoid causing burns.
2. Garlic Oil
Garlic oil has been traditionally used for its antibacterial and anti-inflammatory properties. It can be applied topically to the outer ear canal using a dropper. Before using garlic oil, it is important to ensure that the eardrum is intact and not perforated.
3. Olive Oil
Olive oil can help soothe the ear and provide temporary relief from pain and discomfort. Warm a small amount of olive oil and use a dropper to place a few drops into the affected ear. It is important to lay on your side for a few minutes to allow the oil to reach the ear canal before draining.
4. Breast Milk
Breast milk contains natural antibodies and antimicrobial properties that can help combat infections and reduce inflammation. Applying a few drops of breast milk into the affected ear may help alleviate pain and promote healing.
Managing Ear Infections in Children
Ear infections are particularly common in children, and proper management is essential to prevent complications and promote recovery.
1. Pediatrician Consultation
If you suspect that your child has an ear infection, it is important to seek medical advice from a pediatrician. They can perform a thorough examination, diagnose the condition, and recommend appropriate treatment options. Regular follow-up visits may be necessary to monitor the progress and ensure proper healing.
2. Follow Medication Schedule
If your child is prescribed antibiotics or other medications, it is crucial to follow the prescribed dosage and schedule. Complete the full course of antibiotics, even if symptoms improve, to prevent the recurrence of infection or the development of antibiotic resistance. If your child is receiving ear drops, make sure to administer them as instructed by the healthcare professional.
3. Proper Hygiene
Maintaining proper hygiene practices can help prevent the spread of bacteria or viruses that can lead to ear infections. Encourage your child to wash their hands frequently, especially before meals and after using the restroom. Teach them proper techniques for nose-blowing and covering their mouth and nose when coughing or sneezing.
Complications of Ear Infections
While most ear infections resolve without complications, there are some potential risks to be aware of.
1. Hearing Loss
Untreated or recurrent ear infections can lead to temporary or permanent hearing loss. The buildup of fluid, inflammation, or damage to the delicate structures of the ear can affect hearing ability. It is important to seek prompt medical attention if you experience any changes in hearing or persistent hearing difficulties.
2. Recurrent Infections
Some individuals may be more prone to recurrent ear infections due to factors such as genetic predisposition, anatomical abnormalities, or compromised immune function. If you or your child experiences frequent or recurring ear infections, it is important to work with a healthcare professional to identify the underlying cause and develop a management plan.
3. Spread of Infection
In some cases, ear infections can lead to the spread of infection to nearby structures, such as the mastoid bone or the brain. While these complications are rare, they can be serious and require immediate medical attention if symptoms such as severe headache, neck stiffness, or changes in vision or consciousness occur.
Seeking Medical Attention
Knowing when to seek medical attention for an ear infection is crucial to ensure proper diagnosis and treatment.
1. When to See a Doctor
You should consider seeking medical attention for an ear infection if:
- Symptoms worsen or persist despite home care.
- You experience severe pain or discomfort.
- There is blood or pus draining from the ear.
- You develop a high fever.
- You or your child has difficulty hearing.
- Symptoms are accompanied by severe headaches, neck stiffness, or changes in vision or consciousness.
2. Emergency Situations
If you or your child experience severe symptoms such as a high fever, severe headache, neck stiffness, confusion, seizures, or loss of consciousness, it is considered a medical emergency. Seek immediate medical attention by calling emergency services or going to the nearest emergency room.
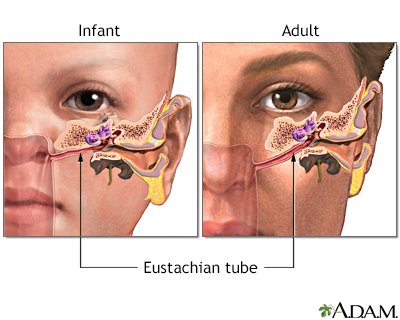
Ear Infections in Adults
While ear infections are commonly associated with children, they can also occur in adults.
1. Age and Risk Factors
Certain risk factors can increase the likelihood of developing ear infections in adulthood. These include a history of frequent or recurrent ear infections, exposure to cigarette smoke or environmental pollutants, allergies, respiratory tract infections, and changes in altitude during air travel or scuba diving. Aging and certain medical conditions that affect the immune system can also increase the risk of ear infections in adults.
2. Treating Adult Ear Infections
The treatment options for adult ear infections are similar to those for children. Antibiotics may be prescribed if the infection is bacterial in nature, and pain relief medications can help alleviate discomfort. In some cases, ear drops may be recommended to relieve inflammation and pain. Follow-up visits may be necessary to monitor the progress and ensure proper healing.
Conclusion
Ear infections can be a painful and discomforting condition, but with proper understanding, prevention, and timely treatment, they can be effectively managed. It is important to be aware of the causes, symptoms, and treatment options for ear infections, as well as the potential complications and when to seek medical attention. By adopting good hygiene practices, staying updated with immunizations, and following the guidance of healthcare professionals, you can minimize the risk of developing ear infections and promote healthy ears for yourself and your loved ones. Remember, the information provided in this article should not replace professional medical advice, and it is always advisable to consult a healthcare professional for an accurate diagnosis and personalized treatment plan.